GERD and esophageal disorders — MCQs

A scientist is studying the mechanism by which the gastrointestinal system coordinates the process of food digestion. Specifically, she is interested in how distension of the lower esophagus by a bolus of food changes responses in the downstream segments of the digestive system. She observes that there is a resulting relaxation and opening of the lower esophageal (cardiac) sphincter after the introduction of a food bolus. She also observes a simultaneous relaxation of the orad stomach during this time. Which of the following substances is most likely involved in the process being observed here?
A 62-year-old man comes to the office complaining of dysphagia that started 4-5 months ago. He reports that he initially had difficulty swallowing only solid foods. More recently, he has noticed some trouble swallowing liquids. The patient also complains of fatigue, a chronic cough that worsens at night, and burning chest pain that occurs after he eats. He says that he has used over-the-counter antacids for "years" with mild relief. He denies any change in diet, but says he has "gone down a pant size or 2." The patient has hypertension and hyperlipidemia. He takes amlodipine and atorvastatin. He smoked 1 pack of cigarettes a day for 12 years while in the military but quit 35 years ago. He drinks 1-2 beers on the weekend while he is golfing with his friends. His diet consists mostly of pasta, pizza, and steak. The patient's temperature is 98°F (36.7°C), blood pressure is 143/91 mmHg, and pulse is 80/min. His BMI is 32 kg/m^2. Physical examination reveals an obese man in no acute distress. No masses or enlarged lymph nodes are appreciated upon palpation of the neck. Cardiopulmonary examination is unremarkable. An endoscopy is performed, which identifies a lower esophageal mass. Which of the following is the most likely diagnosis?
A 62-year-old man is referred to a gastroenterologist because of difficulty swallowing for the past 5 months. He has difficulty swallowing both solid and liquid foods, but there is no associated pain. He denies any shortness of breath or swelling in his legs. He immigrated from South America 10 years ago. He is a non-smoker and does not drink alcohol. His physical examination is unremarkable. A barium swallow study was ordered and the result is given below. Esophageal manometry confirms the diagnosis. What is the most likely underlying cause of this patient’s condition?
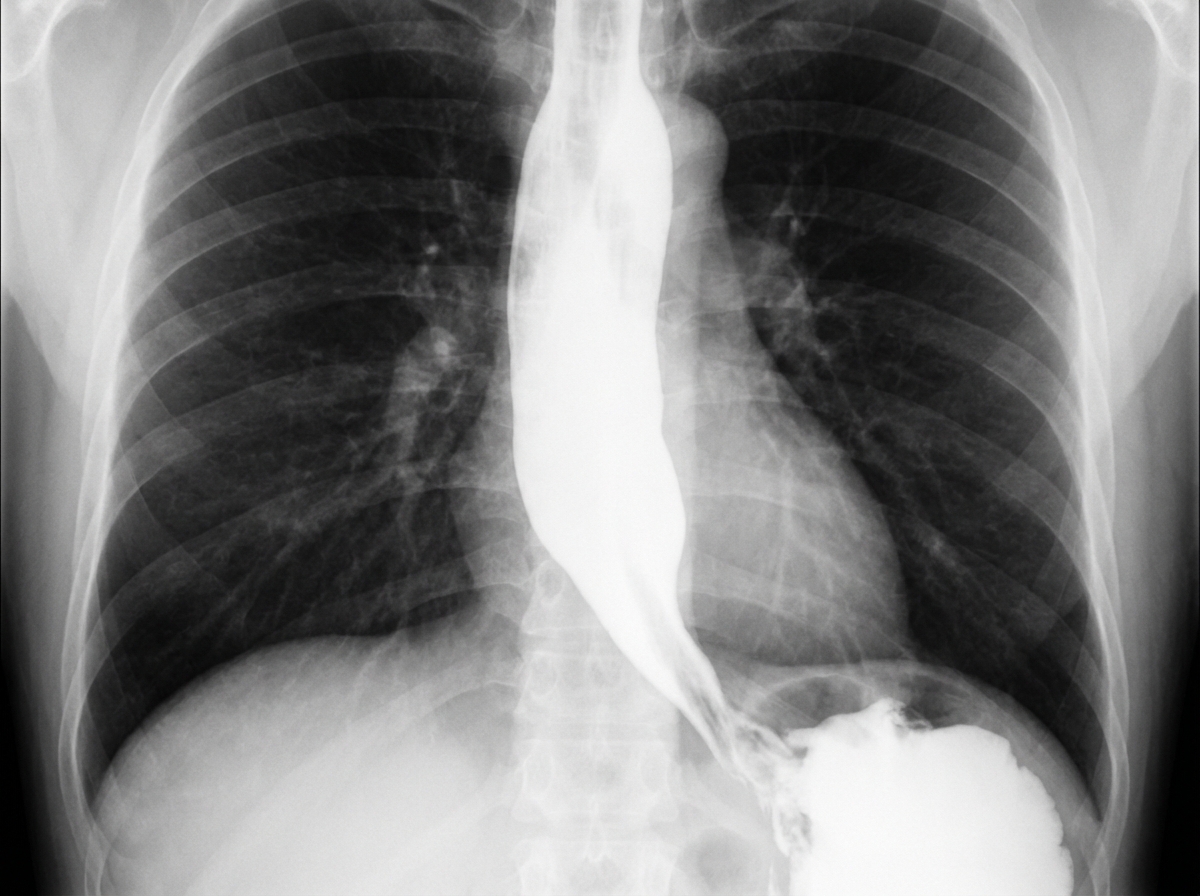
A 45-year-old man presents to the emergency department with difficulties swallowing food. He states that he experiences pain when he attempts to swallow his medications or when he drinks water. He reveals that he was diagnosed with HIV infection five years ago. He asserts that he has been taking his antiretroviral regimen, including emtricitabine, rilpivirine, and tenofovir. His temperature is 98°F (37°C), blood pressure is 100/60 mmHg, pulse is 90/min, respirations are 22/min, and oxygen saturation is 99% on room air. His physical exam is notable for a clear oropharynx, no lymphadenopathy, and a normal cardiac and pulmonary exam. No rashes are noted throughout his body. His laboratory results are displayed below: Hemoglobin: 12 g/dL Hematocrit: 37 % Leukocyte count: 8,000/mm^3 with normal differential Platelet count: 160,000/mm^3 Serum: Na+: 138 mEq/L Cl-: 108 mEq/L K+: 3.5 mEq/L HCO3-: 26 mEq/L BUN: 35 mg/dL Glucose: 108 mg/dL Creatinine: 1.1 mg/dL CD4+ count: 90/mm^3 HIV viral load: 59,000 copies/mL What is the best next step in management?
A 27-year-old woman presents with painful swallowing for the past 2 days. She received a kidney transplant 3 months ago for lupus-induced end-stage renal disease. She takes tacrolimus, mycophenolate mofetil, prednisone, and calcium supplements. The blood pressure is 120/80 mm Hg, the pulse is 72/min, the respirations are 14/min, and the temperature is 38.0°C (100.4°F). Esophagoscopy shows serpiginous ulcers in the distal esophagus with normal surrounding mucosa. Biopsy shows large cytoplasmic inclusion bodies. Which of the following is the most appropriate pharmacotherapy at this time?
A 56-year-old woman presents to her primary care physician complaining of heartburn, belching, and epigastric pain that is aggravated by coffee and fatty foods. She states that she has recently been having difficulty swallowing in addition to her usual symptoms. What is the most appropriate next step in management of this patient?
A 47-year-old man with gastroesophageal reflux disease comes to the physician because of severe burning chest pain and belching after meals. He has limited his caffeine intake and has been avoiding food close to bedtime. Esophagogastroduodenoscopy shows erythema and erosions in the distal esophagus. Which of the following is the mechanism of action of the most appropriate drug for this patient?
A 55-year-old man comes to the physician because of heartburn for the past 2 years. He has no chest pain, dysphagia, weight loss, or fever. He has no history of any serious illnesses. He takes omeprazole daily. Vital signs are within normal limits. Body mass index (BMI) is 34 kg/m2. Physical exam shows no abnormalities. An endoscopic image of the lower esophageal sphincter is shown. Which of the following is the most important next step in management?
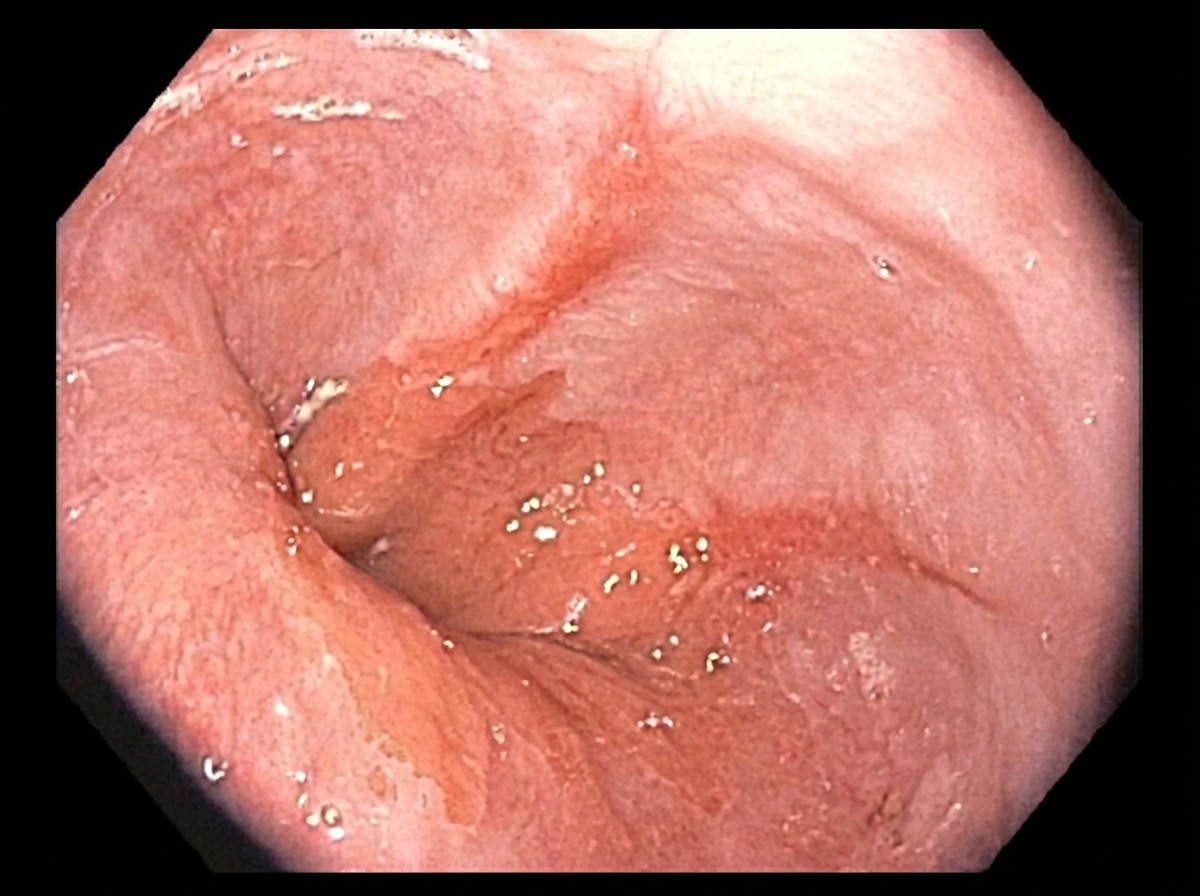
A 45-year-old African American male presents to his primary care physician complaining of difficulty swallowing that was initially limited to solids but has now progressed to liquids. Biopsy of the esophagus reveals dysplastic cells, but does not show evidence of glands or increased mucin. Which of the following most contributed to his condition?
A 28-year-old male presents to his primary care physician with complaints of intermittent abdominal pain and alternating bouts of constipation and diarrhea. His medical chart is not significant for any past medical problems or prior surgeries. He is not prescribed any current medications. Which of the following questions would be the most useful next question in eliciting further history from this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
