Pelvis/Perineum — MCQs

On this page
Q1
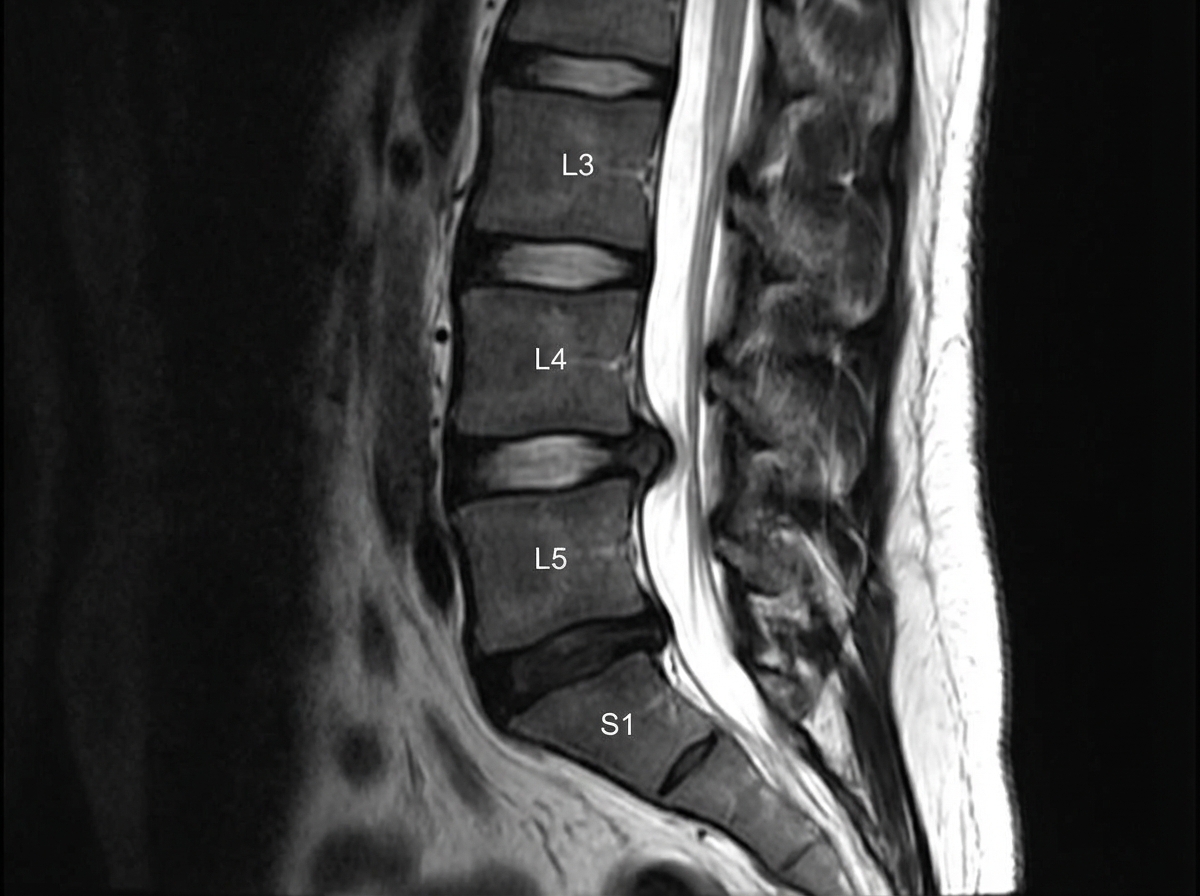
A slipped disc at the level shown in the image would most likely involve which nerve root?
Practice by Chapter
1
Pelvic girdle and ligaments
Practice Questions
2
Pelvic floor muscles
Practice Questions
3
Male reproductive organs
Practice Questions
4
Female reproductive organs
Practice Questions
5
Urinary bladder and urethra
Practice Questions
6
Rectum and anal canal
Practice Questions
7
Perineum and ischioanal fossa
Practice Questions
8
Pudendal nerve and internal pudendal vessels
Practice Questions
9
Pelvic vasculature and lymphatics
Practice Questions
10
Clinical correlations in pelvis/perineum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
