Gastroenterology — MCQs

On this page
A 45-year-old woman comes to the physician because of a 5-month history of recurrent retrosternal chest pain that often wakes her up at night. Physical examination shows no abnormalities. Upper endoscopy shows hyperemia in the distal third of the esophagus. A biopsy specimen from this area shows non-keratinized stratified squamous epithelium with hyperplasia of the basal cell layer and neutrophilic inflammatory infiltrates. Which of the following is the most likely underlying cause of this patient's findings?
A 31-year-old man comes to the physician because of worsening abdominal pain, an inability to concentrate at work, and a general lack of motivation over the past several months. He has a history of spontaneous passage of two kidney stones. His father and uncle underwent thyroidectomy before the age of 35 for thyroid cancer. Physical examination shows diffuse tenderness over the abdomen. Serum studies show: Na+ 142 mEq/L K+ 3.7 mEq/L Glucose 131 mg/dL Ca2+ 12.3 mg/dL Albumin 4.1 g/dL Parathyroid hormone 850 pg/mL Further evaluation is most likely to show elevated levels of which of the following?
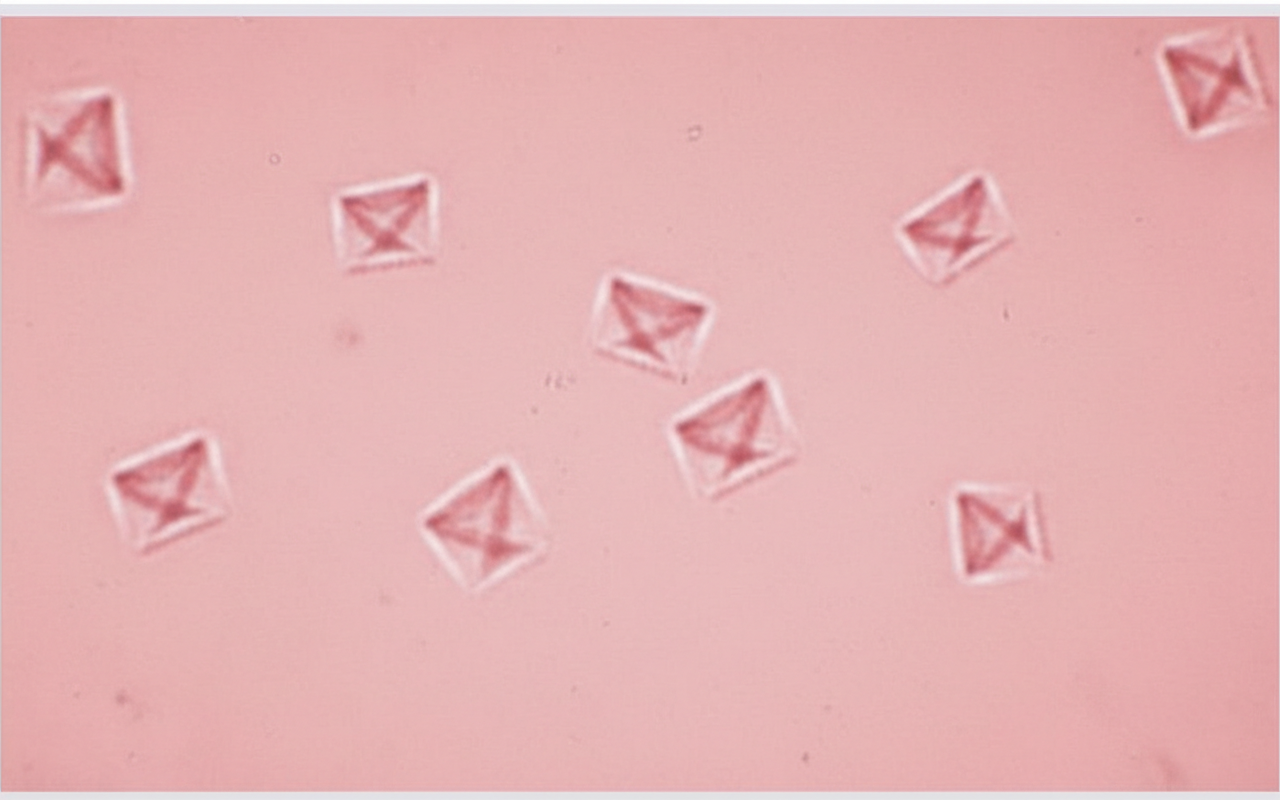
A 46-year-old man comes to the emergency department because of sharp pain in his left flank that began suddenly 30 minutes ago. Physical examination shows costovertebral angle tenderness on the left side. A photomicrograph of the urine is shown. The patient is most likely to benefit from an increase of which of the following components in the urine?
A 30-year-old man who recently emigrated from Southeast Asia presents with heartburn and a bad taste in his mouth. He says the symptoms have been present for the last 6 months and are much worse at night. He describes the pain as moderate to severe, burning in character, and localized to the epigastric region. He mentions that 1 month ago, he was tested for Helicobacter pylori back in his country and completed a course of multiple antibiotics, but there has been no improvement in his symptoms. Which of the following is the most likely diagnosis in this patient?
A 32-year-old woman complains of fatigue and pallor. She says symptoms that started several months ago and have been becoming more serious with time. She reports that she has been exercising regularly and has been adhering to a strict vegan diet. The patient has no significant past medical history and takes no current medications. She denies any smoking history, alcohol use, or recreational drug use. She is tachycardic, but otherwise, her physical examination is unremarkable. A complete blood count (CBC) shows anemia with a low MCV (mean corpuscular volume), and a peripheral blood smear shows small erythrocytes. Which of the following is the most likely diagnosis in this patient?
A 31-year-old man comes to the physician because of a 9-month history of increasing fatigue and recurrent nausea. During this period, he has had a 3.8 kg (8.3 lb) weight loss. He also reports feeling lightheaded when he stands up suddenly. He was diagnosed with alopecia areata 1 year ago and was treated with monthly intralesional triamcinolone injections for 3 months. He does not smoke or drink alcohol. His temperature is 37.4°C (99.3°F), pulse is 86/min, and blood pressure is 102/68 mm Hg. Examination of the scalp shows a few well-defined patches of hair loss without scarring. The creases of the palm are darkened. Serum studies show: Na+ 125 mEq/L Cl- 98 mEq/L K+ 5.6 mEq/L Glucose 72 mg/dL Creatinine 0.8 mg/dL Thyroid-stimulating hormone 4.1 μU/mL Cortisol (AM) 2.5 μg/dL Cortisol (30 min after 250 μg corticotropin) 2.6 μg/dL Which of the following is the most likely underlying mechanism of this patient's symptoms?
A 35-year-old woman comes to the physician with right-sided flank pain and blood in her urine for 1 day. She does not have fever or dysuria. She had similar symptoms several weeks ago but did not seek medical care at the time. Physical examination shows right costovertebral angle tenderness. Her serum uric acid level is 6.9 mg/dL. Urine dipstick shows 3+ blood. Analysis of a 24-hour urine collection specimen shows wedge-shaped prisms. This patient is most likely to benefit from which of the following to prevent recurrence of her condition?
A 70-year-old man with a history of chronic constipation presents to the emergency department with a two-day history of left lower quadrant abdominal pain. He is found to have a temperature of 100.8F, BP 140/90, HR 85, and RR 16. On physical examination, he is tender to light palpation in the left lower quadrant and exhibits voluntary guarding. Rectal examination reveals heme-positive stool. Laboratory values are unremarkable except for a WBC count of 12,500 with a left shift. Which of the following tests would be most useful in the diagnosis of this patient's disease?
A 56-year-old woman presents to the emergency department following a seizure episode. She has a remote history of tonic-clonic seizures; however, her seizures have been well-controlled on valproate, with no seizure episodes occurring over the past 12 years. She was weaned off of the valproate 4 months ago. Her temperature is 97.6°F (36.4°C), blood pressure is 122/80 mmHg, pulse is 85/min, respirations are 15/min, and oxygen saturation is 99% on room air. Examination reveals her to be lethargic and somewhat confused. She is moving all extremities spontaneously. Her mucous membranes appear moist and she does not demonstrate any skin tenting. Laboratory values are ordered as seen below. Arterial blood gas pH: 7.21 PO2: 99 mmHg PCO2: 20 mmHg HCO3-: 10 meq/L The patient's initial serum chemistries and CBC are otherwise unremarkable except for the bicarbonate as indicated above. An ECG demonstrates normal sinus rhythm. Which of the following is the best next step in management for this patient's acid-base status?
A 65-year-old man presents to the emergency department with vague, constant abdominal pain, and worsening shortness of breath for the past several hours. He has baseline shortness of breath and requires 2–3 pillows to sleep at night. He often wakes up because of shortness of breath. Past medical history includes congestive heart failure, diabetes, hypertension, and hyperlipidemia. He regularly takes lisinopril, metoprolol, atorvastatin, and metformin. His temperature is 37.0°C (98.6°F), respiratory rate 25/min, pulse 67/min, and blood pressure 98/82 mm Hg. On physical examination, he has bilateral crackles over both lung bases and a diffusely tender abdomen. His subjective complaint of abdominal pain is more severe than the observed tenderness on examination. Which of the following vessels is involved in the disease affecting this patient?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
