Metabolism — MCQs

On this page
A 10-year-old boy is brought into your clinic by his mother for sunburns that have not been healing. The mother states that he easily gets sunburned. The mother admits she gave birth to him at home and has never taken him to see a doctor. The patient walks with a wide stance gait and appears unstable on his feet. He has an extensive erythematous, scaling, hyperkeratotic rash on his face, neck, arms and legs. After extensive workup, the patient is found to have a genetic disorder that results in defective absorption of an important vitamin. Which of the following is likely to be low if measured?
An investigator is studying severely ill patients who experience hypoglycemia and ketonuria during times of fasting. The investigator determines that during these episodes, amino acids liberated from muscle proteins are metabolized to serve as substrates for gluconeogenesis. Nitrogen from this process is transported to the liver primarily in the form of which of the following molecules?
A 4-year-old boy is brought to the physician because of a rash and difficulty swallowing. His family emigrated from Nigeria 2 months ago. Examination shows an erythematous rash with fine yellow scales on his eyebrows and nasolabial folds. Oral examination shows an erythematous throat and swollen tongue. There is peeling and fissures of the skin at the corners of the mouth and cracking of the lips. His hemoglobin concentration is 9.6 g/dL; mean corpuscular volume is 89 μm3. Erythrocyte glutathione reductase assay shows an increased activity coefficient. This patient is most likely deficient in a vitamin that is a precursor to which of the following molecules?
An 18-month-old boy is brought in to the pediatrician by his mother for concerns that her child is becoming more and more yellow over the past two days. She additionally states that the boy has been getting over a stomach flu and has not been able to keep down any food. The boy does not have a history of neonatal jaundice. On exam, the patient appears slightly sluggish and jaundiced with icteric sclera. His temperature is 99.0°F (37.2°C), blood pressure is 88/56 mmHg, pulse is 110/min, and respirations are 22/min. His labs demonstrate an unconjugated hyperbilirubinemia of 16 mg/dL. It is determined that the best course of treatment for this patient is phenobarbital to increase liver enzyme synthesis. Which of the following best describes the molecular defect in this patient?
In a lab experiment, a researcher treats early cells of the erythrocyte lineage with a novel compound called Pb82. Pb82 blocks the first step of heme synthesis. However, the experiment is controlled such that the cells otherwise continue to develop into erythrocytes. At the end of the experiment, the cells have developed into normal erythrocytes except that they are devoid of heme. A second compound, anti-Pb82 is administered which removes the effect of Pb82. Which of the following is likely to be true of the mature red blood cells in this study?
An investigator is studying nutritional deficiencies in humans. A group of healthy volunteers are started on a diet deficient in pantothenic acid. After 4 weeks, several of the volunteers develop irritability, abdominal cramps, and burning paresthesias of their feet. These symptoms are fully reversed after reintroduction of pantothenic acid to their diet. The function of which of the following enzymes was most likely impaired in the volunteers during the study?
A 54-year-old man comes to the physician because of generalized fatigue and numbness of his legs and toes for 5 months. He has hypertension and hypercholesterolemia. He underwent a partial gastrectomy for peptic ulcer disease 15 years ago. Current medications include amlodipine and atorvastatin. He is a painter. His temperature is 37°C (98.6°F), pulse is 101/min, respirations are 17/min, and blood pressure is 122/82 mm Hg. Examination shows conjunctival pallor and glossitis. Sensation to vibration and position is absent over the lower extremities. He has a broad-based gait. The patient sways when he stands with his feet together and closes his eyes. His hemoglobin concentration is 10.1 g/dL, leukocyte count is 4300/mm3, and platelet count is 110,000/mm3. Which of the following laboratory findings is most likely to be seen in this patient?
The balance between glycolysis and gluconeogenesis is regulated at several steps, and accumulation of one or more products/chemicals can either promote or inhibit one or more enzymes in either pathway. Which of the following molecules if increased in concentration can promote gluconeogenesis?
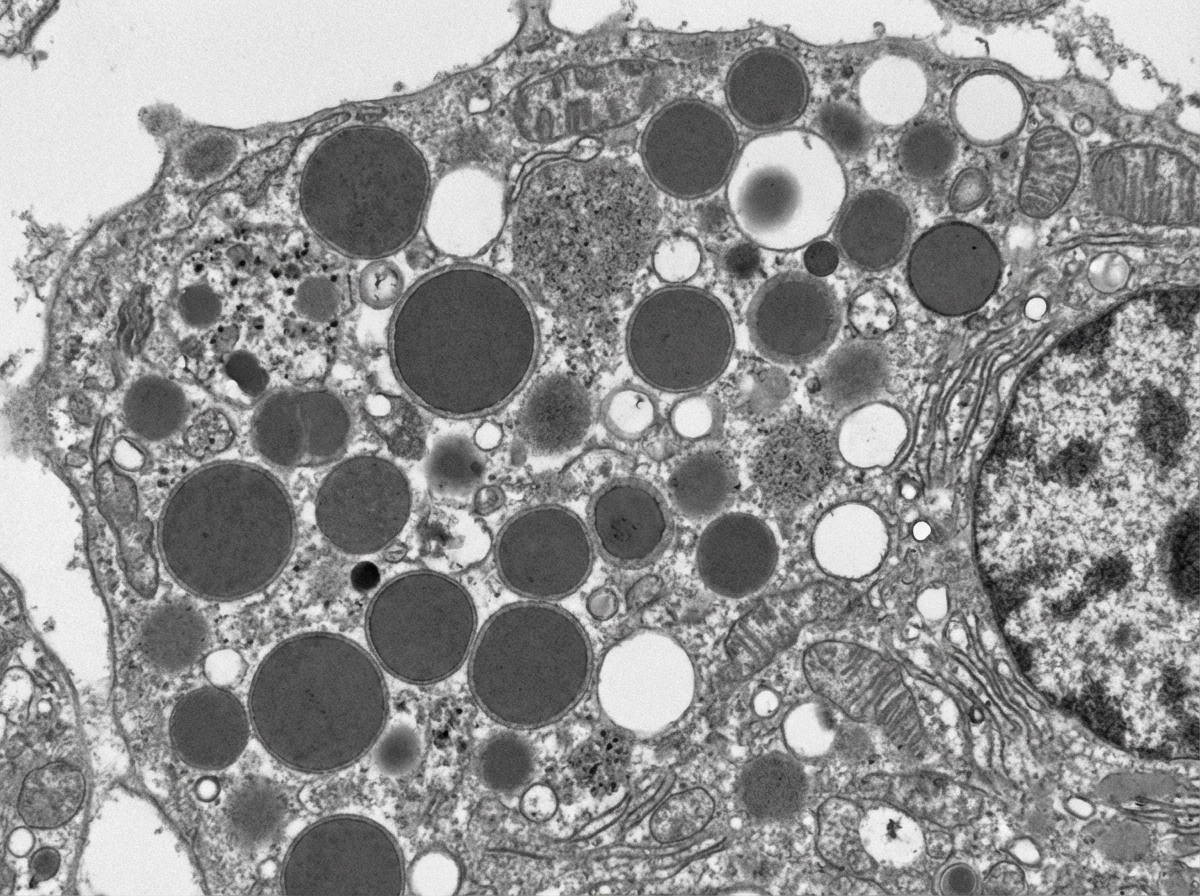
A 3-month-old boy presents for routine health maintenance. The patient has coarse facial features and stiff joint movements with restricted passive and active range of motion. He also has problems following objects with his eyes and seems not to focus on anything. On physical examination, the corneas are clouded, and the patient fails to meet any 3-month developmental milestones. Genetic testing and histopathology are performed and reveal failure of a cellular structure to phosphorylate mannose residues on glycoproteins. An electron microscopy image of one of this patient’s cells is shown. Which of the following is the most likely diagnosis in this patient?
A 6-day-old infant who was born via uncomplicated vaginal delivery at 39 weeks of gestation is brought to the family physician for poor feeding. The mother received adequate prenatal care throughout the pregnancy, and has no medical conditions. On physical exam, the infant's temperature is 36.5°C (97.7°F), blood pressure is 70/45 mmHg, pulse is 170/min, and respirations are 40/min. The infant has dry mucous membranes, capillary refill of 4 seconds, and a depressed anterior fontanelle. No abdominal masses are noted. Genital exam shows enlargement of the clitoris with fusion of the labioscrotal folds. Serum chemistry is remarkable for hyponatremia and hyperkalemia. The infant's karyotype is 46,XX. Which of the following findings are most likely to be discovered upon further workup?
Practice by Chapter
TCA cycle reactions and regulation
Practice Questions
Electron transport chain and oxidative phosphorylation
Practice Questions
Pentose phosphate pathway
Practice Questions
Gluconeogenesis
Practice Questions
Glycogen metabolism
Practice Questions
Amino acid metabolism
Practice Questions
Integration of metabolic pathways
Practice Questions
Fed state vs. fasting state metabolism
Practice Questions
Exercise metabolism
Practice Questions
Alcohol metabolism
Practice Questions
Metabolic adaptations in starvation
Practice Questions
Metabolic disorders overview
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
