Heart failure — MCQs

On this page
A 35-year-old man presents to the physician with concerns that a “bad flu” he has had for the past 10 days is getting worse and causing sleeplessness. On presentation today, his sore throat has improved; however, fever and chest and body aches persist despite the use of ibuprofen. He reports sharp, intermittent chest pain that worsens with exertion. He has not traveled outside the United States recently and does not have a history of substance abuse or alcohol use. Physical examination shows the temperature is 38.3°C (100.9°F), the heart rate is 110/min, the blood pressure is 120/60 mm Hg, and the oxygen saturation is 98% on room air. There is bilateral pedal edema at the level of the ankle. Auscultation reveals normal S1 and S2 and a third early diastolic heart sound. Jugular vein distention is observed. An ECG shows sinus tachycardia and diffuse ST-segment elevation throughout the precordial leads with 1.0-mm PR-segment depression in leads I and II. Laboratory results WBC 14,000/mm3 Lymphocyte count 70% Hematocrit 45% CRP 56 mg/dL Troponin T 1.15 ng/mL Troponin I 0.2 ng/mL Ck-MB 22 ng/mL Coxsackie type b viral antibody positive A chest x-ray shows clear lung fields bilaterally and a mildly enlarged cardiac silhouette. Transthoracic ultrasound reveals a left ventricular ejection fraction of 30%. Which of the following is the cause of difficulty sleeping for this patient?
A 33-year-old woman schedules an appointment at an outpatient clinic for the first time after moving to the US from Peru a few months ago. She complains of easy fatigability and shortness of breath with minimal exertion for the past 6 months. She further adds that her breathlessness is worse when she goes to bed at night. She is also concerned about swelling in her legs. As a child, she says she always had sore throats. She does not smoke or drink alcohol. Medical records are unavailable, but the patient says that she has always been healthy apart from her sore throats. The blood pressure is 114/90 mm Hg, the pulse is 109/min, the respiratory rate is 26/min, and the temperature is 36.7°C (98°F). On examination, she is icteric with distended jugular veins. Bilateral basal crepitations are audible on auscultation of the lungs. Also, a high-pitched apical holosystolic murmur is audible that radiates to the left axilla. A transthoracic echocardiogram reveals mitral regurgitation with an ejection fraction of 25%. Treatment should focus on which of the following?
A 62-year-old woman is hospitalized after a recent viral illness complicated by congestive heart failure. She has a past medical history of obesity and hypertension controlled on lisinopril but was otherwise healthy until she developed fatigue and edema after a recent viral illness. In the hospital, she is started on furosemide to manage her fluid status. On day 5 of her admission, the patient’s temperature is 100.0°F (37.8°C), blood pressure is 136/88 mmHg, pulse is 90/min, and respirations are 14/min. The patient continues to have normal heart sounds, but with crackles bilaterally on lung auscultation. Edema is 3+ up to the bilateral knees. On labs, her leukocyte count is now 13,000/mm^3, up from 9,000/mm^3 the day before. Differential shows that this includes 1,000 eosinophils/mm^3. Creatinine is 1.7 mg/dL from 1.0 mg/dL the day before. Which of the following is most likely expected on urinary analysis?
A 58-year-old man is brought to the Emergency Department after 2 days of shortness of breath, orthopnea, and lower limb edema. His past medical history is significant for hypertension and a myocardial infarction 3 years ago that required a coronary arterial bypass graft. He has not been able to take prescribed medicine in several months due to recent unemployment and issues with insurance. On admission, his blood pressure is 155/92 mmHg, heart rate is 102/min, respiratory rate is 24/min, and temperature is 36.4°C (97.5°F). On physical examination there are fine rales in both lungs, regular and rhythmic cardiac sounds with an S3 gallop and a grade II/VI holosystolic murmur. Initial laboratory tests are shown below: Na+ 140 mEq/L K+ 4.2 mEq/L Cl- 105 mEq/L BUN 20 mg/dL Creatinine 0.8 mg/dL The patient is stabilized and admitted to the hospital. The next day his blood pressure is 110/60 mmHg, heart rate is 110/min, respiratory rate is 18/min, and temperature is 36.4°C (97.5°F). This morning's laboratory tests are shown below: Na+ 135 mEq/L K+ 3.2 mEq/L Cl- 102 mEq/L BUN 45 mg/dL Creatinine 1.7 mg/dL Which of the following best explains the changes seen in this patient?
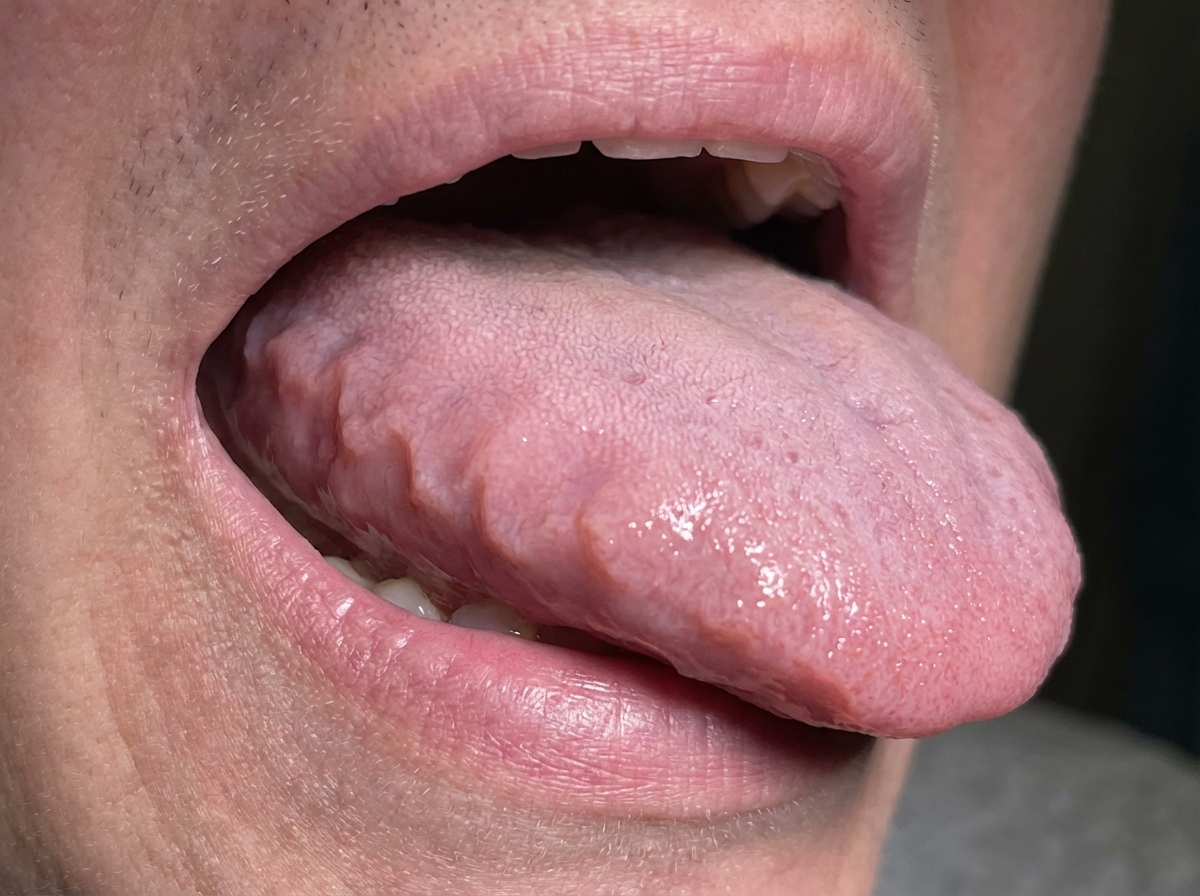
A 71-year-old woman comes to the physician because of progressive shortness of breath and swollen legs for 4 weeks. She has tried sleeping in a raised position using 2 pillows but still wakes up occasionally from a choking sensation. She returned from a safari tour in Tanzania 3 months ago. She has type 2 diabetes mellitus, arterial hypertension, and gastroesophageal reflux disease. Her sister has polymyalgia rheumatica. Her current medications include insulin, enalapril, and omeprazole. She has smoked one half-pack of cigarettes daily for 45 years. Her temperature is 37°C (98.6°F), pulse is 112/min, respirations are 22/min, and blood pressure is 119/76 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 90%. Examination shows pitting edema below the knees and jugular venous distention. Crackles are heard at both lung bases. A photograph of her tongue is shown. Her hemoglobin concentration is 10.0 g/dL, leukocyte count is 6,100/mm3, and erythrocyte sedimentation rate is 62 mm/h. ECG shows sinus rhythm and low-voltage QRS complexes. Echocardiography shows symmetrical left ventricular hypertrophy, reduced diastolic filling, and an ejection fraction of 55%. Which of the following is the most likely cause of this patient's symptoms?
Background and Methods: Aldosterone is important in the pathophysiology of heart failure. In a double-blind study, we enrolled 1,663 patients who had NYHA class III or IV heart failure, a left ventricular ejection fraction of no more than 35%, and who were being treated with an angiotensin-converting-enzyme inhibitor, a loop diuretic, and in most cases digoxin. A total of 822 patients were randomly assigned to receive 25 mg of spironolactone daily and 841 to receive placebo. The primary endpoint was death from all causes. Results: The trial was discontinued early, after a mean follow-up period of 24 months, because an interim analysis determined that spironolactone was efficacious. There were 386 deaths in the placebo group (46%) and 284 in the spironolactone group (35%; relative risk of death, 0.70; 95% confidence interval, 0.60 to 0.82; P<0.001). This 30% reduction in the risk of death among patients in the spironolactone group was attributed to a lower risk of both death from progressive heart failure and sudden death from cardiac causes. The frequency of hospitalization for worsening heart failure was 35% lower in the spironolactone group than in the placebo group (relative risk of hospitalization, 0.65; 95% confidence interval, 0.54 to 0.77; P<0.001). In addition, patients who received spironolactone had a significant improvement in the symptoms of heart failure, as assessed on the basis of the New York Heart Association functional class (P<0.001). Gynecomastia or breast pain was reported in 10% of men who were treated with spironolactone, as compared with 1 percent of men in the placebo group (P<0.001). The incidence of serious hyperkalemia was minimal in both groups of patients. To which of the following patients are the results of this clinical trial applicable?
A 52-year-old man presents to the emergency department with 1-month of progressive dyspnea, decreased exercise tolerance, and inability to sleep flat on his back. He says that he been getting increasingly short of breath over the past few years; however, he attributed these changes to getting older. He started becoming very concerned when he was unable to climb the stairs to his apartment about 3 weeks ago. Since then, he has been experiencing shortness of breath even during activities of daily living. His past medical history is significant for heroin and cocaine use as well as periods of homelessness. Physical exam reveals a gallop that occurs just after the end of systole. Which of the following could lead to the same pathology that is seen in this patient?
A 30-year-old woman visits her local walk-in clinic and reports more than one week of progressive shortness of breath, dyspnea on effort, fatigue, lightheadedness, and lower limb edema. She claims she has been healthy all year round except for last week when she had a low-grade fever, malaise, and myalgias. Upon examination, her blood pressure is 94/58 mm Hg, heart rate is 125/min, respiratory rate is 26/min, and body temperature is 36.4°C (97.5°F). Her other symptoms include fine rattles in the base of both lungs, a laterally displaced pulse of maximum intensity, and regular, rhythmic heart sounds with an S3 gallop. She is referred to the nearest hospital for stabilization and further support. Which of the following best explains this patient’s condition?
A 65-year-old man comes to the physician because of a 10-month history of progressive shortness of breath and a cough productive of a small amount of white phlegm. Bilateral end-expiratory wheezing is heard on auscultation of the chest. Pulmonary function tests show total lung capacity that is 108% of predicted, an FEV1 that is 56% of predicted, and an FEV1:FVC ratio of 62%. Which of the following interventions is most likely to slow the decline in FEV1 in this patient?
A 82-year-old man who is currently being managed by the internal medicine service agrees to be examined by medical students as part of their training in physical examination. He is visited by a small group of medical students under the instruction of a preceptor and allows the students to make observations. They find that he has bibasilar crackles that are most prominent during inspiration as well as some wheezing. Furthermore, he coughs up some sputum during the exam, and this sputum is found to have a rust color. He does not report any pain and no skin findings are seen. Which of the following conditions best explains this patient's physical exam findings?
Practice by Chapter
Classification of heart failure (HFrEF vs HFpEF)
Practice Questions
Heart failure pathophysiology
Practice Questions
Acute decompensated heart failure
Practice Questions
Chronic heart failure management
Practice Questions
Guideline-directed medical therapy
Practice Questions
Device therapy for heart failure
Practice Questions
Cardiomyopathies
Practice Questions
Valvular heart disease and heart failure
Practice Questions
Right heart failure
Practice Questions
Pulmonary hypertension
Practice Questions
Cardio-renal syndrome
Practice Questions
Advanced heart failure and transplantation
Practice Questions
Quality measures in heart failure
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
