Gastroenterology — MCQs

On this page
A 45-year-old man comes to the physician because of severe left knee pain and swelling. He has hypercholesterolemia and hypertension. Current medications include pravastatin and captopril. He eats a low-fat diet that includes fish and leafy green vegetables. He drinks 4–6 cups of coffee daily. He has smoked one pack of cigarettes daily for 26 years and drinks 2–3 beers daily. Vital signs are within normal limits. Examination of the left knee shows swelling, warmth, and severe tenderness to palpation. Arthrocentesis is performed. Gram stain is negative. Analysis of the synovial fluid shows monosodium urate crystals. Which of the following health maintenance recommendations is most appropriate to prevent symptom recurrence?
A 33-year-old man presents with a darkening of the skin on his neck over the past month. Past medical history is significant for primary hypothyroidism treated with levothyroxine. His vital signs include: blood pressure 130/80 mm Hg, pulse 84/min, respiratory rate 18/min, temperature 36.8°C (98.2°F). His body mass index is 35.3 kg/m2. Laboratory tests reveal a fasting blood glucose of 121 mg/dL and a thyroid-stimulating hormone level of 2.8 mcU/mL. The patient’s neck is shown in the exhibit. Which of the following is the best initial treatment for this patient?
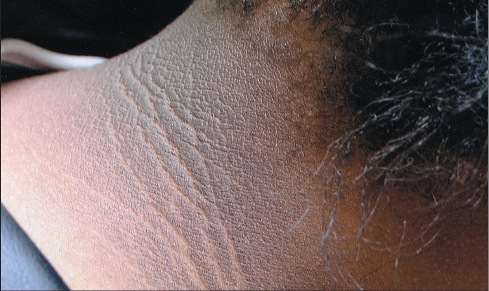
A 33-year-old man presents to the emergency department with back pain. He is currently intoxicated but states that he is having severe back pain and is requesting morphine and lorazepam. The patient has a past medical history of alcohol abuse, drug seeking behavior, and IV drug abuse and does not routinely see a physician. His temperature is 102°F (38.9°C), blood pressure is 127/68 mmHg, pulse is 120/min, respirations are 17/min, and oxygen saturation is 98% on room air. Physical exam is notable for tenderness over the thoracic and lumbar spine. The pain is exacerbated with flexion of the spine. The patient’s laboratory values are notable for the findings below. Hemoglobin: 12 g/dL Hematocrit: 36% Leukocyte count: 16,500/mm^3 with normal differential Platelet count: 197,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 1.1 mg/dL Ca2+: 10.2 mg/dL CRP: 5.2 mg/L Further imaging is currently pending. Which of the following is the most likely diagnosis?
A 35-year-old male with a history of hypertension presents with hematuria and abdominal discomfort. Ultrasound and CT scan reveal large, bilateral cysts in all regions of the kidney. What is the most likely diagnosis?
A 63-year-old man presents to the emergency department complaining of sudden-onset severe dyspnea and right-sided chest pain. The patient has a history of chronic obstructive pulmonary disease, hypertension, peptic ulcer disease, and hyperthyroidism. He has smoked a pack of cigarettes daily for 20 years, drinks socially, and does not take illicit drugs. The blood pressure is 130/80 mm Hg, the pulse is 98/min and regular, and the respiratory rate is 20/min. Pulse oximetry shows 90% on room air. On physical examination, he is in mild respiratory distress. Tactile fremitus and breath sounds are decreased on the right, with hyperresonance on percussion. The trachea is midline and no heart murmurs are heard. Which of the following is the most likely underlying mechanism of this patient's current condition?
A 57-year-old man presents with an ongoing asymptomatic rash for 2 weeks. A similar rash is seen in both axillae. He has a medical history of diabetes mellitus for 5 years and dyspepsia for 6 months. His medications include metformin and aspirin. His vital signs are within normal limits. His BMI is 29 kg/m2. The physical examination shows conjunctival pallor. The cardiopulmonary examination reveals no abnormalities. The laboratory test results are as follows: Hemoglobin 9 g/dL Mean corpuscular volume 72 μm3 Platelet count 469,000/mm3 Red cell distribution width 18% HbA1C 6.5% Which of the following is the most likely underlying cause of this patient’s condition?
A 65-year-old patient presents with acute left lower quadrant abdominal pain and is diagnosed with diverticulitis. Which of the following is most likely to have prevented this patient's condition?
A 47-year-old woman comes to the physician because of progressive pain and stiffness in her hands and wrists for the past several months. Her hands are stiff in the morning; the stiffness improves as she starts her chores. Physical examination shows bilateral swelling and tenderness of the wrists, metacarpophalangeal joints, and proximal interphalangeal joints. Her range of motion is limited by pain. Laboratory studies show an increased erythrocyte sedimentation rate. This patient's condition is most likely associated with which of the following findings?
A 69-year-old man presents with progressive dysphagia and a 5-kg weight loss over 3 months. Initially, he had difficulty swallowing solids, which progressed to include liquids in the past week. Endoscopy reveals a mass 3 cm proximal to the esophagogastric junction. Biopsy shows significant distortion of glandular architecture, consistent with adenocarcinoma. Which of the following is the strongest risk factor for this patient's likely diagnosis?
A 6-year-old girl with no significant past medical, surgical, social, or family history presents to urgent care for a new itchy rash on the fingers of her right hand. When questioned, the patient notes that she recently received a pair of beloved silver rings from her aunt as a birthday present. She denies any history of similar rashes. The patient's blood pressure is 123/76 mm Hg, pulse is 67/min, respiratory rate is 16/min, and temperature is 37.3°C (99.1°F). Physical examination reveals erythematous scaly plaques at the base of her right middle and ring finger. What metal alloy is most likely contained within the patient’s new rings?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
