Differential diagnosis — MCQs

On this page
A 27-year-old woman presents to her primary care physician for foot pain. The patient states that she has pain in her foot and toes whenever she exerts herself or is at work. The patient is an executive at a medical device company and works 60 hours/week. She is currently training for a marathon. She has a past medical history of anxiety, constipation, and irritable bowel syndrome. Her current medications include clonazepam, sodium docusate, and hyoscyamine. Her temperature is 99.5°F (37.5°C), blood pressure is 100/60 mmHg, pulse is 50/min, respirations are 10/min, and oxygen saturation is 99% on room air. Cardiac and pulmonary exams are within normal limits. Examination of the lower extremity reveals 5/5 strength with 2+ reflexes. Palpation of the interdigital space between the third and fourth toes elicits pain and a clicking sound. Which of the following is the most likely diagnosis?
A 52-year-old man is brought to the emergency department with severe epigastric discomfort and left-sided chest pain radiating to the back that began after waking up. He has also vomited several times since the pain began. He underwent an esophagogastroduodenoscopy the previous day for evaluation of epigastric pain. He has ischemic heart disease and underwent a coronary angioplasty 3 years ago. His mother died of pancreatic cancer when she was 60 years old. His current medications include aspirin, clopidogrel, metoprolol, ramipril, and rosuvastatin. He is pale, anxious, and diaphoretic. His temperature is 37.9°C (100.2°F), pulse is 140/min, respirations are 20/min, and blood pressure is 100/60 mm Hg in his upper extremities and 108/68 mm Hg in his lower extremities. Pulse oximetry on room air shows oxygen saturation at 98%. An S4 is audible over the precordium, in addition to crepitus over the chest. Abdominal examination shows tenderness to palpation in the epigastric area. Serum studies show an initial Troponin I level of 0.031 ng/mL (N < 0.1 ng/mL) and 0.026 ng/mL 6 hours later. A 12-lead ECG shows sinus tachycardia with nonspecific ST-T changes. Which of the following is the most likely diagnosis?
A 58-year-old woman comes to the physician because of a 2-year history of progressively worsening pain in her knees and fingers. The knee pain is worse when she walks for longer than 30 minutes. When she wakes up in the morning, her fingers and knees are stiff for about 15 minutes. She cannot recall any trauma to the joints. She was treated with amoxicillin following a tick bite 2 years ago. She is otherwise healthy and only takes a multivitamin and occasionally acetaminophen for the pain. She drinks 1–2 glasses of wine daily. She is 160 cm (5 ft 3 in) tall and weighs 79 kg (174 lb); BMI is 31 kg/m2. Her temperature is 36.9°C (98.4°F), pulse is 70/min, and blood pressure is 133/78 mm Hg. Examination of the lower extremities reveals mild genu varum. Range of motion of both knees is limited; there is palpable crepitus. Complete flexion and extension elicit pain. Tender nodules are present on the proximal and distal interphalangeal joints of the index, ring, and little fingers bilaterally. Which of the following is the most likely diagnosis?
A 15-year-old Caucasian female presents with Parkinson-like symptoms. Serum analysis shows increased levels of free copper and elevated liver enzymes. What test would prove most helpful in diagnosing the patient's underlying disease?
A 67-year-old man presents to his primary care physician for fatigue. This has persisted for the past several months and has been steadily worsening. The patient has a past medical history of hypertension and diabetes; however, he is not currently taking any medications and does not frequently visit his physician. The patient has lost 20 pounds since his last visit. His laboratory values are shown below: Hemoglobin: 9 g/dL Hematocrit: 29% Mean corpuscular volume: 90 µm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L Ca2+: 11.8 mg/dL Which of the following is the most likely diagnosis?
A 45-year-old African-American woman presents with dyspnea, cough, and non-radiating chest pain. Her chest pain is relieved by leaning forward and worsens upon leaning backwards. A scratchy rub is heard best with the patient leaning forward. Physical examination did not elucidate evidence of a positive Kussmaul's sign, pulsus paradoxus, or pericardial knock. The patient most likely is suffering from which of the following?
A 34-year-old G2P1 female at 37 weeks of gestation presents to the clinic for complaints of right-hand numbness and pain for the past month. She reports that the pain is usually worse at night and that she would sometimes wake up in the middle of the night from the “pins and needles.” She denies fever, weakness, or weight changes but endorses paresthesia and pain. The patient also reports a fall on her right hand 2 weeks ago. A physical examination demonstrates mild sensory deficits at the first 3 digits of the right hand but no tenderness with palpation. Strength is intact throughout. Which of the following findings would further support the diagnosis of this patient’s condition?
A 35-year-old woman comes to the physician because of progressive left flank pain and increased urinary frequency for the past two weeks. Her appetite is normal and she has not had any nausea or vomiting. She has a history of type 1 diabetes mellitus that is poorly controlled with insulin. She is sexually active with her boyfriend, and they use condoms inconsistently. Her temperature is 38° C (100.4° F), pulse is 90/min, and blood pressure is 120/80 mm Hg. The abdomen is soft and there is tenderness to palpation in the left lower quadrant; there is no guarding or rebound. There is tenderness to percussion along the left flank. She complains of pain when her left hip is passively extended. Her leukocyte count is 16,000/mm3 and urine pregnancy test is negative. Urinalysis shows 3+ glucose. An ultrasound of the abdomen shows no abnormalities. Which of the following is the most likely diagnosis?
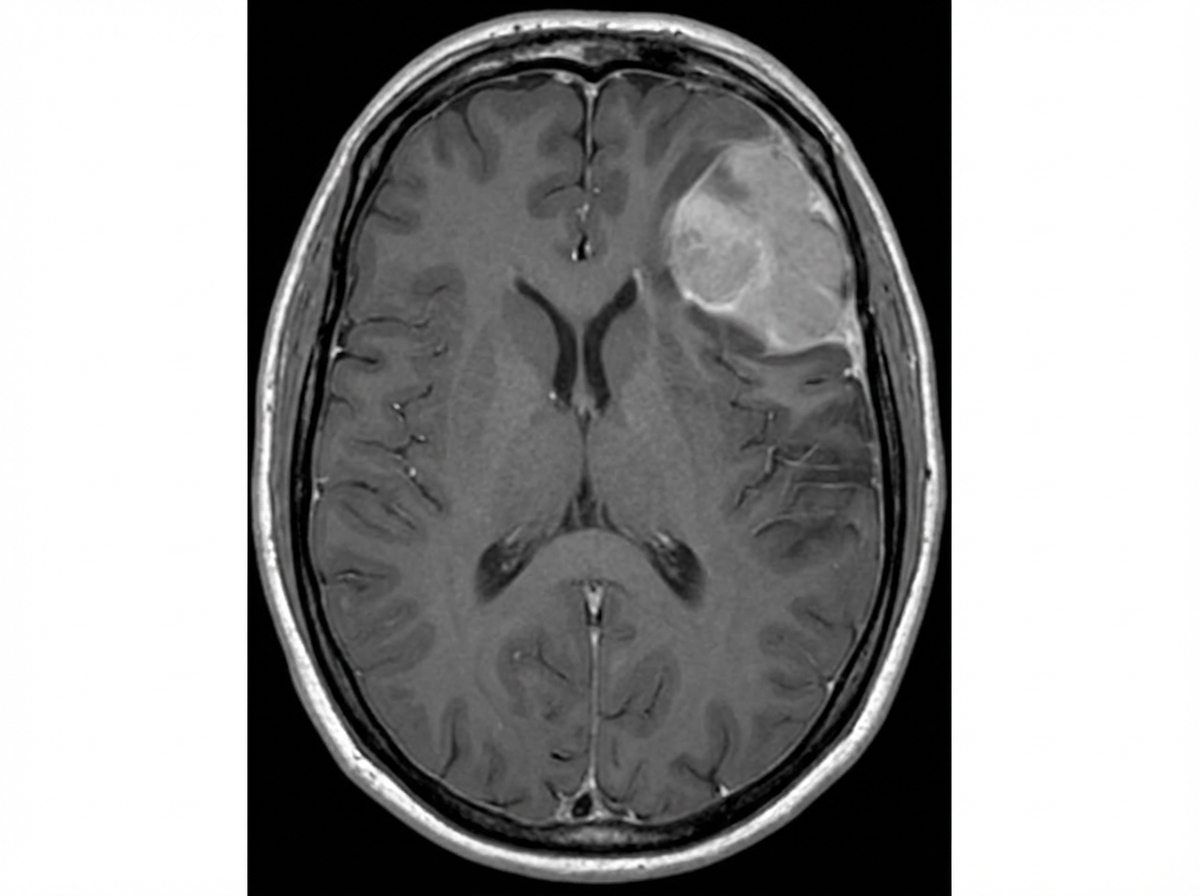
A 59-year-old man is brought to the emergency department 30 minutes after having a seizure. His wife reports that the patient has been having recurrent headaches and has become increasingly irritable over the past 3 months. Physical examination shows a spastic paresis of the right lower extremity. The Babinski sign is present on the right side. An MRI of the brain is shown. Which of the following is the most likely diagnosis?
A 75-year-old man presents to the physician because of bloody urine, which has occurred several times over the past month. He has no dysuria, flank pain, nausea, or vomiting. He has no history of serious illness and takes no medications. He is a 40-pack-year smoker. The vital signs are within normal limits. Physical exam shows no abnormalities except generalized lung wheezing. The laboratory test results are as follows: Urine Blood 3+ RBC > 100/hpf WBC 1–2/hpf RBC casts Negative Bacteria Not seen Which of the following is the most appropriate diagnostic study at this time?
Practice by Chapter
Symptom-based differential diagnosis approach
Practice Questions
System-based differential construction
Practice Questions
Probability ranking in differentials
Practice Questions
Common vs rare disease considerations
Practice Questions
Age and demographic considerations
Practice Questions
Pattern recognition in diagnosis
Practice Questions
Anatomical approach to differential diagnosis
Practice Questions
Syndrome recognition
Practice Questions
Refinement of differential with testing
Practice Questions
Interpreting diagnostic ambiguity
Practice Questions
Ruling in vs ruling out strategies
Practice Questions
Cognitive biases in differential construction
Practice Questions
Integration of diagnostic information
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
