Gastroenterology — MCQs

On this page
A 45-year-old woman presents to the clinic with a variety of complaints on different areas of her body, including telangiectasias on both the upper and lower extremities, bluish discoloration of the fingertips when exposed to cold, and burning midsternal chest pain. She is a tobacco smoker and works as a school teacher. After evaluation, an anti-centromere antibody test is ordered, and returns with an elevated titer. Which of the following symptoms are least likely to be seen in this patient's condition?
A 25-year-old man presents to the emergency department after numerous episodes of vomiting. The patient states that he thinks he ‘ate something weird’ and has been vomiting for the past 48 hours. He says that he came to the hospital because the last few times he "threw up blood". He is hypotensive with a blood pressure of 90/55 mm Hg and a pulse of 120/min. After opening an intravenous line, a physical examination is performed which is normal except for mild epigastric tenderness. An immediate endoscopy is performed and a tear involving the mucosa and submucosa of the gastroesophageal junction is visualized. Which of the following is the most likely diagnosis?
A 55-year-old man presents to his primary care physician for trouble swallowing. The patient claims that he used to struggle when eating food if he did not chew it thoroughly, but now he occasionally struggles with liquids as well. He also complains of a retrosternal burning sensation whenever he eats. He also claims that he feels his throat burns when he lays down or goes to bed. Otherwise, the patient has no other complaints. The patient has a past medical history of obesity, diabetes, constipation, and anxiety. His current medications include insulin, metformin, and lisinopril. On review of systems, the patient endorses a 5 pound weight loss recently. The patient has a 22 pack-year smoking history and drinks alcohol with dinner. His temperature is 99.5°F (37.5°C), blood pressure is 177/98 mmHg, pulse is 90/min, respirations are 17/min, and oxygen saturation is 98% on room air. On physical exam, you note an overweight man in no current distress. Abdominal exam is within normal limits. Which of the following is the best next step in management?
A 33-year-old HIV-positive male is seen in clinic for follow-up care. When asked if he has been adhering to his HIV medications, the patient exclaims that he has been depressed, thus causing him to not take his medication for six months. His CD4+ count is now 33 cells/mm3. What medication(s) should he take in addition to his anti-retroviral therapy?
A 42-year-old man presents to the physician with a painful ulcer in the mouth for 1 week. He has had similar episodes of ulcers over the past year. Every episode lasts about a week and heals without leaving a scar. He has also had similar ulcers on the scrotum, but the ulcers have left scars. He takes no medications. His temperature is 36.8°C (98.2°F), and the rest of the vital signs are stable. On physical examination, a 1-cm yellowish ulcer with a necrotic base is seen on the right buccal mucosa. Also, there are several tender nodules of different sizes on both shins. An image of one of the nodules is shown. Which of the following is the most likely complication of this patient’s current condition?
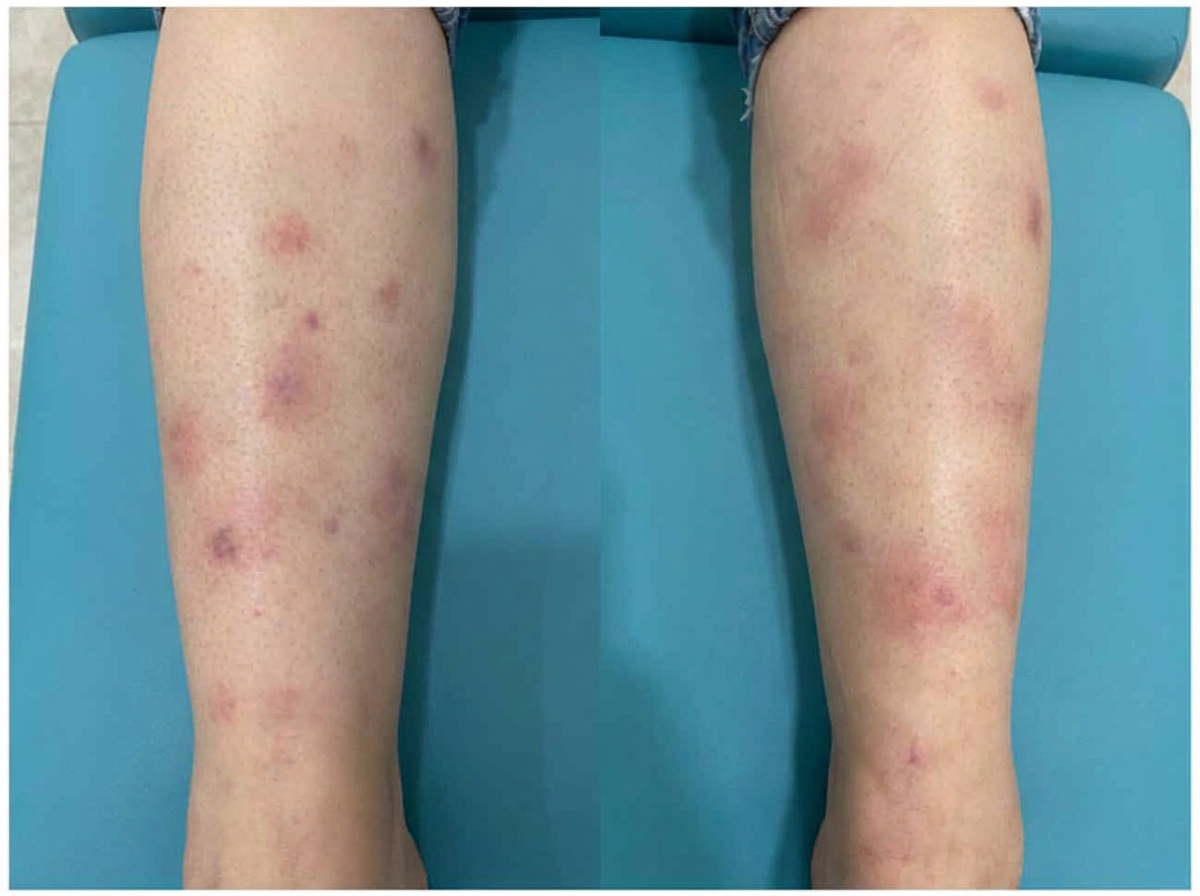
A 45-year-old male presents to his primary care physician complaining of joint pain and stiffness. He reports progressively worsening pain and stiffness in his wrists and fingers bilaterally over the past six months that appears to improve in the afternoon and evening. His past medical history is notable for obesity and diabetes mellitus. He takes metformin and glyburide. His family history is notable for osteoarthritis in his father and psoriasis in his mother. His temperature is 98.6°F (37°C), blood pressure is 130/80 mmHg, pulse is 90/min, and respirations are 16/min. On examination, his bilateral metacarpophalangeal joints and proximal interphalangeal joints are warm and mildly edematous. The presence of antibodies directed against which of the following is most specific for this patient’s condition?
A 15-year-old girl is brought to the physician because of an 8-month history of fatigue, intermittent postprandial abdominal bloating and discomfort, foul-smelling, watery diarrhea, and a 7-kg (15-lb) weight loss. She developed a pruritic rash on her knees 3 days ago. Physical examination shows several tense, excoriated vesicles on the knees bilaterally. The abdomen is soft and nontender. Her hemoglobin concentration is 8.2 g/dL and mean corpuscular volume is 76 μm3. Further evaluation of this patient is most likely to show which of the following findings?
A 26-year-old man presents to his primary doctor with one week of increasing weakness. He reports that he first noticed difficulty walking while attending his sister's graduation last week, and yesterday he had difficulty taking his coffee cup out of the microwave. He remembers having nausea and vomiting a few weeks prior, but other than that has no significant medical history. On exam, he has decreased reflexes in his bilateral upper and lower extremities, with intact sensation. If a lumbar puncture is performed, which of the following results are most likely?
A 52-year-old man presents to the office for evaluation of a 'weird rash' that appeared over his torso last week. The patient states that the rash just seemed to appear, but denies itching, pain, or exposure. On physical examination, the patient has multiple light brown-colored flat plaques on the torso. They appear to be 'stuck on' but do not have associated erythema or swelling. What condition is this clinical presentation most likely associated with?
A 66-year-old woman presents to her primary care physician with complaints of constipation and left lower abdominal discomfort. She says the pain usually gets worse after meals, which is felt as a dull pain. Her past medical history is positive for gastroesophageal reflux disease, for which she takes omeprazole. There is a positive history of chronic constipation but no episodes of bloody stools. On physical examination, she has a temperature of 38.5°C (101.3°F), blood pressure of 110/70 mm Hg, heart rate of 100/min, and respiratory rate of 19/min. Stool occult blood is negative. Which of the following is the most appropriate study to be performed at this stage?
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
