Red flags in skin conditions — MCQs

A 52-year-old woman with type 2 diabetes mellitus comes to the physician because of a 2-day history of blisters on her forearms and pain during sexual intercourse. Her only medications are metformin and glyburide. Examination reveals multiple, flaccid blisters on the volar surface of the forearms and ulcers on the buccal, gingival, and vulvar mucosa. The epidermis on the forearm separates when the skin is lightly stroked. Which of the following is the most likely diagnosis?
A 52-year-old Caucasian man presents to the clinic for evaluation of a mole on his back that he finds concerning. He states that his wife noticed the lesion and believes that it has been getting larger. On inspection, the lesion is 10 mm in diameter with irregular borders. A biopsy is performed. Pathology reveals abnormal melanocytes forming nests at the dermo-epidermal junction and discohesive cell growth into the epidermis. What is the most likely diagnosis?
A 4-year-old boy is presented to the clinic by his mother due to a peeling erythematous rash on his face, back, and buttocks which started this morning. Two days ago, the patient’s mother says his skin was extremely tender and within 24 hours progressed to desquamation. She also says that, for the past few weeks, he was very irritable and cried more than usual during diaper changes. The patient is up to date on his vaccinations and has been meeting all developmental milestones. No significant family history. On physical examination, the temperature is 38.4°C (101.1°F) and the pulse is 70/min. The epidermis separates from the dermis by gentle lateral stroking of the skin. Systemic antibiotics are prescribed, and adequate fluid replacement is provided. Which of the following microorganisms most likely caused this patient’s condition?
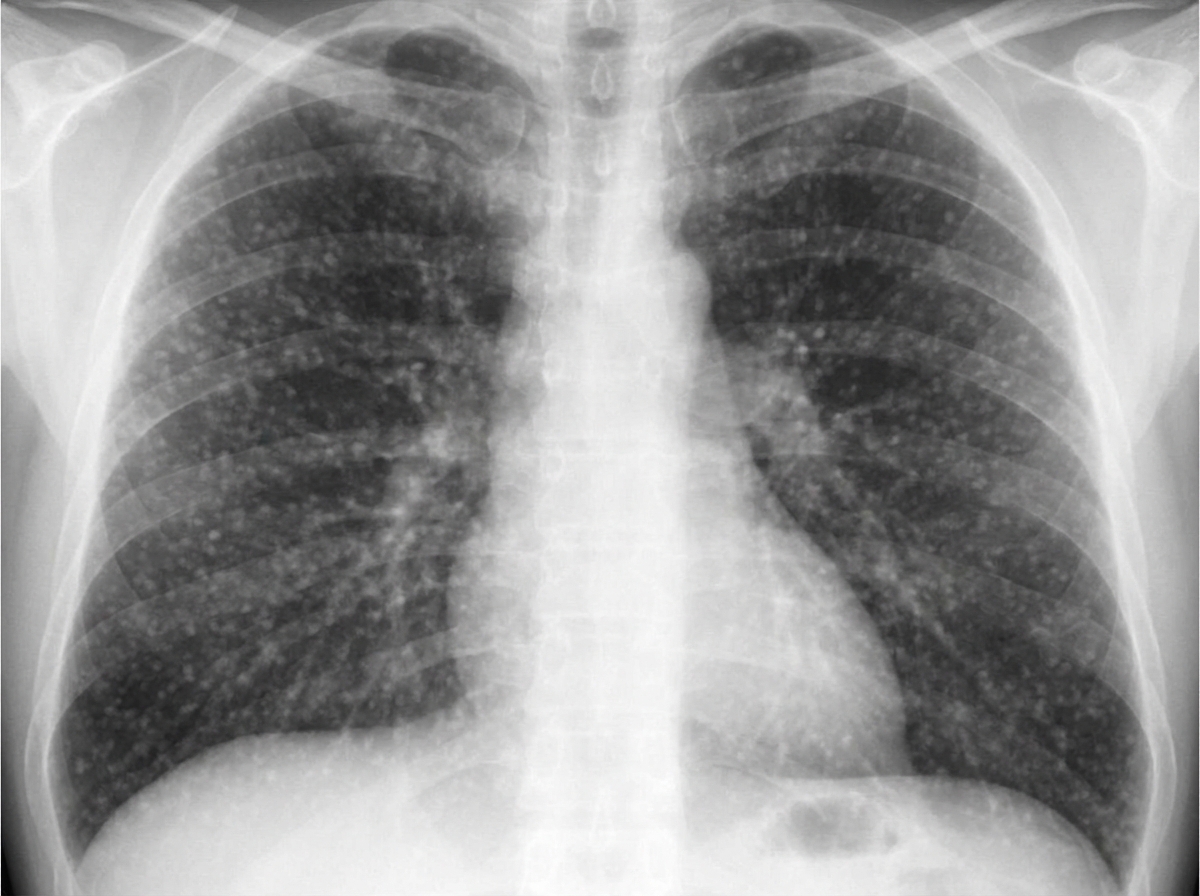
A 68-year-old man presents to the physician with fever, cough, weakness, night sweats, and poor appetite for the past 6 months. Medical records suggest that he has lost 7.5 kg (16.5 lb) of weight during this period. There is no history of breathlessness, nasal discharge, nasal obstruction, palpitations, chest pain, or symptoms related to digestion. He was released from prison 9 months ago after serving a 2-year sentence. His temperature is 38.1°C (100.6°F), pulse is 84/min, respirations are 16/min, and blood pressure is 122/80 mm Hg. Physical examination shows hepatomegaly and generalized lymphadenopathy, and auscultation of the chest reveals diffuse crackles throughout the lung fields bilaterally. On direct ophthalmoscopy, three discrete, yellow-colored, 0.5 mm to 1.0 mm lesions with indistinct borders are seen in the posterior pole. A chest X-ray is shown in the image. Tuberculin skin test with purified protein derivative is negative. What is the most likely diagnosis?
A 4-year-old boy is brought to the emergency department by his mother with a rash on his trunk, malaise, and fever with spikes up to 38.5°C (101.3°F) for the past 2 weeks. The patient's mother says she tried giving him Tylenol with little improvement. Past medical history includes a spontaneous vaginal delivery at full term. The patient's vaccines are up-to-date and he has met all developmental milestones. On physical examination, his lips are cracking, and he has painful cervical lymphadenopathy. The rash is morbilliform and involves his trunk, palms, and the soles of his feet. There is fine desquamation of the skin of the perianal region. Which of the following anatomical structures is most important to screen for possible complications in this patient?
A 52-year-old woman sees you in your office with a complaint of new-onset headaches over the past few weeks. On exam, you find a 2 x 2 cm dark, irregularly shaped, pigmented lesion on her back. She is concerned because her father recently passed away from skin cancer. What tissue type most directly gives rise to the lesion this patient is experiencing?
A 45-year-old woman presents to the clinic with a variety of complaints on different areas of her body, including telangiectasias on both the upper and lower extremities, bluish discoloration of the fingertips when exposed to cold, and burning midsternal chest pain. She is a tobacco smoker and works as a school teacher. After evaluation, an anti-centromere antibody test is ordered, and returns with an elevated titer. Which of the following symptoms are least likely to be seen in this patient's condition?
A 49-year-old woman with a history of intravenous drug use comes to the physician because of a 6-month history of fatigue, joint pain, and episodic, painful discoloration in her fingers when exposed to cold weather. She takes no medications. She has smoked one pack of cigarettes daily for the past 22 years. She appears tired. Physical examination shows palpable, nonblanching purpura over the hands and feet. Neurological examination shows weakness and decreased sensation in all extremities. Serum studies show: Alanine aminotransferase 78 U/L Aspartate aminotransferase 90 U/L Urea nitrogen 18 mg/dL Creatinine 1.5 mg/dL Which of the following processes is the most likely explanation for this patient's current condition?
A 48-year-old male presents to his primary physician with the chief complaints of fever, abdominal pain, weight loss, muscle weakness, and numbness in his lower extremities. UA is normal. A biopsy of the sural nerve reveals transmural inflammation and fibrinoid necrosis of small and medium arteries. Chart review reveals a remote history of cigarette smoking as a teenager and Hepatitis B seropositivity. What is the most likely diagnosis?
A 67-year-old man presents to the emergency department with increased fatigue. He states that he has been feeling very tired lately but today lost consciousness while walking up the stairs. He reports mild abdominal distension/discomfort, weight loss, a persistent cough, and multiple episodes of waking up drenched in sweat in the middle of the night. The patient does not see a primary care physician but admits to smoking 2 to 3 packs of cigarettes per day and drinking 1 to 3 alcoholic beverages per day. He recently traveled to Taiwan and Nicaragua. His temperature is 99.5°F (37.5°C), blood pressure is 177/98 mmHg, pulse is 100/min, respirations are 17/min, and oxygen saturation is 98% on room air. On physical exam, you note a fatigued appearing elderly man who is well-groomed. Cardiopulmonary exam reveals mild expiratory wheezes. Abdominal exam is notable for a non-pulsatile mass in the left upper quadrant. Laboratory values are ordered as seen below. Hemoglobin: 12 g/dL Hematocrit: 36% Leukocyte count: 105,500/mm^3 Platelet count: 197,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 92 mg/dL Creatinine: 1.4 mg/dL Ca2+: 10.2 mg/dL Leukocyte alkaline phosphatase score: 25 (range 20 - 100) AST: 12 U/L ALT: 17 U/L Which of the following is the most likely diagnosis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
