Upper/Lower Limb — MCQs

On this page
Identify the arrow marked nerve
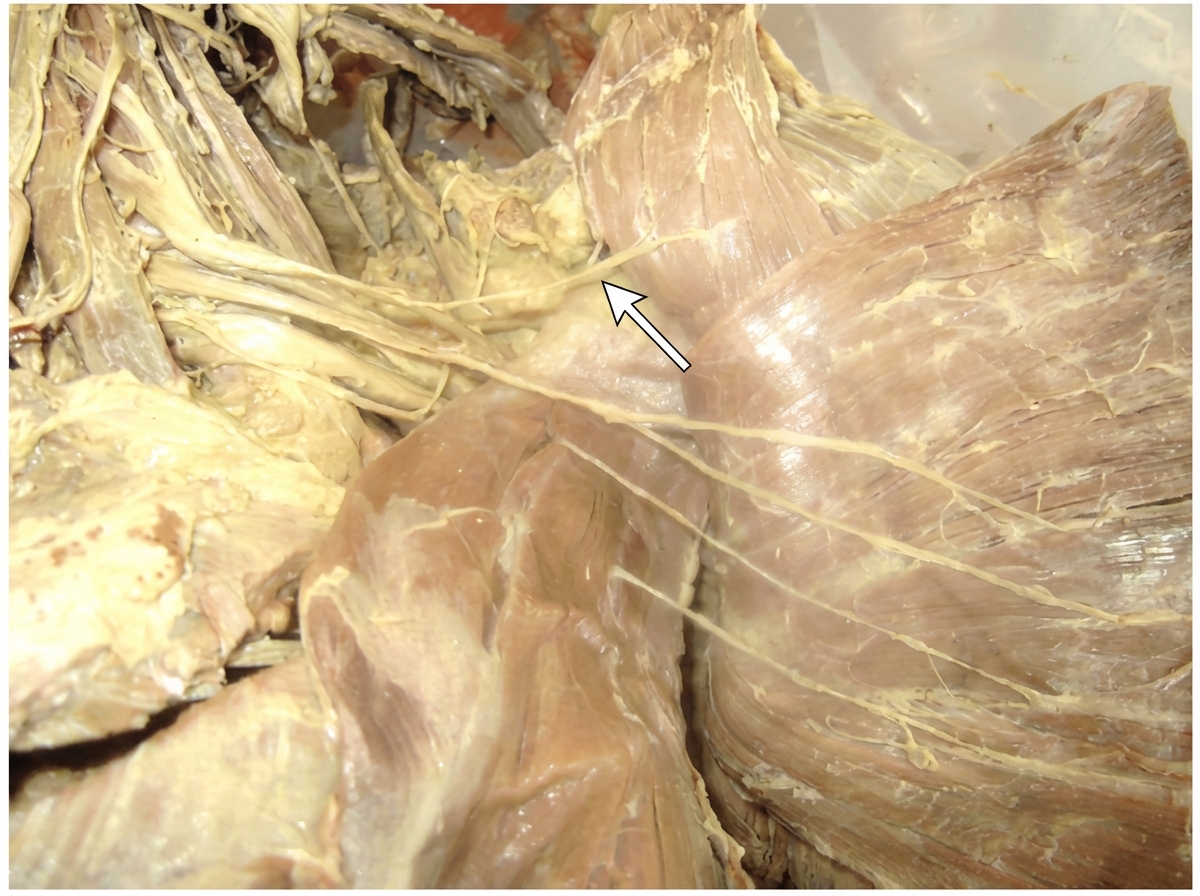
A patient with a nerve injury was asked to form an "O" with their index finger and thumb but was unable to do so. Which muscle is most likely affected?
A patient diagnosed with sciatica has tender hamstrings. Which of the following nerves supplies a hybrid muscle that is partially spared in this patient?
Which artery is palpated behind the medial malleolus and in front of the Achilles tendon?
A patient presents with pain in the back of the thigh and leg after lifting heavy weights. Which spinal segment is most likely involved?
Identify the arrow marked nerve 
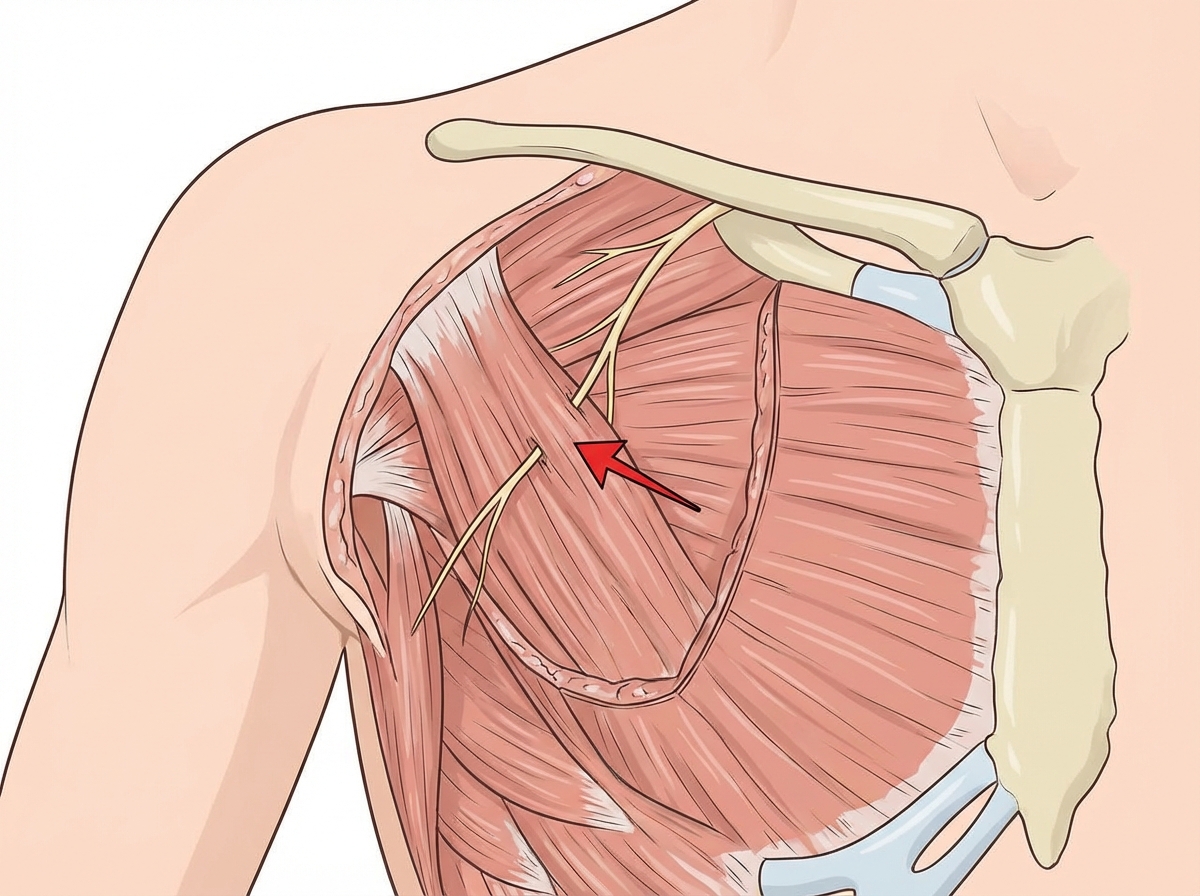
The "O sign" formed by the thumb and index finger is affected. Which muscle is most likely injured?
A patient underwent a coronary artery bypass graft (CABG) using the great saphenous vein. Post-surgery, the patient experiences neuralgia on the medial aspect of the leg and foot. Which nerve is most likely injured?
A young boy presents with multiple humerus fractures, resulting in loss of sensation over the lateral side of the forearm, along with difficulty in elbow flexion and forearm supination. What is the most likely nerve injury responsible for these symptoms?
Pen Test is for which nerve
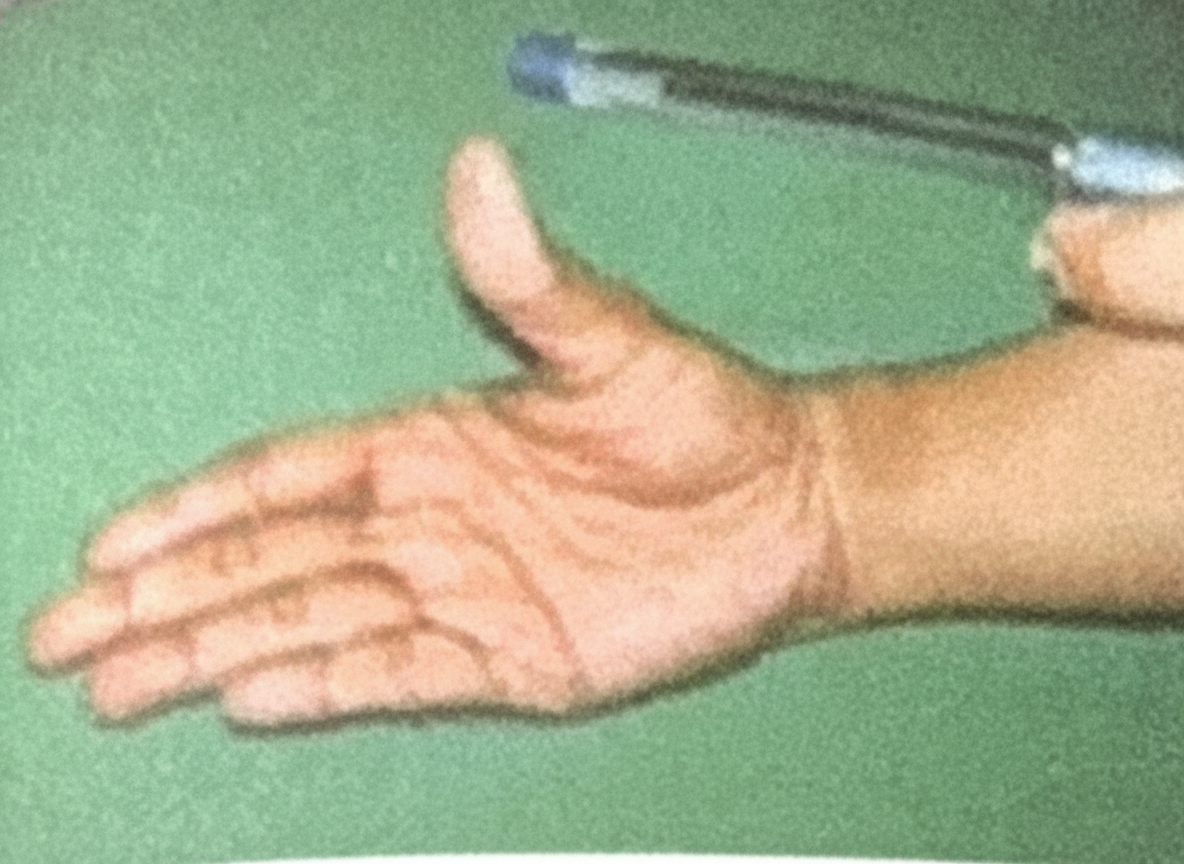
Practice by Chapter
Bones and joints of upper limb
Practice Questions
Muscles and movements of upper limb
Practice Questions
Nerves and blood supply of upper limb
Practice Questions
Clinical correlations of upper limb
Practice Questions
Bones and joints of lower limb
Practice Questions
Muscles and movements of lower limb
Practice Questions
Nerves and blood supply of lower limb
Practice Questions
Clinical correlations of lower limb
Practice Questions
Comparison of upper and lower limb structures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
