Gastroenterology — MCQs

On this page
A 60-year-old patient presents to the urgent care clinic with complaints of pain and abdominal distention for the past several weeks. The pain began with a change in bowel habits 3 months ago, and he gradually defecated less until he became completely constipated, which led to increasing pain and distention. He also mentions that he has lost weight during this period, even though he has not changed his diet. When asked about his family history, the patient reveals that his brother was diagnosed with colorectal cancer at 65 years of age. An abdominal radiograph and CT scan were done which confirmed the diagnosis of obstruction. Which of the following locations in the digestive tract are most likely involved in this patient’s disease process?
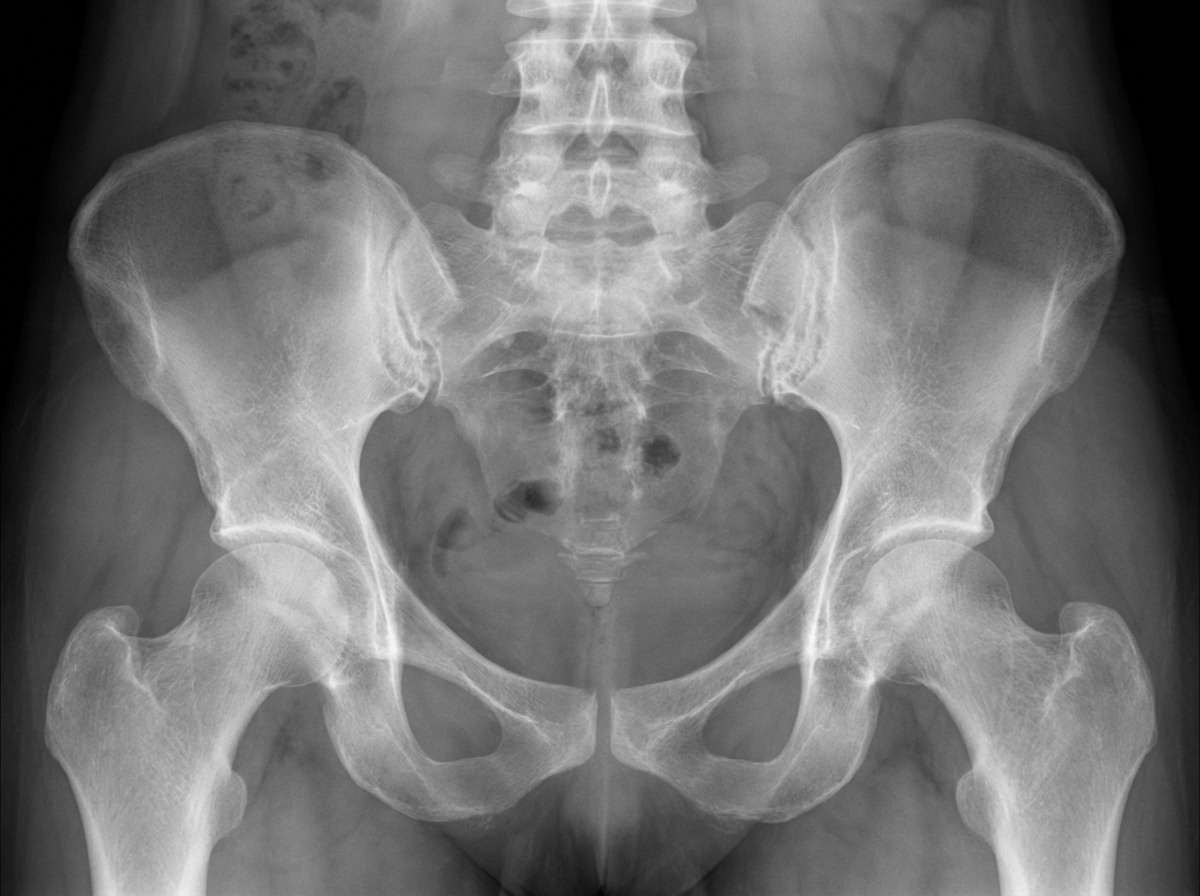
A 32-year-old woman comes to her physician because of increasing back pain for the past 10 months. The pain is worse in the morning when she wakes up and improves with activity. She used to practice yoga, but stopped 5 months ago as bending forward became increasingly difficult. She has also had bilateral hip pain for the past 4 months. She has not had any change in urination. She has celiac disease and eats a gluten-free diet. Her temperature is 37.1°C (98.8°F), pulse is 65/min, respirations are 13/min, and blood pressure is 116/72 mmHg. Examination shows the range of spinal flexion is limited. Flexion, abduction, and external rotation of bilateral hips produces pain. An x-ray of her pelvis is shown. Further evaluation of this patient is likely to show which of the following?
A 25-year-old woman presents to a physician for a new patient physical exam. Aside from occasional shin splints, she has a relatively unremarkable medical history. She takes oral contraceptive pills as scheduled and a multivitamin daily. She reports no known drug allergies. All of her age appropriate immunizations are up to date. Her periods have been regular, occurring once every 28 to 30 days with normal flow. She is sexually active with two partners, who use condoms routinely. She works as a cashier at the local grocery store. Her mother has diabetes and coronary artery disease, and her father passed away at age 45 after being diagnosed with colon cancer at age 40. Her grand-aunt underwent bilateral mastectomies after being diagnosed with breast cancer at age 60. Her physical exam is unremarkable. Which of the following is the best recommendation for this patient?
A 38-year-old man comes to the physician because of progressive pain and swelling of his left knee for the past 2 days. He has been taking ibuprofen for the past 2 days without improvement. Four days ago, he scraped his left knee while playing baseball. He has a 2-month history of progressive pain and stiffness in his back. The pain starts after waking up and lasts for 20 minutes. He has type 2 diabetes mellitus. His older sister has rheumatoid arthritis. He is 170 cm (5 ft 7 in) tall and weighs 91 kg (201 lb); BMI is 31.5 kg/m2. Temperature is 39°C (102.2°F), pulse is 90/min, and blood pressure is 135/85 mm Hg. Examination shows an erythematous, tender, and swollen left knee; range of motion is limited. There are abrasions over the lateral aspect of the left knee. The remainder of the examination shows no abnormalities. Laboratory studies show a leukocyte count of 13,500/mm3 and an erythrocyte sedimentation rate of 70 mm/h. Which of the following is the most appropriate next step in management?
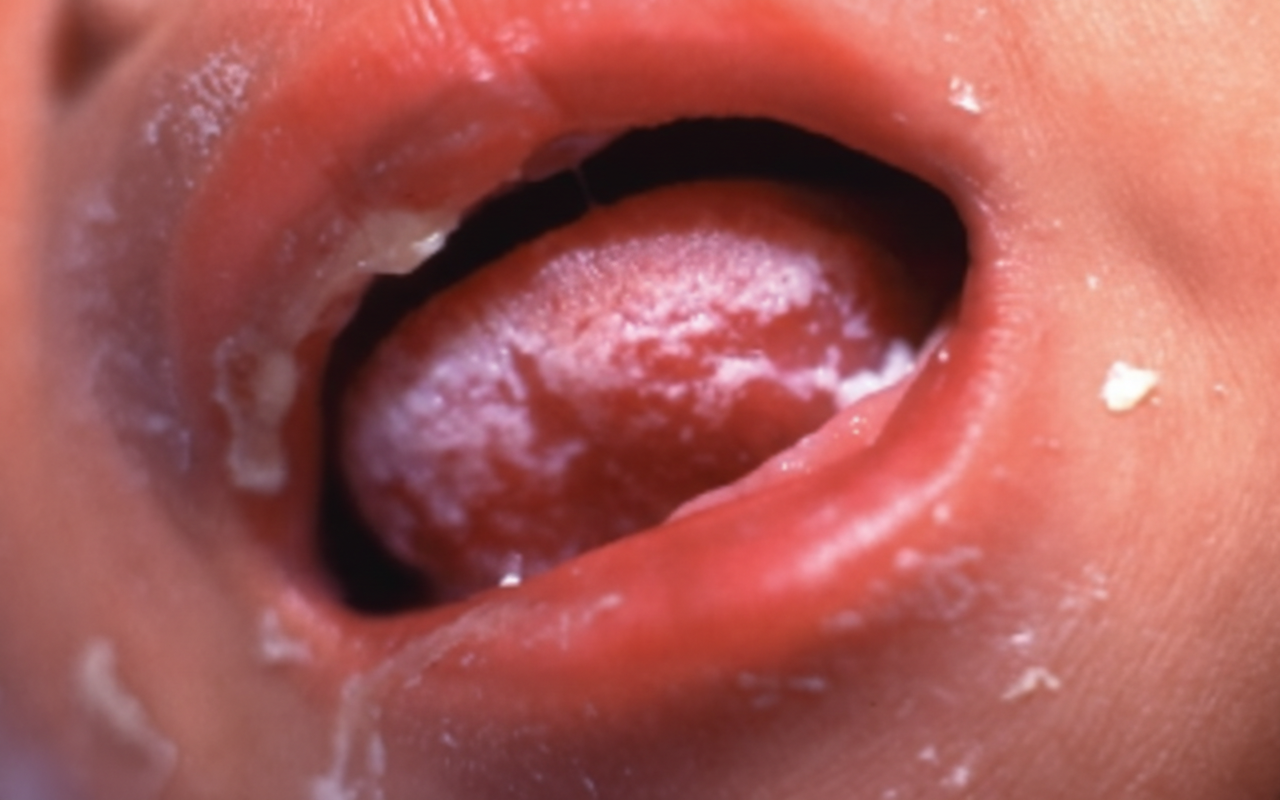
A 36-year-old man presents with soreness and dryness of the oral mucosa for the past 3 weeks. No significant past medical history. The patient reports that he has had multiple bisexual partners over the last year and only occasionally uses condoms. He denies any alcohol use or history of smoking. The patient is afebrile and his vital signs are within normal limits. On physical examination, there is a lesion noted in the oral cavity, which is shown in the exhibit. Which of the following is the next best step in the treatment of this patient?
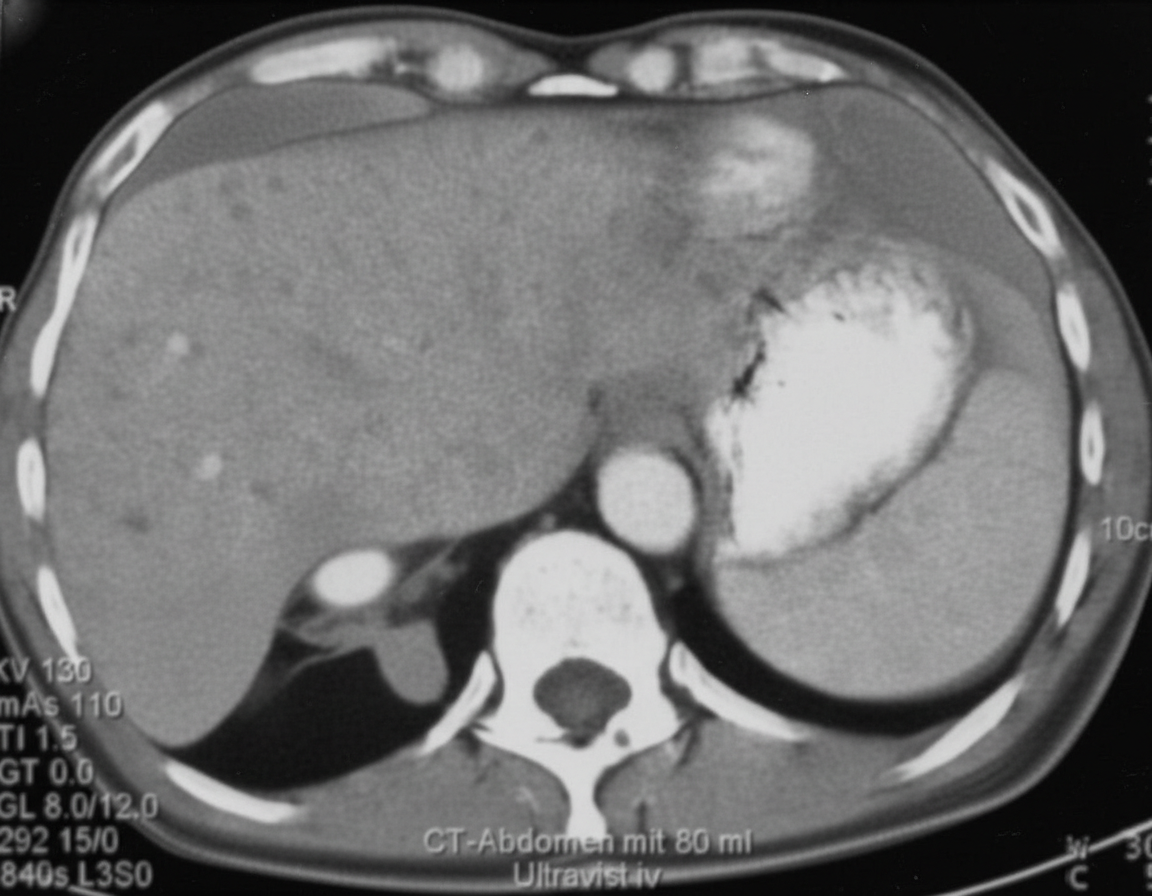
A 64-year-old woman comes to the physician because of a 7.2-kg (16-lb) weight loss over the past 6 months. For the last 4 weeks, she has also had intermittent constipation and bloating. Four months ago, she spent 2 weeks in Mexico with her daughter. She has never smoked. She drinks one glass of wine daily. She appears thin. Her temperature is 38.3°C (101°F), pulse is 80/min, and blood pressure is 136/78 mm Hg. The lungs are clear to auscultation. The abdomen is distended and the liver is palpable 4 cm below the right costal margin with a hard, mildly tender nodule in the left lobe. Test of the stool for occult blood is positive. Serum studies show: Alkaline phosphatase 67 U/L AST 65 U/L ALT 68 U/L Hepatitis B surface antigen negative Hepatitis C antibody negative A contrast-enhanced CT scan of the abdomen is shown. Which of the following is the most likely diagnosis?
A 76-year-old man presents after an acute onset seizure. He lives in a retirement home and denies any previous history of seizures. Past medical history is significant for a hemorrhagic stroke 4 years ago, and type 2 diabetes, managed with metformin. His vital signs include: blood pressure 80/50 mm Hg, pulse 80/min, and respiratory rate 19/min. On physical examination, the patient is lethargic. Mucous membranes are dry. A noncontrast CT of the head is performed and is unremarkable. Laboratory findings are significant for the following: Plasma glucose 680 mg/dL pH 7.37 Serum bicarbonate 17 mEq/L Effective serum osmolality 350 mOsm/kg Urinary ketone bodies negative Which of the following was the most likely trigger for this patient’s seizure?
A 70-year-old woman is brought to the emergency department 1 hour after being found unconscious in her apartment by her neighbor. No medical history is currently available. Her temperature is 37.2°C (99.0°F), pulse is 120/min, respirations are 18/min, and blood pressure is 70/50 mm Hg. Physical examination reveals dry mucous membranes and poor skin turgor. The neighbor mentions that the patient had been complaining of severe diarrhea for the past 2 days. Laboratory studies show a glomerular filtration rate of 70 mL/min/1.73 m2 (N > 90) and an increased filtration fraction. Which of the following is the most likely cause of this patient's findings?
A 24-year-old woman with 45,X syndrome comes to the physician because of diarrhea for 4 months. She also reports bloating, nausea, and abdominal discomfort that persists after defecation. For the past 6 months, she has felt tired and has been unable to do her normal chores. She went on a backpacking trip across Southeast Asia around 7 months ago. She is 144 cm (4 ft 9 in) tall and weighs 40 kg (88 lb); BMI is 19 kg/m2. Her blood pressure is 110/60 mm Hg in the upper extremities and 80/40 mm Hg in the lower extremities. Examination shows pale conjunctivae and angular stomatitis. Abdominal examination is normal. Laboratory studies show: Hemoglobin 9.1 mg/dL Leukocyte count 5100/mm3 Platelet count 200,000/mm3 Mean corpuscular volume 67 μmm3 Serum Na+ 136 mEq/L K+ 3.7 mEq/L Cl- 105 mEq/L Glucose 89 mg/dL Creatinine 1.4 mg/dL Ferritin 10 ng/mL IgA tissue transglutaminase antibody positive Based on the laboratory studies, a biopsy for confirmation of the diagnosis is suggested, but the patient is unwilling to undergo the procedure. Which of the following is the most appropriate next step in management of this patient's gastrointestinal symptoms?
A 30-year-old male visits you in the clinic complaining of chronic abdominal pain and diarrhea following milk intake. Gastrointestinal histology of this patient's condition is most similar to which of the following?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
