Differential diagnosis — MCQs

On this page
A female presents with a 1 × 1 cm thyroid swelling. What is the next best step in management?
What is the most appropriate initial investigation for a solitary thyroid nodule (STN)?
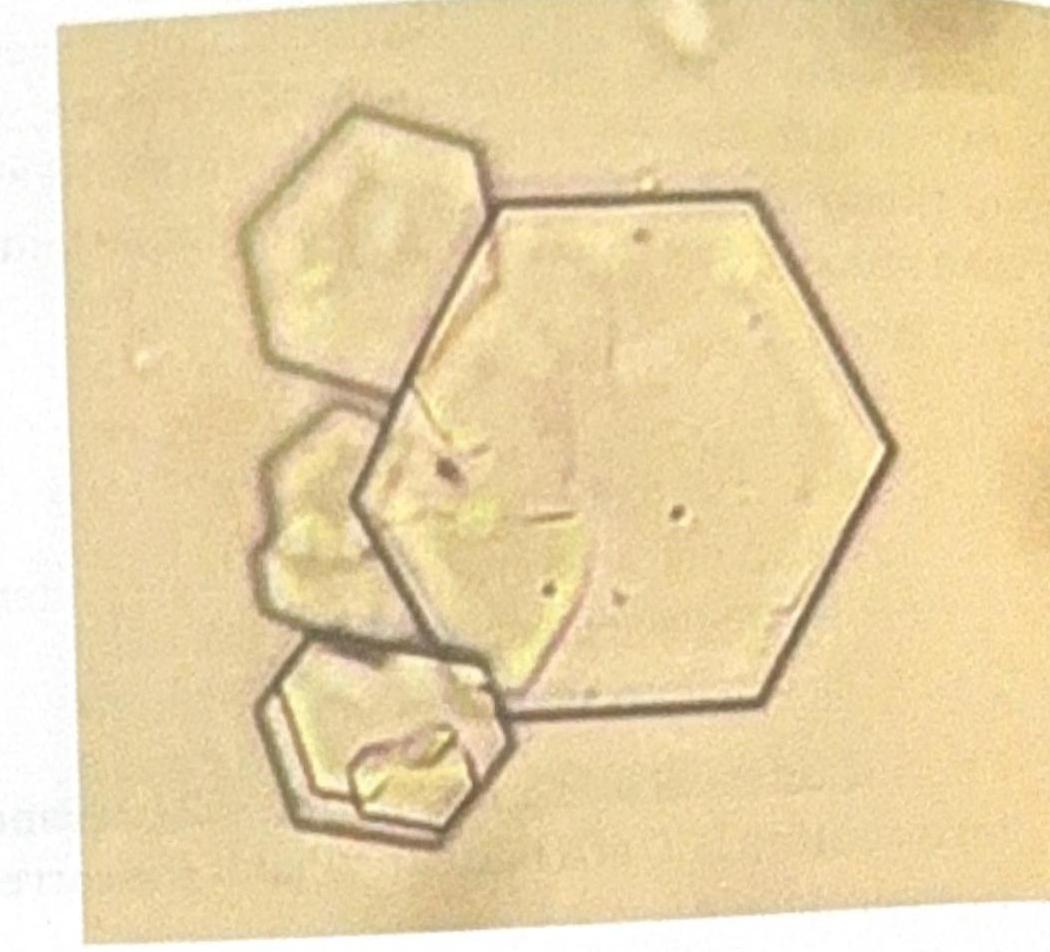
A young patient presents to the OPD with recurrent colicky abdominal pain. Urine examination shows the presence of red blood cells (RBCs) and the following crystal shape in the figure. What is the most likely diagnosis?
An 11-year-old boy is brought to the emergency department 30 minutes after he was found screaming and clutching his head. He has had nausea and occasional episodes of vomiting for 1 week, fever and left-sided headaches for 2 weeks, and increasing tooth pain over the past 3 weeks. He has no history of ear or sinus infections. He is in moderate distress. His temperature is 38.7°C (101.7°F), pulse is 170/min, respirations are 19/min, and blood pressure is 122/85 mmHg. He is confused and only oriented to person. The pupils react sluggishly to light. Fundoscopic examination shows papilledema bilaterally. Extraocular movements are normal. Flexion of the neck causes hip flexion. Which of the following is the most likely diagnosis?
A 70-year-old man is brought to the emergency department for the evaluation of worsening upper abdominal pain that he first noticed this morning after waking up. The pain is of tearing and burning quality and radiates to his back. Yesterday, he underwent an upper endoscopy and was diagnosed with gastritis and a large hiatal hernia. He has hypertension, hypercholesteremia, and a left bundle branch block that was diagnosed 5 years ago. The patient's mother died of myocardial infarction at the age of 70 years, and his father died of aortic dissection at the age of 65 years. The patient smoked one pack of cigarettes daily for the past 40 years, but quit 10 years ago. He drinks three beers daily. Current medications include hydrochlorothiazide, amlodipine, atorvastatin, and pantoprazole. The patient appears to be in mild distress. His temperature is 37.8°C (100.4°F), pulse is 103/min, and blood pressure is 135/89 mm Hg in the left arm and 132/90 mm Hg in the right arm. Cardiopulmonary examination shows crackling with every heartbeat. Abdominal examination shows tenderness to palpation in the epigastric region; bowel sounds are normal. Laboratory studies show: Hemoglobin 16.0 g/dL Leukocyte count 11,000/mm3 Na+ 140 mEq/L K+ 4.2 mEq/L Cl- 101 mEq/L HCO3- 25 mEq/L Creatinine 1.3 mg/dL Alanine aminotransferase 21 U/L Aspartate aminotransferase 43 U/L Lipase 40 U/L (N = 14–280) Troponin I 0.025 ng/mL (N < 0.1) Chest x-ray shows a large hiatal hernia and mediastinal lucency. A 12-lead EKG shows sinus tachycardia and a left bundle branch block. Which of the following is the most appropriate next step in diagnosis?
A 43-year-old woman was admitted to the hospital after a fall. When the emergency services arrived, she was unresponsive, did not open her eyes, but responded to painful stimuli. The witnesses say that she had convulsions lasting about 30 seconds when she lost consciousness after a traumatic event. On her way to the hospital, she regained consciousness. On admission, she complained of intense headaches and nausea. She opened her eyes spontaneously, was responsive but confused, and was able to follow motor commands. Her vital signs are as follows: blood pressure, 150/90 mm Hg; heart rate, 62/min; respiratory rate, 13/min; and temperature, 37.3℃ (99.1℉). There are no signs of a skull fracture. The pupils are round, equal, and poorly reactive to light. She is unable to fully abduct both eyes. Ophthalmoscopy does not show papillary edema or retinal hemorrhages. She has nuchal rigidity and a positive Kernig sign. An urgent head CT does not show any abnormalities. Which of the following is a proper investigation to perform in this patient?
A 52-year-old woman comes to the emergency department because of a 3-hour history of right flank pain and nausea. Her only medication is a multivitamin. Her vital signs are within normal limits. Physical examination shows tenderness in the right costovertebral angle. Urinalysis shows a pH of 5.1, 50–60 RBC/hpf, and dumbbell-shaped crystals. Which of the following best describes the composition of the crystals seen on urinalysis?
A 21-year-old college student is brought to the emergency department in a state of confusion. He also had one seizure approx. 45 minutes ago. He was complaining of fever and headache for the past 3 days. There was no history of nausea, vomiting, head trauma, sore throat, skin rash, or abdominal pain. Physical examination reveals: blood pressure 102/78 mm Hg, heart rate 122/min, and temperature 38.4°C (101.2°F). The patient is awake but confused and disoriented. He is sensitive to light and loud noises. Heart rate is elevated with a normal rhythm. Lungs are clear to auscultation bilaterally. The fundus examination is benign. Brudzinski’s sign is positive. What is the next best step in the management of this patient?
A 45-year-old woman undergoes endoscopic retrograde cholangiopancreatography (ERCP) for evaluation of suspected biliary strictures. The ERCP identifies 2 ducts in the pancreas (a small ventral duct and a larger dorsal duct). A diagnosis of a congenital pancreatic anomaly is made. Which of the following statements best describes this anomaly?
A 24-year-old female presents to her primary care physician with right knee pain for the last week. She states that she first noticed it after a long flight on her way back to the United States from Russia, where she had run a marathon along a mountain trail. The patient describes the pain as dull, aching, and localized to the front of her kneecap, and it worsens with sitting but improves with standing. Aspirin has not provided significant relief. The patient has a history of a torn anterior cruciate ligament (ACL) on the right side from a soccer injury three years ago. In addition, she was treated for gonorrhea last month after having intercourse with a new partner. At this visit, the patient’s temperature is 98.5°F (36.9°C), blood pressure is 112/63 mmHg, pulse is 75/min, and respirations are 14/min. Which of the following is most likely to establish the diagnosis?
Practice by Chapter
Symptom-based differential diagnosis approach
Practice Questions
System-based differential construction
Practice Questions
Probability ranking in differentials
Practice Questions
Common vs rare disease considerations
Practice Questions
Age and demographic considerations
Practice Questions
Pattern recognition in diagnosis
Practice Questions
Anatomical approach to differential diagnosis
Practice Questions
Syndrome recognition
Practice Questions
Refinement of differential with testing
Practice Questions
Interpreting diagnostic ambiguity
Practice Questions
Ruling in vs ruling out strategies
Practice Questions
Cognitive biases in differential construction
Practice Questions
Integration of diagnostic information
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
