Diverticular disease — MCQs

A 62-year-old man presents to the emergency department with acute pain in the left lower abdomen and profuse rectal bleeding. These symptoms started 3 hours ago. The patient has chronic constipation and bloating, for which he takes lactulose. His family history is negative for gastrointestinal disorders. His temperature is 38.2°C (100.8°F), blood pressure is 90/60 mm Hg, and pulse is 110/min. On physical examination, the patient appears drowsy, and there is tenderness with guarding in the left lower abdominal quadrant. Flexible sigmoidoscopy shows multiple, scattered diverticula with acute mucosal inflammation in the sigmoid colon. Which of the following is the best initial treatment for this patient?
A 46-year-old woman comes to the emergency department because of intermittent abdominal pain and vomiting for 2 days. The abdominal pain is colicky and diffuse. The patient's last bowel movement was 3 days ago. She has had multiple episodes of upper abdominal pain that radiates to her scapulae and vomiting over the past 3 months; her symptoms subsided after taking ibuprofen. She has coronary artery disease, type 2 diabetes mellitus, gastroesophageal reflux disease, and osteoarthritis of both knees. Current medications include aspirin, atorvastatin, rabeprazole, insulin, and ibuprofen. She appears uncomfortable. Her temperature is 39°C (102.2°F), pulse is 111/min, and blood pressure is 108/68 mm Hg. Examination shows dry mucous membranes. The abdomen is distended and tympanitic with diffuse tenderness; bowel sounds are high-pitched. Rectal examination shows a collapsed rectum. Her hemoglobin concentration is 13.8 g/dL, leukocyte count is 14,400/mm3, and platelet count is 312,000/mm3. An x-ray of the abdomen is shown. Which of the following is the most likely cause of this patient's findings?
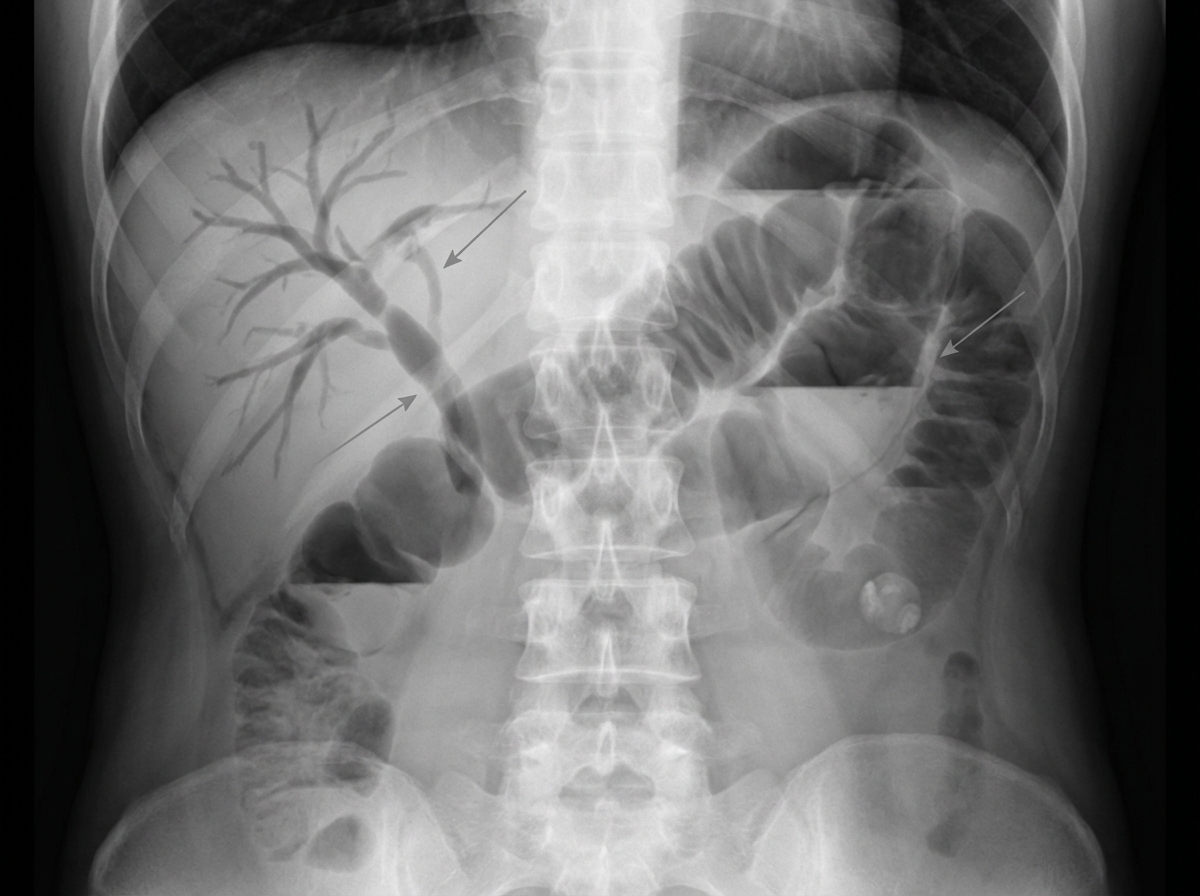
A 75-year-old man presents to the emergency department for abdominal pain. The patient states the pain started this morning and has been worsening steadily. He decided to come to the emergency department when he began vomiting. The patient has a past medical history of obesity, diabetes, alcohol abuse, and hypertension. His current medications include captopril, insulin, metformin, sodium docusate, and ibuprofen. His temperature is 104.0°F (40°C), blood pressure is 160/97 mmHg, pulse is 90/min, respirations are 15/min, and oxygen saturation is 98% on room air. Abdominal exam reveals left lower quadrant tenderness. Cardiac exam reveals a crescendo systolic murmur heard best by the right upper sternal border. Lab values are ordered and return as below. Hemoglobin: 15 g/dL Hematocrit: 42% Leukocyte count: 19,500 cells/mm^3 with normal differential Platelet count: 226,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 101 mEq/L K+: 4.4 mEq/L HCO3-: 24 mEq/L BUN: 22 mg/dL Glucose: 144 mg/dL Creatinine: 1.2 mg/dL Ca2+: 9.8 mg/dL Which of the following is the most accurate test for this patient's condition?
An institutionalized 65-year-old man is brought to the emergency department because of abdominal pain and distension for 12 hours. The pain was acute in onset and is a cramping-type pain associated with nausea, vomiting, and constipation. He has a history of chronic constipation and has used laxatives for years. There is no history of inflammatory bowel disease in his family. He has not been hospitalized recently. There is no recent history of weight loss or change in bowel habits. On physical examination, the patient appears ill. The abdomen is distended with tenderness mainly in the left lower quadrant and is tympanic on percussion. The blood pressure is 110/79 mm Hg, heart rate is 100/min, the respiratory rate is 20/min, and the temperature is 37.2°C (99.0°F). The CBC shows an elevated white blood cell count. The plain abdominal X-ray is shown in the accompanying image. What is the most likely cause of his condition?
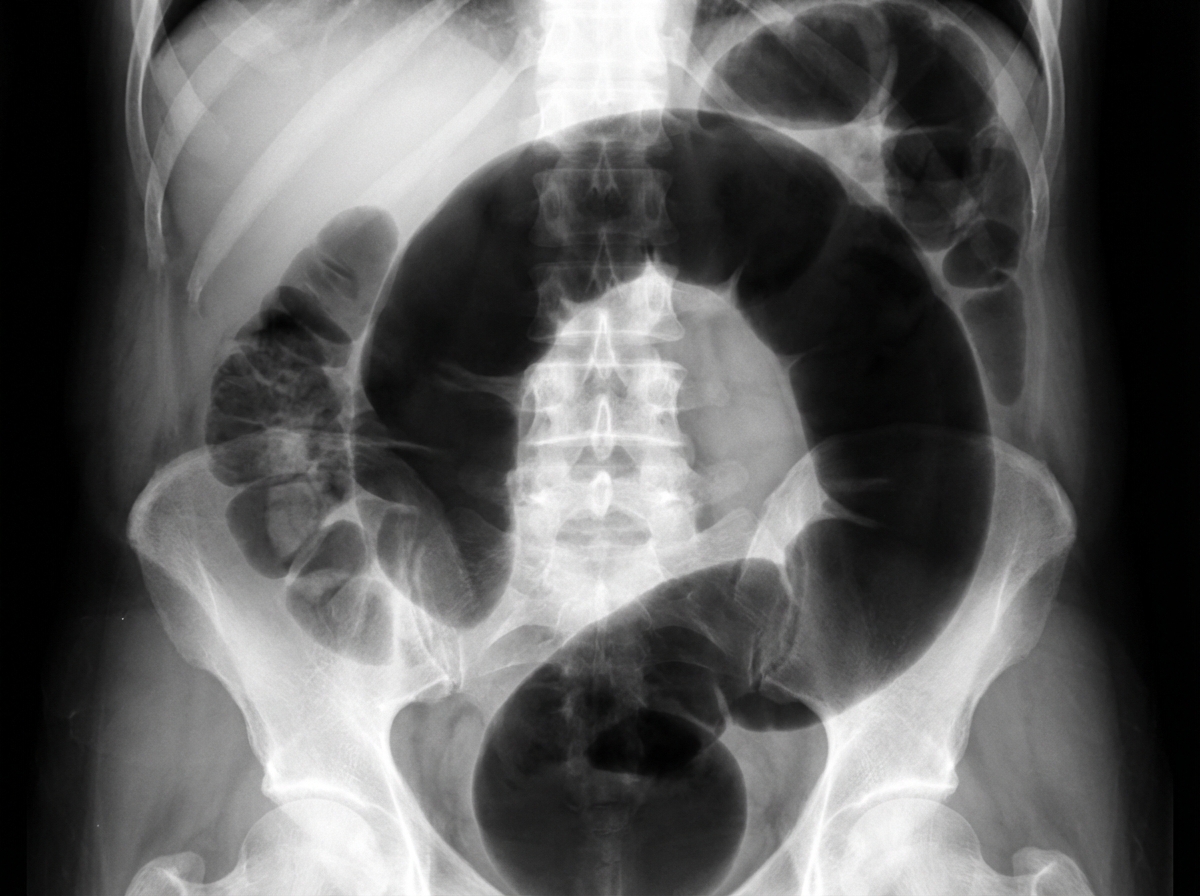
A 24-year-old man presents to the emergency department for severe abdominal pain for the past day. The patient states he has had profuse, watery diarrhea and abdominal pain that is keeping him up at night. The patient also claims that he sees blood on the toilet paper when he wipes and endorses having lost 5 pounds recently. The patient's past medical history is notable for IV drug abuse and a recent hospitalization for sepsis. His temperature is 99.5°F (37.5°C), blood pressure is 120/68 mmHg, pulse is 100/min, respirations are 14/min, and oxygen saturation is 98% on room air. On physical exam, you note a young man clutching his abdomen in pain. Abdominal exam demonstrates hyperactive bowel sounds and diffuse abdominal tenderness. Cardiopulmonary exam is within normal limits. Which of the following is the next best step in management?
A 65-year-old man comes to the physician because of abdominal pain and bloody, mucoid diarrhea for 3 days. He has been taking over-the-counter supplements for constipation over the past 6 months. He was diagnosed with type 2 diabetes mellitus 15 years ago. He has smoked one pack of cigarettes daily for 35 years. His current medications include metformin. His temperature is 38.4°C (101.1°F), pulse is 92/min, and blood pressure is 134/82 mm Hg. Examination of the abdomen shows no masses. Palpation of the left lower abdomen elicits tenderness. A CT scan of the abdomen is shown. Which of the following is the most likely underlying cause of the patient's condition?
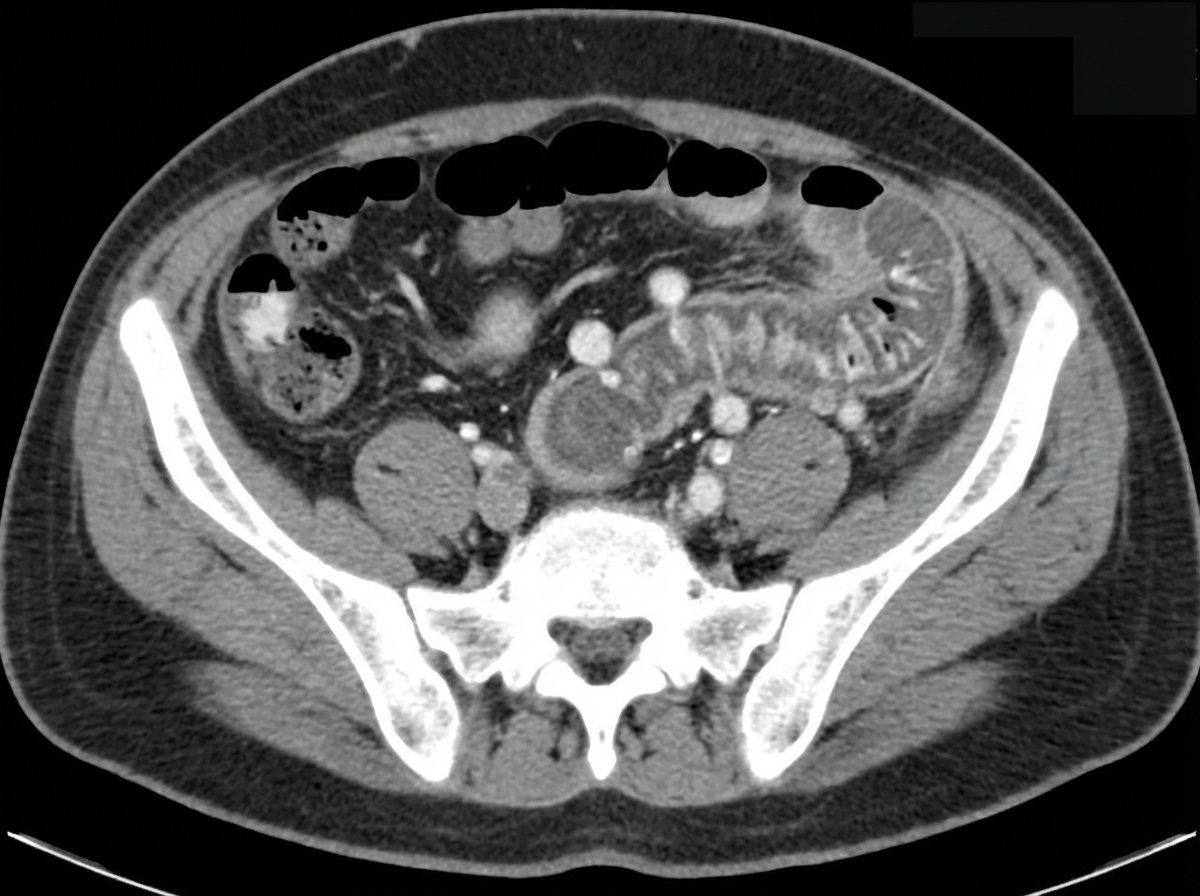
Please refer to the summary above to answer this question Which of the following is the most likely diagnosis? Patient information Age: 61 years Gender: F, self-identified Ethnicity: unspecified Site of care: emergency department History Reason for Visit/Chief Concern: "My belly really hurts." History of Present Illness: developed abdominal pain 12 hours ago pain constant; rated at 7/10 has nausea and has vomited twice has had two episodes of nonbloody diarrhea in the last 4 hours 12-month history of intermittent constipation reports no sick contacts or history of recent travel Past medical history: hypertension type 2 diabetes mellitus mild intermittent asthma allergic rhinitis Social history: diet consists mostly of high-fat foods does not smoke drinks 1–2 glasses of wine per week does not use illicit drugs Medications: lisinopril, metformin, albuterol inhaler, fexofenadine, psyllium husk fiber Allergies: no known drug allergies Physical Examination Temp Pulse Resp. BP O2 Sat Ht Wt BMI 38.4°C (101.1°F) 85/min 16/min 134/85 mm Hg – 163 cm (5 ft 4 in) 94 kg (207 lb) 35 kg/m2 Appearance: lying back in a hospital bed; appears uncomfortable Neck: no jugular venous distention Pulmonary: clear to auscultation; no wheezes, rales, or rhonchi Cardiac: regular rate and rhythm; normal S1 and S2; no murmurs, rubs, or gallops Abdominal: obese; soft; tender to palpation in the left lower quadrant; no guarding or rebound tenderness; normal bowel sounds Extremities: no edema; warm and well-perfused Skin: no rashes; dry Neurologic: alert and oriented; cranial nerves grossly intact; no focal neurologic deficits
A 68-year-old female presents to your office for her annual check-up. Her vitals are HR 85, T 98.8 F, RR 16, BP 125/70. She has a history of smoking 1 pack a day for 35 years, but states she quit five years ago. She had her last pap smear at age 64 and states all of her pap smears have been normal. She had her last colonoscopy at age 62, which was also normal. Which of the following is the next best test for this patient?
A 65-year-old man presents to his primary care physician for a yearly checkup. He states he feels he has been in good health other than minor fatigue, which he attributes to aging. The patient has a past medical history of hypertension and is currently taking chlorthalidone. He drinks 1 glass of red wine every night. He has lost 5 pounds since his last appointment 4 months ago. His temperature is 99.2°F (37.3°C), blood pressure is 147/98 mmHg, pulse is 80/min, respirations are 14/min, and oxygen saturation is 99% on room air. Physical exam reveals an obese man in no acute distress. Laboratory values are ordered as seen below. Hemoglobin: 9 g/dL Hematocrit: 27% Mean corpuscular volume: 72 µm^3 Leukocyte count: 6,500/mm^3 with normal differential Platelet count: 193,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 101 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 1.1 mg/dL Ca2+: 9.0 mg/dL AST: 32 U/L ALT: 20 U/L 25-OH vitamin D: 15 ng/mL Which of the following is the best next step in management?
A 26-year-old white man comes to the physician because of increasing generalized fatigue for 6 months. He has been unable to work out at the gym during this period. He has also had cramping lower abdominal pain and diarrhea for the past 5 weeks that is occasionally bloody. His father was diagnosed with colon cancer at the age of 65. He has smoked half a pack of cigarettes daily for the past 10 years. He drinks 1–2 beers on social occasions. His temperature is 37.3°C (99.1°F), pulse is 88/min, and blood pressure is 116/74 mm Hg. Physical examination shows dry mucous membranes. The abdomen is soft and nondistended with slight tenderness to palpation over the lower quadrants bilaterally. Rectal examination shows stool mixed with blood. His hemoglobin concentration is 13.5 g/dL, leukocyte count is 7,500/mm3, and platelet count is 480,000/mm3. Urinalysis is within normal limits. Which of the following is the most appropriate next step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
