Gastroenterology — MCQs

On this page
A 28-year-old woman presents to the emergency department with fever, chills, nausea, vomiting, and right flank pain for 2 days. Temperature is 39.2°C (102.6°F), blood pressure is 95/60 mmHg, pulse is 110/min, and respirations are 18/min. She appears ill and is unable to tolerate oral fluids. Physical examination shows right costovertebral angle tenderness. Urinalysis shows: Protein 1+ Leukocyte esterase positive Nitrite positive RBC 2/hpf WBC 90/hpf WBC casts numerous Which of the following is the most appropriate next step in management?
A 49-year-old man comes to the hospital for a 10-day history of cough and worsening shortness of breath. He has sharp right-sided chest pain that worsens on inspiration and coughing. Two weeks ago, the patient was admitted to the hospital after passing out on the street from alcohol intoxication but he left against medical advice. He has coronary artery disease and hypertension, and he does not take any medications. He drinks 4 cans of beer daily and has smoked 2 packs of cigarettes daily for 20 years. His temperature is 38.5°C (101.3° F), pulse is 110/min, respirations are 29/min, and blood pressure is 110/65 mmHg. Examination shows poor dentition. There is dullness to percussion at the base of the right lung. Crackles and markedly decreased breath sounds are heard over the right middle and lower lung fields. An x-ray of the chest shows a right-sided loculated pleural effusion and consolidation of the surrounding lung with visible air bronchogram; there are no rib fractures. Thoracocentesis is performed. Examination of this patient's pleural fluid is most likely to show which of the following findings?
A 65-year-old man presents to his primary care physician for fatigue. The patient states that he has not been sleeping well and requests sleep medication to help him with his fatigue. He recently changed his diet to try to increase his energy and has been on a vegetarian diet for the past several months. The patient has no significant past medical history. He smokes 1 pack of cigarettes per day and drinks 5 alcoholic beverages per day. The patient has lost 12 pounds since his last visit 1 month ago. Physical exam demonstrates a tired man. He appears thin, and his skin and sclera are icteric. Abdominal ultrasound is notable for a thin-walled and enlarged gallbladder. A urine sample is collected and is noted to be amber in color. Which of the following is the most likely diagnosis?
A 53-year-old woman presents to the office complaining of an extreme, nonradiating stabbing pain in the epigastric region after having a meal. She states that it has happened several times in the past week approximately 30 minutes after eating and spontaneously resolves. A day before, the patient went to urgent care with the same complaint, but the abdominal X-ray was normal. Surgical history is remarkable for a total knee arthroplasty procedure 6 months ago. She has lost 34 kg (75 lb) since the operation because of lifestyle changes. The vital signs are normal. Laparoscopic surgical scars are well healed. Endoscopy shows benign mucosa to the proximal duodenum. A barium swallow study reveals an extremely narrowed duodenum. Which of the following structures is most likely responsible for this patient’s current symptoms?
A 55-year-old man comes to the physician because of heartburn for the past 2 years. He has no chest pain, dysphagia, weight loss, or fever. He has no history of any serious illnesses. He takes omeprazole daily. Vital signs are within normal limits. Body mass index (BMI) is 34 kg/m2. Physical exam shows no abnormalities. An endoscopic image of the lower esophageal sphincter is shown. Which of the following is the most important next step in management?
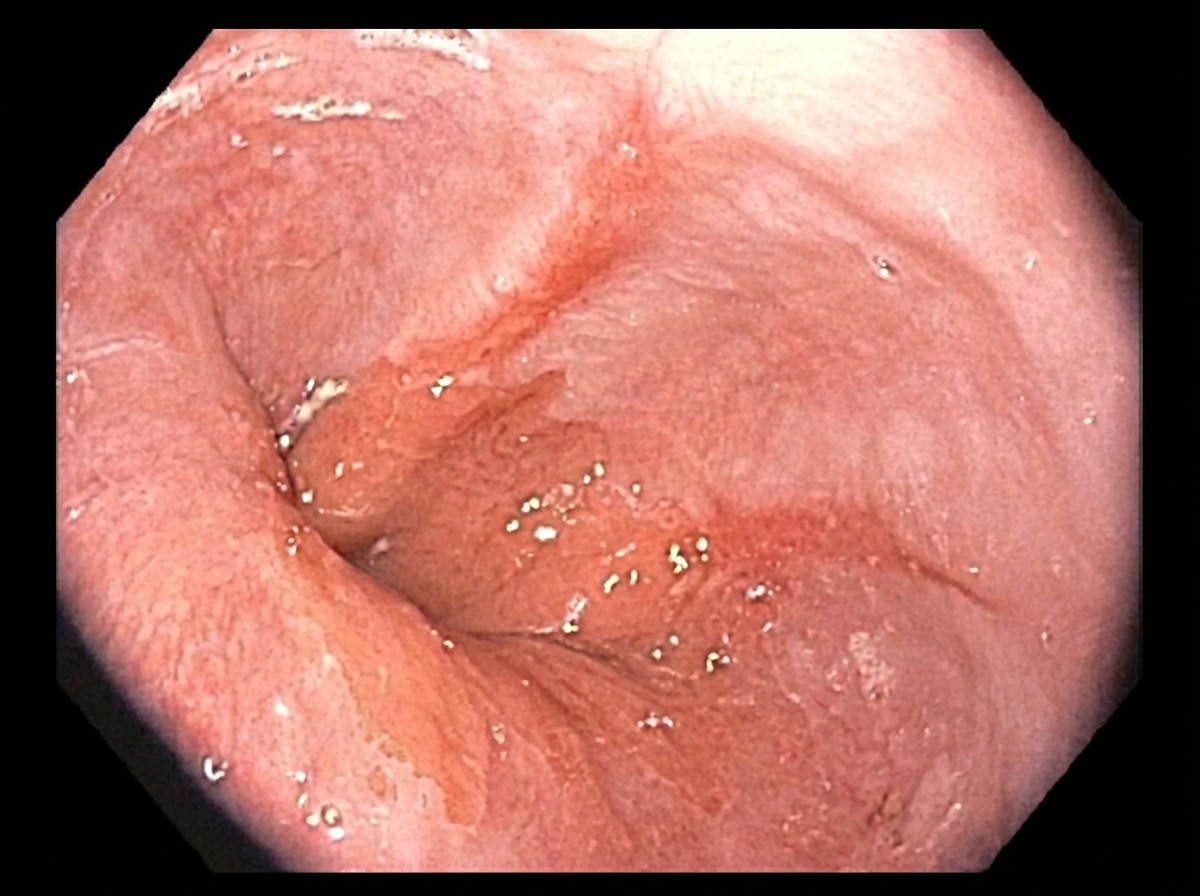
A 48-year-old man presents to an urgent care center with epigastric discomfort following meals and an occasional dry cough worse in the morning, both of which have increased in frequency over the past several months. He is otherwise healthy and has no additional complaints. Past medical history is significant for major depressive disorder, anxiety, and hypothyroidism. Physical examination is unremarkable. His vital signs include temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 74/min, and respiratory rate 14/min. Given the following options, what is the most appropriate next step in patient management?
A 56-year-old man comes to the clinic complaining of intermittent abdominal pain for the past 2 months. He reports that the pain improves with oral intake and is concentrated at the epigastric area. The pain is described as gnawing in quality and improves when he takes his wife’s ranitidine. He denies weight changes, fever, chest pain, or recent travel but endorses “brain fog” and decreased libido. An upper endoscopy reveals ulcerations at the duodenum and jejunum. Physical examination demonstrates bilateral hemianopsia, gynecomastia, and diffuse pain upon palpation at the epigastric area. Laboratory findings are demonstrated below: Serum: Na+: 137 mEq/dL Cl-: 96 mEq/L K+: 3.9 mEq/dL HCO3-: 25 mEq/L Glucose: 110 mg/dL Creatinine: .7 mg/dL Ca2+: 13.5 mg/dL What is the best explanation for this patient’s findings?
A 41-year-old man presents to the office with pain in his right big toe. The pain started yesterday and has been progressively getting worse to the point that it is difficult to walk. He describes his right big toe as being swollen and hot to the touch. He has never had symptoms like this before. He drinks 3 beers per night. Medical history is otherwise significant for chronic kidney disease. Physical examination is notable for an overweight gentleman in moderate pain, with an erythematous, swollen and tender right toe. He is afebrile. A joint fluid analysis in this patient is most likely to show what?
A 24-year-old man comes to the physician for a routine health maintenance examination. He feels well. He has type 1 diabetes mellitus. His only medication is insulin. He immigrated from Nepal 2 weeks ago . He lives in a shelter. He has smoked one pack of cigarettes daily for the past 5 years. He has not received any routine childhood vaccinations. The patient appears healthy and well nourished. He is 172 cm (5 ft 8 in) tall and weighs 68 kg (150 lb); BMI is 23 kg/m2. His temperature is 36.8°C (98.2°F), pulse is 72/min, and blood pressure is 123/82 mm Hg. Examination shows a healed scar over his right femur. The remainder of the examination shows no abnormalities. A purified protein derivative (PPD) skin test is performed. Three days later, an induration of 13 mm is noted. Which of the following is the most appropriate initial step in the management of this patient?
A 42-year-old man is brought to the emergency department by his wife because of a 1-day history of progressive confusion. He recently lost his job. He has a history of chronic alcoholism and has been drinking 14 beers daily for the past week. Before this time, he drank 6 beers daily. He appears lethargic. His vital signs are within normal limits. Serum studies show a sodium level of 111 mEq/L and a potassium level of 3.7 mEq/L. Urgent treatment for this patient's current condition increases his risk for which of the following adverse events?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
