Making the most of available information — MCQs

A 45-year-old man is brought to the emergency department after a car accident with pain in the middle of his chest and some shortness of breath. He has sustained injuries to his right arm and leg. He did not lose consciousness. His temperature is 37°C (98.6°F), pulse is 110/min, respirations are 18/min, and blood pressure is 90/60 mm Hg. He is alert and oriented to person, place, and time. Examination shows several injuries to the upper extremities and chest. There are jugular venous pulsations 10 cm above the sternal angle. Heart sounds are faint on cardiac examination. The lungs are clear to auscultation. An ECG is shown. Which of the following is the most appropriate next step in management?
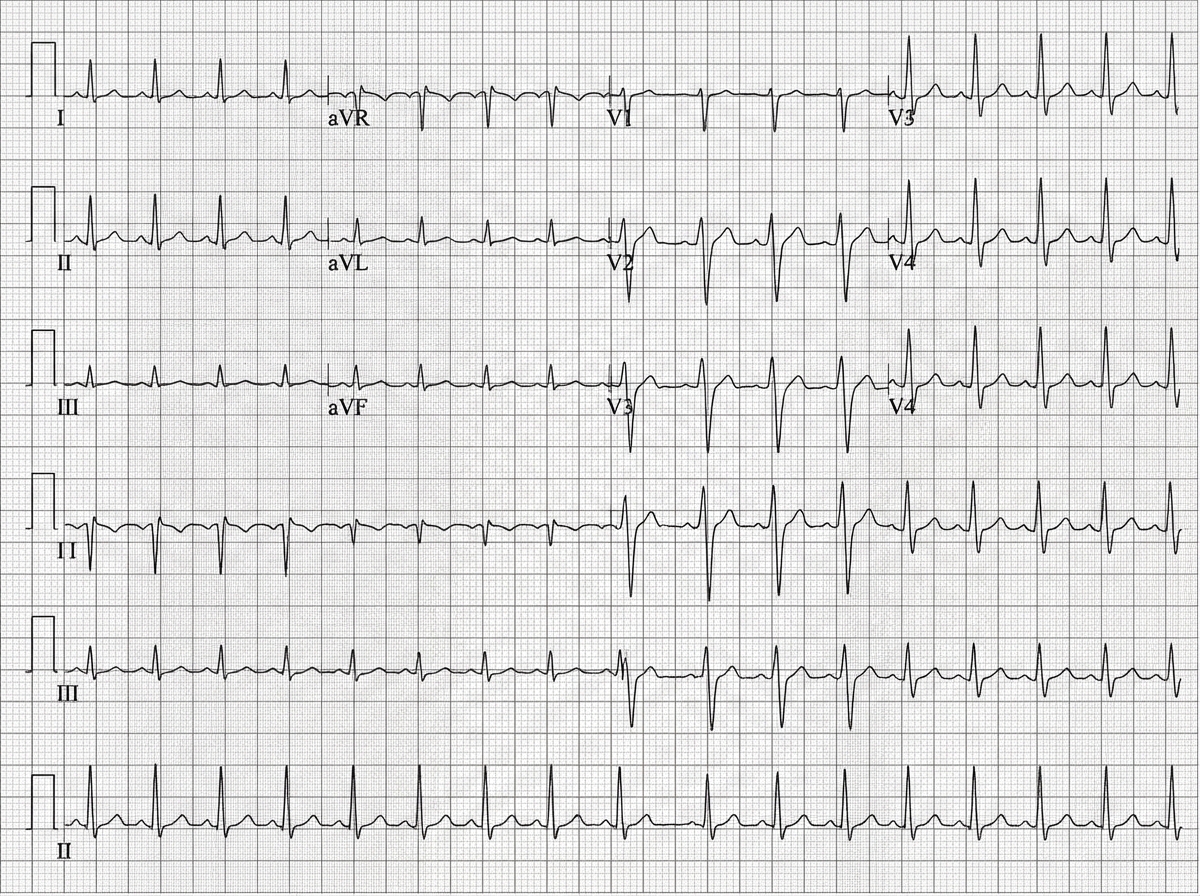
A 75-year-old man presents to the emergency department after an episode of syncope while walking outside with his wife. His wife states that he suddenly appeared pale and collapsed to the ground. She says he remained unconscious for 1 minute. He says he noticed a fluttering in his chest and excessive sweating before the episode. He has type 2 diabetes mellitus, essential hypertension, and chronic stable angina. He has not started any new medications in the past few months. Vital signs reveal: temperature 37.0°C (98.6°F), blood pressure 135/72 mm Hg, and pulse 72/min. Physical examination is unremarkable. ECG shows an old bifascicular block. Echocardiogram and 24-hour Holter monitoring are normal. Which of the following is the best next step in the evaluation of this patient's condition?
A 24-year-old man presents to the emergency department after a motor vehicle collision. He was in the front seat and unrestrained driver in a head on collision. His temperature is 99.2°F (37.3°C), blood pressure is 90/65 mmHg, pulse is 152/min, respirations are 16/min, and oxygen saturation is 100% on room air. Physical exam is notable for a young man who opens his eyes spontaneously and is looking around. He answers questions with inappropriate responses but discernible words. He withdraws from pain but does not have purposeful movement. Which of the following is this patient's Glasgow coma scale?
A 52-year-old man comes to the physician because of a 3-week history of a cough and hoarseness. He reports that the cough is worse when he lies down after lunch. His temperature is 37.5°C (99.5°F); the remainder of his vital signs are within normal limits. Because the physician has recently been seeing several patients with the common cold, the diagnosis of a viral upper respiratory tract infection readily comes to mind. The physician fails to consider the diagnosis of gastroesophageal reflux disease, which the patient is later found to have. Which of the following most accurately describes the cognitive bias that the physician had?
A 39-year-old woman presents with progressive weakness, exercise intolerance, and occasional dizziness for the past 3 months. Past medical history is unremarkable. She reports an 18-pack-year smoking history and drinks alcohol rarely. Her vital signs include: temperature 36.6°C (97.8°F), blood pressure 139/82 mm Hg, pulse 98/min. Physical examination is unremarkable. Her laboratory results are significant for the following: Hemoglobin 9.2 g/dL Erythrocyte count 2.1 million/mm3 Mean corpuscular volume (MCV) 88 μm3 Mean corpuscular hemoglobin (MCH) 32 pg/cell Leukocyte count 7,500/mm3 Which of the following is the best next step in the management of this patient’s condition?
A 41-year-old woman comes to the primary care physician’s office with a 7-day history of headaches, sore throat, diarrhea, fatigue, and low-grade fevers. The patient denies any significant past medical history, recent travel, or recent sick contacts. On review of systems, the patient endorses performing sex acts in exchange for money and recreational drugs over the last several months. You suspect primary HIV infection, but the patient refuses further evaluation. At a follow-up appointment 1 week later, she reports that she had been previously tested for HIV, and it was negative. Physical examination does not reveal any external abnormalities of her genitalia. Her heart and lung sounds are normal on auscultation. Her vital signs show a blood pressure of 123/82 mm Hg, heart rate of 82/min, and a respiratory rate of 16/min. Of the following options, which is the next best step in patient management?
A 21-year-old U.S. born first year medical student with no prior hospital or healthcare work presents to the physician for a routine physical exam. The patient is HIV negative, denies drug use, and denies sick contacts. The physician places a purified protein tuberculin test in the patient's right forearm intradermally. What is the proper time to read the test and induration diameter that would indicate a positive test result?
A 57-year-old man presents to the emergency department for weight loss and abdominal pain. The patient states that he has felt steadily more fatigued over the past month and has lost 22 pounds without effort. Today, he fainted prompting his presentation. The patient has no significant past medical history. He does have a 33 pack-year smoking history and drinks 4 to 5 alcoholic drinks per day. His temperature is 99.5°F (37.5°C), blood pressure is 100/58 mmHg, pulse is 100/min, respirations are 17/min, and oxygen saturation is 98% on room air. On physical exam, you see a patient who is very thin and appears to be pale. Stool fecal occult blood testing is positive. A CT scan of the abdomen is performed demonstrating a mass in the colon with multiple metastatic lesions scattered throughout the abdomen. The patient is informed of his diagnosis of metastatic colon cancer. When the patient conveys the information to his family he focuses his efforts on discussing the current literature in the field and the novel therapies that have been invented. He demonstrates his likely mortality outcome which he calculated using the results of a large multi-center study. Which of the following is this patient most likely demonstrating?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
