IBD — MCQs

On this page
A 61-year-old man comes to the physician because of fatigue, diarrhea, and crampy abdominal pain for 3 weeks. The abdominal pain is worse after eating. During the past week, he has had up to 4 watery stools daily. He has also had pain in his mouth and gums for 6 days. He has not had nausea, vomiting, or fever. Four months ago, he went on a 1-week trip to the Dominican Republic. He has atrial fibrillation, hypertension, and hypothyroidism. Current medications include levothyroxine, metoprolol, and warfarin. He has smoked one pack of cigarettes daily for 40 years. His temperature is 37.9°C (100.2°F), pulse is 81/min, and blood pressure is 120/75 mm Hg. Examination shows two 1-cm, tender ulcerative lesions in the mouth. Abdominal examination shows mild tenderness to palpation in the right lower quadrant without guarding or rebound. Bowel sounds are normal. His hemoglobin concentration is 11.5 g/dL, mean corpuscular volume is 77 fL, leukocyte count is 11,800/mm³, and platelet count is 360,000/mm³. Colonoscopy with biopsy of the colonic mucosa is performed. Analysis of the specimen shows non-caseating granulomas and neutrophilic inflammation of the crypts. Which of the following is the most likely diagnosis?
A 25-year-old man presents to the emergency department for severe abdominal pain. The patient states that for the past week he has felt fatigued and had a fever. He states that he has had crampy lower abdominal pain and has experienced several bouts of diarrhea. The patient states that his pain is somewhat relieved by defecation. The patient returned from a camping trip 2 weeks ago in the Rocky Mountains. He is concerned that consuming undercooked meats on his trip may have caused this. He admits to consuming beef and chicken cooked over a fire pit. The patient is started on IV fluids and morphine. His temperature is 99.5°F (37.5°C), blood pressure is 130/77 mmHg, pulse is 90/min, respirations are 12/min, and oxygen saturation is 98% on room air. Laboratory studies are ordered and are seen below. Hemoglobin: 10 g/dL Hematocrit: 28% Leukocyte count: 11,500 cells/mm^3 with normal differential Platelet count: 445,000/mm^3 Serum: Na+: 140 mEq/L Cl-: 102 mEq/L K+: 4.1 mEq/L HCO3-: 24 mEq/L BUN: 24 mg/dL Glucose: 145 mg/dL Creatinine: 1.4 mg/dL Ca2+: 9.6 mg/dL Erythrocyte sedimentation rate (ESR): 75 mm/hour Physical exam is notable for a patient who appears to be uncomfortable. Gastrointestinal (GI) exam is notable for abdominal pain upon palpation. Ear, nose, and throat exam is notable for multiple painful shallow ulcers in the patient's mouth. Inspection of the patient's lower extremities reveals a pruritic ring-like lesion. Cardiac and pulmonary exams are within normal limits. Which of the following best describes this patient's underlying condition?
A 24-year-old woman presents to the clinic with chronic abdominal discomfort and cramping. She seeks medical attention now as she is concerned about the diarrhea that she has developed that is occasionally mixed with tiny streaks of blood. Her medical history is significant for lactose intolerance and asthma. She has a family history of wheat allergy and reports that she has tried to make herself vomit on several occasions to lose weight. After counseling the patient about the dangers of bulimia, physical examination reveals the rectum is red, inflamed, tender, and a perirectal abscess is seen draining purulent material. Colonoscopy demonstrates scattered mucosal lesions involving the colon and terminal ileum. A complete blood count is given below: Hb%: 10 gm/dL Total count (WBC): 12,500/mm3 Differential count: Neutrophils: 50% Lymphocytes: 40% Monocytes: 5% ESR: 22 mm/hr What is the most likely diagnosis?
A 28-year-old woman comes to the physician because of a 2-month history of multiple right inframammary lumps. They are tender and have a foul-smelling odor. She has had previous episodes of painful swellings in the axillae 12 months ago that resolved with antibiotic therapy, leaving some scarring. She has Crohn disease. Menses occur at irregular 18- to 40-day intervals and last 1–5 days. The patient's only medication is mesalamine. She appears anxious. She is 162 cm (5 ft 4 in) tall and weighs 87 kg (192 lb); BMI is 33 kg/m2. Vital signs are within normal limits. Examination of the right inframammary fold shows multiple tender, erythematous nodules and fistulas with purulent discharge. Hirsutism is present. Her fasting glucose concentration is 136 mg/dL. Which of the following areas is most likely to also be affected by this patient's condition?
A 42-year-old woman comes to the physician because of increasing fatigue and difficulty concentrating at work for the last 2 months. She has hypertension and a 22-year history of Crohn disease. She has been hospitalized and treated for acute exacerbations, sometimes involving strictures, multiple times in the past. She has not had significant gastrointestinal symptoms in over a year. Current medications include mesalamine, thiazide, and bisoprolol. Her temperature is 37.2°C (99°F), pulse is 72/min, and blood pressure is 140/90 mm Hg. Examination shows a soft abdomen and pale conjunctivae. Rectal examination is unremarkable. Laboratory studies show: Hemoglobin 9.4 g/dL Mean corpuscular volume 112 fL Mean corpuscular hemoglobin 37.2 pg/cell Leukocyte count 8,700 /mm3 Platelet count 150,000 /mm3 Erythrocyte sedimentation rate 42 mm/h Serum Ferritin 88 ng/mL Iron 117 μg/dL Thyroid-stimulating hormone 3.2 μU/mL Thyroxine 7 μg/dL Further evaluation of this patient is most likely to reveal which of the following findings?
A 33-year-old primigravid visits the clinic at the 22 weeks’ gestation with concerns about several episodes of loose watery stool over the past 4 months, which are sometimes mixed with blood. Use of over-the-counter antidiarrheal medications has not been helpful. She also reports having painful ulcers in her mouth for the last 2 months. Pregnancy has been otherwise uncomplicated so far. On physical examination, the blood pressure is 110/60 mm Hg, the pulse rate is 90/min, the respiratory rate is 19/min, and the temperature is 36.6°C (97.8°F). There is bilateral conjunctival redness. Abdominal examination shows minimal tenderness but no guarding or rebound tenderness. Fundal height is proportionate to 22 weeks of gestation, and fetal heart sounds are audible. Colonoscopy shows focal areas of inflammation in the ileum, separated by normal mucosa, with rectal sparing. Based on the colonoscopy results, which of the following complications is the patient at risk for?
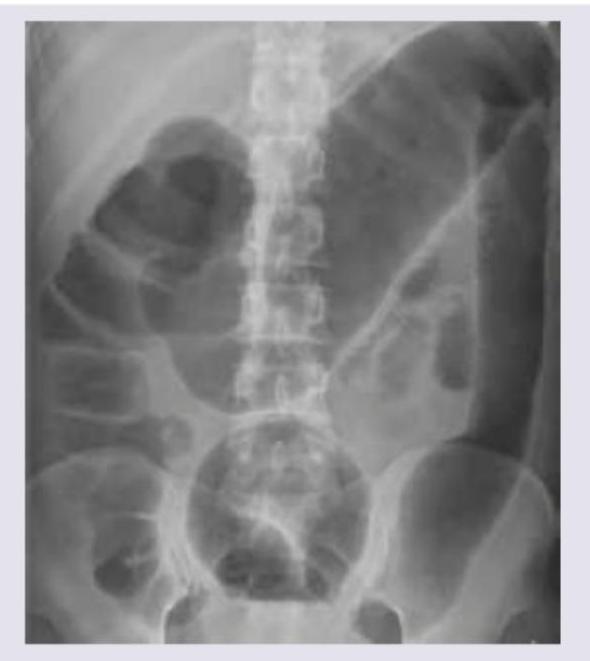
A 53 year-old woman with history of ulcerative colitis presents to the emergency department with a severe flare. The patient reports numerous bloody loose stools, and has been febrile for two days. Vital signs are: T 101.9 HR 98 BP 121/86 RR 17 Sat 100%. Abdominal exam is notable for markedly distended abdomen with tympani and tenderness to palpation without guarding or rebound. KUB is shown in figure A. CT scan shows markedly dilated descending and sigmoid colon with no perforations. What is the next best step in management for this patient?
A 26-year-old male presents to the emergency room with weight loss, abdominal pain, and bloody diarrhea. He reports having intermittent bloody stools and crampy left lower quadrant abdominal pain over the past several days. He is otherwise healthy, does not smoke, and takes no medications. His family history is notable for colon cancer in his father. He subsequently undergoes a colonoscopy which demonstrates a hyperemic friable mucosa with inflammation extending continuously from the rectum proximally through the colon. A biopsy of the rectal mucosa is notable for crypt abscesses and pseudopolyps. This patient’s condition is most commonly associated with what other condition?
A 33-year-old man presents to the clinic complaining of multiple painful joints for the past 2 weeks. The patient notes no history of trauma or any joint disorders. The patient states that he is generally healthy except for a recent emergency room visit for severe bloody diarrhea, which has resolved. On further questioning, the patient admits to some discomfort with urination but notes no recent sexual activity. On examination, the patient is not in acute distress, with no joint deformity, evidence of trauma, swelling, or erythema. He has a decreased range of motion of his right knee secondary to pain. Vital signs are as follows: heart rate 75/min, blood pressure 120/78 mm Hg, respiratory rate 16/min, and temperature 37.3°C (99.0°F). What is the next step in the treatment of this patient?
A 22-year-old woman comes to the physician because of a 1-month history of persistent abdominal cramping, diarrhea, and rectal pain. During the past 2 weeks, she has had up to 4 small volumed, blood-tinged stools with mucus daily. She has also had intermittent fevers and a 4.5-kg (10-lb) weight loss during this time. She traveled to Southeast Asia 3 months ago and received all appropriate vaccinations and medications beforehand. She has no history of serious illness and takes no medications. Her temperature is 37.2°C (99°F), pulse is 90/min, respirations are 16/min, and blood pressure is 125/80 mm Hg. The abdomen is soft, and there is tenderness to palpation of the left lower quadrant with guarding but no rebound. Bowel sounds are normal. The stool is brown, and a test for occult blood is positive. Flexible sigmoidoscopy shows a granular, hyperemic, and friable rectal mucosa that bleeds easily on contact. Which of the following is this patient at greatest risk of developing?
Practice by Chapter
Crohn's disease pathophysiology
Practice Questions
Ulcerative colitis pathophysiology
Practice Questions
Diagnostic approach to IBD
Practice Questions
Extraintestinal manifestations
Practice Questions
Medical management of Crohn's disease
Practice Questions
Medical management of ulcerative colitis
Practice Questions
Biologic therapies for IBD
Practice Questions
Surgical management in IBD
Practice Questions
Nutritional considerations in IBD
Practice Questions
IBD in pregnancy
Practice Questions
Cancer risk and surveillance in IBD
Practice Questions
IBD-related complications
Practice Questions
IBD in special populations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
