Gastroenterology — MCQs

On this page
A 22-year-old female college student comes to your clinic to establish care. She has no significant past medical history and her only complaint today is that she has had trouble maintaining a consistent weight. Her temperature is 98.6°F (37.0°C), blood pressure is 100/65 mmHg, pulse is 62/min, and respirations are 12/min. Her body mass index is 19.5. Her physical exam is significant for callused knuckles and dental enamel erosions. What laboratory abnormalities are likely to be found in this patient?
A 49-year-old man comes with odynophagia, abdominal pain, fatigue, headache, and fever for several weeks. The patient reports no chronic medical problems, no travel, and no recent sick exposures. Physical examination is significant only for an erythematous oral mucosa and cervical lymphadenopathy. His vital signs show a blood pressure of 121/72 mm Hg, heart rate of 82/min, and respiratory rate of 16/min. On a review of systems, the patient reports regular, unprotected sexual encounters with men and women. Of the following options, which disease must be excluded?
A 27-year old woman comes to the physician for a rash that began 5 days ago. The rash involves her abdomen, back, arms, and legs, including her hands and feet. Over the past month, she has also had mild fever, headache, and myalgias. She has no personal history of serious illness. She smokes 1 pack of cigarettes a day and binge drinks on the weekends. She uses occasional cocaine, but denies other illicit drug use. Vital signs are within normal limits. Physical examination shows a widespread, symmetric, reddish-brown papular rash involving the trunk, upper extremities, and palms. There is generalized, nontender lymphadenopathy. Skin examination further shows patchy areas of hair loss on her scalp and multiple flat, broad-based, wart-like papules around her genitalia and anus. Rapid plasma reagin and fluorescent treponemal antibody test are both positive. In addition to starting treatment, which of the following is the most appropriate next step in management?
A 70-year-old man presents with severe abdominal pain over the last 24 hours. He describes the pain as severe and associated with diarrhea, nausea, and vomiting. He says he has had a history of postprandial abdominal pain over the last several months. The patient denies any fever, chills, recent antibiotic use. Past medical history is significant for peripheral arterial disease and type 2 diabetes mellitus. The patient reports a 20 pack-year smoking history. His vital signs include blood pressure 90/60 mm Hg, pulse 100/min, respiratory rate 22/min, temperature 38.0°C (100.5°F), and oxygen saturation of 98% on room air. On physical examination, the patient is ill-appearing. His abdomen is severely tender to palpation and distended with no rebound or guarding. Pain is disproportionate to the exam findings. Rectal examination demonstrates bright red-colored stool. Abdominal X-ray is unremarkable. Stool culture was negative for C. difficile. A contrast-enhanced CT scan reveals segmental colitis involving the distal transverse colon. Which of the following is the most likely cause of this patient's symptoms?
A 66-year-old woman is brought to the emergency department because of fever, chills, night sweats, and progressive shortness of breath for 1 week. She also reports generalized fatigue and nausea. She has type 2 diabetes mellitus and hypothyroidism. Current medications include metformin, sitagliptin, and levothyroxine. She appears ill. Her temperature is 38.7°C (101.7°F), pulse is 104/min, and blood pressure is 160/90 mm Hg. Examination shows pale conjunctivae and small nontender hemorrhagic macules over her palms and soles. Crackles are heard at both lung bases. A grade 2/6 mid-diastolic murmur is heard best at the third left intercostal space and is accentuated by leaning forward. The spleen is palpated 1–2 cm below the left costal margin. Laboratory studies show: Hemoglobin 10.6 g/dL Leukocyte count 18,300/mm3 Erythrocyte sedimentation rate 48 mm/h Urine Protein 1+ Blood 2+ RBCs 20-30/hpf WBCs 0-2/hpf An echocardiography shows multiple vegetations on the aortic valve. Blood cultures grow S. gallolyticus. She is treated with ampicillin and gentamicin for 2 weeks and her symptoms resolve. A repeat echocardiography at 3 weeks shows mild aortic regurgitation with no vegetations. Which of the following is the most appropriate next step in management?
A 39-year-old man comes to the emergency department because of fever, urinary frequency, and lower back pain for the last 3 days. During this period, he has also had pain with the 3 times he has defecated. He is sexually active with one female partner and does not use condoms. His father died of colon cancer at the age of 67 years. The patient has smoked one pack of cigarettes daily for 14 years and drinks alcohol occasionally. His temperature is 39.1°C (102.3°F), pulse is 114/min, and blood pressure is 140/90 mm Hg. Physical examination shows mild suprapubic pain on deep palpation and a swollen, tender prostate. The remainder of the examination shows no abnormalities. His hemoglobin concentration is 15.4 g/dL, leukocyte count is 18,400/mm3, and platelet count is 260,000/mm3. Which of the following is the most appropriate next step in the management of this patient's condition?
A 54-year-old man comes to the physician because of diarrhea that has become progressively worse over the past 4 months. He currently has 4–6 episodes of foul-smelling stools per day. Over the past 3 months, he has had fatigue and a 5-kg (11-lb) weight loss. He returned from Bangladesh 6 months ago after a year-long business assignment. He has osteoarthritis and hypertension. Current medications include amlodipine and naproxen. He appears pale and malnourished. His temperature is 37.3°C (99.1°F), pulse is 76/min, and blood pressure is 140/86 mm Hg. Examination shows pale conjunctivae and dry mucous membranes. Angular stomatitis and glossitis are present. The abdomen is distended but soft and nontender. Rectal examination shows no abnormalities. Laboratory studies show: Hemoglobin 8.9 g/dL Leukocyte count 4100/mm3 Platelet count 160,000/mm3 Mean corpuscular volume 110 μm3 Serum Na+ 133 mEq/L Cl- 98 mEq/l K+ 3.3 mEq/L Creatinine 1.1 mg/dL IgA 250 mg/dL Anti-tissue transglutaminase, IgA negative Stool culture and studies for ova and parasites are negative. Test of the stool for occult blood is negative. Fecal fat content is 22 g/day (N < 7). Fecal lactoferrin is negative and elastase is within normal limits. Which of the following is the most appropriate next step in diagnosis?
A 70-year-old man comes to the physician because of episodes of watery stools for the past 6 weeks. During this period, he has also had recurrent episodes of reddening of the face, neck, and chest that last up to 30 minutes, especially following alcohol consumption. He has hypertension. He smoked one pack of cigarettes daily for 20 years but quit 8 years ago. He drinks two glasses of wine daily. Current medications include enalapril. He appears pale. He is 185 cm (6 ft 1 in) tall and weighs 67 kg (147.7 lb); BMI is 19.6 kg/m2. His temperature is 36.7°C (98°F), pulse is 85/min, and blood pressure is 130/85 mm Hg. Scattered expiratory wheezing is heard throughout both lung fields. Cardiac examination shows no abnormalities. The abdomen is soft and mildly tender. The remainder of the physical examination shows no abnormalities. A complete blood count and serum concentrations of urea nitrogen and creatinine are within the reference range. Which of the following is the most likely diagnosis in this patient?
Please refer to the summary above to answer this question Which of the following is the most likely diagnosis? Patient information Age: 61 years Gender: F, self-identified Ethnicity: unspecified Site of care: emergency department History Reason for Visit/Chief Concern: "My belly really hurts." History of Present Illness: developed abdominal pain 12 hours ago pain constant; rated at 7/10 has nausea and has vomited twice has had two episodes of nonbloody diarrhea in the last 4 hours 12-month history of intermittent constipation reports no sick contacts or history of recent travel Past medical history: hypertension type 2 diabetes mellitus mild intermittent asthma allergic rhinitis Social history: diet consists mostly of high-fat foods does not smoke drinks 1–2 glasses of wine per week does not use illicit drugs Medications: lisinopril, metformin, albuterol inhaler, fexofenadine, psyllium husk fiber Allergies: no known drug allergies Physical Examination Temp Pulse Resp. BP O2 Sat Ht Wt BMI 38.4°C (101.1°F) 85/min 16/min 134/85 mm Hg – 163 cm (5 ft 4 in) 94 kg (207 lb) 35 kg/m2 Appearance: lying back in a hospital bed; appears uncomfortable Neck: no jugular venous distention Pulmonary: clear to auscultation; no wheezes, rales, or rhonchi Cardiac: regular rate and rhythm; normal S1 and S2; no murmurs, rubs, or gallops Abdominal: obese; soft; tender to palpation in the left lower quadrant; no guarding or rebound tenderness; normal bowel sounds Extremities: no edema; warm and well-perfused Skin: no rashes; dry Neurologic: alert and oriented; cranial nerves grossly intact; no focal neurologic deficits
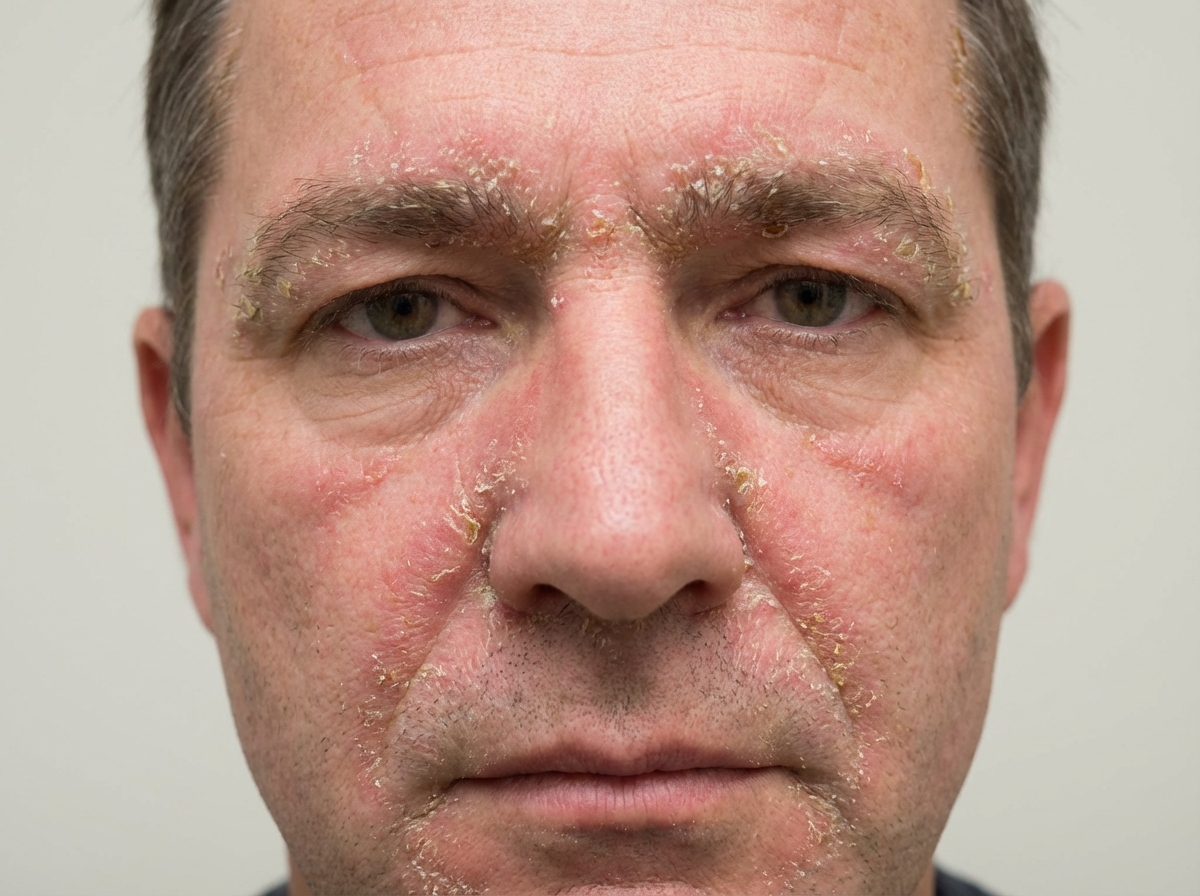
A 28-year-old man comes to the physician because of a 3-month history of a recurrent pruritic rash on his face and scalp. He reports that he has been using a new shaving cream once a week for the past 5 months. A year ago, he was diagnosed with HIV and is currently receiving triple antiretroviral therapy. He drinks several six-packs of beer weekly. Vital signs are within normal limits. A photograph of the rash is shown. A similar rash is seen near the hairline of the scalp and greasy yellow scales are seen at the margins of the eyelids. Which of the following is the most likely diagnosis?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
