Tuberculosis — MCQs

A 32-year-old man who recently emigrated from Somalia comes to the physician because of a 4-week history of fever, cough, and chest pain. He has had a 5-kg (11-lb) weight loss over the last 3 months despite no changes in appetite. His temperature is 38.1°C (100.6°F). Physical examination shows enlarged cervical lymph nodes. The lungs are clear to auscultation. The results of an interferon-γ release assay are positive. An x-ray of the chest shows bilateral mediastinal lymphadenopathy. A transbronchial needle aspiration biopsy of a mediastinal lymph node is performed; a photomicrograph of the specimen is shown. The structure indicated by the arrow is most likely comprised of which of the following types of cells?
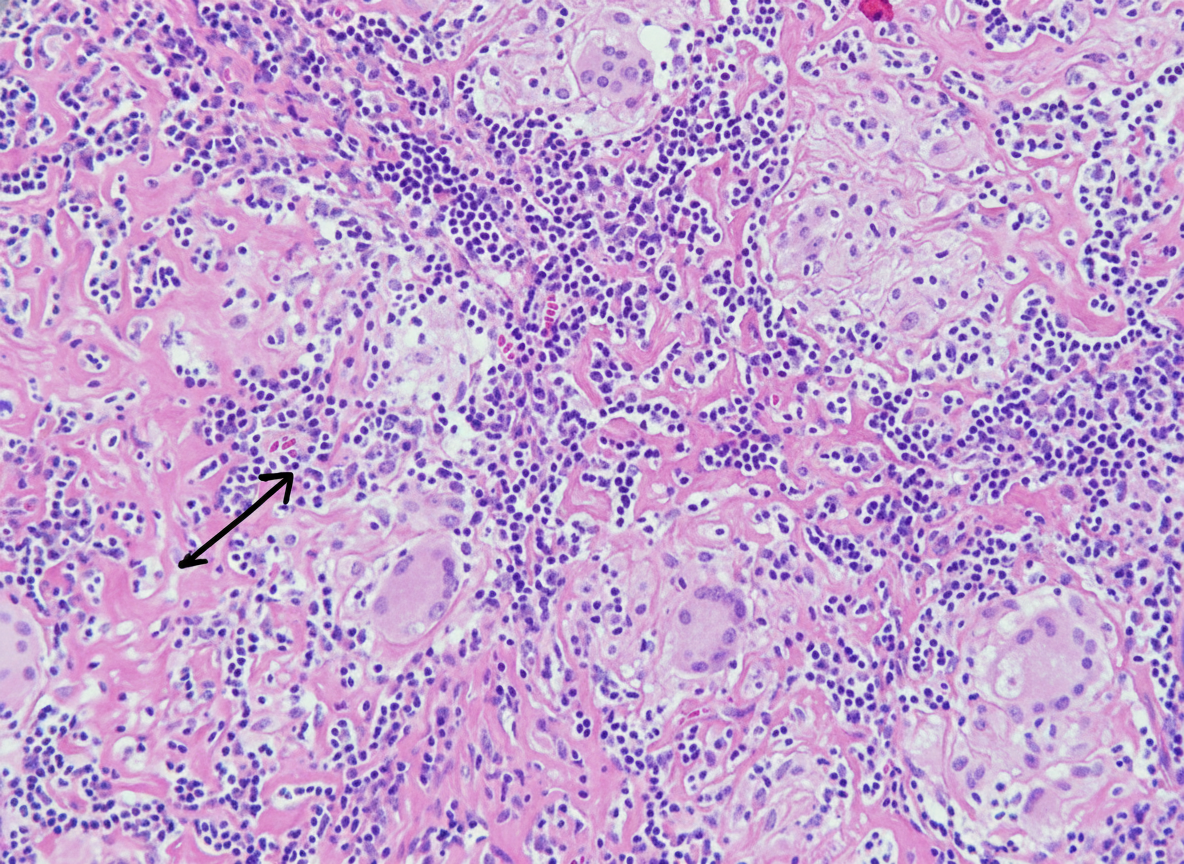
A 24-year-old man comes to the physician for a routine health maintenance examination. He feels well. He has type 1 diabetes mellitus. His only medication is insulin. He immigrated from Nepal 2 weeks ago . He lives in a shelter. He has smoked one pack of cigarettes daily for the past 5 years. He has not received any routine childhood vaccinations. The patient appears healthy and well nourished. He is 172 cm (5 ft 8 in) tall and weighs 68 kg (150 lb); BMI is 23 kg/m2. His temperature is 36.8°C (98.2°F), pulse is 72/min, and blood pressure is 123/82 mm Hg. Examination shows a healed scar over his right femur. The remainder of the examination shows no abnormalities. A purified protein derivative (PPD) skin test is performed. Three days later, an induration of 13 mm is noted. Which of the following is the most appropriate initial step in the management of this patient?
An x-ray of the chest is conducted and shown below. Which of the following is the most appropriate next step in management?
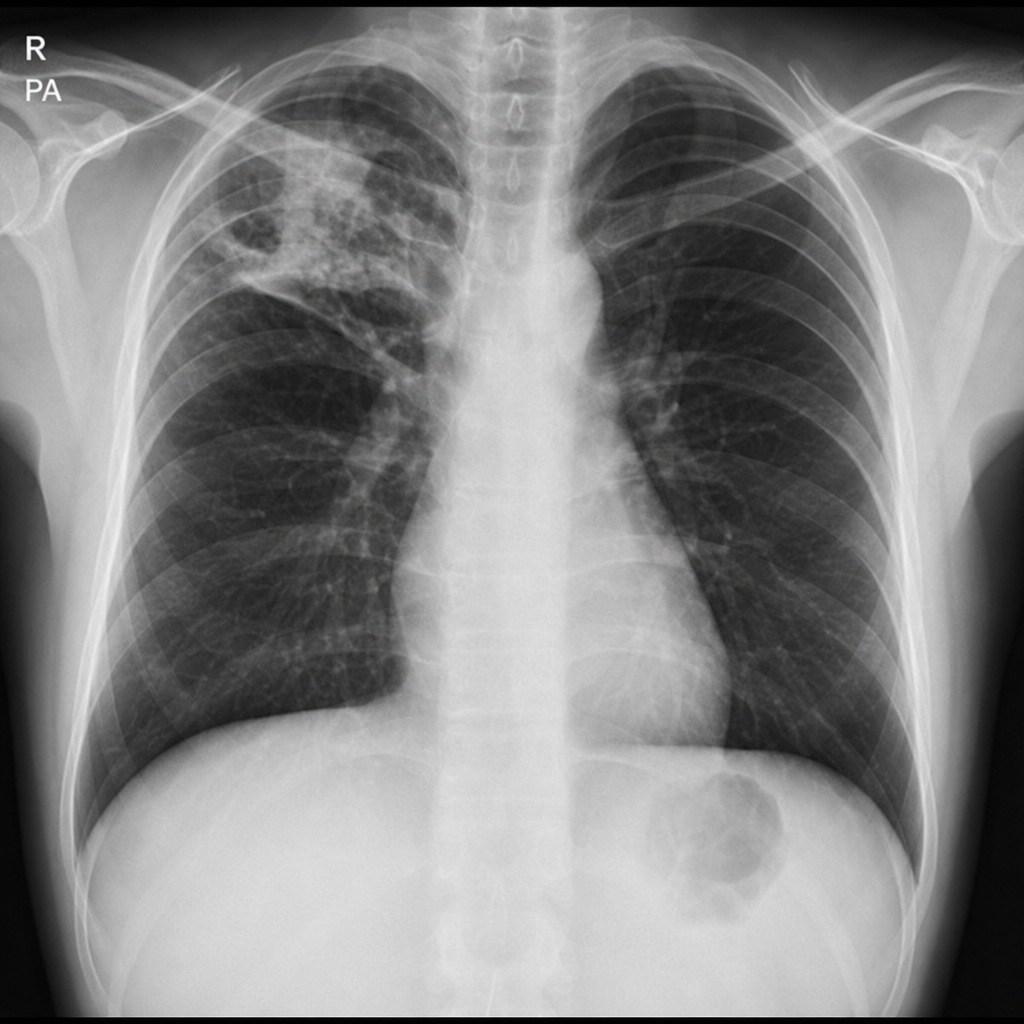
A 68-year-old man presents to the physician with fever, cough, weakness, night sweats, and poor appetite for the past 6 months. Medical records suggest that he has lost 7.5 kg (16.5 lb) of weight during this period. There is no history of breathlessness, nasal discharge, nasal obstruction, palpitations, chest pain, or symptoms related to digestion. He was released from prison 9 months ago after serving a 2-year sentence. His temperature is 38.1°C (100.6°F), pulse is 84/min, respirations are 16/min, and blood pressure is 122/80 mm Hg. Physical examination shows hepatomegaly and generalized lymphadenopathy, and auscultation of the chest reveals diffuse crackles throughout the lung fields bilaterally. On direct ophthalmoscopy, three discrete, yellow-colored, 0.5 mm to 1.0 mm lesions with indistinct borders are seen in the posterior pole. A chest X-ray is shown in the image. Tuberculin skin test with purified protein derivative is negative. What is the most likely diagnosis?
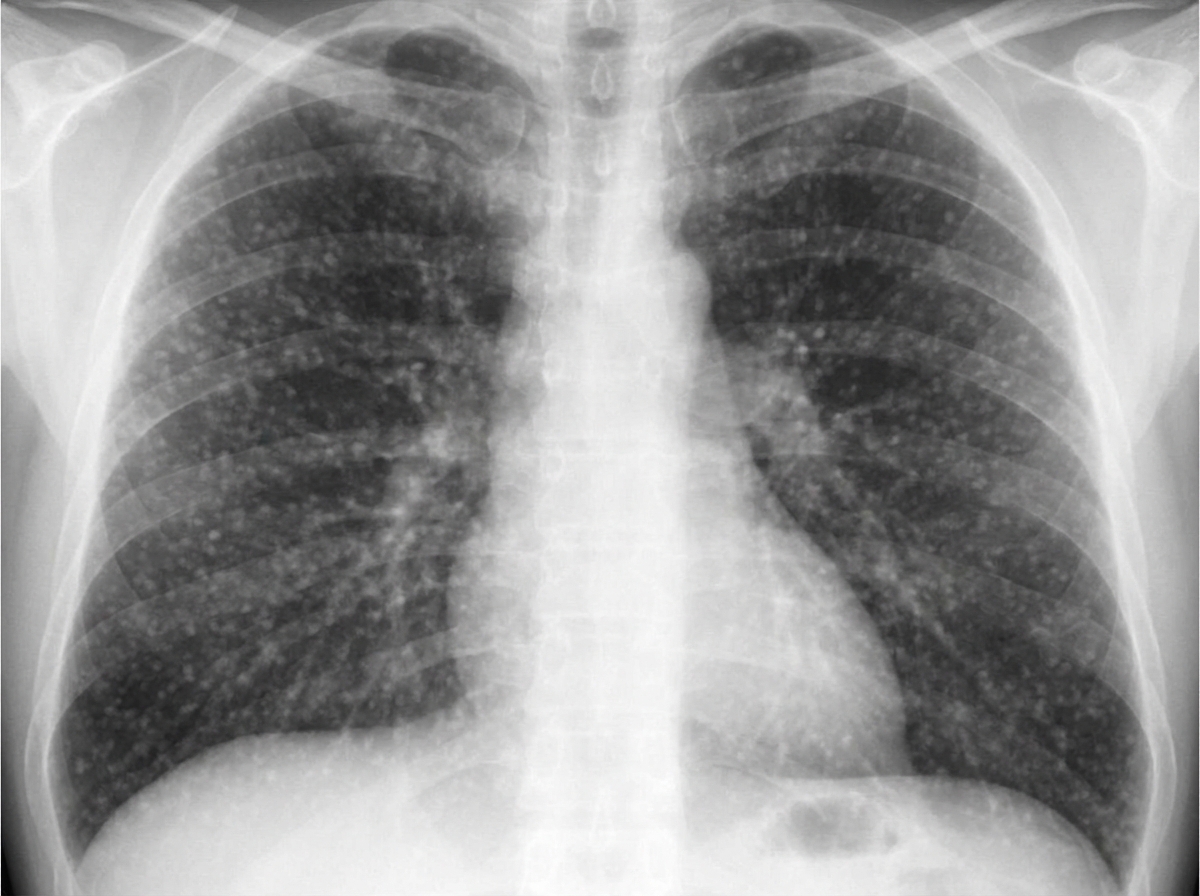
A 55-year-old homeless man is presented to the emergency department by a group of volunteers after they found him coughing up blood during 1 of the beneficiary dinners they offer every week. His medical history is unknown as he recently immigrated from Bangladesh. He says that he has been coughing constantly for the past 3 months with occasional blood in his sputum. He also sweats a lot at nights and for the past 2 days, he has been thirsty with increased frequency of urination and feeling hungrier than usual. The respiratory rate is 30/min and the temperature is 38.6°C (101.5°F). He looks emaciated and has a fruity smell to his breath. The breath sounds are reduced over the apex of the right lung. The remainder of the physical exam is unremarkable. Biochemical tests are ordered, including a hemoglobin A1c (HbA1c) (8.5%) and chest radiography reveals cavitations in the apical region of the right lung. Which of the following immune cells is most critical in orchestrating the formation and maintenance of the granulomatous structure that led to these cavitations?
A 21-year-old U.S. born first year medical student with no prior hospital or healthcare work presents to the physician for a routine physical exam. The patient is HIV negative, denies drug use, and denies sick contacts. The physician places a purified protein tuberculin test in the patient's right forearm intradermally. What is the proper time to read the test and induration diameter that would indicate a positive test result?
A 25-year-old woman presented to an urgent care center with a complaint of a cough for more than 3 weeks that was accompanied by night sweats, weight loss, and malaise. On physical examination, the patient had slightly pale palpebral conjunctivae, bilateral posterior cervical lymphadenopathy, but with no adventitious breath sounds in the lung fields bilaterally. The remainder of the physical examination was routine. The patient was started on a drug regimen that was to be taken for 6 months. On follow-up after 2 months, the ALT and AST levels were elevated. Which of the following anti-tubercular drugs could have contributed to this laboratory result?
A 62-year-old man presents to the emergency department with increased fatigue and changes in his vision. The patient states that for the past month he has felt abnormally tired, and today he noticed his vision was blurry. The patient also endorses increased sweating at night and new onset headaches. He states that he currently feels dizzy. The patient has a past medical history of diabetes and hypertension. His current medications include insulin, metformin, and lisinopril. His temperature is 99.5°F (37.5°C), blood pressure is 157/98 mmHg, pulse is 90/min, respirations are 17/min, and oxygen saturation is 98% on room air. Cardiopulmonary exam is within normal limits. HEENT exam reveals non-tender posterior and anterior chain lymphadenopathy. Abdominal exam reveals splenomegaly and hepatomegaly. There are large, non-tender palpable lymph nodes in the patient's inguinal region. Neurological exam is notable for decreased sensation in the patient's hands and feet. He also complains of a numb/tingling pain in his extremities that has been persistent during this time. Dermatologic exam is notable for multiple bruises on his upper and lower extremities. Which of the following is most likely to be abnormal in this patient?
A 67-year-old man presents to his primary care provider for routine follow-up. He complains of mild fatigue and occasional tingling in both feet. He reports that this numbness and tingling has led to him having 3 falls over the last month. He has had type 2 diabetes mellitus for 23 years and hypertension for 15 years, for which he takes metformin and enalapril. He denies tobacco or alcohol use. His blood pressure is 126/82 mm Hg, the heart rate is 78/min, and the respiratory rate is 15/min. Significant laboratory results are shown: Hemoglobin 10 g/dL Hematocrit 30% Mean corpuscular volume (MCV) 110 fL Serum B12 level 210 picograms/mL Which of the following is the best next step in the management of this patient’s condition?
A 25-year-old woman presents to the emergency department with fatigue and weakness. She states over the past 24 hours she has not felt like herself and has felt like she has no strength. The patient has no significant past medical history other than a single episode of blood-tinged diarrhea 1 week ago which resolved on its own. Her temperature is 99.4°F (37.4°C), blood pressure is 124/62 mmHg, pulse is 95/min, respirations are 29/min, and oxygen saturation is 95% on room air. Physical exam is notable for 2/5 strength of the lower extremities and decreased sensation in the lower extremities and finger tips. Which of the following is the best initial step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
