Upper/Lower Limb — MCQs

On this page
A 31-year-old woman with multiple sclerosis comes to the physician because of a 4-day history of cramps in her left leg. Physical examination shows flexion of the left hip and increased tone in the thigh muscles. A local anesthetic block of which of the following nerves would most likely improve this patient's condition the most?
A 28-year-old woman presents to the emergency department with lateral knee pain that started this morning. The patient is a college student who is currently on the basketball team. She states her pain started after she twisted her knee. Her current medications include albuterol and ibuprofen. The patient's vitals are within normal limits and physical exam is notable for tenderness to palpation over the lateral right knee. When the patient lays on her left side and her right hip is extended and abducted it does not lower to the table in a smooth fashion and adduction causes discomfort. The rest of her exam is within normal limits. Which of the following is the most likely diagnosis?
A 23-year-old woman presents to the emergency department with an acute exacerbation of her 3-month history of low back and right leg pain. She says she has had similar symptoms in the past, but this time the pain was so excruciating, it took her breath away. She describes the pain as severe, shock-like, and localized to her lower back and radiating straight down the back of her right thigh and to her calf, stopping at the ankle. Her pain is worse in the morning, and, sometimes, the pain wakes her up at night with severe buttock and posterior thigh pain but walking actually makes the pain subside somewhat. The patient reports no smoking history or alcohol or drug use. She has been working casually as a waitress and does find bending over tables a strain. She is afebrile, and her vital signs are within normal limits. On physical examination, her left straight leg raise test is severely limited and reproduces her buttock pain at 20° of hip flexion. Pain is worsened by the addition of ankle dorsiflexion. The sensation is intact. Her L4 and L5 reflexes are normal, but her S1 reflex is absent on the right side. A CT of the lumbar spine shows an L5–S1 disc protrusion with right S1 nerve root compression. Which of the following muscle-nerve complexes is involved in producing an S1 reflex?
A 37-year-old obese woman presents to the neurology clinic complaining of severe pain in her left wrist and tingling sensation in her left thumb, index finger, and middle finger, and some part of her ring finger. The pain started as an occasional throb and she could ignore it or takes analgesics but now the pain is much worse and wakes her up at night. She is also concerned that these fingers are occasionally numb and sometimes tingle. She works as a typist and her pain mostly increases after typing all day. Her right wrist and fingers are fine. Nerve conduction studies reveal nerve compression. Which of the following additional clinical findings would most likely be present in this patient?
A 24-year-old professional soccer player presents to the clinic with discomfort and pain while walking. He says that he has an unstable knee joint that started after an injury during a match last week. He adds that he heard a popping sound at the time of the injury. Physical examination of the knee reveals swelling of the knee joint with a positive anterior drawer test. Which of the following structures is most likely damaged in this patient?
A 25-year-old man comes to the physician because of a 2-week history of numbness in his left lower extremity. One month ago, he sustained a fracture of the neck of the left fibula during soccer practice that was treated with immobilization in a plaster cast. Physical examination of the left lower extremity is most likely to show which of the following findings?
A 32-year-old man comes to the emergency department because of a wound in his foot. Four days ago, he stepped on a nail while barefoot at the beach. Examination of the plantar surface of his right foot shows a purulent puncture wound at the base of his second toe with erythema and tenderness of the surrounding skin. The afferent lymphatic vessels from the site of the lesion drain directly into which of the following groups of regional lymph nodes?
A 52-year-old man comes to the physician because of right shoulder pain that began after he repainted his house 1 week ago. Physical examination shows right subacromial tenderness. The pain is reproduced when the patient is asked to abduct the shoulder against resistance with the arm flexed forward by 30° and the thumb pointing downwards. The tendon of which of the following muscles is most likely to be injured in this patient?
A 33-year-old woman presents to the emergency department with pain in her right wrist. She says she was walking on the sidewalk a few hours ago when she suddenly slipped and landed forcefully on her outstretched right hand with her palm facing down. The patient is afebrile, and vital signs are within normal limits. Physical examination of her right wrist shows mild edema and tenderness on the lateral side of the right hand with a decreased range of motion. Sensation is intact. The patient is able to make a fist and OK sign with her right hand. A plain radiograph of her right wrist is shown in the image. Which of the following bones is most likely fractured in this patient?
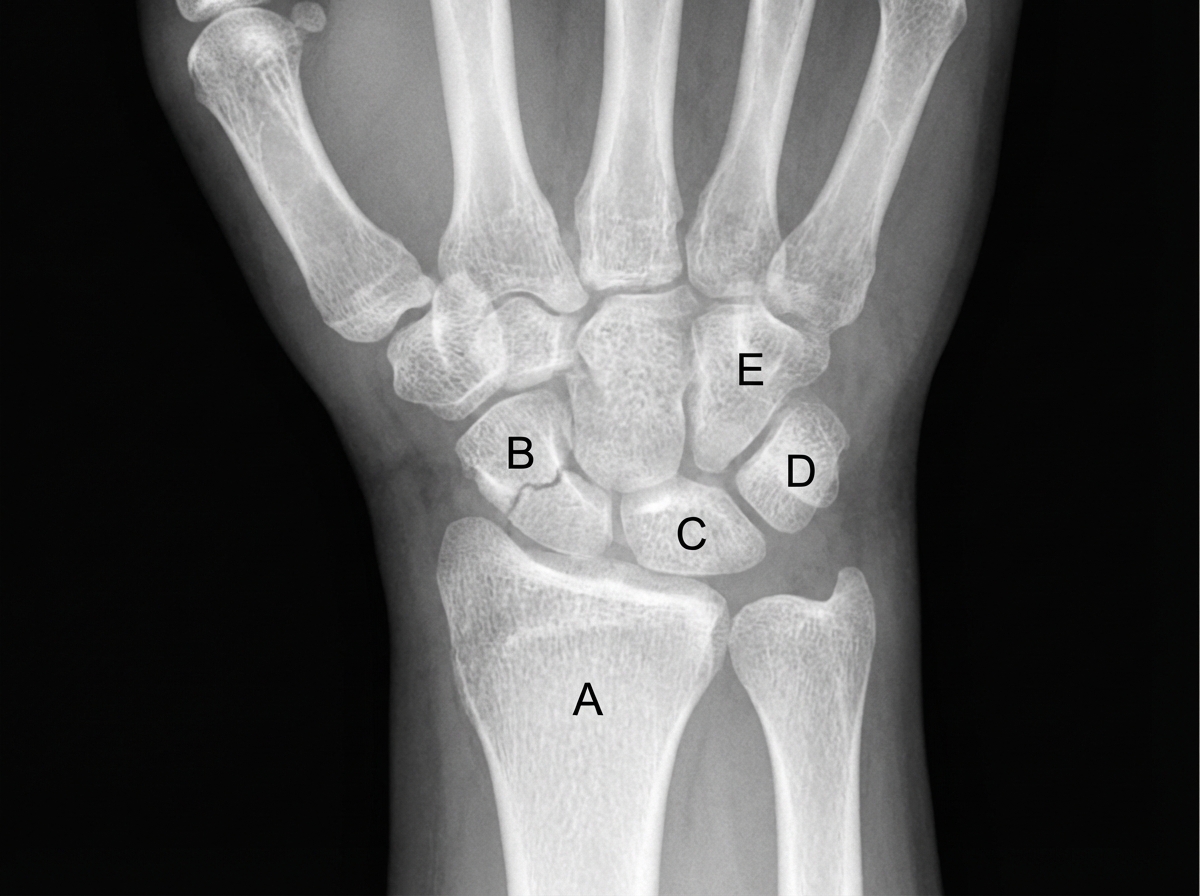
A 41-year-old woman comes to the doctor because of gradually progressive weakness in her right hand over the past few weeks. She goes to the gym to lift weights 5 times a week. With the dorsum of the right hand on a flat surface, the patient is unable to move her thumb to touch a pen held 2 cm above the interphalangeal joint of the thumb. An MRI of the right arm shows compression of a nerve that passes through the pronator teres muscle. Based on the examination findings, loss of innervation of which of the following muscles is most likely in this patient?
Practice by Chapter
Bones and joints of upper limb
Practice Questions
Muscles and movements of upper limb
Practice Questions
Nerves and blood supply of upper limb
Practice Questions
Clinical correlations of upper limb
Practice Questions
Bones and joints of lower limb
Practice Questions
Muscles and movements of lower limb
Practice Questions
Nerves and blood supply of lower limb
Practice Questions
Clinical correlations of lower limb
Practice Questions
Comparison of upper and lower limb structures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
