Gastroenterology — MCQs

On this page
A 47-year-old man presents with upper GI (upper gastrointestinal) bleeding. The patient is known to have a past medical history of peptic ulcer disease and was previously admitted 4 years ago for the same reason. He uses proton-pump inhibitors for his peptic ulcer. Upon admission, the patient is placed on close monitoring, and after 8 hours, his hematocrit is unchanged. The patient has also been hemodynamically stable after initial fluid resuscitation. An upper endoscopy is performed. Which of the following endoscopy findings most likely indicates that this patient will not experience additional GI bleeding in the next few days?
A 76-year-old Japanese man is admitted to the hospital because of a 3-month history of loose stools and worsening peripheral edema. He also reports fatigue, a 10-pound weight loss over the past 6 weeks, and a tingling sensation in his hands and feet over the same time period. Aside from the family dog, he has not had contact with animals for over 1 year and has not traveled outside the country. He has hypertension and benign prostatic hyperplasia. Five years ago, he underwent a partial gastrectomy with jejunal anastomosis for gastric cancer. Current medications include hydrochlorothiazide and tamsulosin. His temperature is 36.8°C (98.2°F), pulse is 103/min, and blood pressure is 132/83 mm Hg. Examination shows a soft and nontender abdomen. There is a well-healed scar on the upper abdomen. Cardiopulmonary examination shows no abnormalities. The conjunctivae appear pale. Sensation to vibration and position is absent over the lower extremities. His hemoglobin concentration is 9.9 g/dL, MCV is 108 μm3, total protein 3.9 g/dL, and albumin 1.9 g/dL. Which of the following is the most likely cause of this patient's condition?
A 25-year-old woman presents to the emergency department with nausea and vomiting. She denies any recent illnesses, sick contacts, or consumption of foods outside of her usual diet. She reports smoking marijuana at least three times a day. Her temperature is 97.7°F (36.5°C), blood pressure is 90/74 mmHg, pulse is 100/min, respirations are 10/min, and SpO2 is 94% on room air. Her conjunctiva are injected. Her basic metabolic panel is obtained below. Serum: Na+: 132 mEq/L Cl-: 89 mEq/L K+: 2.9 mEq/L HCO3-: 30 mEq/L BUN: 35 mg/dL Glucose: 80 mg/dL Creatinine: 1.5 mg/dL Magnesium: 2.0 mEq/L She continues to have multiple bouts of emesis and dry retching. What is the next best step in management?
A 61-year-old woman presents for a routine health visit. She complains of generalized fatigue and lethargy on most days of the week for the past 4 months. She has no significant past medical history and is not taking any medications. She denies any history of smoking or recreational drug use but states that she drinks "socially" approx. 6 nights a week. She says she also enjoys a "nightcap," which is 1–2 glasses of wine before bed every night. The patient is afebrile, and her vital signs are within normal limits. On physical examination, there is significant pallor of the mucous membranes. Laboratory findings are significant for a mean corpuscular volume (MCV) of 72 fL, leukocyte count of 4,800/mL, hemoglobin of 11.0 g/dL, and platelet count of 611,000/mL. Stool guaiac test is negative. She is started on oral ferrous sulfate supplements. On follow-up, her laboratory parameters show no interval change in her MCV or platelet level, and she reports good compliance with the medication. Which of the following is the best next step in the management of this patient?
A 37-year-old man presents to his primary care provider with dysphagia. He notes that his symptoms began several weeks ago and have worsened over time. He now has trouble swallowing solids and liquids. He denies any other symptoms. He has no significant past medical history. Travel history reveals a recent trip to South America but no other travel outside the United States. His temperature is 100°F (37.8°C), blood pressure is 120/81 mmHg, pulse is 99/min, respirations are 14/min, and oxygen saturation is 98% on room air. HEENT exam is unremarkable. He has no palpable masses in his abdomen. What is the most appropriate next step in management?
A 74-year-old man presents to the emergency department with sudden onset of abdominal pain that is most felt around the umbilicus. The pain began 16 hours ago and has no association with meals. He has not been vomiting, but he has had several episodes of bloody loose bowel movements. He was hospitalized 1 week ago for an acute myocardial infarction. He has had diabetes mellitus for 35 years and hypertension for 20 years. He has smoked 15–20 cigarettes per day for the past 40 years. His temperature is 36.9°C (98.4°F), blood pressure is 95/65 mm Hg, and pulse is 95/min. On physical examination, the patient is in severe pain, there is a mild periumbilical tenderness, and a bruit is heard over the epigastric area. Which of the following is the most likely diagnosis?
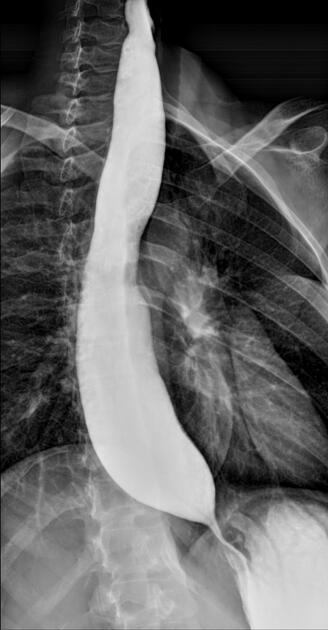
A 37-year-old man presents to the physician because of dysphagia and regurgitation for the past 5 years. In recent weeks, it has become very difficult for him to ingest solid or liquid food. He has lost 3 kg (6 lb) during this time. He was admitted to the hospital last year because of pneumonia. Three years ago, he had an endoscopic procedure which partially improved his dysphagia. He takes amlodipine and nitroglycerine before meals. His vital signs are within normal limits. BMI is 19 kg/m2. Physical examination shows no abnormalities. A barium swallow X-ray is shown. Which of the following patterns of esophageal involvement is the most likely cause of this patient’s condition?
A 52-year-old woman presents to the clinic with complaints of intermittent chest pain for 3 days. The pain is retrosternal, 3/10, and positional (laying down seems to make it worse). She describes it as “squeezing and burning” in quality, is worse after food intake and emotional stress, and improves with antacids. The patient recently traveled for 4 hours in a car. Past medical history is significant for osteoarthritis, hypertension and type 2 diabetes mellitus, both of which are moderately controlled. Medications include ibuprofen, lisinopril, and hydrochlorothiazide. She denies palpitations, dyspnea, shortness of breath, weight loss, fever, melena, or hematochezia. What is the most likely explanation for this patient’s symptoms?
A 42-year-old Caucasian male presents to your office with hematuria and right flank pain. He has no history of renal dialysis but has a history of recurrent urinary tract infections. You order an intravenous pyelogram, which reveals multiple cysts of the collecting ducts in the medulla. What is the most likely diagnosis?
A 50-year-old Caucasian man presents for a routine checkup. He does not have any current complaint. He is healthy and takes no medications. He has smoked 10–15 cigarettes per day for the past 10 years. His family history is negative for gastrointestinal disorders. Which of the following screening tests is recommended for this patient according to the United States Preventive Services Task Force (USPSTF)?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
