Warning signs review with patients — MCQs

A 79-year-old male presents to your office for his annual flu shot. On physical exam you note several linear bruises on his back. Upon further questioning he denies abuse from his daughter and son-in-law, who live in the same house. The patient states he does not want this information shared with anyone. What is the most appropriate next step, paired with its justification?
A 66-year-old man is brought to the emergency department after a motor vehicle accident. The patient was a restrained passenger in a car that was struck on the passenger side while crossing an intersection. In the emergency department, he is alert and complaining of abdominal pain. He has a history of hyperlipidemia, gastroesophageal reflux disease, chronic kidney disease, and perforated appendicitis for which he received an interval appendectomy four years ago. His home medications include rosuvastatin and lansoprazole. His temperature is 99.2°F (37.3°C), blood pressure is 120/87 mmHg, pulse is 96/min, and respirations are 20/min. He has full breath sounds bilaterally. He is tender to palpation over the left 9th rib and the epigastrium. He is moving all four extremities. His FAST exam reveals fluid in Morrison's pouch. This patient is most likely to have which of the following additional signs or symptoms?
A 68-year-old woman presents to the hospital for an elective right hemicolectomy. She is independently mobile and does her own shopping. She has had type 2 diabetes mellitus for 20 years, essential hypertension for 15 years, and angina on exertion for 6 years. She has a 30-pack-year history of smoking. The operation was uncomplicated. On post-op day 5, she becomes confused. She has a temperature of 38.5°C (101.3°F), respiratory rate of 28/min, and oxygen saturation of 92% on 2 L of oxygen. She is tachycardic at 118/min and her blood pressure is 110/65 mm Hg. On chest auscultation, she has coarse crackles in the right lung base. Her surgical wound appears to be healing well, and her abdomen is soft and nontender. Which of the following is the most likely diagnosis?
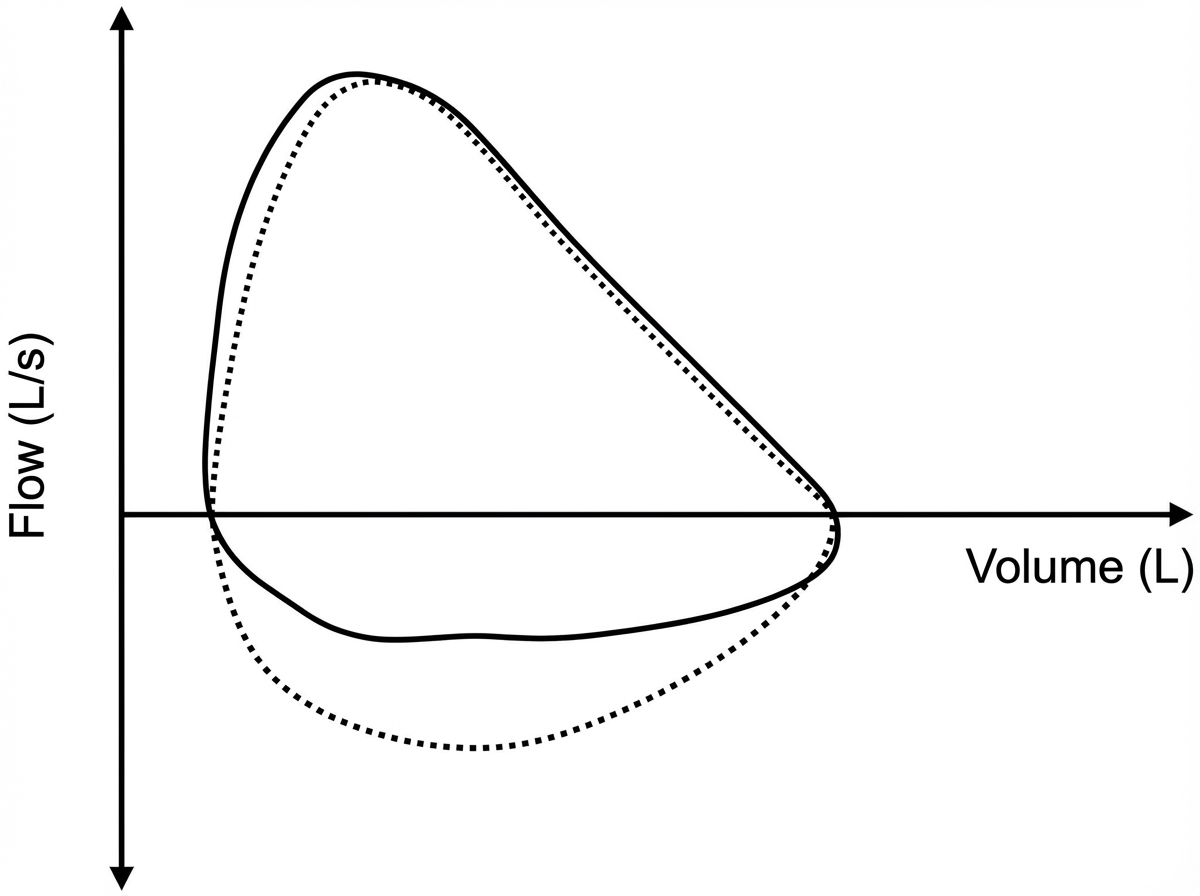
Five minutes after arriving in the postoperative care unit following total knee replacement under general anesthesia, a 55-year-old woman is acutely short of breath. The procedure was uncomplicated. Postoperatively, prophylactic treatment with cefazolin was begun and the patient received morphine and ketorolac for pain management. She has generalized anxiety disorder. Her only other medication is escitalopram. She has smoked one pack of cigarettes daily for 25 years. Her temperature is 37°C (98.6°F), pulse is 108/min, respirations are 26/min, and blood pressure is 95/52 mm Hg. A flow-volume loop obtained via pulmonary function testing is shown. Which of the following is the most likely underlying cause of this patient's symptoms?
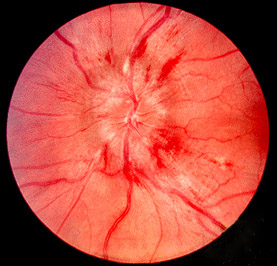
A 72-year-old woman comes to the emergency department 1 hour after the sudden onset of a diffuse, dull, throbbing headache. She also reports blurred vision, nausea, and one episode of vomiting. She has a history of poorly controlled hypertension. A photograph of her fundoscopic examination is shown. Which of the following is the most likely underlying cause of this patient's symptoms?
A 29-year-old man presents to the emergency department with chest pain and fatigue for the past week. The patient is homeless and his medical history is not known. His temperature is 103°F (39.4°C), blood pressure is 97/58 mmHg, pulse is 140/min, respirations are 25/min, and oxygen saturation is 95% on room air. Physical exam is notable for scars in the antecubital fossa and a murmur over the left sternal border. The patient is admitted to the intensive care unit and is treated appropriately. On day 3 of his hospital stay, the patient presents with right-sided weakness in his arm and leg and dysarthric speech. Which of the following is the most likely etiology of his current symptoms?
A 55-year-old man presents to the emergency department with hematemesis that started 1 hour ago but has subsided. His past medical history is significant for cirrhosis with known esophageal varices which have been previously banded. His temperature is 97.5°F (36.4°C), blood pressure is 114/64 mmHg, pulse is 130/min, respirations are 12/min, and oxygen saturation is 98% on room air. During the patient's physical exam, he begins vomiting again and his heart rate increases with a worsening blood pressure. He develops mental status changes and on exam he opens his eyes and flexes his arms only to sternal rub and is muttering incoherent words. Which of the following is the most appropriate next step in management?
A 28-year-old male presents to his primary care physician with complaints of intermittent abdominal pain and alternating bouts of constipation and diarrhea. His medical chart is not significant for any past medical problems or prior surgeries. He is not prescribed any current medications. Which of the following questions would be the most useful next question in eliciting further history from this patient?
A 38-year-old woman comes to the physician for the first time because of a 2-year history of lower back pain and fatigue. She also says that she occasionally feels out of breath. Her symptoms are not associated with physical activity. She has seen multiple physicians over the past year. Extensive workup including blood and urine tests, abdominal ultrasound, MRI of the back, and cardiac stress testing have shown no abnormalities. The patient asks for a medication to alleviate her symptoms. Which of the following is the most appropriate response by the physician?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
