Gastroenterology — MCQs

On this page
An adult female presents with pallor and fatigue. Blood investigations show low hemoglobin ( Hb ), low serum iron, low ferritin, low transferrin saturation, and increased total iron-binding capacity (TIBC). What is the likely diagnosis?
Which of the following is typically observed in the investigation results for a patient with iron deficiency anemia (IDA)?
Which of the following antibodies is associated with Celiac disease?
An endoscopic image shows the following finding. What is the most likely diagnosis?
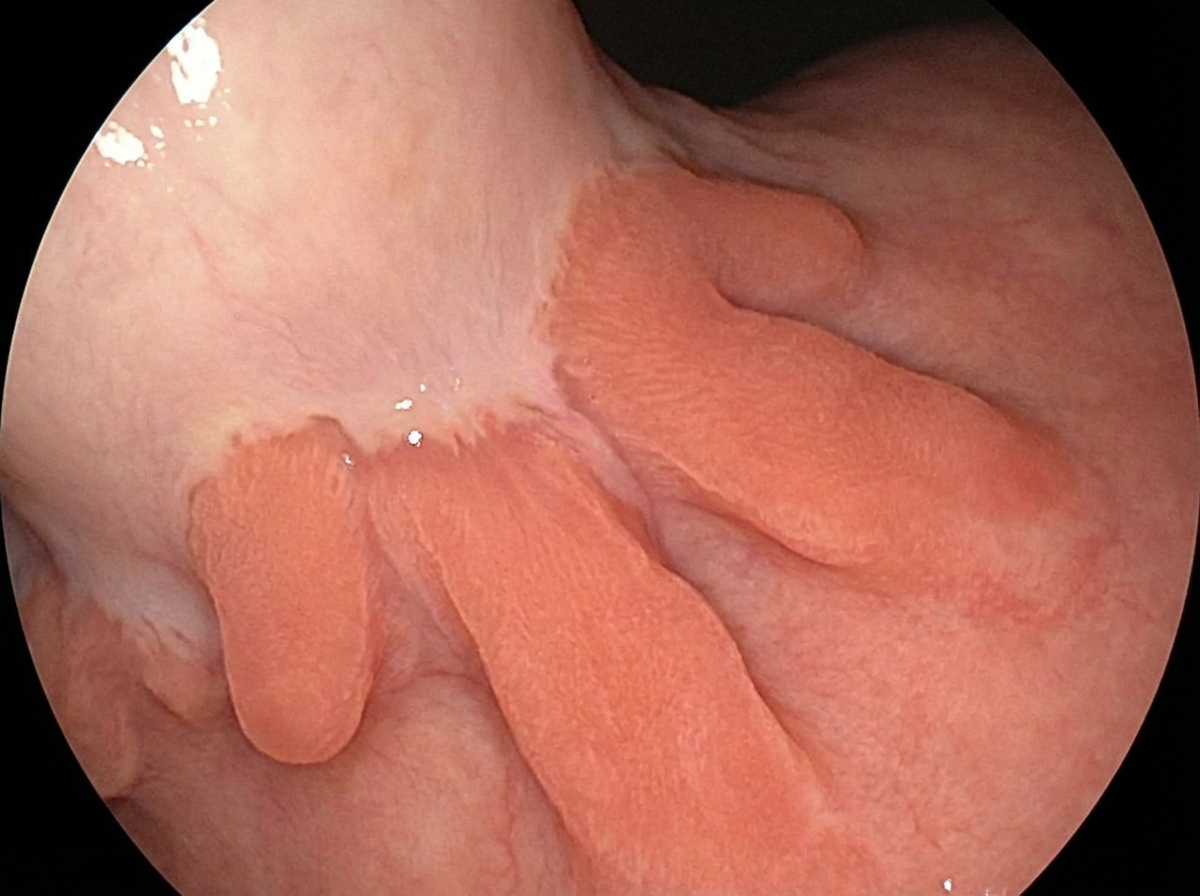
A female engineer works for 12-14 hours a day and reports consuming only fast food, with no vegetables or fruits in her diet. Her hemoglobin (Hb) count is $9 \mathrm{~g} / \mathrm{dL}$, and her mean corpuscular volume (MCV) is 120 fL . Peripheral smear (PS) shows the presence of macrocytes. What is the most likely diagnosis?
A 71-year-old man presents to the emergency department because of blood in his stool. The patient states that he is not experiencing any pain during defecation and is without pain currently. The patient recently returned from a camping trip where he consumed meats cooked over a fire pit and drank water from local streams. The patient has a past medical history of obesity, diabetes, constipation, irritable bowel syndrome, ulcerative colitis that is in remission, and a 70 pack-year smoking history. The patient has a family history of breast cancer in his mother and prostate cancer in his father. His temperature is 98.9°F (37.2°C), blood pressure is 160/87 mmHg, pulse is 80/min, respirations are 14/min, and oxygen saturation is 98% on room air. Physical exam is notable for an obese man in no current distress. Abdominal exam reveals a non-tender and non-distended abdomen with normal bowel sounds. An abdominal radiograph and barium swallow are within normal limits. Assuming appropriate diagnostic workup identifies the most likely cause of his symptoms, which of the following would be the most appropriate treatment?
A 43-year-old man comes to the physician because of a 2-week history of nonbloody diarrhea, abdominal discomfort, and bloating. When the symptoms began, several of his coworkers had similar symptoms but only for about 3 days. Abdominal examination shows diffuse tenderness with no guarding or rebound. Stool sampling reveals a decreased stool pH. Which of the following is the most likely underlying cause of this patient's prolonged symptoms?
A 45-year-old man presents to the emergency department with upper abdominal pain. He reports vomiting blood 2 times at home. He has smoked 30–40 cigarettes daily for 15 years. He is otherwise well, takes no medications, and abstains from the use of alcohol. While in the emergency department, he vomits bright red blood into a bedside basin and becomes light-headed. Blood pressure is 86/40 mm Hg, pulse 120/min, and respiratory rate 24/min. His skin is cool to touch, pale, and mottled. Which of the following is a feature of this patient’s condition?
A 68-year-old man comes to the physician for a routine health maintenance examination. Over the past six months, he has had an increase in the frequency of his bowel movements and occasional bloody stools. He has hypertension, coronary artery disease, and chronic obstructive pulmonary disease. He has smoked one pack of cigarettes daily for 40 years. His current medications include aspirin, lisinopril, and salmeterol. His temperature is 37°C (98.6°F), pulse is 75/min, and blood pressure is 128/75 mm Hg. The lungs are clear to auscultation. Cardiac examination shows no murmurs, rubs, or gallops. The abdomen is soft with no organomegaly. Digital rectal examination shows a large internal hemorrhoid. Test of the stool for occult blood is positive. Which of the following is the most appropriate next step in the management of this patient?
A 42-year-old woman presents for a follow-up visit. She was diagnosed with iron deficiency anemia 3 months ago, for which she was prescribed ferrous sulfate twice daily. She says the medication has not helped, and she still is suffering from fatigue and shortness of breath when she exerts herself. Past medical history is remarkable for chronic dyspepsia. The patient denies smoking, drinking alcohol, or use of illicit drugs. She immigrated from Egypt 4 years ago. No significant family history. Physical examination is unremarkable. Laboratory findings are significant for the following: 3 month ago Current Hemoglobin 10.1 g/dL 10.3 g/dL Erythrocyte count 3.2 million/mm3 3.3 million/mm3 Mean corpuscular volume (MCV) 72 μm3 74 μm3 Mean corpuscular hemoglobin (MCH) 20.1 pg/cell 20.3 pg/cell Red cell distribution width (RDW) 17.2% 17.1% Serum ferritin 10.1 ng/mL 10.3 ng/mL Total iron binding capacity (TIBC) 475 µg/dL 470 µg/dL Transferrin saturation 11% 12% Which of the following is the next best step in the management of this patient’s most likely condition?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
