Gastroenterology — MCQs

On this page
A 70-year-old man is admitted with fever, chills, and rigor which have lasted for 4 days. He also complains of associated recent-onset fatigue. Past medical history is insignificant. He drinks a can of beer every night. His temperature is 39.0°C (102.2°F), pulse is 120/min, blood pressure is 122/80 mm Hg, and respirations are 14/min. Physical examination reveals splinter hemorrhages in the fingernails, and a 2/6 apical pansystolic murmur is heard which was not present during his last visit a month ago. A transoesophageal echocardiogram shows evidence of vegetations over the mitral valve. Blood cultures are taken from 3 different sites, which reveal the growth of Streptococcus gallolyticus. The patient is started on the appropriate antibiotic therapy which results in rapid clinical improvement. Which of the following would be the best next step in management in this patient after he is discharged?
A 33-year-old man comes to the physician 1 hour after he slipped in the shower and fell on his back. Since the event, he has had severe neck pain. He rates the pain as an 8–9 out of 10. On questioning, he has had lower back pain for the past 2 years that radiates to the buttocks bilaterally. He reports that the pain sometimes awakens him at night and that it is worse in the morning or when he has been resting for a while. His back is very stiff in the morning and he is able to move normally only after taking a hot shower. His temperature is 36.3°C (97.3°F), pulse is 94/min, and blood pressure is 145/98 mm Hg. Range of motion of the neck is limited due to pain; the lumbar spine has a decreased range of motion. There is tenderness over the sacroiliac joints. Neurologic examination shows no abnormalities. An x-ray of the cervical spine shows decreased bone density of the vertebrae. An MRI shows a C2 vertebral fracture as well as erosions and sclerosis of the sacroiliac joints bilaterally. The patient's condition is most likely associated with which of the following findings?
Two days after undergoing emergent laparotomy with splenectomy for a grade IV splenic laceration sustained in a motor vehicle collision, a 54-year-old man develops decreased urinary output. His urine output is < 350 mL/day despite aggressive fluid resuscitation. During the emergent laparotomy, he required three units of packed RBCs. He has type 2 diabetes mellitus and is on an insulin sliding scale. His vital signs are within normal limits. Physical examination shows a healing surgical incision in the upper abdomen and multiple large ecchymoses of the superior right and left abdominal wall. His hematocrit is 28%, platelet count is 400,000/mm3, serum creatinine is 3.9 mg/dL, and serum urea nitrogen concentration is 29 mg/dL. Urinalysis shows brown granular casts. Which of the following is the most likely underlying cause of these findings?
A 32-year-old man recently visiting from Thailand presents with diarrhea and fatigue for the past 6 days, which began before leaving Thailand. The patient denies any recent history of laxatives, nausea, or vomiting. His vital signs include: blood pressure 80/50 mm Hg, heart rate 105/min, and temperature 37.7°C (99.8°F). On physical examination, the patient is pale with dry mucous membranes. A stool sample is obtained for culture, which is copious and appears watery. Which of the following is the correct categorization of this diarrheal disease?
A 72-year-old woman presents to her primary care provider complaining of fatigue for the last 6 months. She can barely complete her morning chores before having to take a long break in her chair. She rarely climbs the stairs to the second floor of her house anymore because it is too tiring. Past medical history is significant for Hashimoto's thyroiditis, hypertension, and hyperlipidemia. She takes levothyroxine, chlorthalidone, and atorvastatin. Her daughter developed systemic lupus erythematosus. She is retired and lives by herself in an old house built in 1945 and does not smoke and only occasionally drinks alcohol. She eats a well-balanced diet with oatmeal in the morning and some protein such as a hardboiled egg in the afternoon and at dinner. Today, her blood pressure is 135/92 mm Hg, heart rate is 110/min, respiratory rate is 22/min, and temperature is 37.0°C (98.6°F). On physical exam, she appears frail and her conjunctiva are pale. Her heart is tachycardic with a regular rhythm and her lungs are clear to auscultation bilaterally. A complete blood count (CBC) shows that she has macrocytic anemia. Peripheral blood smear shows a decreased red blood cell count, anisocytosis, and poikilocytosis with occasional hypersegmented neutrophils. An endoscopy and colonoscopy are performed to rule out an occult GI bleed. Her colonoscopy was normal. Endoscopy shows thin and smooth gastric mucosa without rugae. Which of the following is the most likely cause of this patient's condition?
A 49-year-old man presents to his primary care physician complaining of heartburn and mild epigastric pain after eating for the past 6 months. He reports that his symptoms occur within an hour of eating a meal and persist for approximately an hour. He admits his symptoms have been progressively worsening. He recently began having these symptoms when he lies in the supine position. He has tried eating smaller meals and avoiding spicy food to no avail. He denies vomiting, difficulty swallowing, recent weight loss, or changes in stool color. He does admit to having a "sour" taste in his mouth when symptomatic. His temperature is 99.0°F (37.2°C), blood pressure is 149/82 mmHg, pulse is 86/min, respirations are 18/min, and BMI is 32 kg/m^2. His abdomen is soft, non-tender, and bowel sounds are auscultated in all quadrants. Laboratory results demonstrate the following: Serum: Hemoglobin: 13.5 g/dL Hematocrit: 41% Leukocyte count: 4,500/mm^3 with normal differential Platelet count: 257,000/mm^3 Fecal occult blood test (FOBT): Negative Which of the following is the next best step in management?
A 61-year-old man with HIV comes to the physician because of a 3-week history of fatigue, nonproductive cough, and worsening shortness of breath. He appears ill. Pulse oximetry on room air shows an oxygen saturation of 89%. Laboratory studies show a CD4+ T-lymphocyte count of 67/mm3 (N ≥ 500/mm3) and an elevated HIV viral load. An x-ray of the chest shows diffuse interstitial infiltrates bilaterally. A bronchoalveolar lavage shows disc-shaped yeast cells. In addition to starting antiretroviral therapy, the appropriate treatment for the patient's current illness is initiated. Maintaining the patient on a medication to prevent recurrence of his current illness will also prevent which of the following conditions?
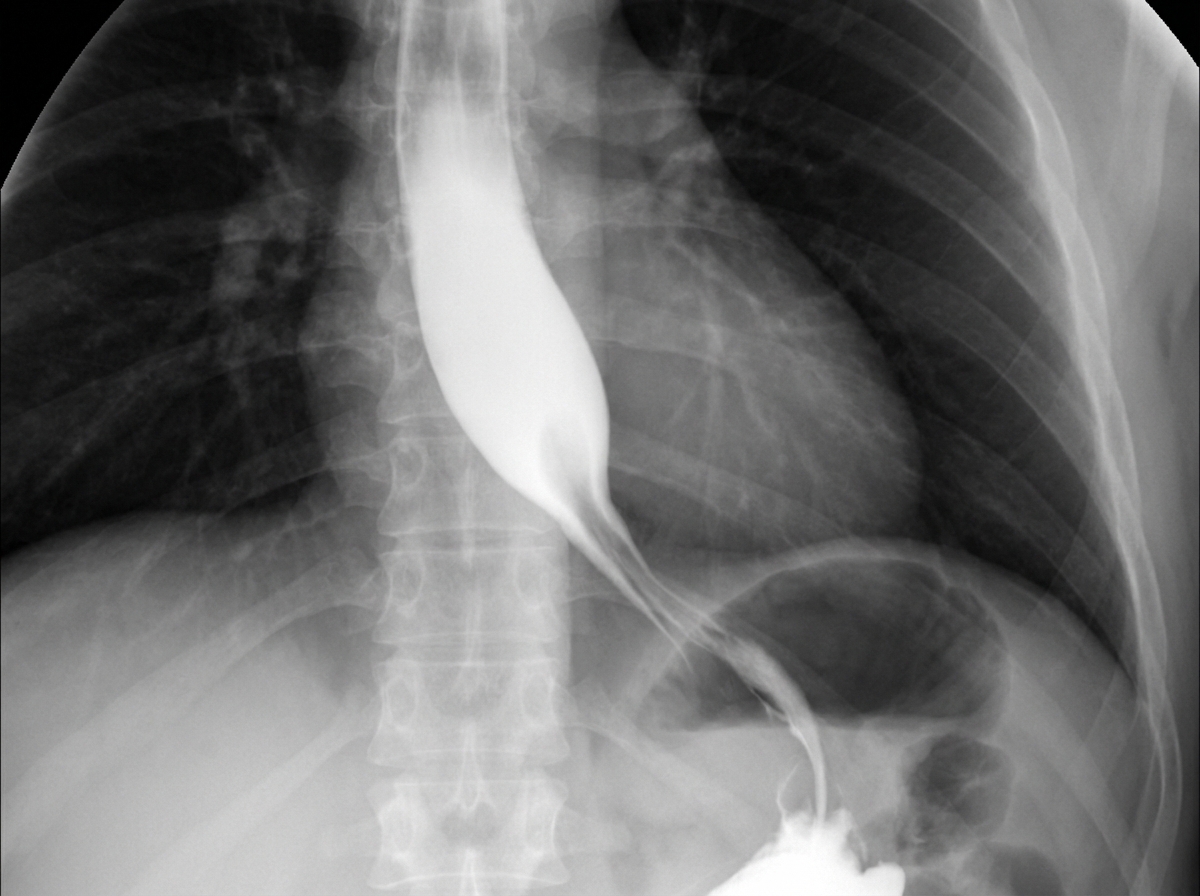
A 56-year-old woman comes to the physician because of a 6-month history of difficulty swallowing food. Initially, only solid food was problematic, but liquids have also become more difficult to swallow over the last 2 months. She also reports occasional regurgitation of food when she lies down. The patient is an avid birdwatcher and returned from a 3-week trip to the Amazon rainforest 3 months ago. She has had a 3.5-kg (7.7-lb) weight loss over the past 6 months. She has not had abdominal pain, blood in her stools, or fever. She underwent an abdominal hysterectomy for fibroid uterus 6 years ago. She has smoked a pack of cigarettes daily for 25 years. Current medications include metformin and sitagliptin. The examination shows no abnormalities. Her hemoglobin concentration is 12.2 g/dL. A barium esophagram is shown. Esophageal manometry monitoring shows the lower esophageal sphincter fails to relax during swallowing. Which of the following is the next best step in management?
A 57-year-old woman presents to her primary care physician with complaints of nausea, vomiting, abdominal pain, and bloating that have increased in severity over the past several months. She reports that she occasionally vomits after eating. She states that the emesis contains undigested food particles. Additionally, the patient states that she often is satiated after only a few bites of food at meals. Her medical history is significant for hypertension and type II diabetes mellitus. Initial laboratory values are notable only for a hemoglobin A1c of 14%. Which of the following is the best initial treatment for this patient?
A 63-year-old man comes to the physician because of a 2-day history of redness, swelling, and pain of the right leg. He also has fever, chills, and nausea. He has noticed liquid oozing from the affected area on his right leg. He has a history of hypertension and gastroesophageal reflux disease. Three months ago, he was hospitalized for treatment of a hip fracture. His current medications include metoprolol, enalapril, and omeprazole. His temperature is 38.7°C (101.7°F), pulse is 106/min, and blood pressure is 142/94 mm Hg. Examination of the right lower leg shows a large area of erythema with poorly-demarcated borders and purulent drainage. The area is nonfluctuant, warm, and tender to touch. Examination of the right groin shows several enlarged, tender lymph nodes. There is mild edema of the ankles bilaterally. Blood and wound cultures are collected. Which of the following is the best next step in management?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
