Collateral circulation — MCQs

A 61-year-old man is brought to the emergency room with slurred speech. According to the patient's wife, they were watching a movie together when he developed a minor headache. He soon developed difficulty speaking in complete sentences, at which point she decided to take him to the emergency room. His past medical history is notable for hypertension and hyperlipidemia. He takes aspirin, lisinopril, rosuvastatin. The patient is a retired lawyer. He has a 25-pack-year smoking history and drinks 4-5 beers per day. His father died of a myocardial infarction, and his mother died of breast cancer. His temperature is 98.6°F (37°C), blood pressure is 143/81 mmHg, pulse is 88/min, and respirations are 21/min. On exam, he can understand everything that is being said to him and is able to repeat statements without difficulty. However, when asked to speak freely, he hesitates with every word and takes 30 seconds to finish a short sentence. This patient most likely has an infarct in which of the following vascular distributions?
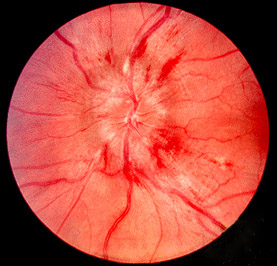
A 72-year-old woman comes to the emergency department 1 hour after the sudden onset of a diffuse, dull, throbbing headache. She also reports blurred vision, nausea, and one episode of vomiting. She has a history of poorly controlled hypertension. A photograph of her fundoscopic examination is shown. Which of the following is the most likely underlying cause of this patient's symptoms?
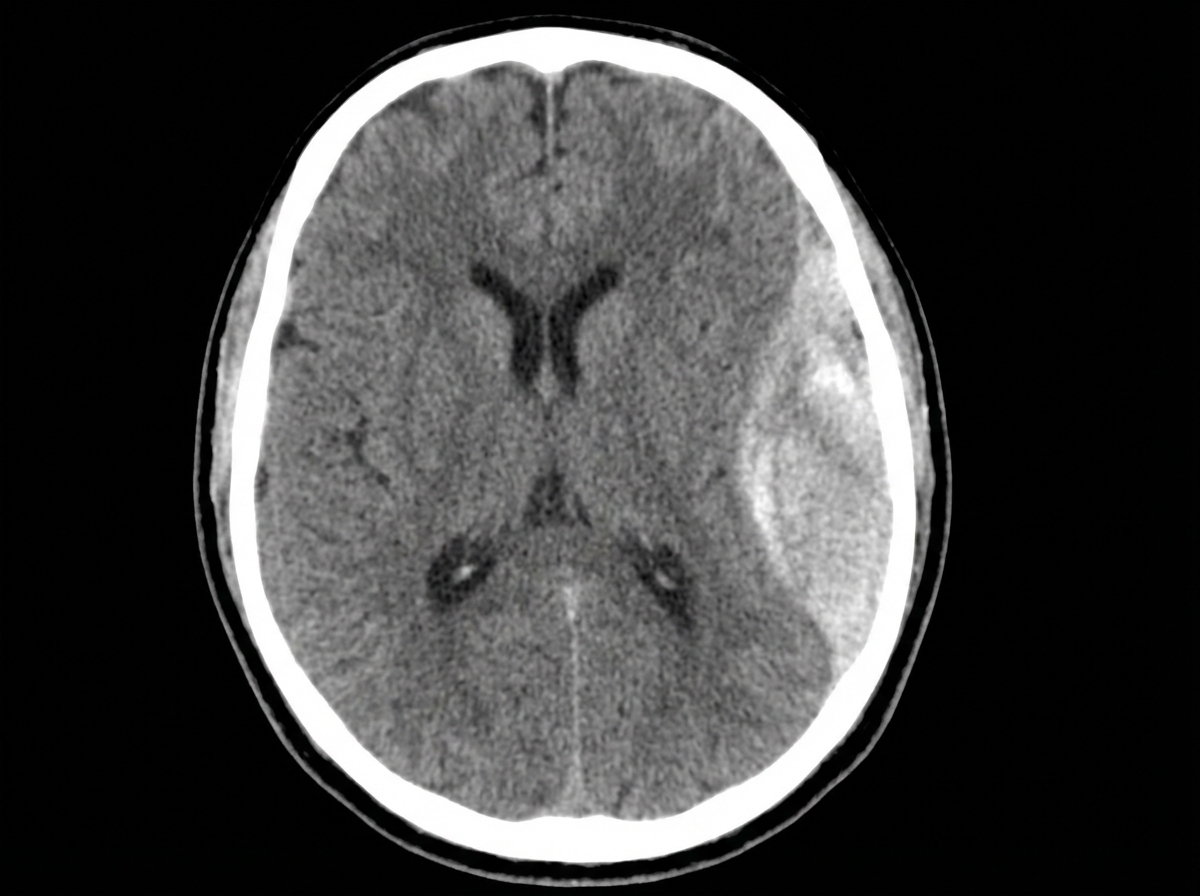
A 28-year-old man is brought to the emergency department by ambulance after developing an altered mental state following blunt trauma to the head. The patient was competing at a local mixed martial arts competition when he was struck in the head and lost consciousness. A few minutes later, upon regaining consciousness, he had a progressive decline in mental status. Past medical history is noncontributory. Upon arrival at the hospital, the temperature is 37.0°C (98.6°F), the blood pressure is 145/89 mm Hg, the pulse is 66/min, the respiratory rate is 14/min, and the oxygen saturation is 99% on room air. He is alert now. A noncontrast CT scan is performed, and the result is provided in the image. Which of the following structures is most likely affected in this patient?
A 54-year-old man was brought to the emergency room due to acute onset of slurred speech while at work, after which he lost consciousness. The patient's wife says this occurred approximately 30 minutes ago. Past medical history is significant for poorly controlled hypertension and type 2 diabetes mellitus. His blood pressure is 90/50 mm Hg, respiratory rate is 12/min, and heart rate is 48/min. The patient passes away shortly after arriving at the hospital. At autopsy, bilateral wedge-shaped strips of necrosis are seen in this patient's brain in the medial temporal lobe structures. Which of the following is the most likely location of these necrotic cells?
A 75-year-old man is brought to the emergency room after being found unresponsive in his home. His medical history is unknown. On physical examination he does not demonstrate any spontaneous movement of his extremities and is unable to respond to voice or painful stimuli. You notice that he is able blink and move his eyes in the vertical plane. Based on these physical exam findings, you expect that magnetic resonance angiogram will most likely reveal an occlusion in which of the following vessels?
A 53-year-old man with a past medical history significant for hyperlipidemia, hypertension, and hyperhomocysteinemia presents to the emergency department complaining of 10/10 crushing, left-sided chest pain radiating down his left arm and up his neck into the left side of his jaw. His ECG shows ST-segment elevation in leads V2-V4. He is taken to the cardiac catheterization laboratory for successful balloon angioplasty and stenting of a complete blockage in his left anterior descending coronary artery. Echocardiogram the following day shows decreased left ventricular function and regional wall motion abnormalities. A follow-up echocardiogram 14 days later shows a normal ejection fraction and no regional wall motion abnormalities. This post-infarct course illustrates which of the following concepts?
A 68-year-old man is brought to the emergency department by ambulance after he was found to be altered at home. Specifically, his wife says that he fell and was unable to get back up while walking to bed. When she approached him, she found that he was unable to move his left leg. His past medical history is significant for hypertension, atrial fibrillation, and diabetes. In addition, he has a 20-pack-year smoking history. On presentation, he is found to still have difficulty moving his left leg though motor function in his left arm is completely intact. The cause of this patient's symptoms most likely occurred in an artery supplying which of the following brain regions?
A 38-year-old woman with moyamoya disease undergoes cerebral angiography showing bilateral progressive stenosis of distal internal carotid arteries with extensive collateral formation. She has had multiple TIAs despite medical management. CT perfusion shows reduced flow in bilateral MCA territories. The neurosurgery team debates between direct bypass (STA-MCA) versus indirect revascularization (EDAS). Evaluate the optimal approach considering Circle of Willis pathophysiology.
A 70-year-old man undergoes elective clipping of an unruptured basilar tip aneurysm. Preoperative angiography shows bilateral fetal-type posterior cerebral arteries (PCAs arising from internal carotid arteries) with hypoplastic P1 segments. The aneurysm involves both posterior communicating artery origins. Synthesize an approach to surgical planning that optimally preserves cerebral perfusion.
A 42-year-old woman presents with progressive cognitive decline, early-onset dementia, and recurrent subcortical strokes. Genetic testing reveals CADASIL (Cerebral Autosomal Dominant Arteriopathy with Subcortical Infarcts and Leukoencephalopathy). MR angiography shows no large vessel abnormalities but extensive white matter changes. Her sister, also affected, is considering pregnancy. Evaluate the counseling regarding Circle of Willis anatomy and implications for disease manifestations.
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
