Gastroenterology — MCQs

On this page
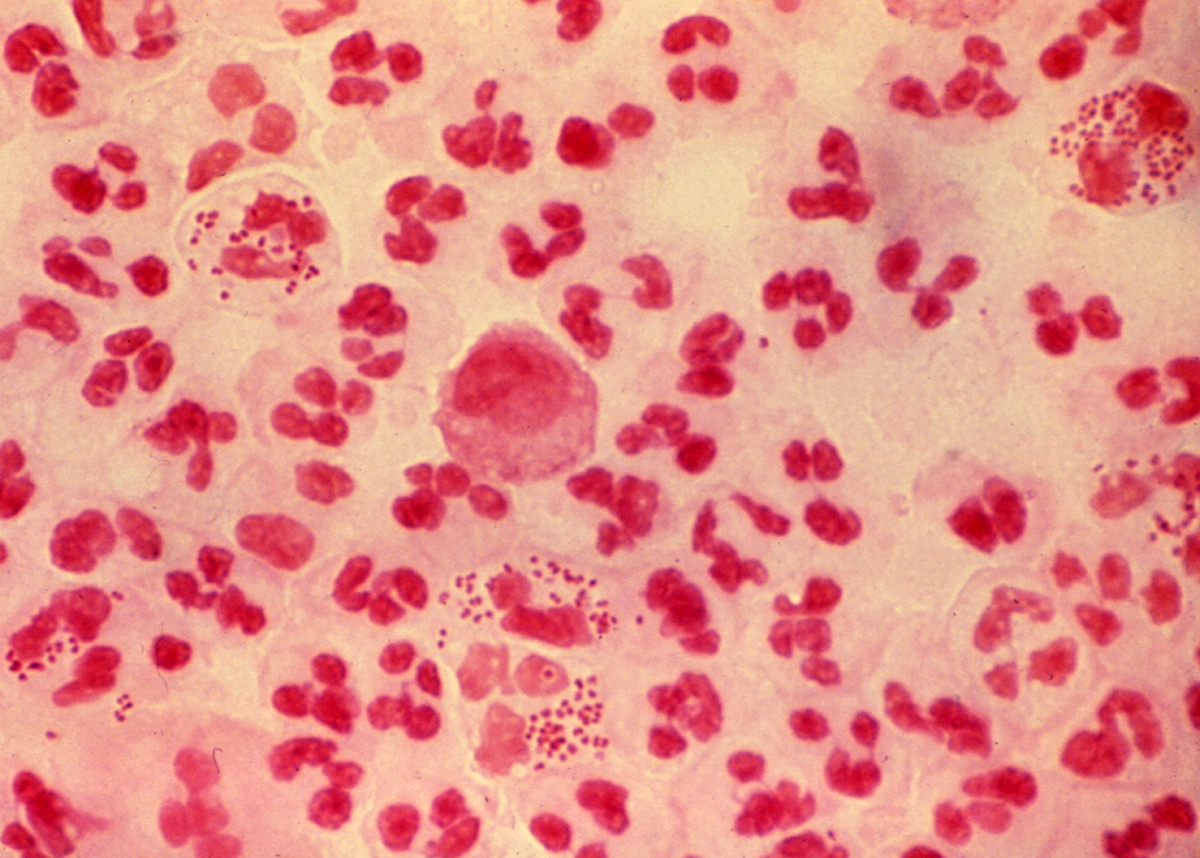
A 33-year-old man is brought to the emergency department by his partner for 24 hours of fever, severe headache, and neck stiffness. His companion also comments that he has been vomiting several times in the past 8 hours and looks confused. His personal medical history is unremarkable. Upon examination, his blood pressure is 125/82 mm Hg, heart rate 110/min, and temperature is 38.9 C (102F). There is no rash or any other skin lesions, his lung sounds are clear and symmetrical. There is nuchal rigidity, jolt accentuation of a headache, and photophobia. A lumbar puncture is taken, and cerebrospinal fluid is sent for analysis and a Gram stain (shown in the picture). The patient is put on empirical antimicrobial therapy with ceftriaxone and vancomycin. According to the clinical manifestations and Gram stain, which of the following should be considered in the management of this case?
A 48-year-old woman presents to the physician because of facial flushing and weakness for 3 months, abdominal discomfort and bloating for 6 months, and profuse watery diarrhea for 1 year. She reports that her diarrhea was episodic initially, but it has been continuous for the past 3 months. The frequency ranges from 10 to 12 bowel movements per day, and the diarrhea persists even if she is fasting. She describes the stools as odorless, watery in consistency, and tea-colored, without blood or mucus. She has not been diagnosed with any specific medical conditions, and there is no history of substance use. Her temperature is 36.9°C (98.4°F), heart rate is 88/min, respiratory rate is 18/min, and blood pressure is 110/74 mm Hg. Her physical exam shows decreased skin turgor, and the abdominal exam does not reveal any significant abnormality. Laboratory studies show: Serum glucose 216 mg/dL (12.0 mmol/L) Serum sodium 142 mEq/L (142 mmol/L) Serum potassium 3.1 mEq/L (3.1 mmol/L) Serum chloride 100 mEq/L (100 mmol/L) Serum calcium 11.1 mg/dL (2.77 mmol/L) Her 24-hour stool volume is 4 liters. Which of the following tests is most likely to yield an accurate diagnosis?
A 67-year-old man comes to the physician because of worsening lower back pain for 6 weeks. He reports that the pain is most intense with movement and that it sometimes occurs at night. Over the past 3 months, he has noticed a weakened urinary stream. He has not seen any blood in his urine. His only daily medication is ibuprofen. Examination shows no spinal deformities. Palpation of the lumbar spinal process elicits tenderness. Muscle strength is normal. Which of the following is the most likely cause of this patient’s back pain?
A 19-year-old man with unknown medical history is found down on a subway platform and is brought to the hospital by ambulance. He experiences two episodes of emesis en route. In the emergency department, he appears confused and is complaining of abdominal pain. His temperature is 37.0° C (98.6° F), pulse is 94/min, blood pressure is 110/80 mmHg, respirations are 24/min, oxygen saturation is 99% on room air. His mucus membranes are dry and he is taking rapid, deep breathes. Laboratory work is presented below: Serum: Na+: 130 mEq/L K+: 4.3 mEq/L Cl-: 102 mEq/L HCO3-: 12 mEq/L BUN: 15 mg/dL Glucose: 362 mg/dL Creatinine: 1.2 mg/dL Urine ketones: Positive The patient is given a bolus of isotonic saline and started on intravenous insulin drip. Which of the following is the most appropriate next step in management?
A 54-year-old woman presents to her primary care physician complaining of watery diarrhea for the last 3 weeks. She reports now having over 10 bowel movements per day. She denies abdominal pain or rash. A basic metabolic profile is notable for the following: Na: 127 mEq/L; K 2.1 mEq/L; Glucose 98 mg/dL. Following additional work-up, octreotide was started with significant improvement in symptoms and laboratory values. Which of the following is the most likely diagnosis?
A previously healthy 31-year-old woman comes to the emergency department because of sudden, severe epigastric pain and vomiting for the past 4 hours. She reports that the pain radiates to the back and began when she was having dinner and drinks at a local brewpub. Her temperature is 37.9°C (100.2°F), pulse is 98/min, respirations are 19/min, and blood pressure is 110/60 mm Hg. Abdominal examination shows epigastric tenderness and guarding but no rebound. Bowel sounds are decreased. Laboratory studies show: Hematocrit 43% Leukocyte count 9000/mm3 Serum Na+ 140 mEq/L K+ 4.5 mEq/L Ca2+ 9.0 mg/dL Lipase 170 U/L (N = < 50 U/L) Amylase 152 U/L Alanine aminotransferase (ALT, GPT) 140 U/L Intravenous fluid resuscitation is begun. Which of the following is the most appropriate next step in management?
A 40-year-old woman presents with ongoing heartburn despite being on treatment for the last few months. She describes a burning sensation in her chest even after small meals. She has stopped eating fatty and spicy foods as they aggravate her heartburn significantly. She has also stopped drinking alcohol but is unable to quit smoking. Her attempts to lose weight have failed. Three months ago, she was started on omeprazole and ranitidine, but she still is having symptoms. She had previously used oral antacids but had to stop because of intolerable constipation. Past medical history is significant for a mild cough for the past several years. Her vital signs are pulse 90/min, blood pressure 120/67 mm Hg, respiratory rate 14/min, and temperature of 36.7°C (98.0°F). Her current BMI is 26 kg/m2. Her teeth are yellow-stained, but the physical examination is otherwise unremarkable. What is the next best step in her management?
A 38-year-old woman presents with dysphagia. She says the dysphagia is worse for solids than liquids and is progressive. She also complains of associated weakness, fatigue, and dyspnea. The patient denies any recent history of weight loss. Laboratory findings are significant for a hemoglobin of 8.7 g/dL. A peripheral blood smear shows evidence of microcytic hypochromic anemia. Which of the following is the most likely cause of her dysphagia?
A 50-year-old woman comes to the physician for a routine health maintenance examination. She has no personal or family history of serious illness. She smoked one pack of cigarettes daily for 5 years during her 20s. Her pulse is 70/min, and blood pressure is 120/78 mm Hg. Serum lipid studies and glucose concentration are within the reference ranges. Which of the following health maintenance recommendations is most appropriate at this time?
A 72-year-old man presents to the emergency department when he discovered a large volume of blood in his stool. He states that he was going to the bathroom when he saw a large amount of bright red blood in the toilet bowl. He was surprised because he did not feel pain and felt it was a normal bowel movement. The patient has a past medical history of diabetes, obesity, hypertension, anxiety, fibromyalgia, diabetic nephropathy, and schizotypal personality disorder. His current medications include atorvastatin, lisinopril, metformin, insulin, clonazepam, gabapentin, sodium docusate, polyethylene glycol, fiber supplements, and ibuprofen. His temperature is 99.5°F (37.5°C), blood pressure is 132/84 mmHg, pulse is 80/min, respirations are 11/min, and oxygen saturation is 96% on room air. On physical exam, the patient's cardiac exam reveals a normal rate and rhythm, and his pulmonary exam is clear to auscultation bilaterally. Abdominal exam is notable for an obese abdomen without tenderness to palpation. Which of the following is an appropriate treatment for this patient's condition?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
