Gastroenterology — MCQs

On this page
A 26-year-old woman presents with sudden-onset pain in her lower back. She says she was exercising in the gym several hours ago when she felt a sharp pain. The pain is radiating down the side of her leg and into her foot. On physical exam, her vital signs are as follows: HR 95, BP 120/70, T 37.2 degrees C. She has extreme pain shooting down her leg with a straight leg raise. Her sensation to light touch and pin-prick is intact throughout. Which of the following is the most likely diagnosis?
A 47-year-old man presents to the clinic with a 10-day history of a sore throat and fever. He has a past medical history significant for ulcerative colitis and chronic lower back pain. He smokes at least 1 pack of cigarettes daily for 10 years. The father of the patient died of colon cancer at the age of 50. He takes sulfasalazine and naproxen. The temperature is 38.9°C (102.0°F), the blood pressure is 131/87 mm Hg, the pulse is 74/min, and the respiratory rate is 16/min. On physical examination, the patient appears tired and ill. His pharynx is erythematous with exudate along the tonsillar crypts. The strep test comes back positive. In addition to treating the bacterial infection, what else would you recommend for the patient at this time?
A 31-year-old woman visits the clinic with chronic diarrhea on most days for the past four months. She also complains of lower abdominal discomfort and cramping, which is relieved by episodes of diarrhea. She denies any recent change in her weight. Bowel movements are preceded by a sensation of urgency, associated with mucus discharge, and followed by a feeling of incomplete evacuation. The patient went camping several months earlier, and another member of her camping party fell ill recently. Her temperature is 37° C (98.6° F), respiratory rate is 15/min, pulse is 67/min, and blood pressure is 122/98 mm Hg. Her physical examination is unremarkable. A routine stool examination is within normal limits and blood test results show: Hb% 13 gm/dL Total count (WBC): 11,000/mm3 Differential count: Neutrophils: 70% Lymphocytes: 25% Monocytes: 5% ESR: 10 mm/hr What is the most likely diagnosis?
A 17-year-old boy is brought to the physician because of increasing pain and swelling of his right knee for 12 days. He has had episodes of pain with urination for 3 weeks. He had a painful, swollen left ankle joint that resolved without treatment one week ago. His mother has rheumatoid arthritis. He is sexually active with 2 female partners and uses condoms inconsistently. He appears anxious. His temperature is 38°C (100.4°F), pulse is 68/min, and blood pressure is 100/80 mm Hg. Examination shows bilateral inflammation of the conjunctiva. The right knee is tender, erythematous, and swollen; range of motion is limited by pain. There is tenderness at the left Achilles tendon insertion site. Genital examination shows no abnormalities. Laboratory studies show: Hemoglobin 14.5 g/dL Leukocyte count 12,300/mm3 Platelet count 310,000/mm3 Erythrocyte sedimentation rate 38 mm/h Serum Urea nitrogen 18 mg/dL Glucose 89 mg/dL Creatinine 1.0 mg/dL Urine Protein negative Blood negative WBC 12–16/hpf RBC 1–2/hpf An ELISA test for HIV is negative. Arthrocentesis is done. The synovial fluid is cloudy and a Gram stain is negative. Analysis of the synovial fluid shows a leukocyte count of 26,000/mm3 and 75% neutrophils. Which of the following is the most likely diagnosis?
A 75-year-old male is hospitalized for bloody diarrhea and abdominal pain after meals. Endoscopic work-up and CT scan lead the attending physician to diagnose ischemic colitis at the splenic flexure. Which of the following would most likely predispose this patient to ischemic colitis:
A 21-year-old woman presents with the complaints of nausea, vomiting, and diarrhea for 5 days. She adds that she has fever and abdominal cramping as well. She had recently attended a large family picnic and describes eating many varieties of cold noodle salads. Her past medical history is insignificant. Her temperature is 37.5°C (99.6°F), respiratory rate is 15/min, pulse is 67/min, and blood pressure is 92/68 mm Hg. Physical examination is non-contributory. Given the clinical information provided and most likely diagnosis, which of the following would be the next best step in the management of this patient?
A 23-year-old female is found by her roommate in her dormitory. The patient has a history of Type 1 Diabetes Mellitus and was binge drinking the night prior with friends at a local bar. The patient is brought to the emergency department, where vital signs are as follow: T 97.3 F, HR 119 bpm, BP 110/68 mmHg, RR 24, SpO2 100% on RA. On physical exam, the patient is clammy to touch, mucous membranes are tacky, and she is generally drowsy and disoriented. Finger stick glucose is 342 mg/dL; additional lab work reveals: Na: 146 K: 5.6 Cl: 99 HCO3: 12 BUN: 18 Cr: 0.74. Arterial Blood Gas reveals: pH 7.26, PCO2 21, PO2 102. Which of the following statements is correct regarding this patient's electrolyte and acid/base status?
A 37-year-old woman comes to the physician because of a 6-month history of weight loss, bloating, and diarrhea. She does not smoke or drink alcohol. Her vital signs are within normal limits. She is 173 cm (5 ft 8 in) tall and weighs 54 kg (120 lb); BMI is 18 kg/m2. Physical examination shows bilateral white spots on the temporal half of the conjunctiva, dry skin, and a hard neck mass in the anterior midline that does not move with swallowing. Urinalysis after a D-xylose meal shows a decrease in renal D-xylose excretion. Which of the following is most likely to have prevented this patient's weight loss?
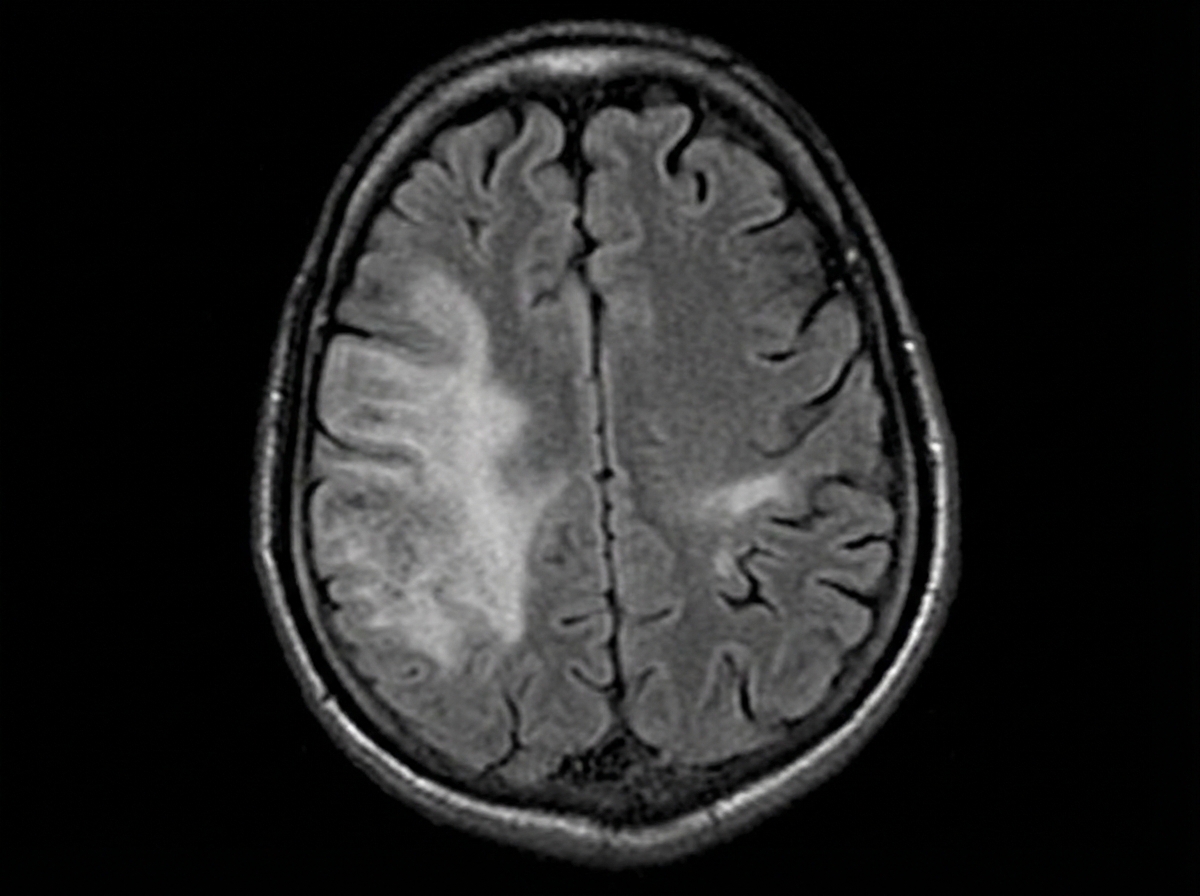
A 35-year-old woman with a history of Crohn disease presents for a follow-up appointment. She says that lately, she has started to notice difficulty walking. She says that some of her friends have joked that she appears to be walking as if she was drunk. Past medical history is significant for Crohn disease diagnosed 2 years ago, managed with natalizumab for the past year because her intestinal symptoms have become severe and unresponsive to other therapies. On physical examination, there is gait and limb ataxia present. Strength is 4/5 in the right upper limb. A T1/T2 MRI of the brain is ordered and is shown. Which of the following is the most likely diagnosis?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
