Gastroenterology — MCQs

On this page
A 53-year-old man presents to your office with a 2 month history of abdominal bloating. He states that he feels full after eating only a small amount and has experienced bloating, diarrhea, and occasionally vomiting when he tries to eat large amounts. He states his diarrhea has now become more profuse and is altering the quality of his life. One week ago, the patient was given antibiotics for an ear infection. He states he is trying to eat more healthy and has replaced full fat with fat free dairy and is reducing his consumption of meat. His temperature is 99.0°F (37.2°C), blood pressure is 164/99 mmHg, pulse is 85/min, respirations are 14/min, and oxygen saturation is 98% on room air. Laboratory values from a previous office visit are notable for a hemoglobin A1c of 13%. Which of the following is the best treatment of this patient's diarrhea?
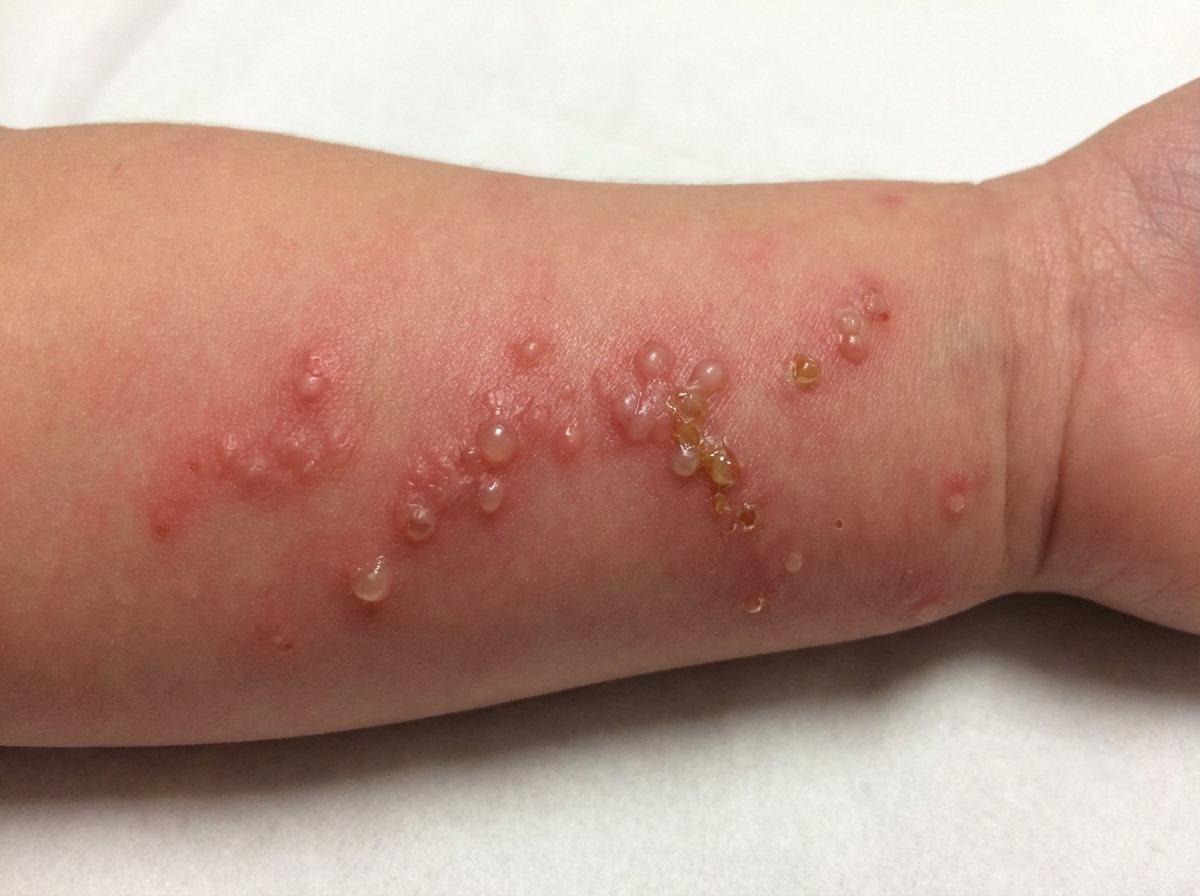
A 14-year-old boy comes to the physician because of an itchy rash on his right arm for 1 day. The rash started as small papules, then progressed into blisters with oozing. He has had atopic dermatitis at the age of 6 years. His vital signs are within normal limits. A photograph of the patient's arm is shown. There is no lymphadenopathy. Avoidance of contact with which of the following would most likely have prevented this patient's symptoms?
A 51-year-old white female presents to her primary care physician for a regular check-up. She endorses eating a healthy diet with a balance of meat and vegetables. She also states that she has a glass of wine each night with dinner. As part of the evaluation, a complete blood count and blood smear were performed and are remarkable for: Hemoglobin 8.7 g/dL, Hematocrit 27%, MCV 111 fL, and a smear showing macrocytes and several hypersegmented neutrophils. Suspecting an autoimmune condition with anti-intrinsic factor antibodies, what other finding might you expect in this patient?
Treatment with intravenous acyclovir is initiated. Three days later, the patient develops progressively worse fatigue, headache, and colicky pain in his right flank. His temperature is 36.7°C (98°F), pulse is 85/min, and blood pressure is 135/80 mm Hg. Examination shows no new lesions. Laboratory studies show: Hemoglobin 11.3 g/dL Serum Na+ 140 mEq/L Cl- 99 mEq/L K+ 5.5 mEq/L HCO3- 22 mEq/L Urea nitrogen 56 mg/dL Creatinine 3.2 mg/dL Which of the following is the most likely finding on urinalysis?
A 28-year-old man comes to the physician for the evaluation of five episodes of painful oral ulcers over the past year. During this period, he has also had two painful genital ulcers that healed without treatment. He reports frequently having diffuse joint pain, malaise, and low-grade fever. There is no personal or family history of serious illness. He emigrated to the US from Syria with his family four years ago. He is sexually active with one female partner and they do not use condoms. He takes no medications. His temperature is 38°C (100.4°F), pulse is 90/min, and blood pressure is 130/80 mm Hg. Physical examination shows three painful ulcers on the oral buccal mucosa. Pelvic examination shows that the external genitalia has several healing scars. The remainder of the examination shows no abnormalities. Which of the following is the most likely diagnosis?
A 67-year-old man presents to his primary care physician for abdominal pain. The patient states that he has had abdominal pain for the past month that has been steadily worsening. In addition, he endorses weight loss and general fatigue. The patient has a past medical history of obesity, diabetes, and hypertension. His current medications include metformin, insulin, and lisinopril. The patient is a current smoker and drinks roughly 3 drinks per day. His temperature is 99.5°F (37.5°C), blood pressure is 139/79 mmHg, pulse is 95/min, respirations are 17/min, and oxygen saturation is 98% on room air. The patient's cardiac and pulmonary exams are within normal limits. Examination of the patient's lower extremity reveals multiple tender palpable masses bilaterally that track linearly along the patient's lower extremity. Which of the following is the next best step in management?
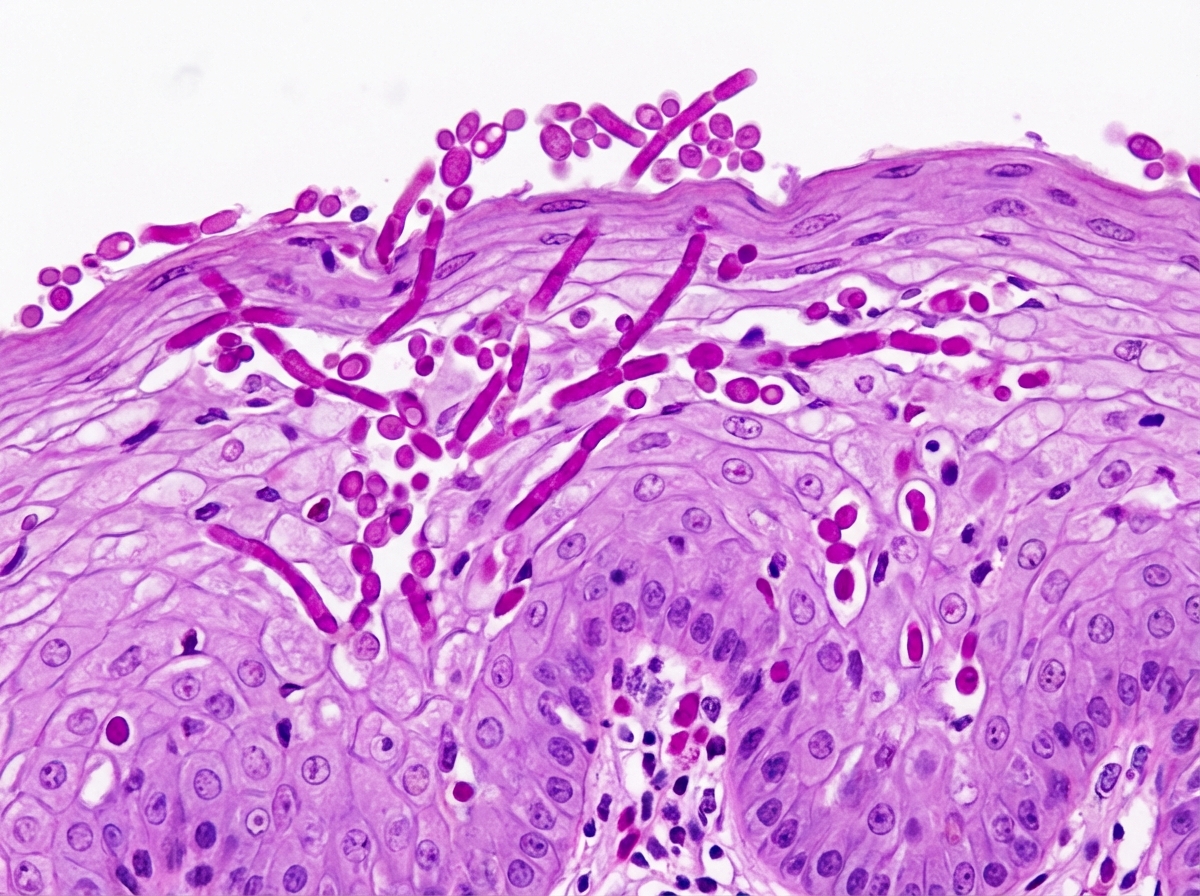
A 44-year-old man presents to a clinic for the evaluation of difficulty swallowing for the past few days. He says that he has noticed progressively worsening chest pain when he attempts to swallow solids or liquids. He works from a home office, has not had any recent sick contacts, and is currently not sexually active. His medical history includes AIDS. His current medications include emtricitabine, rilpivirine, and tenofovir. His temperature is 38.1°C (100.6°F), pulse is 72/min, respirations are 18/min, and blood pressure is 136/84 mm Hg. A physical examination is notable for a dry mouth with red mucosa and no distinct plaques or patches, and a supple neck with no masses or cervical lymphadenopathy. An esophagogastroduodenoscopy shows small white patches within the esophageal lumen. A biopsy of one of the lesions is performed and the microscopic appearance of the finding is shown below. Which of the following is the most likely diagnosis?
A 36-year-old Caucasian woman is referred to the outpatient clinic by a physician at a health camp for 6-months of foul-smelling diarrhea with bulky and floating stools as well as significant flatulence which makes her extremely uncomfortable at work and social events. She has concomitant weight loss and recently fractured her wrist in a seemingly insignificant fall from her own height. Vital signs are normal and a physical examination shows grouped, papulovesicular, pruritic skin lesions, as well as areas of hypoesthesia in the hands and feet. Which of the following would be most useful in this case?
A 73-year-old man presents to his primary care physician complaining of increased urinary frequency, nocturia, and incomplete emptying after void. He is otherwise healthy, with no active medical problems. On examination, a large, symmetric, firm, smooth prostate is palpated, but otherwise the exam is normal. Which of the following is a potential complication of the patient's present condition?
A 52-year-old woman with HIV infection is brought to the emergency department 20 minutes after she had a generalized tonic-clonic seizure. She appears lethargic and confused. Laboratory studies show a CD4+ count of 89 cells/μL (N > 500). A CT scan of the head with contrast shows multiple ring-enhancing lesions in the basal ganglia and subcortical white matter. An India ink preparation of cerebrospinal fluid is negative. Which of the following is the most likely diagnosis?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
