Gastroenterology — MCQs

On this page
A patient presents with right upper quadrant pain, fever, and nonbloody vomiting. Which of the following risk factors is most likely associated with the patient's condition?
A 42-year-old man comes to his primary care physician complaining of abdominal pain. He describes intermittent, burning, epigastric pain over the past 4 months. He reports that the pain worsens following meals. He had an upper gastrointestinal endoscopy done 2 months ago that showed a gastric ulcer without evidence of malignancy. The patient was prescribed pantoprazole with minimal improvement in symptoms. He denies nausea, vomiting, diarrhea, or melena. The patient has no other medical problems. He had a total knee replacement 3 years ago following a motor vehicle accident for which he took naproxen for 2 months for pain management. He has smoked 1 pack per day since the age of 22 and drinks 1-2 beers several nights a week with dinner. He works as a truck driver, and his diet consists mostly of fast food. His family history is notable for hypertension in his paternal grandfather and coronary artery disease in his mother. On physical examination, the abdomen is soft, nondistended, and mildly tender in the mid-epigastric region. A stool test is positive for Helicobacter pylori antigen. In addition to antibiotic therapy, which of the following is the most likely to decrease the recurrence of the patient's symptoms?
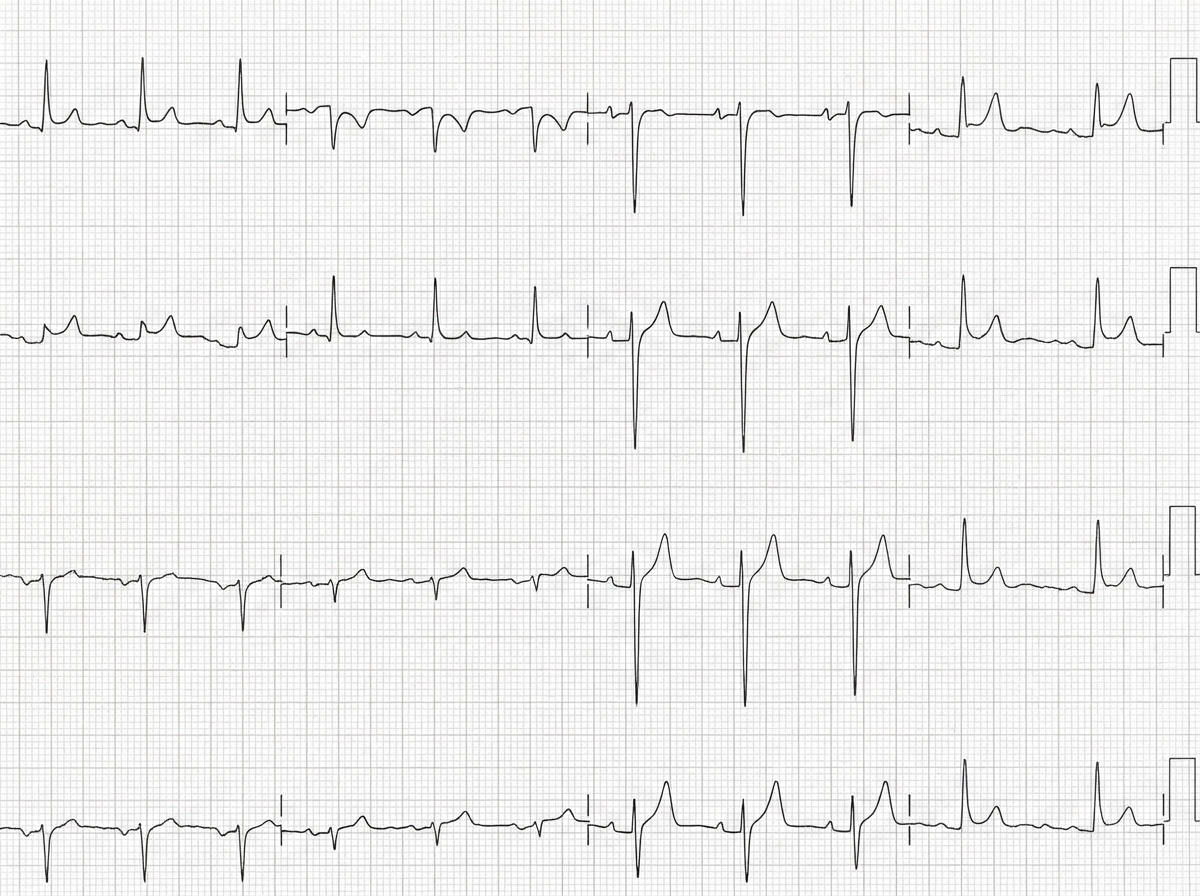
A 50-year-old man with a history of stage 4 kidney disease was admitted to the hospital for an elective hemicolectomy. His past medical history is significant for severe diverticulitis. After the procedure he becomes septic and was placed on broad spectrum antibiotics. On morning rounds, he appear weak and complains of fatigue and nausea. His words are soft and he has difficulty answering questions. His temperature is 38.9°C (102.1°F), heart rate is 110/min, respiratory rate is 15/min, blood pressure 90/65 mm Hg, and saturation is 89% on room air. On physical exam, his mental status appears altered. He has a bruise on his left arm that spontaneously appeared overnight. His cardiac exam is positive for a weak friction rub. Blood specimens are collected and sent for evaluation. An ECG is performed (see image). What therapy will this patient most likely receive next?
A 44-year-old man comes to the physician for a pre-employment evaluation. On questioning, he reports a mild cough, sore throat, and occasional headaches for 1 week. He has not had fever or weight loss. Nine years ago, he was diagnosed with HIV. He has gastroesophageal reflux disease. He has a history of IV drug abuse but quit 8 years ago. He has smoked one pack of cigarettes daily for 27 years and does not drink alcohol. Current medications include tenofovir, emtricitabine, efavirenz, and esomeprazole. He is 180 cm (5 ft 11 in) tall and weighs 89 kg (196 lbs); BMI is 27.5 kg/m2. His temperature is 37.3°C (99.1°F), pulse is 81/min, respirations are 17/min, and blood pressure is 145/75 mm Hg. Pulmonary examination shows no abnormalities. There are a few scattered old scars along the left elbow flexure. Laboratory studies show a leukocyte count of 6200/mm3, hemoglobin of 13.8 g/dL, and CD4+ count of 700/m3 (N = ≥ 500/mm3). A tuberculin skin test (TST) comes back after 50 hours with an induration of 3 mm in diameter. Which of the following is the most appropriate next step in management?
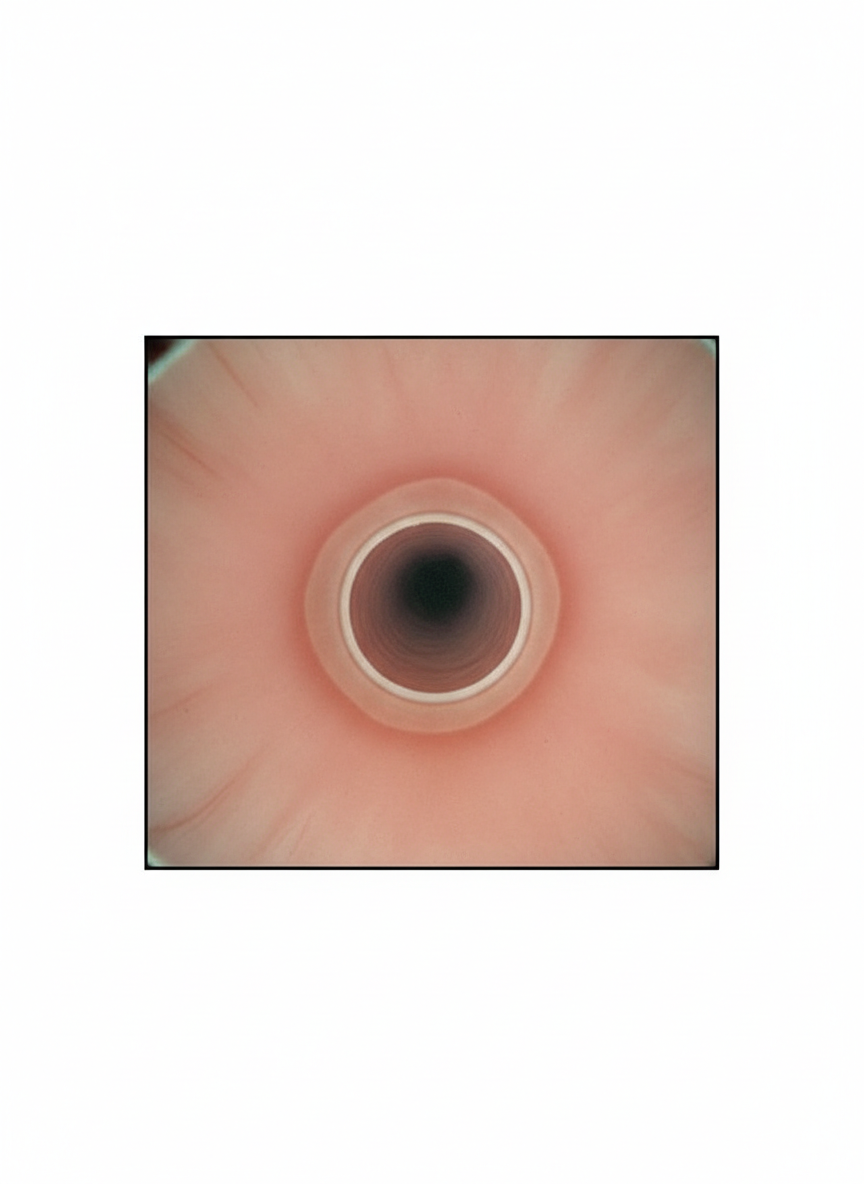
A 45-year-old man presents to an ambulatory clinic for evaluation after feeling food stuck behind the sternum when he was eating a hamburger last night. He was not in pain. He had to drink a whole glass of water to get the food down; however, he did manage to finish his dinner without any further problems. He is concerned because he has had 2 similar episodes this year. He is otherwise healthy. He has smoked 1 half-pack of cigarettes a day for 20 years and enjoys a can of beer every night. His vital signs are as follows: blood pressure 125/75 mm Hg, pulse 68/min, respiratory rate 14/min, and temperature 36.5°C (97.7°F). His oral examination reveals 2 decayed teeth. The physical exam is otherwise unremarkable. An endoscopic image of the lower esophagus is shown. Which of the following is the most appropriate next step in management?
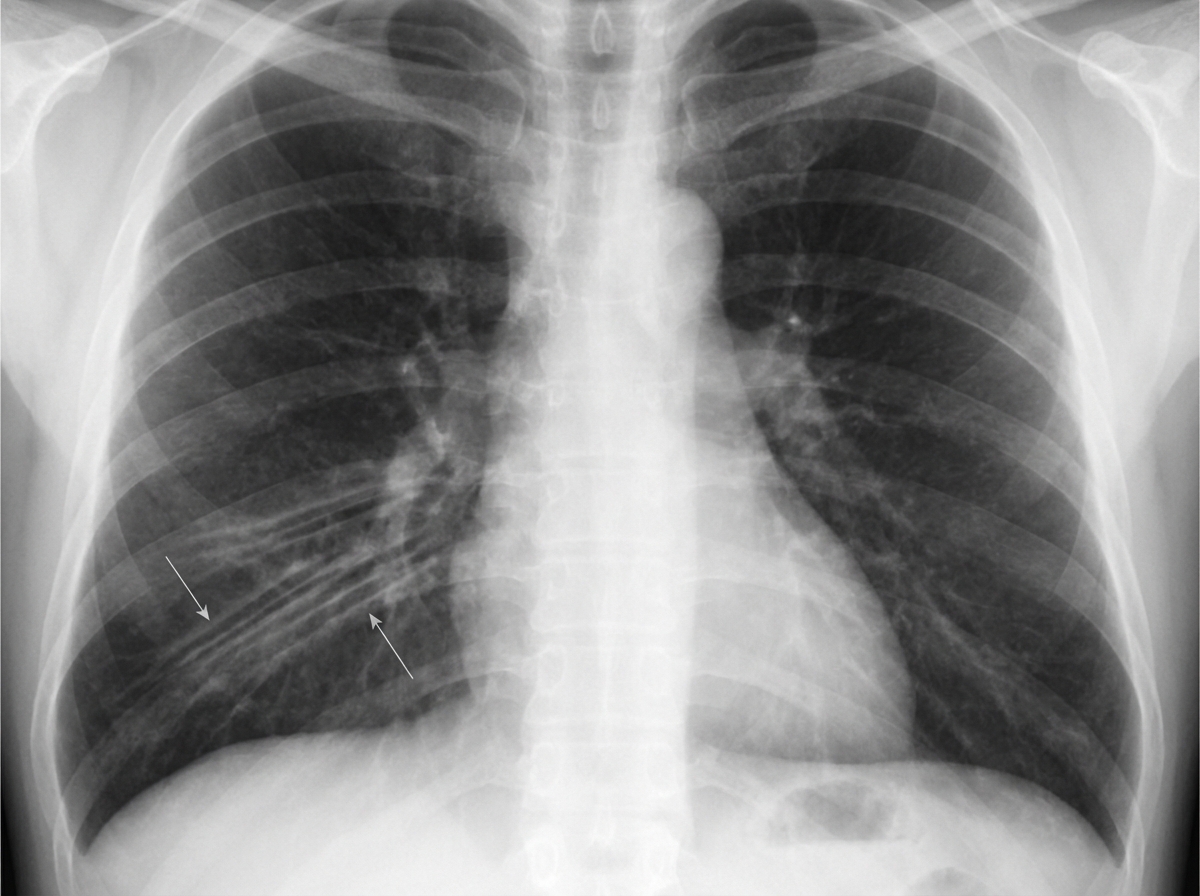
A 65-year-old man is brought to the emergency department after coughing up copious amounts of blood-tinged sputum at his nursing home. He recently had an upper respiratory tract infection that was treated with antibiotics. He has a long-standing history of productive cough that has worsened since he had a stroke 3 years ago. He smoked a pack of cigarettes daily for 40 years until the stroke, after which he quit. The patient appears distressed and short of breath. His temperature is 38°C (100.4°F), pulse is 92/min, and blood pressure is 145/85 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 92%. Physical examination shows digital clubbing and cyanosis of the lips. Coarse crackles are heard in the thorax. An x-ray of the chest shows increased translucency and tram-track opacities in the right lower lung field. Which of the following is the most likely diagnosis?
A 57-year-old woman comes to the physician because of a 3-month history of easy fatigability and dyspnea on exertion. Menopause occurred 5 years ago. Her pulse is 105/min and blood pressure is 100/70 mm Hg. Physical examination shows pallor of the nail beds and conjunctivae. A peripheral blood smear shows small, pale red blood cells. Further evaluation is most likely to show which of the following findings?
A 31-year old man presents to the emergency department for blood in his stool. The patient states that he saw a small amount of bright red blood on his stool and on the toilet paper this morning, which prompted his presentation to the emergency department. The patient denies any changes in his bowel habits or in his weight. The patient has a past medical history of asthma managed with albuterol and fluticasone. The patient has a family history of alcoholism in his father and suicide in his mother. His temperature is 97°F (36.1°C), blood pressure is 120/77 mmHg, pulse is 60/min, respirations are 12/min, and oxygen saturation is 98% on room air. On physical exam, the patient has a cardiac and pulmonary exam that are within normal limits. On abdominal exam, there is no tenderness or guarding and normal bowel sounds. Laboratory values are ordered and return as below. Hemoglobin: 15 g/dL Hematocrit: 42% Leukocyte count: 4,500 cells/mm^3 with normal differential Platelet count: 230,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 24 mEq/L BUN: 20 mg/dL Glucose: 92 mg/dL Creatinine: 1.0 mg/dL Ca2+: 9.9 mg/dL Which of the following is the next best step in management?
A 25-year-old man comes to the physician because of a 4-day history of bloody stools. During this time, he has not had nausea, vomiting, abdominal cramps, or pain while defecating. He has had recurrent episodes of non-bloody diarrhea for the past 6 months. His father died of colon cancer at the age of 39 years. His vital signs are within normal limits. Physical examination shows small, painless bony swellings on the mandible, forehead, and right shin. There are multiple non-tender, subcutaneous nodules with central black pores present over the trunk and face. Fundoscopic examination shows multiple, oval, darkly pigmented lesions on the retina. Colonoscopy shows approximately 150 colonic polyps. Which of the following is the most likely diagnosis?
An 18-year-old woman comes to see her primary care physician for a physical for school. She states she has not had any illnesses last year and is on her school's volleyball team. She exercises daily, does not use any drugs, and has never smoked cigarettes. On physical exam you note bruising around the patients neck, and what seems to be burn marks on her back and thighs. The physician inquires about these marks. The patient explains that these marks are the result of her sexual activities. She states that in order for her to be aroused she has to engage in acts such as hitting, choking, or anything else that she can think of. The physician learns that the patient lives with her boyfriend and that she is in a very committed relationship. She is currently monogamous with this partner. The patient is studying with the hopes of going to law school and is currently working in a coffee shop. The rest of the patient’s history and physical is unremarkable. Which of the following is the most likely diagnosis?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
