Gastroenterology — MCQs

On this page
A 54-year-old man comes to the physician for the evaluation of difficulty swallowing of both solids and liquids for 1 month. During the past 5 months, he has also had increased weakness of his hands and legs. He sails regularly and is unable to hold the ropes as tightly as before. Ten years ago, he was involved in a motor vehicle collision. Examination shows atrophy of the tongue. Muscle strength is decreased in the right upper and lower extremities. There is muscle stiffness in the left lower extremity. Deep tendon reflexes are 1+ in the right upper and lower extremities, 3+ in the left upper extremity, and 4+ in the left lower extremity. Plantar reflex shows an extensor response on the left foot. Sensation to light touch, pinprick, and vibration is intact. Which of the following is the most likely diagnosis?
A 77-year-old woman, gravida 2, para 2, is brought to the physician by staff of the nursing home where she resides because of involuntary loss of urine and increased frequency of urination over the past 2 weeks. She reports that she has very little time to get to the bathroom after feeling the urge to urinate. “Accidents” have occurred 4–6 times a day during this period. She has never had urinary incontinence before. She has also been more tired than usual. She drinks 3 cups of coffee daily. Her last menstrual period was 15 years ago. She takes no medications. Vital signs are within normal limits. The abdomen is soft and nontender. Pelvic examination shows a normal-appearing vagina and cervix; uterus and adnexa are small. Which of the following is the most appropriate next step in management?
A 42-year-old woman comes to the physician for a follow-up appointment. Two months ago, she was diagnosed with asthma after a 1-year history of a chronic cough and dyspnea with exertion. Her symptoms have improved since starting inhaled albuterol and beclomethasone, but she still coughs most nights when she is lying in bed. Over the past 2 weeks, she has also had occasional substernal chest pain. She does not smoke. She is 158 cm (5 ft 2 in) tall and weighs 75 kg (165 lb); BMI is 30 kg/m2. Vital signs are within normal limits. She has a hoarse voice and frequently clears her throat during the examination. The lungs are clear to auscultation. Pulmonary function tests show a FEV1 of 78% of expected. Which of the following is the most appropriate next step in management?
A 38-year-old man comes to the physician because of an 8-month history of upper abdominal pain. During this period, he has also had nausea, heartburn, and multiple episodes of diarrhea with no blood or mucus. He has smoked one pack of cigarettes daily for the past 18 years. He does not use alcohol or illicit drugs. Current medications include an antacid. The abdomen is soft and there is tenderness to palpation in the epigastric and umbilical areas. Upper endoscopy shows several ulcers in the duodenum and the upper jejunum as well as thick gastric folds. Gastric pH is < 2. Biopsies from the ulcers show no organisms. Which of the following tests is most likely to confirm the diagnosis?
A 42-year-old man presents to clinic complaining of increasing difficulty climbing stairs and standing up from sitting in his chair. On exam you perceive his strength to be 5/5 distally, but only 3/5 in proximal muscle groups bilaterally. There is a distinctive rash on his upper eyelids and around his eyes. Examination of the fingers is most likely to reveal which of the following?
A 62-year-old man comes to the office complaining of dysphagia that started 4-5 months ago. He reports that he initially had difficulty swallowing only solid foods. More recently, he has noticed some trouble swallowing liquids. The patient also complains of fatigue, a chronic cough that worsens at night, and burning chest pain that occurs after he eats. He says that he has used over-the-counter antacids for "years" with mild relief. He denies any change in diet, but says he has "gone down a pant size or 2." The patient has hypertension and hyperlipidemia. He takes amlodipine and atorvastatin. He smoked 1 pack of cigarettes a day for 12 years while in the military but quit 35 years ago. He drinks 1-2 beers on the weekend while he is golfing with his friends. His diet consists mostly of pasta, pizza, and steak. The patient's temperature is 98°F (36.7°C), blood pressure is 143/91 mmHg, and pulse is 80/min. His BMI is 32 kg/m^2. Physical examination reveals an obese man in no acute distress. No masses or enlarged lymph nodes are appreciated upon palpation of the neck. Cardiopulmonary examination is unremarkable. An endoscopy is performed, which identifies a lower esophageal mass. Which of the following is the most likely diagnosis?
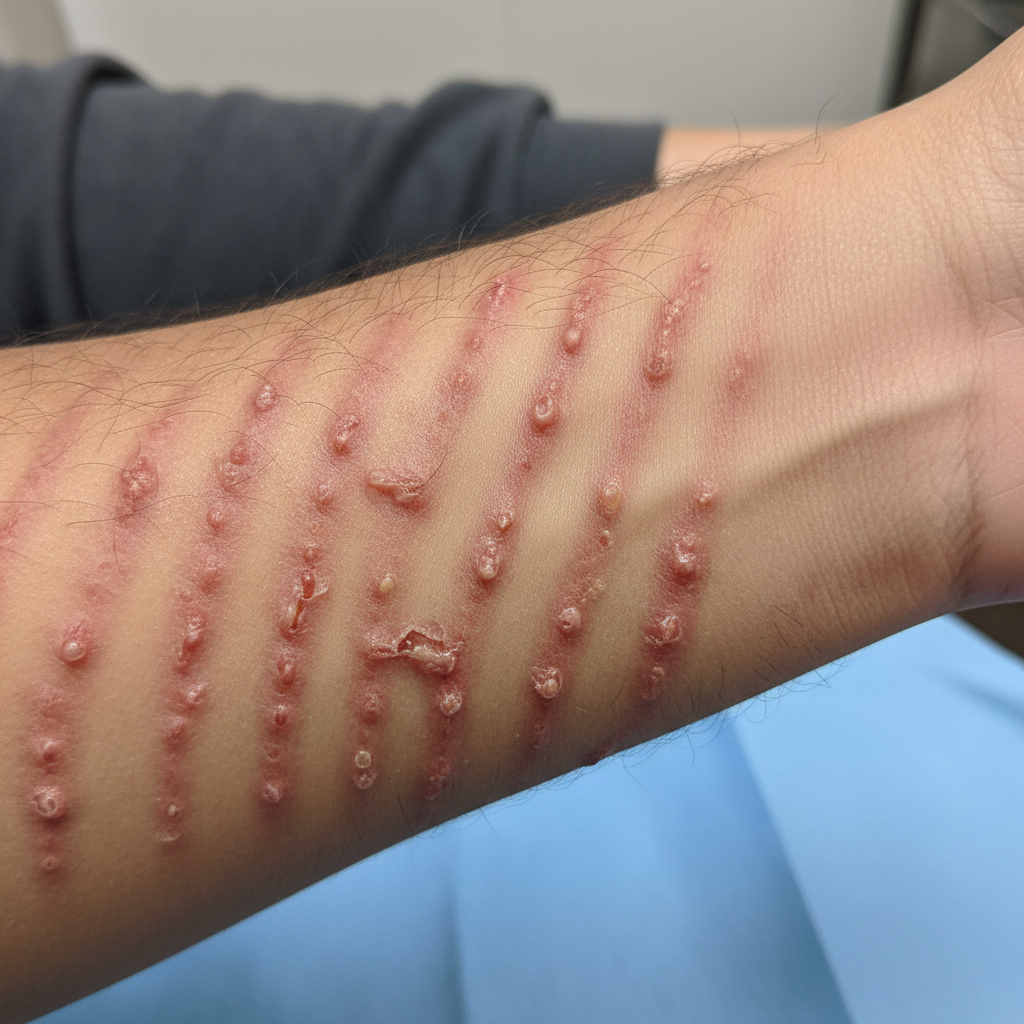
A 20-year-old man comes to the physician because of a 2-day history of a pruritic rash on both arms. He returned from a 2-week hiking trip in North Carolina 1 day ago. He has ulcerative colitis. He works as a landscape architect. His only medication is a mesalazine suppository twice daily. He has smoked a pack of cigarettes daily for 4 years and drinks one alcoholic beverage daily. He does not use illicit drugs. His temperature is 36.8°C (98.2°F), pulse is 65/min, respirations are 16/min, and blood pressure is 127/74 mm Hg. A photograph of the rash is shown. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in management?
A 40-year-old South Asian male presents to a primary care provider complaining of a chronic cough that is worse at night. Through a translator, he reports that he has had the cough for several years but that it has been getting worse over the last few months. He recently moved to the United States to work in construction. He attributes some weight loss of ten pounds in the last three months along with darker stools to difficulties adjusting to a Western diet. He denies any difficulty swallowing or feeling of food getting stuck in his throat. He drinks alcohol once or twice per week and has never smoked. He denies any family history of cancer. On physical exam, his lungs are clear to auscultation bilaterally without wheezing. His abdomen is soft and non-distended. He has no tenderness to palpation, and bowel sounds are present. He expresses concern that he will be fired from work if he misses a day and requests medication to treat his cough. Which of the following is the best next step in management?
A 17-year-old girl comes to the physician because of a 4-month history of fatigue. She has not had any change in weight. She had infectious mononucleosis 4 weeks ago. Menses occur at regular 28-day intervals and last 5 days with moderate flow. Her last menstrual period was 3 weeks ago. Her mother has Hashimoto thyroiditis. Examination shows pale conjunctivae, inflammation of the corners of the mouth, and brittle nails. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 10.3 g/dL Mean corpuscular volume 74 μm3 Platelet count 280,000/mm3 Leukocyte count 6,000/mm3 Which of the following is the most appropriate next step in evaluating this patient's illness?
A 56-year-old male with a history of hypertension, asthma, intravenous drug use, and recent incarceration 2 months ago presents to your office with an erythematous, itchy rash on his arms and chest. He does not recall exactly when the rash first started but he believes it was several days ago. Review of symptoms is notable for cough, runny nose, and diarrhea for several weeks. He is currently taking medications for a cough that he developed while he was incarcerated. He does not know the name of his medications and does not remember his diagnosis. Temperature is 99°F (37.2°C), blood pressure is 145/90 mmHg, pulse is 90/min, respirations are 20/min. He has difficulty remembering his history and appears thin. There is a scaly, symmetrical rash on his arms and neck with areas of dusky brown discoloration. He has mild abdominal tenderness to palpation but no rebound or guarding. Physical exam is otherwise unremarkable. Which of the following is associated with this disease syndrome?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
