Gastroenterology — MCQs

On this page
A 41-year-old man presents to the emergency department because of brownish discoloration of his urine for the last several days. The review of symptoms includes complaints of increasing abdominal girth, early satiety, and difficulty breathing on exertion. The past medical history includes essential hypertension for 19 years. The medication list includes lisinopril and hydrochlorothiazide. He had a right inguinal hernia repair when he was a teenager. He smokes 20–30 cigarettes daily for the last 21 years, and drinks alcohol socially. His father died of a hemorrhagic stroke at the age of 69 years. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 131/88 mm Hg, and pulse 82/min. The physical examination is positive for a palpable right upper quadrant mass. The abdominal ultrasound shows multiple bilateral kidney cysts and hepatic cysts. Which of the following is the most likely diagnosis?
A 75-year-old man comes to the physician because of a 3-month history of upper abdominal pain, nausea, and sensation of early satiety. He has also had a 9.4-kg (20.7-lb) weight loss over the past 4 months. He has osteoarthritis. He drinks two beers every night with dinner. His only medication is ibuprofen. Esophagogastroduodenoscopy shows an ulcerated mass in the lesser curvature of the stomach. A biopsy specimen obtained during endoscopy shows irregular-shaped tubules with intraluminal mucus and debris. Which of the following is the most likely predisposing factor for this patient's condition?
A 72-year-old male with a past medical history significant for aortic stenosis and hypertension presents to the emergency department complaining of weakness for the past 3 weeks. He states that, apart from feeling weaker, he also has noted lightheadedness, pallor, and blood-streaked stools. The patient's vital signs are stable, and he is in no acute distress. Laboratory workup reveals that the patient is anemic. Fecal occult blood test is positive for bleeding. EGD was performed and did not reveal upper GI bleeding. Suspecting a lower GI bleed, a colonoscopy is performed after prepping the patient, and it is unremarkable. What would be an appropriate next step for localizing a lower GI bleed in this patient?
A 53-year-old woman is brought to the emergency department because of an episode of lightheadedness and left arm weakness for the last hour. Her symptoms were preceded by tremors, palpitations, and diaphoresis. During the past 3 months, she has had increased appetite and has gained 6.8 kg (15 lbs). She has hypertension, hyperlipidemia, anxiety disorder, and gastroesophageal reflux. She works as a nurse in an ICU and has been under more stress than usual. She does not smoke. She drinks 5 glasses of wine every week. Current medications include enalapril, atorvastatin, fluoxetine, and omeprazole. She is 168 cm (5 ft 6 in) tall and weighs 100 kg (220 lb); BMI is 36 kg/m2. Her temperature is 37°C (98.8°F), pulse is 78/min, and blood pressure is 130/80 mm Hg. Cardiopulmonary examination shows no abnormalities. The abdomen is soft and nontender. Fasting serum studies show: Na+ 140 mEq/L K+ 3.5 mEq/L HCO3- 22 mEq/L Creatinine 0.8 mg/dL Glucose 37 mg/dL Insulin 280 μU/mL (N=11–240) Thyroid-stimulating hormone 2.8 μU/mL C-peptide 4.9 ng/mL (N=0.8–3.1) Urine screen for sulfonylurea is negative. Which of the following is the most likely diagnosis?
A 28-year-old man presents with one week of redness and discharge in his eyes, pain and swelling in his left second and third toes, and rash on the soles of his feet. He is sexually active with multiple partners and uses condoms occasionally. He denies any recent travel or illness and does not take any medications. Review of systems is otherwise unremarkable. On physical exam, he has bilateral conjunctivitis, dactylitis of the left second and third toes, and crusty yellow-brown vesicles on his plantar feet. Complete blood count and chemistries are within normal limits. Erythrocyte sedimentation rate (ESR) is 40 mm/h. Toe radiographs demonstrate soft tissue swelling but no fractures. Which diagnostic test should be performed next?
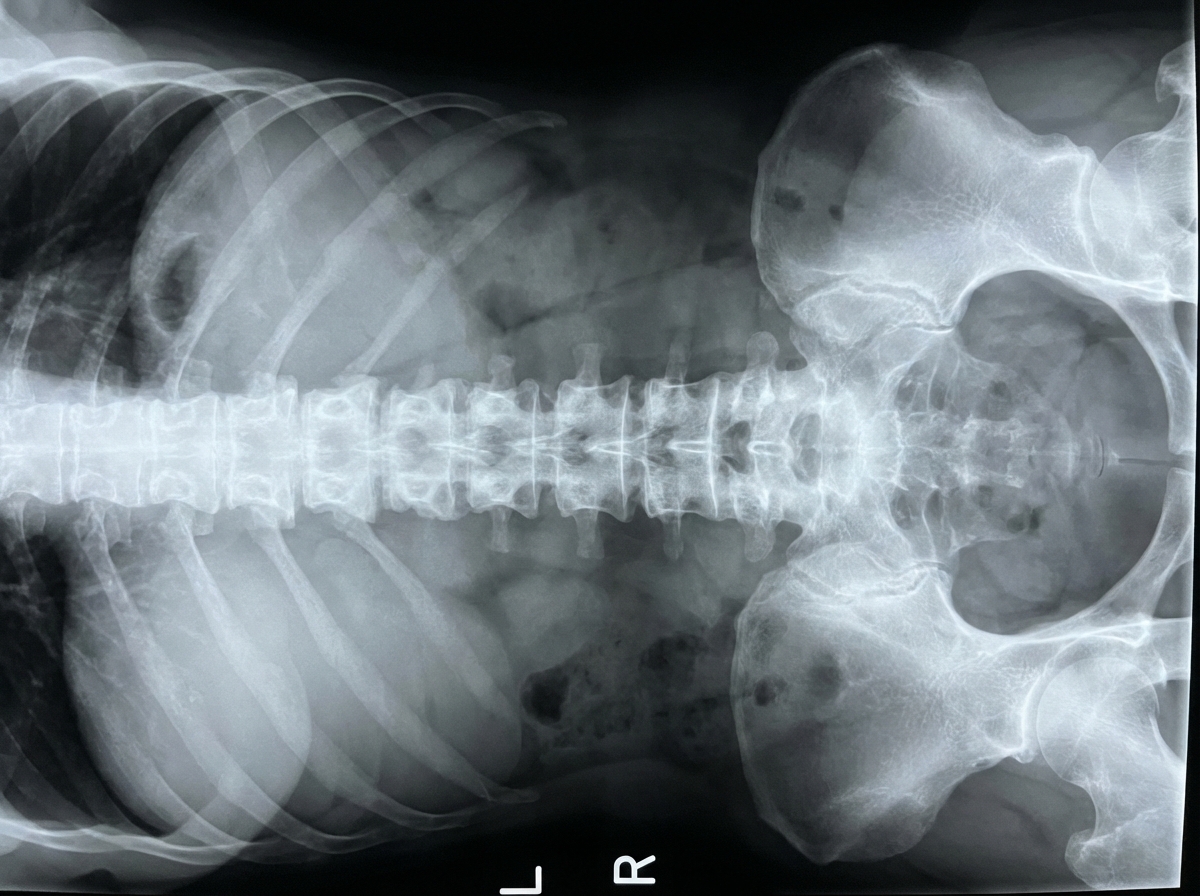
A 32-year-old man presents to the clinic with a dull low back pain radiating to the buttocks. He first noted it about 2 years ago and it has progressed since then. He notes that it is worse in the morning and improves later in the day after physical activity. The patient also reports morning stiffness lasting up to 30 minutes and blurred vision, which started about 7 months ago. The patient's vital signs include: blood pressure 130/80 mm Hg, heart rate 88/min, respiratory rate 16/min, and temperature 36.8°C (98.2°F). Physical examination reveals tenderness over the sacroiliac joints and limitation of the lumbar spine movements in the sagittal plane. The patient's X-ray is shown in the picture below. Which of the following HLA variants is associated with this patient's condition?
A 45-year-old man presents to his primary care physician because of abdominal pain. He has had this pain intermittently for several years but feels that it has gotten worse after he started a low carbohydrate diet. He says that the pain is most prominent in the epigastric region and is also associated with constipation and foul smelling stools that float in the toilet bowl. He has a 15-year history of severe alcoholism but quit drinking 1 year ago. Laboratory studies are obtained showing a normal serum amylase and lipase. Both serum and urine toxicology are negative. His physician starts him on appropriate therapy and checks to make sure that his vitamin and mineral levels are appropriate. Which of the following deficiency syndromes is most closely associated with the cause of this patient's abdominal pain?
A 60-year-old man has had intermittent pain in his right great toe for the past 2 years. Joint aspiration and crystal analysis shows thin, tapered, needle shaped intracellular crystals that are strongly negatively birefringent. Radiograph demonstrates joint space narrowing of the 1st metatarsophalangeal (MTP) joint with medial soft tissue swelling. What is the most likely cause of this condition?
A 67-year-old woman presents to the clinic with a 9-month history of seeing bright red blood in the toilet after defecating. Additional complaints include fatigue, shortness of breath, and mild lethargy. She denies the loss of weight, abdominal pain, or changes in dietary behavior. She consumes a balanced diet and takes multiple vitamins every day. The current vital signs include the following: temperature is 37.0°C (98.6°F), pulse rate is 68/min, blood pressure is 130/81 mm Hg, and the respiratory rate is 13/min. On physical examination, you notice increased capillary refill time and pale mucosa. What are the most likely findings for hemoglobin, hematocrit, red blood cell count, and mean corpuscular volume?
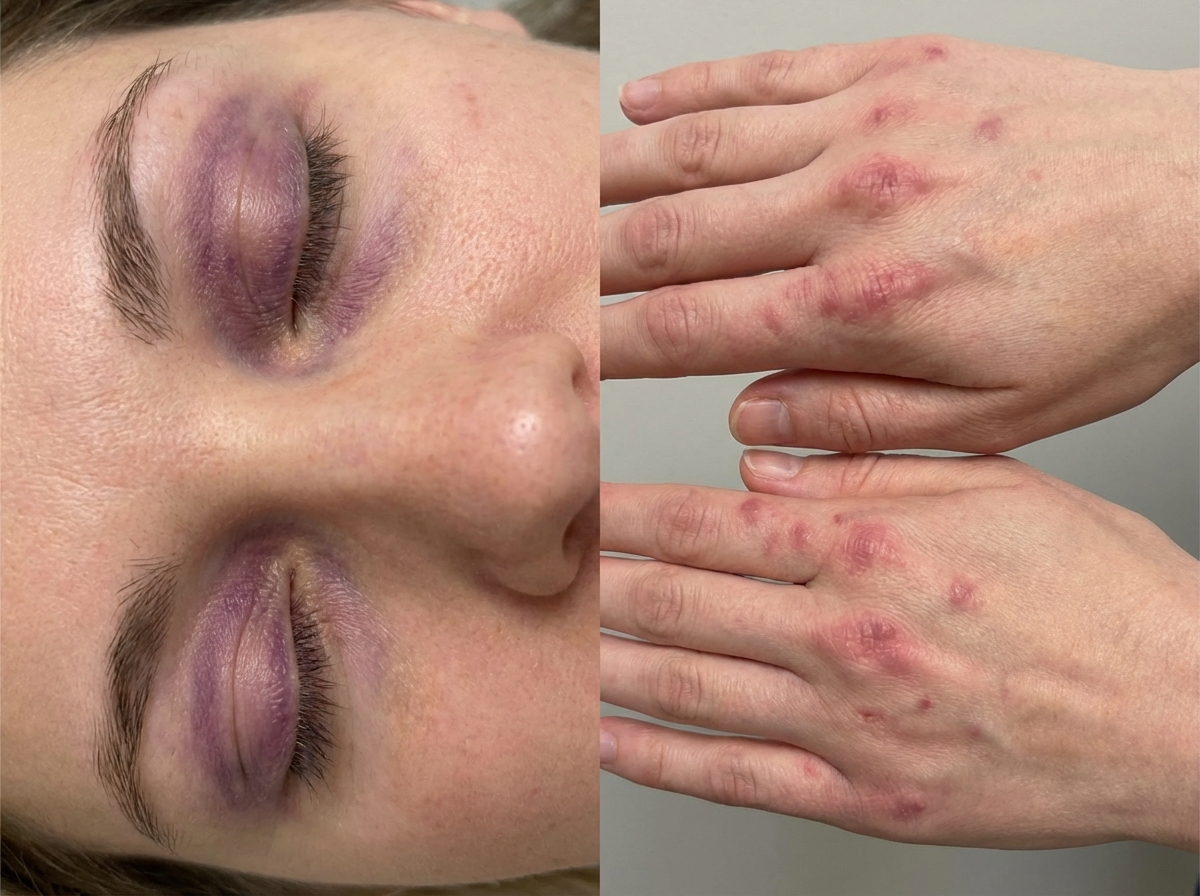
A 35-year-old woman presents for evaluation of symmetric proximal muscle weakness. The patient also presents with a blue-purple discoloration of the upper eyelids accompanied by rashes on the knuckles, as shown in the picture below. What is the most likely cause?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
