Lipid metabolism — MCQs

On this page
A 12-year-old boy is brought to the physician because of difficulty in walking for 5 months. His mother reports that he has trouble keeping his balance and walking without support. Over the past year, he has started to have difficulty seeing in the dark and his hearing has been impaired. Examination shows marked scaling of the skin on the face and feet and a shortened 4th toe. Muscle strength is 3/5 in the lower extremities and 4/5 in the upper extremities. Sensation to pinprick is symmetrically decreased over the legs. Fundoscopy shows peripheral pigment deposits and retinal atrophy. His serum phytanic acid concentration is markedly elevated. The patient's condition is most likely caused by a defect in which of the following cellular structures?
A 3-week-old newborn is brought to the pediatrician by his mother. His mother is concerned about her son’s irritability and vomiting, particularly after breastfeeding him. The infant was born at 39 weeks via spontaneous vaginal delivery. His initial physical was benign. Today the newborn appears mildly jaundiced with palpable hepatomegaly, and his eyes appear cloudy, consistent with the development of cataracts. The newborn is also in the lower weight-age percentile. The physician considers a hereditary enzyme deficiency and orders blood work and a urinalysis to confirm his diagnosis. He recommends that milk and foods high in galactose and/or lactose be eliminated from the diet. Which of the following is the most likely deficient enzyme in this metabolic disorder?
A startup is working on a novel project in which they claim they can replicate the organelle that is defective in MELAS syndrome. Which of the following metabolic processes must they be able to replicate if their project is to mimic the metabolic processes of this organelle?
Researchers are experimenting with hormone levels in mice in fasting and fed states. To test hormone levels in the fed state, the mice are given an oral glucose load and various hormones are measured in a blood sample. Researchers are most interested in the hormone whose blood levels track evenly with C-peptide levels. The hormone the researchers are most interested in is responsible for which of the following actions in the body?
A 21-year-old Syrian refugee, who arrived in the US 2 weeks ago after living in refugee camps in Jordan and Turkey for 2 years, presents with decreased night vision, severe dry eyes unresponsive to eye drops, and a corneal ulcer. She reports limiting her food intake to ensure her 3-year-old son's nutrition. Her BMI is 18.1 kg/m2. Examination reveals lethargy, dry mucous membranes, decreased skin turgor, and dry, thickened conjunctiva. This patient's symptoms are most consistent with a deficiency in a vitamin that contributes to which of the following processes?
An 18-month-old boy of Ashkenazi-Jewish descent presents with loss of developmental milestones. On ocular exam, a cherry-red macular spot is observed. No hepatomegaly is observed on physical exam. Microscopic exam shows lysosomes with onion-skin appearance. What is the most likely underlying biochemical abnormality?
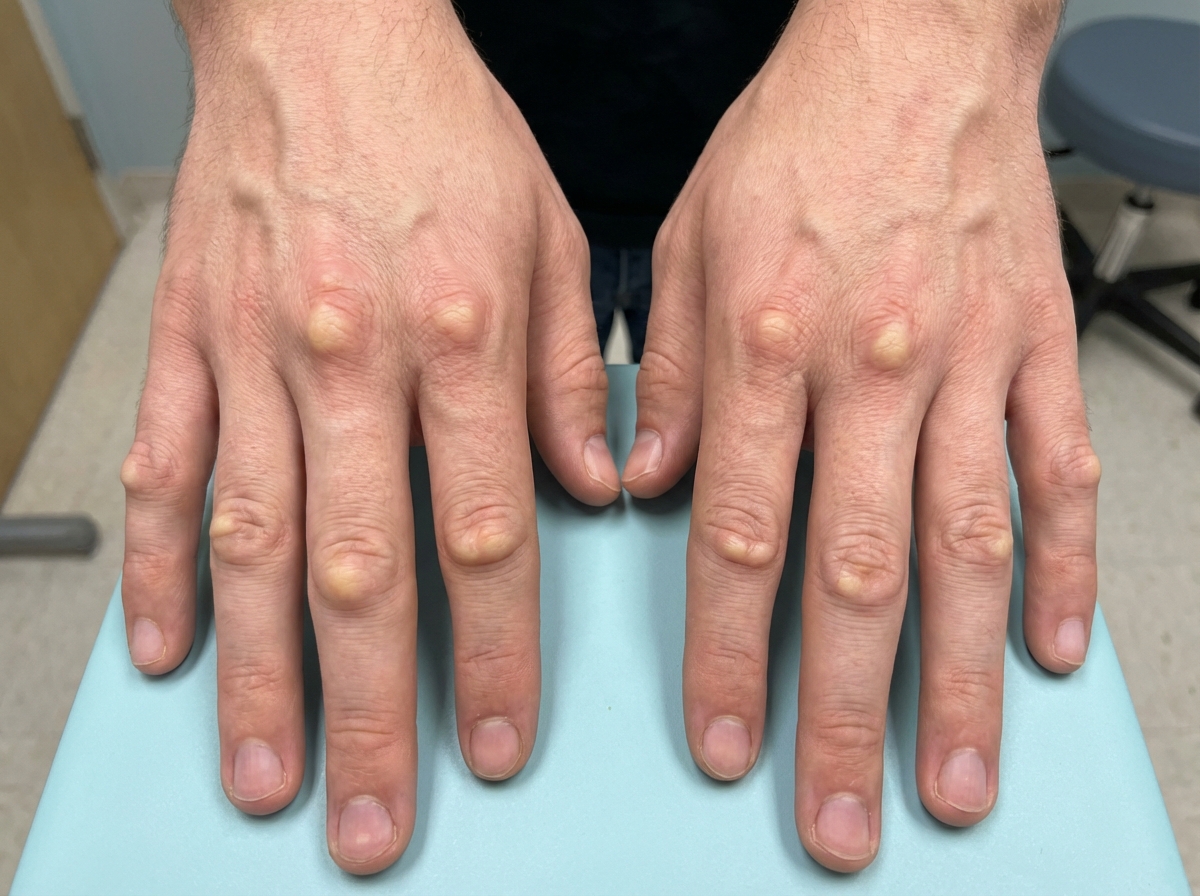
A previously healthy 22-year-old man comes to the physician because of multiple nodules on his hands that first appeared a few months ago. He works as a computer game programmer. His father died of a myocardial infarction at 37 years of age, and his mother has rheumatoid arthritis. A photograph of the lesions is shown. The nodules are firm, mobile, and nontender. Which of the following is the most likely mechanism underlying this patient's skin findings?
A 30-year-old woman is brought to the emergency department by ambulance after being found unconscious in her bedroom by her roommate. The roommate says the patient has type 1 diabetes and takes her insulin regularly. Her pulse is 110/min, the respiratory rate is 24/min, the temperature is 36.6°C (97.9°F), and the blood pressure is 95/65 mm Hg. She is breathing heavily and gives irrelevant responses to questions. Her skin and mucous membranes appear dry. Her breath has a fruity smell to it. Tendon reflexes are slightly delayed. The laboratory findings include: Finger-stick glucose 530 mg/dL Arterial blood gas analysis pH 7.1 pO2 94 mm Hg pCO2 32 mm Hg HCO3 17 mEq/L Serum Sodium 136 mEq/L Potassium 3.2 mEq/L Chloride 136 mEq/L Blood urea nitrogen 20 mg/dL Serum creatinine 1.2 mg/dL Urine examination Glucose positive Ketones positive Leucocytes negative Nitrite negative RBC negative Casts negative Which of the following abnormalities accounts for her sweet smelling breath?
A 43-year-old woman, gravida 2, para 2, comes to the physician because of a 6-month history of heavy, irregular menstrual bleeding. Pelvic examination shows blood and clots in the posterior fornix and normal-appearing internal and external genitalia. An endometrial biopsy specimen shows straight uniform tubular glands lined with tall pseudostratified columnar epithelial cells with high mitotic activity embedded in an edematous stroma. Increased activity of which of the following is directly responsible for the histologic appearance of the biopsy specimen?
A 24-year-old woman with a past medical history of anorexia nervosa presents to the clinic due to heavy menses, bleeding gums, and easy bruisability. She says she is trying to lose weight by restricting her food intake. She has taken multiple courses of antibiotics for recurrent sinusitis over the past month. No other past medical history or current medications. She is not sexually active. Her vital signs are as follows: temperature 37.0°C (98.6°F), blood pressure 90/60 mm Hg, heart rate 100/min, respiratory rate 16/min. Her BMI is 16 kg/m2. Her physical examination is significant for ecchymosis on the extremities, dry mucous membranes, and bleeding gums. A gynecological exam is non-contributory. Laboratory tests show a prolonged PT, normal PTT, and normal bleeding time. CBC shows microcytic anemia, normal platelets, and normal WBC. Her urine pregnancy test is negative. Which of the following is the most likely cause of her condition?
Practice by Chapter
Fatty acid oxidation (beta-oxidation)
Practice Questions
Fatty acid synthesis
Practice Questions
Ketone body metabolism
Practice Questions
Cholesterol synthesis and regulation
Practice Questions
Lipoprotein metabolism
Practice Questions
Phospholipid metabolism
Practice Questions
Eicosanoid synthesis and function
Practice Questions
Steroid hormone synthesis
Practice Questions
Adipose tissue metabolism
Practice Questions
Brown vs. white adipose tissue
Practice Questions
Disorders of lipid metabolism
Practice Questions
Integration with carbohydrate metabolism
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
