Upper/Lower Limb — MCQs

On this page
Seven hours after undergoing left hip arthroplasty for chronic hip pain, a 67-year-old woman reports a prickling sensation in her left anteromedial thigh and lower leg. Neurologic examination shows left leg strength 3/5 on hip flexion and 2/5 on knee extension. Patellar reflex is decreased on the left. Sensation to pinprick and light touch are decreased on the anteromedial left thigh as well as medial lower leg. Which of the following is the most likely underlying cause of this patient's symptoms?
A 25-year-old man presents to the emergency department after a car accident. He was the front seat restrained driver in a head-on collision. He has no significant past medical history. The patient’s vitals are stabilized and he is ultimately discharged with his injuries appropriately treated. At the patient’s follow up primary care appointment, he complains of being unable to lift his left foot. He otherwise states that he feels well and is not in pain. His vitals are within normal limits. Physical exam is notable for 1/5 strength upon dorsiflexion of the patient’s left foot, and 5/5 plantarflexion of the same foot. Which of the following initial injuries most likely occurred in this patient?
A 21-year-old man comes to the physician for a follow-up examination. Four days ago, he injured his right knee while playing soccer. Increased laxity of the right knee joint is noted when the knee is flexed to 30° and an abducting force is applied to the lower leg. The examination finding in this patient is most likely caused by damage to which of the following structures?
A 34-year-old woman comes to the physician because of a 3-month history of pain in her right thumb and wrist that radiates to her elbow. It is worse when she holds her infant son and improves with the use of an ice pack. Six months ago, she slipped on a wet floor and fell on her right outstretched hand. Her mother takes methotrexate for chronic joint pain. The patient takes ibuprofen as needed for her current symptoms. Examination of the right hand shows tenderness over the radial styloid with swelling but no redness. There is no crepitus. Grasping her right thumb and exerting longitudinal traction toward the ulnar side elicits pain. Range of motion of the finger joints is normal. There is no swelling, redness, or tenderness of any other joints. Which of the following is the most likely diagnosis?
A 37-year-old man presents to his primary care provider complaining of bilateral arm numbness. He was involved in a motor vehicle accident 3 months ago. His past medical history is notable for obesity and psoriatic arthritis. He takes adalimumab. His temperature is 99.3°F (37.4°C), blood pressure is 130/85 mmHg, pulse is 90/min, and respirations are 18/min. On exam, superficial skin ulcerations are found on his fingers bilaterally. His strength is 5/5 bilaterally in shoulder abduction, arm flexion, arm extension, wrist extension, finger abduction, and thumb flexion. He demonstrates loss of light touch and pinprick response in the distal tips of his 2nd and 5th fingertips and over the first dorsal web space. Vibratory sense is intact in the bilateral upper and lower extremities. Which of the following nervous system structures is most likely affected in this patient?
A 60-year-old woman is rushed to the emergency room after falling on her right elbow while walking down the stairs. She cannot raise her right arm. Her vital signs are stable, and the physical examination reveals loss of sensation over the upper lateral aspect of the right arm and shoulder. A radiologic evaluation shows a fracture of the surgical neck of the right humerus. Which of the following muscles is supplied by the nerve that is most likely damaged?
A 28-year-old man comes to the physician because of a 1-week history of weakness in the fingers of his right hand. One week ago, he experienced sudden pain in his right forearm during weight training. He has no history of serious illness. Physical examination shows impaired flexion of the proximal interphalangeal joints, while flexion of the distal interphalangeal joints is intact. Which of the following muscles is most likely injured?
A 17-year-old boy comes to the physician because of a 3-month history of pain in his right shoulder. He reports that he has stopped playing for his high school football team because of persistent difficulty lifting his right arm. Physical examination shows impaired active abduction of the right arm from 0 to 15 degrees. After passive abduction of the right arm to 15 degrees, the patient is able to raise his arm above his head. The dysfunctional muscle in this patient is most likely to be innervated by which of the following nerves?
A 28-year-old man comes to the physician because of a 3-month history of pain in his left shoulder. He is physically active and plays baseball twice a week. The pain is reproduced when the shoulder is externally rotated against resistance. Injury of which of the following tendons is most likely in this patient?
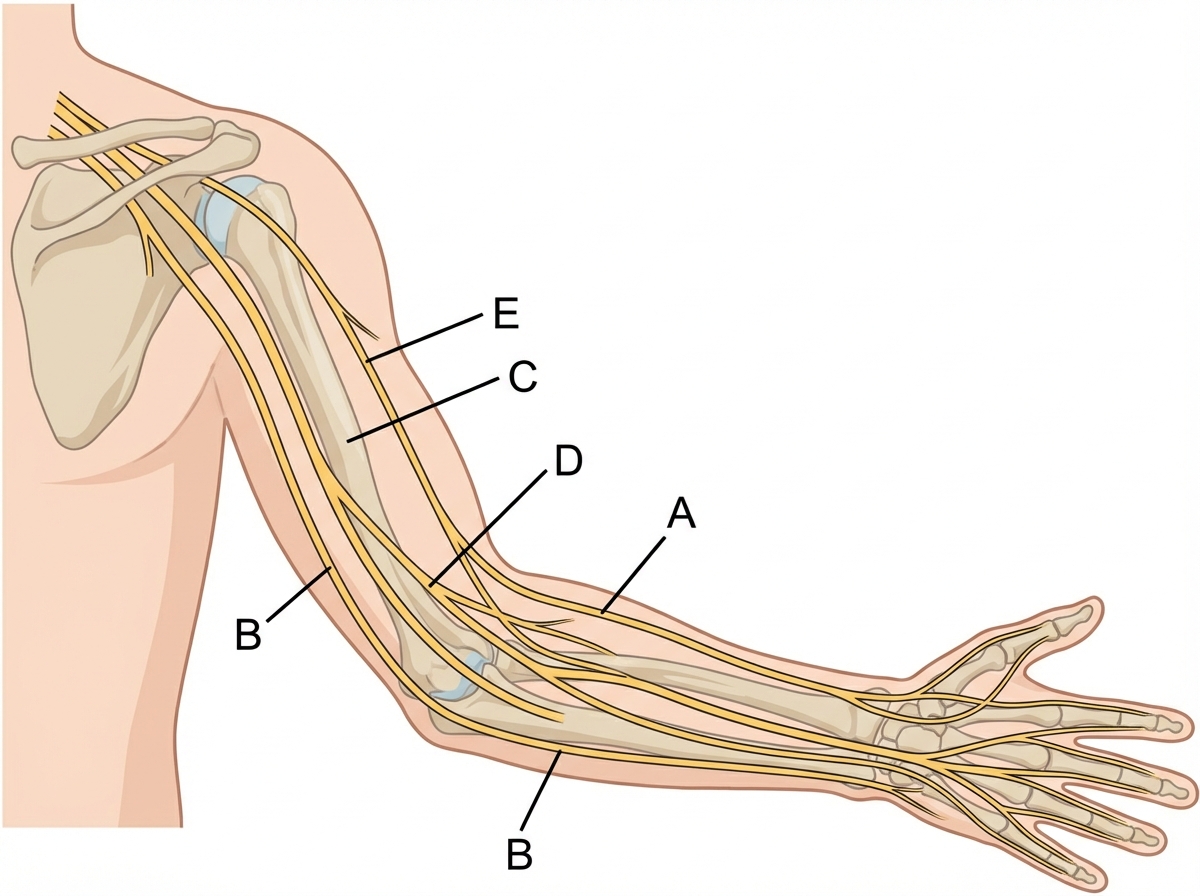
A 52-year-old female with a history of poorly-controlled diabetes presents to her primary care physician because of pain and tingling in her hands. These symptoms began several months ago and have been getting worse such that they interfere with her work as a secretary. She says that the pain is worse in the morning and she has been woken up at night by the pain. The tingling sensations have been located primarily in the thumb, index and middle fingers. On physical exam atrophy of the thenar eminence is observed and the pain is reproduced when the wrist is maximally flexed. The most likely cause of this patient's symptoms affects which of the nerves shown in the image provided?
Practice by Chapter
Bones and joints of upper limb
Practice Questions
Muscles and movements of upper limb
Practice Questions
Nerves and blood supply of upper limb
Practice Questions
Clinical correlations of upper limb
Practice Questions
Bones and joints of lower limb
Practice Questions
Muscles and movements of lower limb
Practice Questions
Nerves and blood supply of lower limb
Practice Questions
Clinical correlations of lower limb
Practice Questions
Comparison of upper and lower limb structures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
