IBD — MCQs

On this page
A 26-year-old man comes to the emergency room complaining of severe, episodic back pain. He states that it started suddenly this morning. The pain is 9/10 and radiates to his left groin. He endorses seeing blood in his urine earlier but denies dysuria or abnormal urethral discharge. His medical history is significant for Crohn disease, gout, and insulin-dependent diabetes. He takes insulin, allopurinol, and sulfasalazine. He is sexually active with multiple women and uses condoms inconsistently. He drinks 4 cans of beer on the weekends. He denies tobacco use or other recreational drug use. The patient’s temperature is 99°F (37.2°C), blood pressure is 121/73 mmHg, pulse is 89/min, and respirations are 14/min with an oxygen saturation of 94% on room air. A contrast computed tomography of the abdomen and pelvis reveals a 5-mm stone in the left ureter without evidence of hydronephrosis. Urinalysis and urine microscopy reveal hematuria and envelope-shaped crystals. Which of the following most likely contributed to the development of the patient’s acute symptoms?
A 37-year-old man presents to his gastroenterologist due to a transaminitis found by his primary care physician (PCP). He reports currently feeling well and has no acute concerns. Medical history is significant for ulcerative colitis treated with 5-aminosalicylate. He recently went on a trip to Mexico and experienced an episode of mild diarrhea. The patient is 5 ft 4 in and weighs 220 lbs (99.8 kg). His temperature is 98°F (36.7°C), blood pressure is 138/88 mmHg, pulse is 90/min, and respirations are 18/min. Physical examination is unremarkable. Laboratory testing demonstrates: Leukocyte count: 7,200 /mm^3 Alkaline phosphatase: 205 U/L Aspartate aminotransferase (AST): 120 U/L Alanine aminotransferase (ALT): 115 U/L Perinuclear antineutrophil cytoplasmic antibody (pANCA): Positive Antimitochondrial antibody: Negative Which of the following is most likely the diagnosis?
A 44-year-old woman comes to the physician with increasingly yellow sclera and pruritus over the past 3 months. She has intermittent right-upper-quadrant pain and discomfort. She has no history of any serious illnesses and takes no medications. Her vital signs are within normal limits. Her sclera are icteric. Skin examination shows linear scratch marks on the trunk and limbs. The remainder of the physical examination is unremarkable. Laboratory studies show: Complete blood count Hemoglobin 15 g/dL Mean corpuscular volume 95 μm3 Leukocyte count 6,000/mm3 with a normal differential Serum Alkaline phosphatase 470 U/L Aspartate aminotransferase (AST, GOT) 38 U/L Alanine aminotransferase (ALT, GPT) 45 U/L γ-Glutamyltransferase (GGT) 83 U/L (N=5–50 U/L) Bilirubin, total 2.7 mg/dL Bilirubin, direct 1.4 mg/dL Magnetic resonance cholangiopancreatography (MRCP) shows a multifocal and diffuse beaded appearance of the intrahepatic and extrahepatic biliary ducts. Which of the following is the most appropriate diagnostic study at this time?
A 22-year-old white woman comes to the physician because of a 6-month history of lower abdominal pain. She has also had multiple episodes of loose stools with blood during this period. She has had painful bowel movements for 1 month. Over the past year, she has had a 10-kg (22-lb) weight loss. She was treated for streptococcal pharyngitis last week. Her maternal grandfather died of colon cancer at the age of 52 years. She does not smoke. She drinks three to five beers on social occasions. She is 162 cm (5 ft 4 in) tall and weighs 52 kg (115-lb); BMI is 19.7 kg/m2. Her temperature is 37°C (98.6°F), pulse is 60/min, respirations are 13/min, and blood pressure is 110/70 mm Hg. Cardiopulmonary examination shows no abnormalities. The abdomen is soft and there is tenderness to palpation of the left lower quadrant. There is no guarding or rigidity. Rectal examination shows no masses. Laboratory studies show: Hemoglobin 10.4 g/dL Leukocyte count 10,800/mm3 Platelet count 450,000/mm3 Serum Na+ 138 mEq/L Cl- 103 mEq/L K+ 4.9 mEq/L HCO3- 22 mEq/L Urea nitrogen 18 mg/dL Creatinine 0.6 mg/dL Antinuclear antibodies negative Perinuclear antineutrophil cytoplasmic antibodies positive Anti-Saccharomyces cerevisiae antibodies negative A colonoscopy is scheduled for the next day. Which of the following findings is most likely to be present on colonoscopy of this patient?
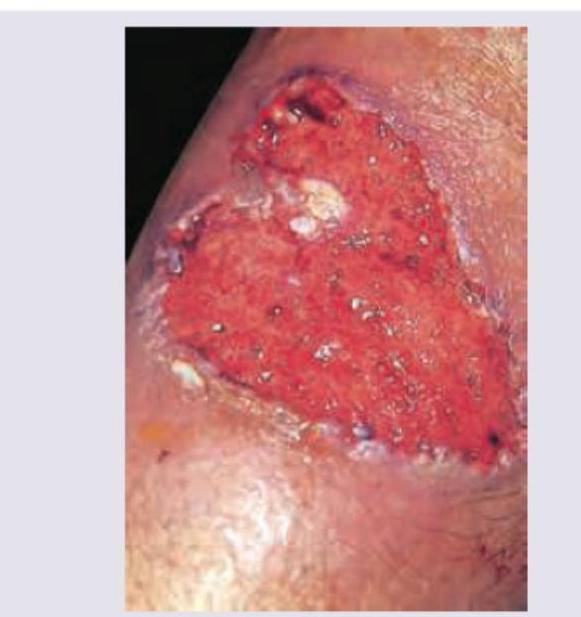
A 24-year-old woman presents with a 3-month history of bloody diarrhea and intermittent abdominal pain. She says that after she has a bowel movement, she still feels as though she needs to go more. She also reports a 10-pound weight loss, significant fatigue, and frequent cravings to chew ice. Her past medical history is significant only for chronic iron deficiency anemia since high school. She currently takes a women’s multivitamin and ferrous sulfate 65 mg orally once daily. She is on the college track team but now is too tired to participate in practice. Her family history is significant for colon cancer and her grandmother died from breast cancer in her 70’s. Her vital signs include: temperature 37.0°C (98.6°F), pulse 102/min, respiratory rate 16/min, blood pressure 100/75 mm Hg. Physical examination is significant for conjunctival pallor, koilonychia, and the cutaneous findings shown in the exhibit. Laboratory tests show elevated ESR and C-reactive protein and findings consistent with iron deficiency anemia. A barium enema demonstrates a lead pipe appearance and a loss of haustra. Which of the following are the recommended screening guidelines for colorectal cancer for this patient?
A 28-year-old woman presents with right lower quadrant abdominal pain, fatigue, and low-volume diarrhea of intermittent frequency for the past 4 months. She also reports weight loss and believes it to be due to a decreased appetite. She has noticed herself being more "forgetful" and she denies seeing any blood in her stool, changes in diet, infection, or recent travel history. Her temperature is 99.5°F (37.5°C), blood pressure is 112/72 mmHg, pulse is 89/min, and respirations are 17/min. Physical examination is unremarkable. Laboratory testing is shown below: Hemoglobin: 10.8 g/dL Hematocrit: 32% Platelet count: 380,000/mm^3 Mean corpuscular volume: 118 µm^3 Reticulocyte count: 0.27% Leukocyte count: 9,900 cells/mm^3 with normal differential Erythrocyte sedimentation rate: 65 mm/h A colonoscopy is performed and demonstrates focal ulcerations with polypoid mucosal changes adjacent to normal appearing mucosa. A biopsy is obtained and shows ulcerations and acute and chronic inflammatory changes. Involvement of which of the following sites most likely explains this patient's clinical presentation?
A 25-year-old man comes to the physician with intermittent bloody diarrhea over the past 2 months. He has occasional abdominal pain. His symptoms have not improved over this time. He has no history of a serious illness and takes no medications. His blood pressure is 110/70 mm Hg, pulse is 75/min, respirations are 14/min, and temperature is 37.8°C (100.0°F). Deep palpation of the abdomen shows mild tenderness in the right lower quadrant. Colonoscopy shows diffuse erythema with a sandpaper pattern involving the rectosigmoid and descending colon, with normal mucosa of the rest of the colon. Biopsy shows involvement of the mucosal and submucosal layers with distortion of crypt architecture and crypt abscess formation. This patient is most likely to develop which of the following hepatobiliary diseases?
A 22-year-old man presents to the emergency department with abdominal pain. The patient states that he has had right lower quadrant abdominal pain for "a while now". The pain comes and goes, and today it is particularly painful. The patient is a college student studying philosophy. He drinks alcohol occasionally and is currently sexually active. He states that sometimes he feels anxious about school. The patient's father died of colon cancer at the age of 55, and his mother died of breast cancer when she was 57. The patient has a past medical history of anxiety and depression which is not currently treated. Review of systems is positive for bloody diarrhea. His temperature is 99.5°F (37.5°C), blood pressure is 100/58 mmHg, pulse is 120/min, respirations are 17/min, and oxygen saturation is 98% on room air. Cardiopulmonary exam is within normal limits. Abdominal exam reveals diffuse tenderness. A fecal occult blood test is positive. Which of the following is the most likely diagnosis?
A 33-year-old woman comes to the physician because of a 4-month history of intermittent lower abdominal cramps associated with diarrhea, bloating, and mild nausea. During this period, she has had a 5-kg (11-lb) weight loss. She feels like she cannot fully empty her bowels. She has no history of serious illness. She has a high-fiber diet. Her father is of Ashkenazi Jewish descent. She appears well. Her temperature is 36.9°C (98.5°F), pulse is 90/min, and blood pressure is 130/90 mm Hg. The lungs are clear to auscultation. Cardiac examination shows no murmurs, rubs, or gallops. Abdominal examination shows mild tenderness to palpation in the right lower quadrant without guarding or rebound. Bowel sounds are normal. Test of the stool for occult blood is negative. Her hemoglobin concentration is 10.5 g/dL, leukocyte count is 12,000 mm3, platelet count is 480,000 mm3, and erythrocyte sedimentation rate is 129 mm/h. A barium enema shows ulceration and narrowing of the right colon. Which of the following is the most likely diagnosis?
A 39-year-old woman presents to your office with 4 days of fever, sore throat, generalized aching, arthralgias, and tender nodules on both of her shins that arose in the last 48 hours. Her medical history is negative for disease and she does not take oral contraceptives or any other medication regularly. The physical examination reveals the vital signs that include body temperature 38.5°C (101.3°F), heart rate 85/min, blood pressure 120/65 mm Hg, tender and enlarged submandibular lymph nodes, and an erythematous, edematous, and swollen pharynx with enlarged tonsils and a patchy white exudate on the surface. She is not pregnant. Examination of the lower limbs reveals erythematous, tender, immobile nodules on both shins. You do not identify ulcers or similar lesions on other areas of her body. What is the most likely diagnosis in this patient?
Practice by Chapter
Crohn's disease pathophysiology
Practice Questions
Ulcerative colitis pathophysiology
Practice Questions
Diagnostic approach to IBD
Practice Questions
Extraintestinal manifestations
Practice Questions
Medical management of Crohn's disease
Practice Questions
Medical management of ulcerative colitis
Practice Questions
Biologic therapies for IBD
Practice Questions
Surgical management in IBD
Practice Questions
Nutritional considerations in IBD
Practice Questions
IBD in pregnancy
Practice Questions
Cancer risk and surveillance in IBD
Practice Questions
IBD-related complications
Practice Questions
IBD in special populations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
