Chronic disease management models — MCQs

A father brings his 3-year-old son to the pediatrician because he is concerned about his health. He states that throughout his son's life he has had recurrent infections despite proper treatment and hygiene. Upon reviewing the patient's chart, the pediatrician notices that the child has been infected multiple times with S. aureus, Aspergillus, and E. coli. Which of the following would confirm the most likely cause of this patient's symptoms?
A pathologist receives a skin biopsy specimen from a patient who is suspected to have developed graft-versus-host disease (GVHD) following allogeneic stem-cell transplantation. The treating physician informs the pathologist that he is specifically concerned about the diagnosis as the patient developed skin lesions on the 90th-day post-transplantation and therefore, by definition, it should be considered a case of acute GVHD. However, the lesions clinically appear like those of chronic GVHD. The pathologist examines the slide under the microscope and confirms the diagnosis of chronic GVHD. Which of the following findings on skin biopsy is most likely to have helped the pathologist to confirm the diagnosis?
A 38-year-old woman comes to the physician for the first time because of a 2-year history of lower back pain and fatigue. She also says that she occasionally feels out of breath. Her symptoms are not associated with physical activity. She has seen multiple physicians over the past year. Extensive workup including blood and urine tests, abdominal ultrasound, MRI of the back, and cardiac stress testing have shown no abnormalities. The patient asks for a medication to alleviate her symptoms. Which of the following is the most appropriate response by the physician?
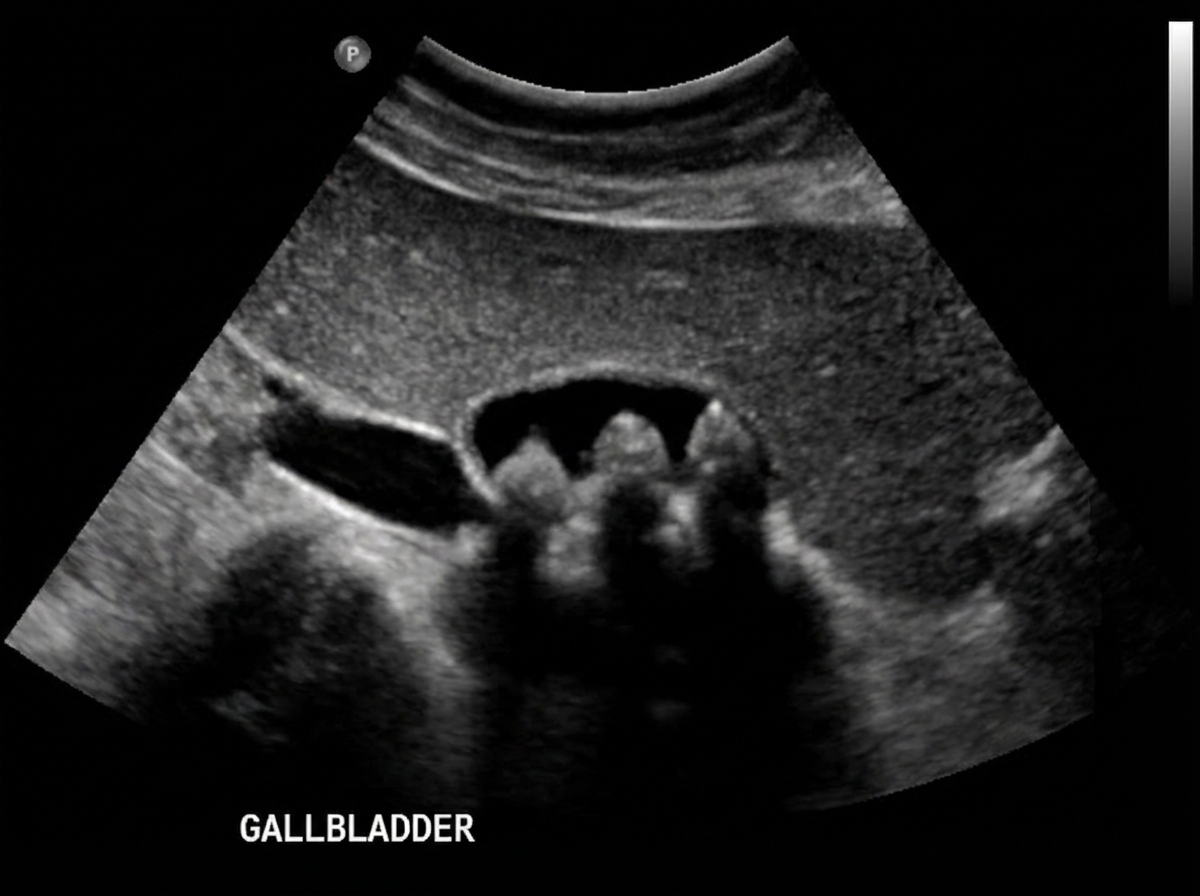
A 13-year-old African American boy with sickle cell disease is brought to the emergency department with complaints of abdominal pain over the last 24 hours. The pain is situated in the right upper quadrant and is sharp in nature with a score of 8/10 and radiates to tip of the right scapula. He also complains of anorexia and nausea over the past 2 days. He has been admitted into the hospital several times for pain episodes involving his legs, hands, thighs, lower back, and abdomen. His last hospital admission was 4 months ago for acute chest pain, and he was treated with antibiotics, analgesics, and intravenous fluid. He takes hydroxyurea with occasional red blood cell exchange. Both of his parents are in good health. Temperature is 38°C (100.4°F), blood pressure is 133/88 mm Hg, pulse is 102/min, respiratory rate is 20/min, and BMI is 18 kg/m2. On examination, he is in pain with a tender abdomen with painful inspiration. Soft palpation of the right upper quadrant causes the patient to cry out in pain. Laboratory test Complete blood count Hemoglobin 8.5 g/dL MCV 82 fl Leukocytes 13,500/mm3 Platelets 145,000/mm3 Basic metabolic panel Serum Na+ 135 mEq/L Serum K+ 3.9 mEq/L Serum Cl- 101 mEq/L Serum HCO3- 23 mEq/L Liver function test Serum bilirubin 2.8 mg/dL Direct bilirubin 0.8 mg/dL AST 30 U/L ALT 35 U/L Serum haptoglobin 23 mg/dL (41–165 mg/dL) Ultrasonography of abdomen shows the following image. What is the pathogenesis of this ultrasound finding?
A 55-year-old woman with rheumatoid arthritis comes to the physician because of a 3-month history of worsening fatigue and dyspnea. She has felt short-of-breath when walking up the stairs to her apartment. Menopause occurred 5 years ago. Her medications are methotrexate and folic acid supplementation. Physical examination shows conjunctival pallor, tenderness of bilateral wrists and knees, and ulnar deviation of the fingers. Her hematocrit is 27%, mean corpuscular volume is 84 μm3, and serum ferritin is 375 ng/mL. Which of the following has most likely contributed to the patient's current symptoms?
A 60-year-old woman presents to the emergency department due to progressive shortness of breath and a dry cough for the past week. She notes that her symptoms are exacerbated by physical activity and relieved by rest. The woman was diagnosed with chronic kidney disease 2 years ago and was recently started on regular dialysis treatment. Her pulse rate is 105/min, blood pressure is 110/70 mm Hg, respiratory rate is 30/min, and temperature is 37.8°C (100.0°F). On examination of the respiratory system, there is dullness on percussion, decreased vocal tactile fremitus, and decreased breath sounds over the right lung base. The rest of the physical exam is within normal limits. Which of the following is the most likely cause of this patient’s symptoms?
A 3-month-old male is brought to the emergency room by his mother who reports that the child has a fever. The child was born at 39 weeks of gestation and is at the 15th and 10th percentiles for height and weight, respectively. The child has a history of eczema. Physical examination reveals an erythematous fluctuant mass on the patient's inner thigh. His temperature is 101.1°F (38.4°C), blood pressure is 125/70 mmHg, pulse is 120/min, and respirations are 22/min. The mass is drained and the child is started on broad-spectrum antibiotics until the culture returns. The physician also orders a flow cytometry reduction of dihydrorhodamine, which is found to be abnormal. This patient is at increased risk of infections with which of the following organisms?
A 55-year-old woman comes to the physician because of a 6-month history of worsening shortness of breath on exertion and fatigue. She has type 1 diabetes mellitus, hypertension, hypercholesterolemia, and chronic kidney disease. Her mother was diagnosed with colon cancer at the age of 65 years. Her blood pressure is 145/92 mm Hg. Examination shows conjunctival pallor. Laboratory studies show: Hemoglobin 9.2 g/dL Mean corpuscular volume 88 μm3 Reticulocyte count 0.6 % Serum Ferritin 145 ng/mL Creatinine 3.1 mg/dL Calcium 8.8 mg/dL A fecal occult blood test is pending. Which of the following is the most likely underlying cause of this patient's symptoms?
A 53-year-old woman presents to her primary care physician with complaints of pain and swelling in her hands and fingers. She states that she has had these symptoms since she was in her 20s, but they have recently become more severe. She states that her wedding ring no longer fits, due to increased swelling of her fingers. She is a 30-pack-year smoker with a body mass index (BMI) of 31 kg/m2. The vital signs include: blood pressure 122/78 mm Hg, heart rate 72/min, and respiratory rate 15/min. On physical exam, a mild systolic murmur is heard over the apex, and her lungs are clear bilaterally. There is swelling of all the digits bilaterally, and a yellow-white plaque is noted beneath 3 of her nail beds. When asked about the plaques, she states that she was given itraconazole for them about 3 weeks ago; however, the plaques did not resolve. When asked further about joint pain, she notes that she has had shoulder and knee pain for the last several years, although she has not sought medical care for this. Which of the following is the best initial step in this patient’s therapeutic management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
