Gastroenterology — MCQs

On this page
A 63-year-old woman presents to the primary care physician’s clinic complaining of fatigue, diarrhea, headaches, and a loss of appetite. She denies any personal history of blood clots in her past, but she says that her mother has also had to be treated for pulmonary embolism in the recent past. Her past medical history is significant for preeclampsia, hypertension, polycystic ovarian syndrome, and hypercholesterolemia. She currently smokes 1 pack of cigarettes per day, drinks a glass of wine per day, and she currently denies any illicit drug use, although she has a remote past of injection drug use with heroin. The vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 111/min and irregular, and respiratory rate 17/min. On physical examination, her pulses are bounding and complexion is pale, but breath sounds remain clear. Oxygen saturation was initially 91% on room air and electrocardiogram (ECG) showed atrial fibrillation. Upon further discussion with the patient, her physician discovers that she is having some cognitive difficulty. The laboratory results reveal: mean corpuscular volume (MCV) 111 fL; hemoglobin (Hgb) 9.3 g/dL; methylmalonic acid (MMA) and homocysteine are both elevated. Schilling test is positive. What is the next best step in the management of this patient?
A 52-year-old woman presents with fatigue, difficulty swallowing solid foods, and frequent choking spells. She says her symptoms gradually onset 3 months ago and have progressively worsened. Past medical history is unremarkable. She reports drinking alcohol occasionally but denies smoking or illicit drug use. Her vital signs include: temperature 36.6°C (97.8°F), blood pressure 115/72 mm Hg, pulse 82/min. Physical examination shows conjunctival pallor but is otherwise unremarkable. Laboratory results are significant for the following: Hemoglobin 9.8 g/dL Red cell count 2.5 million/mm3 Mean corpuscular volume 73 μm3 Serum ferritin 9.7 ng/mL A barium swallow study is performed, which shows a proximal esophageal web. Which of the following is the most likely diagnosis in this patient?
A 57-year-old woman comes to the physician because of a 2-week history of worsening epigastric pain that improves with meals. She has had similar pain of lesser intensity for the past 4 years. Physical examination shows no abnormalities. Upper endoscopy shows a 0.5-cm mucosal breach in the anterior duodenal bulb that extends into the submucosa. A biopsy specimen of the lesion shows hypertrophy of the Brunner glands. This patient is at the greatest risk for which of the following complications?
A 23-year-old man presents to his primary care physician with complaints of fatigue and cheek pain that started a day ago. He notes that he has nasal discharge that is yellow/green as well. Otherwise, he feels well and is generally healthy. The patient has a past medical history of type I diabetes mellitus and occasionally uses IV drugs. His temperature is 99.0°F (37.2°C), blood pressure is 120/84 mmHg, pulse is 70/min, respirations are 16/min, and oxygen saturation is 98% on room air. There is pain to palpation of the left and right maxilla. Pain is worsened when the patient bends over. Which of the following is the most appropriate initial step in management?
A 42-year-old man presents to his primary care provider for abdominal pain. He reports that for several months he has been experiencing a stabbing pain above the umbilicus during meals. He denies associated symptoms of nausea, vomiting, or diarrhea. The patient’s past medical history is significant for hypertension and hyperlipidemia for which he takes amlodipine and atorvastatin. His family history is significant for lung cancer in his father. The patient is a current smoker with a 20 pack-year smoking history and drinks 3-5 beers per week. Initial laboratory testing is as follows: Serum: Na+: 141 mEq/L K+: 4.6 mEq/L Cl-: 102 mEq/L HCO3-: 25 mEq/L Urea nitrogen: 14 mg/dL Creatinine: 1.1 mg/dL Glucose: 120 mg/dL Calcium: 8.4 mg/dL Alkaline phosphatase: 66 U/L Aspartate aminotransferase (AST): 40 U/L Alanine aminotransferase (ALT): 52 U/L Gastrin: 96 pg/mL (<100 pg/mL) Lipase: 90 U/L (<160 U/L) The patient is started on a proton pump inhibitor without symptomatic improvement after 6 weeks. He is referred for an upper endoscopy, which demonstrates erosive gastritis, three ulcers in the duodenum, and one ulcer in the jejunum. Biopsy of the gastric mucosa is negative for H. pylori. Which of the following is the best next step in management?
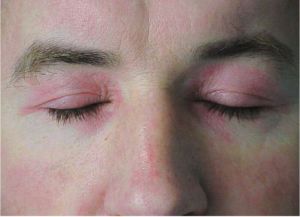
A 43-year-old woman comes to the physician because of a 3-week history of progressive weakness. She has had increased difficulty combing her hair and climbing stairs. She has hypertension. She has smoked a pack of cigarettes daily for 25 years. She does not drink alcohol. Her mother had coronary artery disease and systemic lupus erythematosus. Her current medications include chlorthalidone and vitamin supplements. Her temperature is 37.8°C (100.0°F), pulse is 71/min, and blood pressure is 132/84 mm Hg. Cardiopulmonary examination is unremarkable. A rash is shown that involves both her orbits. Skin examination shows diffuse erythema of the upper back, posterior neck, and shoulders. Which of the following antibodies are most likely to be present in this patient?
A 35-year old Caucasian woman visits a community clinic and is presenting with a long history of early satiety, diarrhea, fatigue, hair loss, and brittle nails. Her family history is insignificant. Her personal history is relevant for iron deficiency anemia and vitamin B12 deficiency, as seen in her lab reports a few months back. Her physical examination is unremarkable except for pale skin and mucous surfaces, and glossitis. She brings with herself an upper endoscopy report describing body and fundal atrophic gastritis. Which of the following tests would you expect to be positive in this patient?
A 52-year-old man presents to the emergency department with severe pain of the left first metatarsophalangeal joint. He says that the pain started 3 hours ago and describes it as sharp in character. The pain has been so severe that he has not been able to tolerate any movement of the joint. His past medical history is significant for hypertension for which he takes a thiazide diuretic. His diet consists primarily of red meat, and he drinks 5 bottles of beer per night. On physical exam, his left first metatarsophalangeal joint is swollen, erythematous, and warm to the touch. Which of the following characteristics would be seen with the most likely cause of this patient's symptoms?
A 46-year-old woman presents to your medical office complaining of ‘feeling tired’. The patient states that she has been having some trouble eating because her ‘tongue hurts’, but she has no other complaints. On examination, the patient has pale conjunctiva and skin and also appears tired. She has a smooth, red tongue that is tender to touch with a tongue depressor. The patient’s hands and feet feel cold. Fluoroscopic evaluation of the swallowing mechanism and esophagus is normal. Which of the following diagnoses is most likely?
A 53-year-old man comes to the emergency department for severe left knee pain for the past 8 hours. He describes it as an unbearable, burning pain that woke him up from his sleep. He has been unable to walk since. He has not had any trauma to the knee. Ten months ago, he had an episode of acute pain and swelling of the right great toe that subsided after treatment with indomethacin. He has hypertension, type 2 diabetes mellitus, psoriasis, and hyperlipidemia. Current medications include topical betamethasone, metformin, glipizide, losartan, and simvastatin. Two weeks ago, hydrochlorothiazide was added to his medication regimen to improve blood pressure control. He drinks 1–2 beers daily. He is 170 cm (5 ft 7 in) tall and weighs 110 kg (242 lb); BMI is 38.1 kg/m2. His temperature is 38.4°C (101.1°F). Examination shows multiple scaly plaques over his palms and soles. The left knee is erythematous, swollen, and tender; range of motion is limited by pain. Which of the following is the most appropriate next step in management?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
