Liver disease — MCQs

On this page
A person with a history of chronic alcohol consumption who indulged in binge drinking 10 days ago is brought to the emergency department in an unconscious state. A non-contrast CT scan was normal, and his blood glucose level is 45 mg/dL. What is the most appropriate treatment?
A 40-year-old farmer presents with fever, calf tenderness, conjunctival suffusion, retro-orbital pain, and hypokalemia. What is the diagnosis?
A 51-year-old man presents to the office with complaints of a gradual swelling of his face and frothy urine, which was first noticed by his wife 4 days ago. He also noticed that his limbs appear swollen. His past medical history includes diabetes mellitus for the past 10 years. He is currently on metformin and has well-controlled blood sugar and HbA1c levels. He does not smoke and drinks alcohol occasionally. His laboratory results during his last visit 6 months ago were normal. On physical examination, there is pitting edema in the lower extremities and on his face. His vital signs include: blood pressure 121/78 mm Hg, pulse 77/min, temperature 36.7°C (98.1°F), and respiratory rate 10/min. The urinalysis shows: pH 6.2 Color light yellow RBC none WBC 3–4/HPF Protein 4+ Cast fat globules Glucose absent Crystal none Ketone absent Nitrite absent 24-hour urine protein excretion 5.1 g Which of the following is the most likely cause of the generalized edema in this patient?
A 27-year-old man with a history of intravenous drug use comes to the physician because of anorexia, nausea, dark urine, and abdominal pain for 2 weeks. Physical examination shows scleral icterus and right upper quadrant tenderness. Serum studies show: Alanine aminotransferase 1248 U/L Aspartate aminotransferase 980 U/L Hepatitis B surface antigen negative Anti-hepatitis B surface antibody positive Anti-hepatitis C antibody negative Further evaluation shows hepatitis C virus RNA detected by PCR. Without appropriate treatment, which of the following is the most likely outcome of this patient's current condition?
A 40-year-old man visits the office with complaints of fever and abdominal pain for the past 6 days. He is also concerned about his weight loss as he weighs 3.6 kg (8 lb) less, today, than he did 2 months ago. He has a previous history of being admitted to the hospital for recurrent cholangitis. The vital signs include: heart rate 97/min, respiratory rate 17/min, temperature 39.0°C (102.2°F), and blood pressure 114/70 mm Hg. On physical examination, there is tenderness on palpation of the right upper quadrant. The laboratory results are as follows: Hemoglobin 16 g/dL Hematocrit 44% Leukocyte count 18,000/mm3 Neutrophils 60% Bands 4% Eosinophils 2% Basophils 1% Lymphocytes 27% Monocytes 6% Platelet count 345,000/mm3 Aspartate aminotransferase (AST) 57 IU/L Alanine aminotransferase (ALT) 70 IU/L Alkaline phosphatase 140 U/L Total bilirubin 8 mg/dL Direct bilirubin 5 mg/dL An ultrasound is also done to the patient which is shown in the picture. What is the most likely diagnosis?
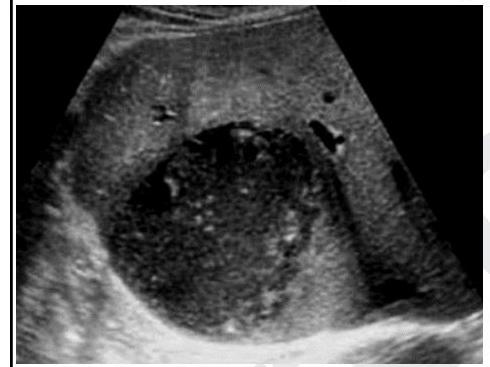
A 36-year-old female presents to the emergency department with right upper quadrant (RUQ) pain. She describes the pain as dull and getting progressively worse over the last several weeks. She denies any relationship to eating. Her past medical history is significant for endometriosis, which she manages with oral contraceptive pills, and follicular thyroid cancer, for which she underwent total thyroidectomy and now takes levothyroxine. The patient drinks a six pack of beer most nights of the week, and she has a 20 pack-year smoking history. She recently returned from visiting cousins in Mexico who have several dogs. Her temperature is 98.2°F (36.8°C), blood pressure is 132/87 mmHg, pulse is 76/min, and respirations are 14/min. On physical exam, her abdomen is soft and non-distended with tenderness in the right upper quadrant and palpable hepatomegaly. Laboratory testing is performed and reveals the following: Aspartate aminotransferase (AST, GOT): 38 U/L Alanine aminotransferase (ALT, GPT): 32 U/L Alkaline phosphatase: 196 U/L gamma-Glutamyltransferase (GGT): 107 U/L Total bilirubin: 0.8 mg/dL RUQ ultrasound demonstrates a solitary, well-demarcated, heterogeneous 6 cm mass in the right lobe of the liver. CT scan with contrast reveals peripheral enhancement during the early phase with centripetal flow during the portal venous phase. Which of the following is a risk factor for this condition?
A 30-year-old woman presents with a history of progressive forgetfulness, fatigue, unsteady gait, and tremor. Family members also report that not only has her speech become slurred, but her behavior has significantly changed over the past few years. On physical examination, there is significant hepatomegaly with a positive fluid wave. There is also distended and engorged veins present radiating from the umbilicus and 2+ lower extremity pitting edema worst in the ankles. There are corneal deposits noted on slit lamp examination. Which of the following conditions present with a similar type of edema? I. Hypothyroidism II. Kwashiorkor III. Mastectomy surgery IV. Heart failure V. Trauma VI. Chronic viral hepatitis VII. Hemochromatosis
A 57-year-old woman comes to the physician because of a 1-month history of lesions on her eyelids. A photograph of the lesions is shown. This patient's eye condition is most likely associated with which of the following processes?
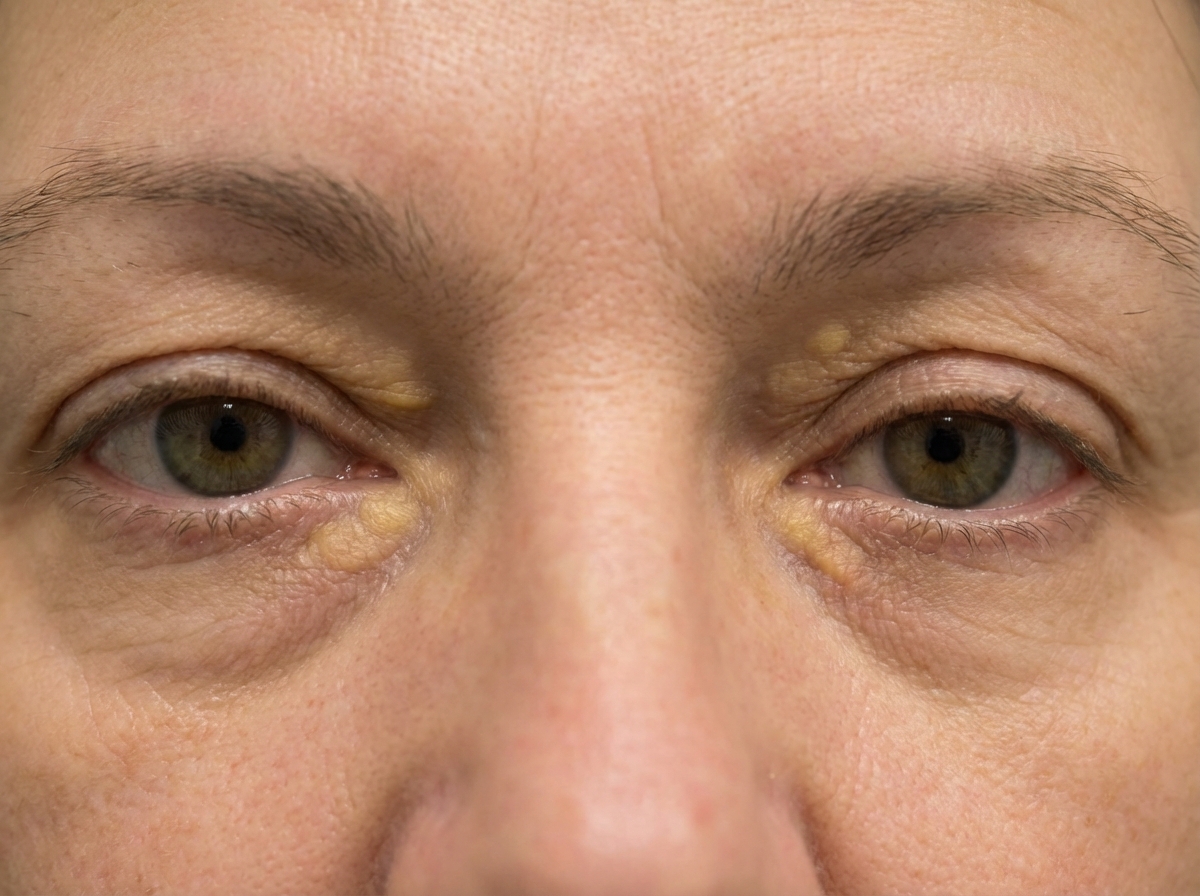
A 37-year-old woman comes to the office complaining of fatigue and itchiness for the past 2 months. She tried applying body lotion with limited improvement. Her symptoms have worsened over the past month, and she is unable to sleep at night due to intense itching. She feels very tired throughout the day and complains of decreased appetite. She does not smoke cigarettes or drink alcohol. Her past medical history is noncontributory. Her father has diabetes and is on medications, and her mother has hypothyroidism for which she is on thyroid supplementation. Temperature is 36.1°C (97°F), blood pressure is 125/75 mm Hg, pulse is 80/min, respiratory rate is 16/min, and BMI is 25 kg/m2. On examination, her sclera appears icteric. There are excoriations all over her body. Abdominal and cardiopulmonary examinations are negative. Laboratory test Complete blood count Hemoglobin 11.5 g/dL Leukocytes 9,000/mm3 Platelets 150,000/mm3 Serum cholesterol 503 mg/dL Liver function test Serum bilirubin 1.7 mg/dL AST 45 U/L ALT 50 U/L ALP 130 U/L (20–70 U/L) Which of the following findings will favor primary biliary cirrhosis over primary sclerosing cholangitis?
A 54-year-old man presents to the emergency department for fatigue and weight loss. He reports feeling increasingly tired over the last several weeks and has lost seven pounds over the last month. His wife has also noticed a yellowing of the eyes. He endorses mild nausea but denies vomiting, abdominal pain, or changes in his stools. Ten years ago, he was hospitalized for an episode of acute pancreatitis. His past medical history is otherwise significant for hyperlipidemia, diabetes mellitus, and obesity. He has two glasses of wine most nights with dinner and has a 30-pack-year smoking history. On physical exam, the patient has icteric sclera and his abdomen is soft, non-distended, and without tenderness to palpation. Bowel sounds are present. Laboratory studies reveal the following: Alanine aminotransferase (ALT): 67 U/L Aspartate aminotransferase (AST): 54 U/L Alkaline phosphatase: 771 U/L Total bilirubin: 12.1 mg/dL Direct bilirubin: 9.4 mg/dL Which of the following would most likely be seen on abdominal imaging?
Practice by Chapter
Viral hepatitis (A, B, C, D, E)
Practice Questions
Alcoholic liver disease
Practice Questions
Non-alcoholic fatty liver disease
Practice Questions
Drug-induced liver injury
Practice Questions
Autoimmune hepatitis
Practice Questions
Cirrhosis management
Practice Questions
Portal hypertension complications
Practice Questions
Ascites diagnosis and management
Practice Questions
Hepatic encephalopathy
Practice Questions
Spontaneous bacterial peritonitis
Practice Questions
Hepatorenal syndrome
Practice Questions
Hepatocellular carcinoma
Practice Questions
Liver transplantation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
