Gastroenterology — MCQs

On this page
A 30-year-old patient presents with loose stools, lower abdominal pain, weight loss, diarrhea and passage of blood and mucus. On sigmoidoscopy this is the presentation of the patient. All of the following statements regarding this condition are true except:
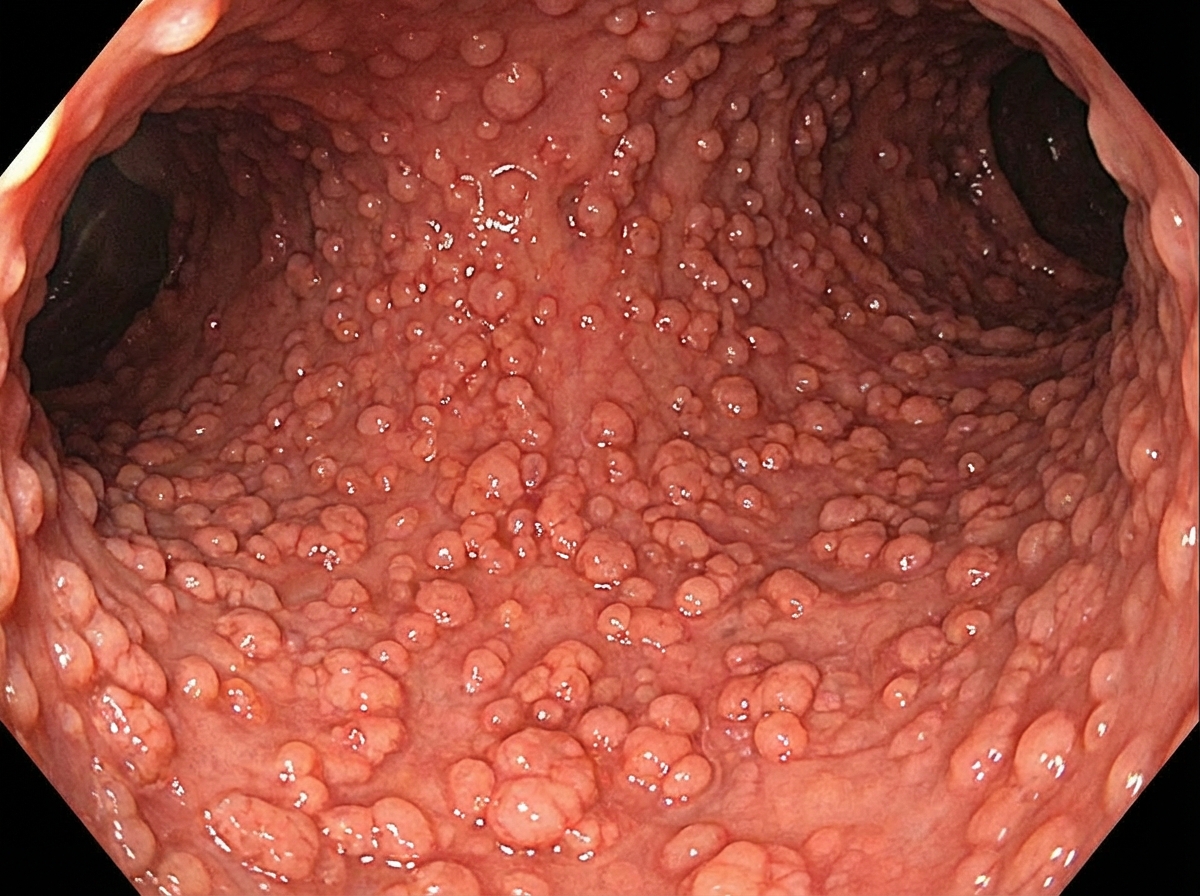
All of the following statements regarding this picture are true except:
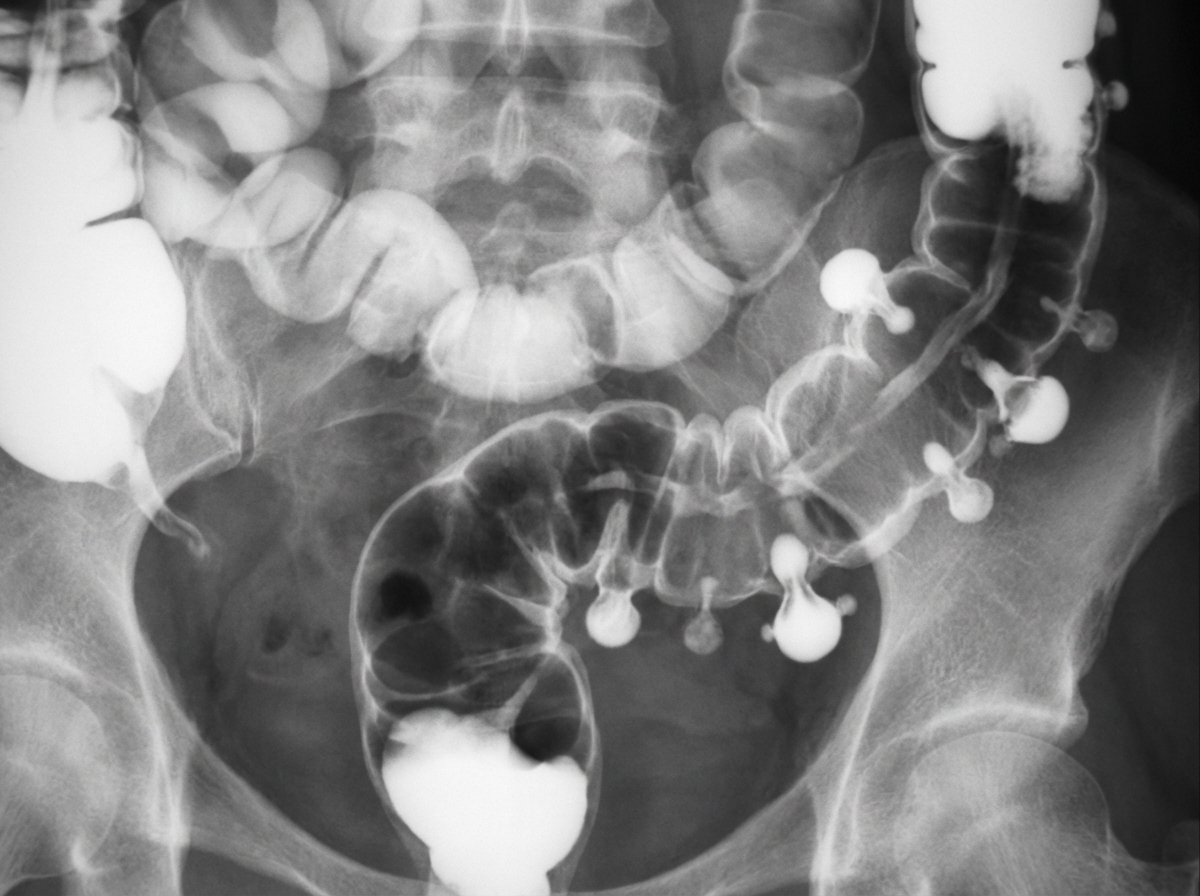
The following pus was drained from a liver abscess. Which complication(s) is/are seen with this condition?

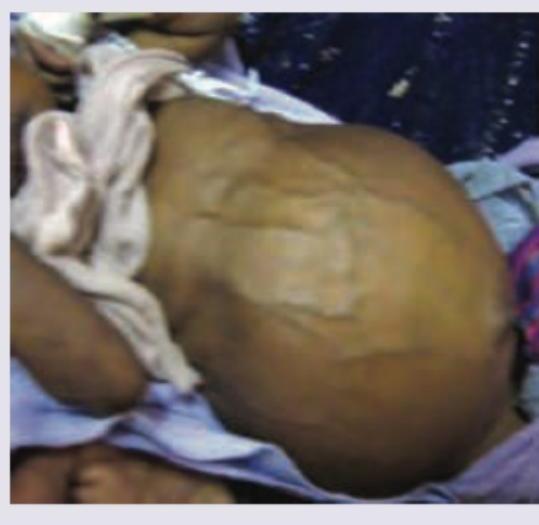
The following pus was drained from a liver abscess. Diagnosis is:

All investigations should be done in this case except:
Practice by Chapter
GERD and esophageal disorders
Practice Questions
Peptic ulcer disease
Practice Questions
Helicobacter pylori infection
Practice Questions
Celiac disease
Practice Questions
Irritable bowel syndrome
Practice Questions
Diverticular disease
Practice Questions
GI bleeding (upper and lower)
Practice Questions
Small intestinal bacterial overgrowth
Practice Questions
Malabsorption syndromes
Practice Questions
Colorectal cancer screening
Practice Questions
Functional GI disorders
Practice Questions
Anorectal disorders
Practice Questions
GI motility disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
