Gastroenterology — MCQs

On this page
A 21-year-old female presents to her obstetrician because she has stopped getting her period, after being irregular for the last 3 months. Upon further questioning, the patient reveals that she has had a 17 lb. unintended weight loss, endorses chronic diarrhea, abdominal pain, and constipation that waxes and wanes. Family history is notable only for an older brother with Type 1 Diabetes. She is healthy, and is eager to gain back some weight. Her OBGYN refers her to a gastroenterologist, but first sends serology laboratory studies for IgA anti-tissue transglutaminase antibodies (IgA-tTG). These results come back positive at > 10x the upper limit of normal. Which of the following is the gastroenterologist likely to find on endoscopy and duodenal biopsy?
A 55-year-old woman presents with fatigue. She says her symptoms are present throughout the day and gradually started 4 months ago. Her past medical history is significant for rheumatoid arthritis–treated with methotrexate, and diabetes mellitus type 2–treated with metformin. The patient is afebrile, and her vital signs are within normal limits. A physical examination reveals pallor of the mucous membranes. Initial laboratory tests show hemoglobin of 7.9 g/dL, hematocrit of 22%, and mean corpuscular volume of 79 fL. Which of the following is the best next diagnostic step in this patient?
A 55-year-old woman comes to the physician because of a 6-month history of worsening fatigue. During this time, she has noted a decrease in her exercise capacity and she becomes short of breath when walking briskly. She has had occasional streaks of blood in her stools during periods of constipation. She was diagnosed with type 1 diabetes mellitus at the age of 24 years and has a history of hypertension and hypercholesterolemia. She does not smoke or drink alcohol. Her current medications include insulin, lisinopril, aspirin, and atorvastatin. Her diet mostly consists of white meat and vegetables. Her pulse is 92/min and blood pressure is 145/92 mm Hg. Examination shows conjunctival pallor. Cardiac auscultation shows a grade 2/6 midsystolic ejection murmur best heard along the right upper sternal border. Sensation to pinprick is decreased bilaterally over the dorsum of her feet. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 9.2 g/dL WBC count 7,200/mm3 Erythrocyte count 3.06 million/mm3 Mean corpuscular volume 84 μm3 Platelets 250,000/mm3 Reticulocyte count 0.6 % Erythrocyte sedimentation rate 15 mm/h Serum Na+ 142 mEq/L K+ 4.8 mEq/L Ca2+ 8.1 mEq/L Ferritin 145 ng/mL Urea nitrogen 48 mg/dL Creatinine 3.1 mg/dL A fecal occult blood test is pending. Which of the following is the most likely underlying cause of this patient's condition?
A previously healthy 65-year-old man comes to the physician for chronic left-sided abdominal discomfort. About 3 months ago, he started experiencing early satiety and eating less. He has lost 7 kg (15.4 lb) during this period. He also occasionally has left shoulder pain. He recently retired from his job on a production line at a shoe factory. His pulse is 72/min, blood pressure is 130/70 mm Hg, and temperature is 37.8°C (100.1°F). Physical examination shows nontender, bilateral axillary and right-sided inguinal lymphadenopathy. The spleen is palpated 7 cm below the costal margin. Which of the following is the strongest indicator of a poor prognosis for this patient's condition?
A 27-year-old school teacher visits her doctor because of disfiguring skin lesions that started to appear in the past few days. The lesions are mostly located on her chest, shoulders, and back. They are 2–5 mm in diameter, droplike, erythematous papules with fine silver scales. Besides a sore throat and laryngitis requiring amoxicillin several weeks ago, she has no significant medical history. What is the most likely diagnosis?
A 32-year-old woman presents with a three-month history of difficulty swallowing. She says that it occurs with both solids and liquids with the sensation that food is getting stuck in her throat. Additionally, the patient reports that while shoveling snow this past winter, she had noticed that her hands would lose their color and become numb. She denies any cough, regurgitation, joint pains, shortness of breath, fever, or changes in weight. She does not smoke or drink alcohol. The patient’s physical exam is within normal limits, although she does appear to have thickened, tight skin on her fingers. She does not have any other skin findings. Which antibody will most likely be found on serological study in this patient?
A 65-year-old man with chronic myelogenous leukemia comes to the physician because of severe pain and swelling in both knees for the past day. He finished a cycle of chemotherapy 1 week ago. His temperature is 37.4°C (99.4°F). Physical examination shows swelling and erythema of both knees and the base of his left big toe. Laboratory studies show: Leukocyte count 13,000/mm3 Serum Creatinine 2.2 mg/dL Calcium 8.2 mg/dL Phosphorus 7.2 mg/dL Arthrocentesis of the involved joints is most likely to show which of the following?
A 30-year-old forest landscape specialist is brought to the emergency department with hematemesis and confusion. One week ago she was diagnosed with influenza when she had fevers, severe headaches, myalgias, hip and shoulder pain, and a maculopapular rash. After a day of relative remission, she developed abdominal pain, vomiting, and diarrhea. A single episode of hematemesis occurred prior to admission. Two weeks ago she visited rainforests and caves in western Africa where she had direct contact with animals, including apes. She has no history of serious illnesses or use of medications. She is restless. Her temperature is 38.0℃ (100.4℉); the pulse is 95/min, the respiratory rate is 20/min; and supine and upright blood pressure is 130/70 mm Hg and 100/65 mm Hg, respectively. Conjunctival suffusion is noted. Ecchymoses are observed on the lower extremities. She is bleeding from one of her intravenous lines. The peripheral blood smear is negative for organisms. Filovirus genomes were detected during a reverse transcription-polymerase chain reaction. The laboratory studies show the following: Laboratory test Hemoglobin 10 g/dL Leukocyte count 1,000/mm3 Segmented neutrophils 65% Lymphocytes 20% Platelet count 50,000/mm3 Partial thromboplastin time (activated) 60 seconds Prothrombin time 25 seconds Fibrin split products positive Serum Alanine aminotransferase (ALT) 85 U/L Aspartate aminotransferase (AST) 120 U/L γ-Glutamyltransferase (GGT) 83 U/L Creatinine 2 mg/dL Which of the following is the most appropriate immediate step in management?
A 37-year-old woman comes to the physician because of difficulty swallowing for the past 1 year. She was diagnosed with gastroesophageal reflux 3 years ago and takes pantoprazole. She has smoked a pack of cigarettes daily for 14 years. Examination shows hardening of the skin of the fingers and several white papules on the fingertips. There are small dilated blood vessels on the face. Which of the following is the most likely cause of this patient's difficulty swallowing?
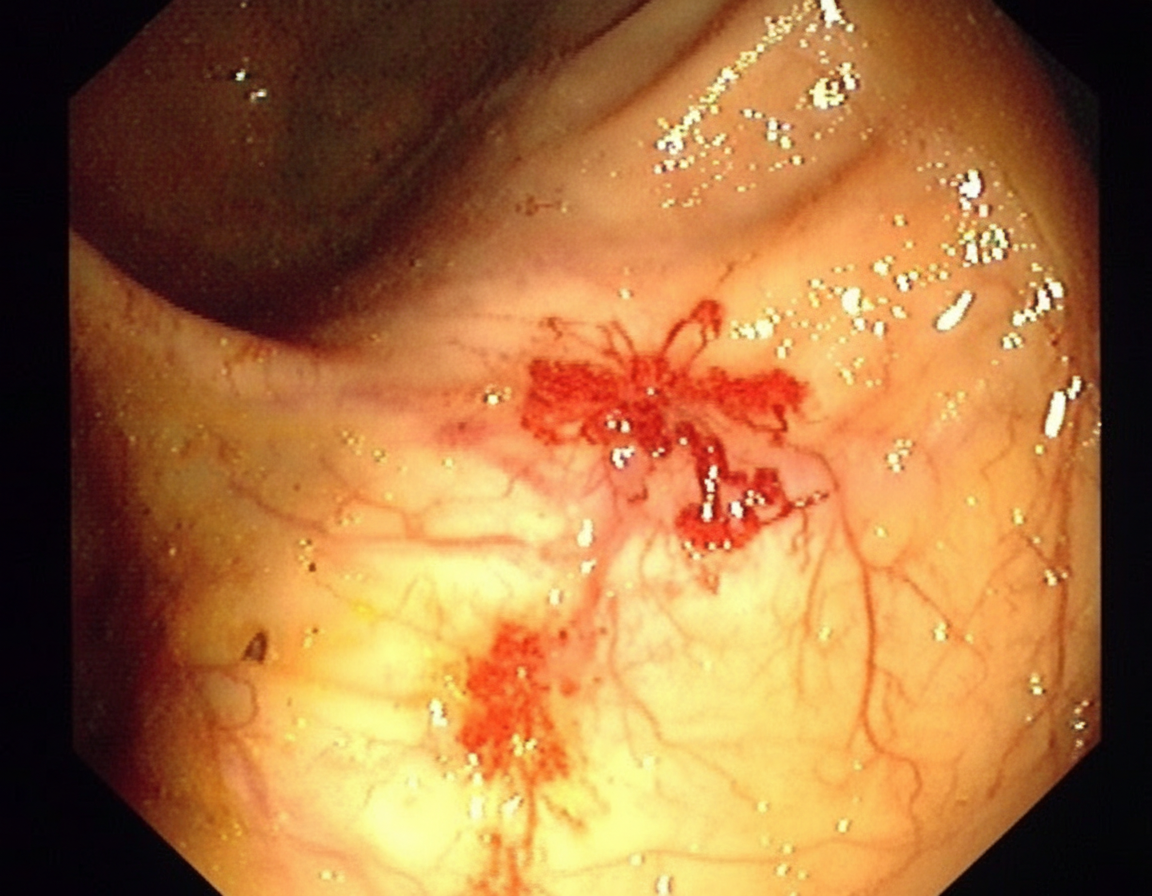
A 70-year-old man comes to the clinic for generalized fatigue. He says that he is more tired than before and has difficulty catching his breath while walking upstairs. He feels tired quickly doing his usual activity such as gardening and shopping. He does not have any symptoms of fever, change in bowel habits, abdominal pain, rectal bleeding, or weight loss. His appetite is normal. His last colonoscopy was done 10 years ago and it was normal. His blood pressure is 116/74 and heart rate is 87/min. On physical examination, his conjunctivae are pale. A routine blood test shows iron deficiency anemia with hemoglobin of 10 gm/dL. His stool is positive for occult blood. He is then sent for a colonoscopy (image is shown). What is the most likely diagnosis for the above condition?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
