Metabolism — MCQs

On this page
A group of scientists is studying the mechanism of action of various pancreatic hormones in rats. The scientists studied hormone A, which is secreted by the β-cells of the pancreas, and found that hormone A binds to a complex dimeric receptor on the cell membrane and exerts its effects via phosphorylation and subsequent downstream signaling that includes dephosphorylation of different intracellular proteins. Now they are studying hormone B, which is secreted by the α-cells and antagonizes the actions of hormone A. Which 2nd messenger system would hormone B utilize to exert its cellular effects?
A 7-year-old boy is brought to the physician for evaluation of developmental delay and intellectual disability. He has been admitted to the hospital twice in the past 6 months because of a cerebral venous thrombosis and a pulmonary embolism, respectively. He is at 10th percentile for weight and 95th percentile for height. Physical examination shows bilateral downward and inward subluxation of the lenses. He has a high-arched palate and kyphosis. Laboratory studies show increased serum concentration of 5-methyltetrahydrofolate. Which of the following additional findings is most likely in this patient's serum?
A 59-year-old man comes to the physician because of bilateral blurry vision and difficulty driving at night that has been worsening progressively over the past 5 months. He has hypertension, type 2 diabetes mellitus, and hyperlipidemia. His hemoglobin A1c concentration is 8.9 mg/dL. A slit-lamp shows cloudy opacities of the lenses bilaterally. The patient's eye condition is most likely due to increased activity of which of the following enzymes?
A 45-year-old woman with type 1 diabetes mellitus is brought to the emergency department by her husband because of polyuria, nausea, vomiting, and altered mental status for 4 hours. On arrival, she is unconscious. Treatment with a drug is begun that increases glucose transport to skeletal muscle and adipose tissue. Which of the following cellular events is most likely to also occur in response to this drug?
An 8-month-old female infant from a first-degree consanguineous couple was brought to the physician because the mother noticed abnormalities in the growth of her child as well as the different lengths of her child's legs. The infant had gingival hyperplasia, restricted movement in both shoulders, a prominent, pointed forehead, and enophthalmos with a slight opacity in both corneas. A blood test revealed 10 fold higher than normal levels of the following enzymes: N-acetyl-ß-glucosaminidase, ß-glucuronidase, ß-hexosaminidase A, and alkaline phosphatase. Which of the following is most likely deficient in this patient?
A 22-year-old man comes to the physician for a routine physical examination. He feels well. He has no history of major medical illness and takes no medications. His vital signs are within normal limits. Examination shows no abnormalities. Laboratory studies, including a complete blood count and a standard electrolyte panel, are within normal limits. Urine dipstick is negative for glucose; a reducing substance test result of the urine is positive. Which of the following is the most appropriate dietary recommendation for this patient?
A 20-year-old male presents to the emergency department because of several days of back pain and fatigue. He is a college student who just returned from a study abroad program in Morocco. During his final week abroad he engaged in a number of recreational activities including swimming at the beach, eating local foods such as couscous and bean salad, and riding a camel into the desert. His temperature is 99°F (37°C), blood pressure is 121/79 mmHg, pulse is 70/min, and respirations are 11/min. He says that otherwise he has been healthy except for some episodes of dark urine. Upon physical exam, his skin is found to be more yellow than usual under his eyelids. Which of the following findings would most likely be seen in this patient?
A 3400-g (7 lb 8 oz) female newborn is delivered at 40 weeks' gestation. Physical examination shows pale skin, blonde hair, and blue irides. Her parents are from Haiti and express concern regarding the newborn's appearance. The most likely cause of this newborn's condition is a defect in which of the following processes?
A 3-day-old girl is brought to the physician by her mother because of difficulty feeding and lethargy for 1 day. She had jaundice after birth and was scheduled for a follow-up visit the next day. Her hemoglobin is 18.5 g/dL, total bilirubin is 38.1 mg/dL, and direct bilirubin is 0.1 mg/dL. Despite appropriate measures, the infant dies. At autopsy, examination of the brain shows deep yellow staining of the basal ganglia and subthalamic nuclei bilaterally. Which of the following is the most likely cause of this infant's findings?
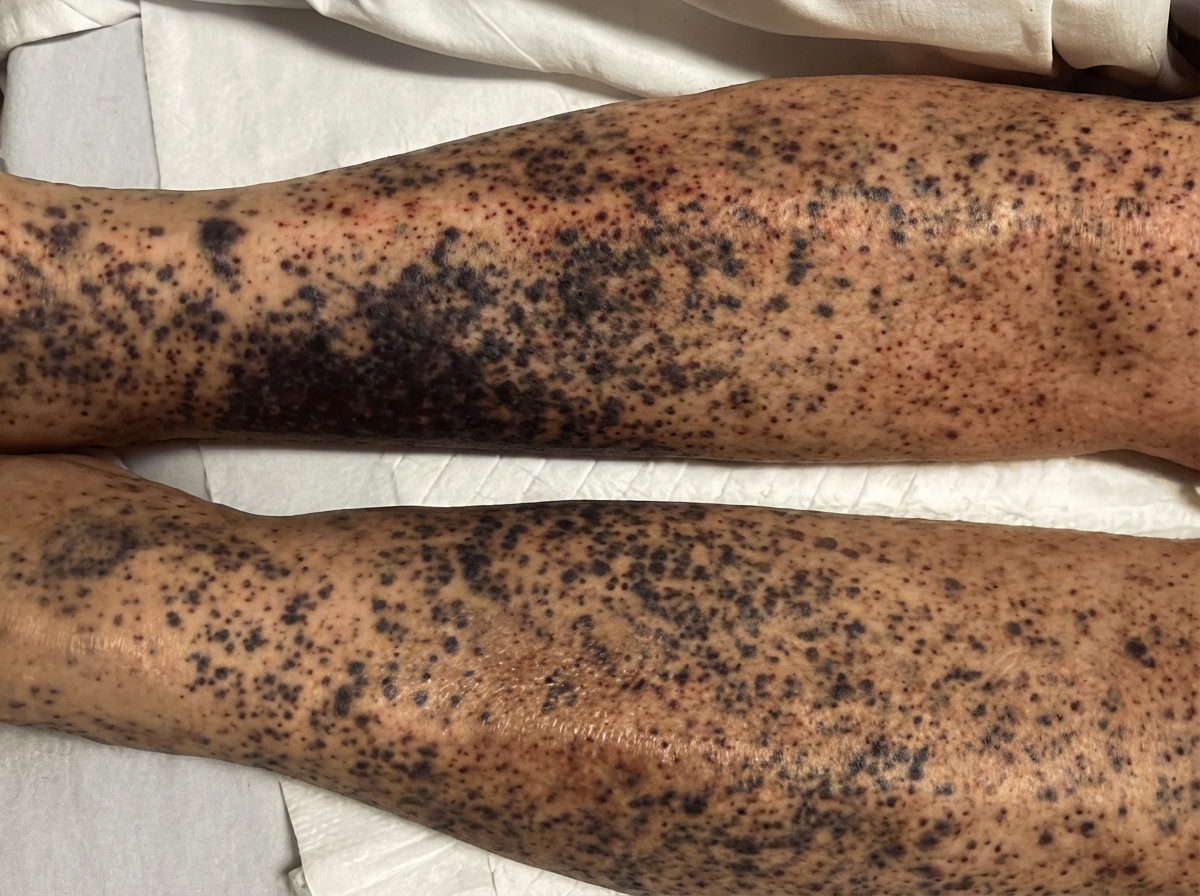
A 59-year-old man is brought to the emergency department with signs of spontaneous bruising of the lower legs. The patient has a history of alcohol use disorder and has been unemployed for the last 2 years. He reports a 1-year history of fatigue and joint pain. Physical examination of the patient’s legs reveals the findings illustrated in the image. Oral examination shows swollen gums, petechiae of the hard palate, and poor dentition. The most likely underlying cause of this patient's current findings involves which of the following metabolic deficiencies?
Practice by Chapter
TCA cycle reactions and regulation
Practice Questions
Electron transport chain and oxidative phosphorylation
Practice Questions
Pentose phosphate pathway
Practice Questions
Gluconeogenesis
Practice Questions
Glycogen metabolism
Practice Questions
Amino acid metabolism
Practice Questions
Integration of metabolic pathways
Practice Questions
Fed state vs. fasting state metabolism
Practice Questions
Exercise metabolism
Practice Questions
Alcohol metabolism
Practice Questions
Metabolic adaptations in starvation
Practice Questions
Metabolic disorders overview
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
