Gastroenterology — MCQs

On this page
A 47-year-old woman presents with weakness, shortness of breath, and lightheadedness. She says her symptoms onset gradually 4 months ago and have progressively worsened. Past medical history is significant for a long history of menorrhagia secondary to uterine fibroids. Her vital signs include: temperature 36.9°C (98.4°F), blood pressure 135/82 mm Hg, and pulse 97/min. Physical examination is unremarkable. Laboratory test results are shown below: Hemoglobin 9.2 g/dL Mean corpuscular volume (MCV) 74 μm3 Mean corpuscular hemoglobin (MCH) 21 pg/cell Reticulocyte count 0.4 % Serum ferritin 10 ng/mL Which of the following is a specific feature of this patient's condition?
A 32-year-old male patient presents to a medical office requesting screening for colorectal cancer. He currently has no symptoms and his main concern is that his father was diagnosed with colorectal cancer at 55 years of age. What screening strategy would be the most appropriate?
A 55-year-old female presents to clinic with recurrent episodes of abdominal discomfort and pain for the past month. She reports that the pain occurs 2-3 hours after meals, usually at midnight, and rates it as moderate to severe in intensity when it occurs. She also complains of being fatigued all the time. Past medical history is insignificant. She is an office secretary and says that the job has been very stressful recently. Her temperature is 98.6°F (37.0°C), respiratory rate is 15/min, pulse is 67/min, and blood pressure is 122/98 mm Hg. Her BMI is 34. A physical examination reveals conjunctival pallor and mild tenderness over her epigastric region. Blood tests show: Hb%: 10 gm/dL Total count (WBC): 11,000 /mm3 Differential count: Neutrophils: 70% Lymphocytes: 25% Monocytes: 5% ESR: 10 mm/hr Which of the following is the most likely diagnosis?
A 72-year-old man presents to his primary care physician with the symptom of generalized malaise over the last month. He also has abdominal pain that has been persistent and not relieved by ibuprofen. He has unintentionally lost 22 pounds recently. During this time, the patient has experienced intermittent diarrhea when he eats large meals. The patient has a past medical history of alcohol use, obesity, diabetes mellitus, hypertension, IV drug use, and asthma. His current medications include disulfiram, metformin, insulin, atorvastatin, lisinopril, albuterol, and an inhaled corticosteroid. The patient attends weekly Alcoholics Anonymous meetings and was recently given his two week chip for not drinking. His temperature is 99.5°F (37.5°C), blood pressure is 100/57 mmHg, pulse is 88/min, respirations are 11/min, and oxygen saturation is 98% on room air. The patient's abdomen is tender to palpation, and the liver edge is palpable 2 cm inferior to the rib cage. Neurologic exam demonstrates gait that is not steady. Which of the following is the best initial diagnostic test for this patient?
A 44-year-old woman comes to the emergency department because of a 10-hour history of severe nausea and abdominal pain that began 30 minutes after eating dinner. The pain primarily is in her right upper quadrant and occasionally radiates to her back. She has a history of type 2 diabetes mellitus and hypercholesterolemia. Current medications include metformin and atorvastatin. She is 163 cm (5 ft 4 in) tall and weighs 91 kg (200 lb); BMI is 34 kg/m2. Her temperature is 38.8°C (101.8°F), pulse is 100/min, respirations are 14/min, and blood pressure is 150/76 mm Hg. Abdominal examination shows right upper quadrant tenderness with guarding. A bedside ultrasound shows a gall bladder wall measuring 6 mm, pericholecystic fluid, sloughing of the intraluminal membrane, and a 2 x 2-cm stone at the neck of the gallbladder. The common bile duct appears unremarkable. Laboratory studies show leukocytosis and normal liver function tests. Intravenous fluids are started, and she is given ketorolac for pain control. Which of the following is the most appropriate next step in management?
A 45-year-old man presents to the office for evaluation of pruritic skin lesions, which he has had for 1 month on his elbows and knees. He has been using over-the-counter ointments, but they have not helped. He has not seen a healthcare provider for many years. He has no known allergies. His blood pressure is 140/80 mm Hg, his pulse is 82 beats per minute, his respirations are 18 breaths per minute, and his temperature is 37.2°C (98.9°F). On examination, clustered vesicular lesions are noted on both elbows and knees. Cardiovascular and pulmonary exams are unremarkable. Which of the following would most likely be associated with this patient’s condition?
A 59-year-old man presents to the emergency department with a 6 day history of persistent fevers. In addition, he has noticed that he feels weak and sometimes short of breath. His past medical history is significant for congenital heart disease though he doesn't remember the specific details. He has been unemployed for the last 3 years and has been occasionally homeless. Physical exam reveals nailbed splinter hemorrhages and painful nodes on his fingers and toes. Blood cultures taken 12 hours apart grow out Streptococcus gallolyticus. Which of the following is most likely associated with this patient's disease?
A 23-year-old woman comes to the physician because of a 2-month history of diarrhea, flatulence, and fatigue. She reports having 3–5 episodes of loose stools daily that have an oily appearance. The symptoms are worse after eating. She also complains of an itchy rash on her elbows and knees. A photograph of the rash is shown. Further evaluation of this patient is most likely to show which of the following findings?
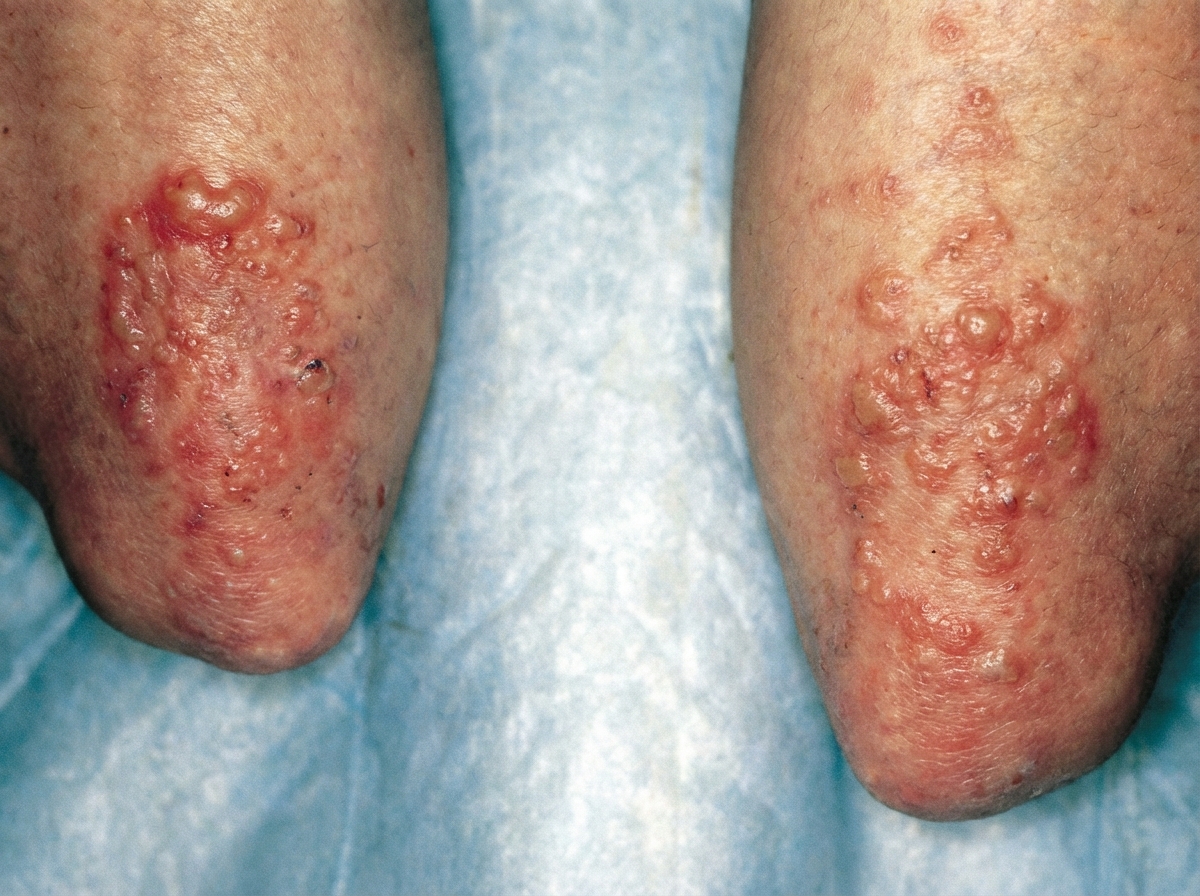
A 28-year-old male comes to the physician for worsening back pain. The pain began 10 months ago, is worse in the morning, and improves with activity. He has also had bilateral hip pain and difficulty bending forward during exercise for the past 3 months. He has celiac disease and eats a gluten-free diet. Examination shows a limited range of spinal flexion. Flexion, abduction, and external rotation of both hips produces pain. Further evaluation of this patient is most likely to show which of the following laboratory findings?
A 13-year-old girl is admitted to the hospital due to muscle weakness, pain, and arthralgia in her wrist joints. The patient says, "I am having trouble walking home after school, especially climbing steep hills." She also complains of malaise. On physical examination, a heliotrope rash is observed around her eyes, and multiple hyperkeratotic, flat, red papules with central atrophy are present on the back of the metacarpophalangeal and interphalangeal joints. Deposits of calcium are also noted on the pads of her fingers. Her serum creatine kinase levels are elevated. Which of the following antibodies is most likely to be found in this patient?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
