Neuroanatomy — MCQs

On this page
A 72-year-old man comes to his primary care provider because of double vision and headache. He says these symptoms developed suddenly last night and have not improved. He has had type 2 diabetes mellitus for 32 years and essential hypertension for 19 years for which he takes metformin and lisinopril. His last recorded A1c was 9.4%. He has smoked 10 to 15 cigarettes a day for the past 35 years. Family history is significant for chronic kidney disease in his mother. Vital signs reveal a temperature of 36.9 °C (98.42°F), blood pressure of 137/82 mm Hg, and pulse of 72/min. On examination, there is ptosis of the right eye and it is deviated down and out. Visual acuity is not affected in either eye. Which of the following cranial nerves is most likely impaired in this patient?
A 75-year-old woman is brought to the physician by her daughter for a 4-month history of increasing difficulty recognizing her friends and family. She has had to rely on recognizing haircuts, gait, and voices because she cannot remember their faces. Neurologic examination shows that she is able to recognize objects and name facial features such as the eyes and nose. On mental status examination, she is alert and has no deficits in cognition or short-term memory. An MRI of her head shows an inhomogeneous 2-cm mass with perifocal edema in her brain. Which of the following brain regions is most likely affected?
A 72-year-old man is brought to your office by his daughter due to concern over recent behavioral changes. Over the last several months he has had increasing difficulty with remembering recent events. She mentions that he is embarrassed due to a new inability to control urination. His medical history is significant for hypertension and insomnia. His medications include alprazolam and hydrochlorothiazide. On physical exam, he is oriented to time and place and thinks his daughter is exaggerating; however, when asked to recall 3 items, the patient refuses to continue the mental status exam. He has 5/5 strength bilaterally. He walks in short strides by sliding his feet across the floor. Which of the following would you expect to see in this patient?
A patient with a known spinal cord ependymoma presents to his neurologist for a check up. He complains that he has had difficulty walking, which he attributes to left leg weakness. On exam, he is noted to have 1/5 strength in his left lower extremity, as well as decreased vibration and position sensation in the left lower extremity and decreased pain and temperature sensation in the right lower extremity. Which of the following spinal cord lesions is most consistent with his presentation?
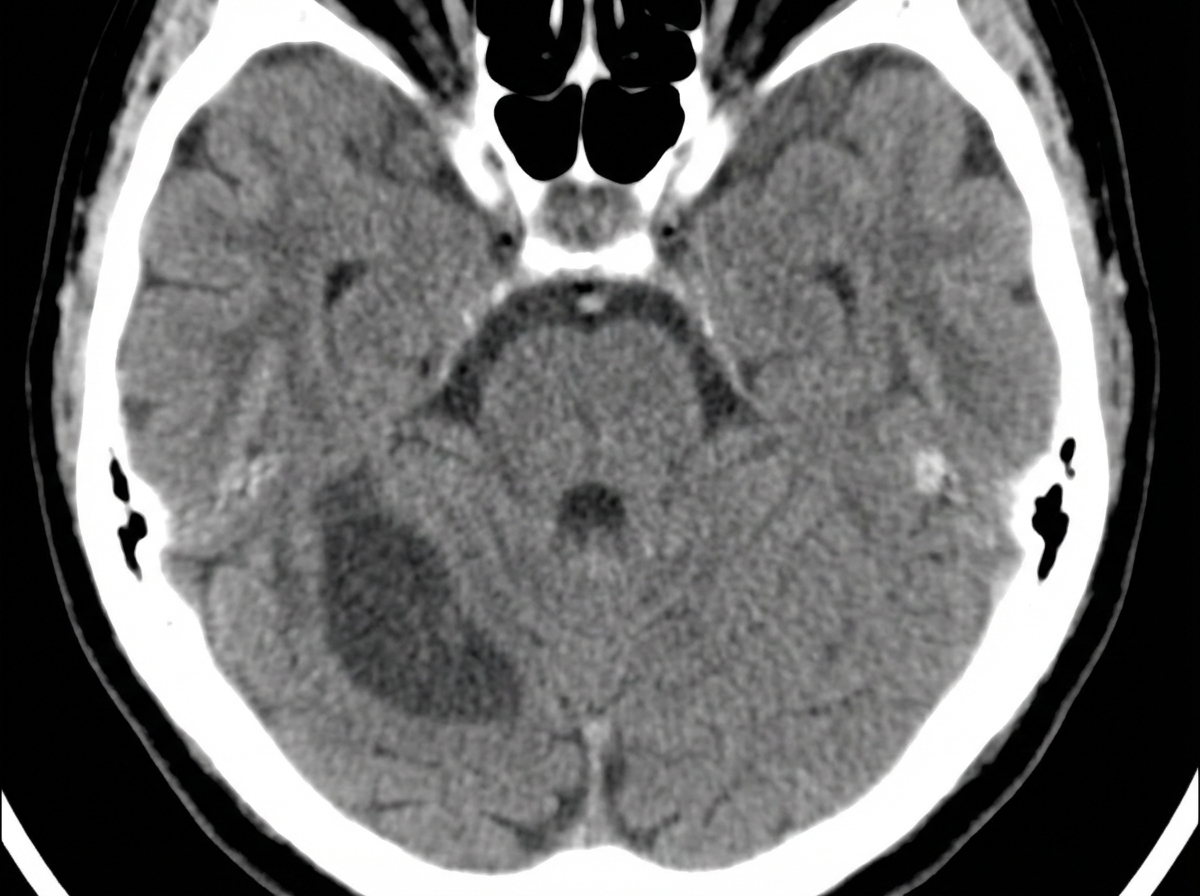
A 52-year-old man is brought to the emergency department while on vacation with a history of sudden onset vertigo and difficulty walking. He was in normal health since starting his vacation a week ago, but today he is suffering from a loss of balance, mild headache, and has had 5–6 episodes of vomiting over the last few hours. He denies fever, neck pain, head trauma, weakness, and diplopia. Past medical history is significant for hypertension and dyslipidemia. His medications include valsartan and atorvastatin, but he missed several doses since leaving for this trip. Blood pressure is 198/112 mm Hg, the heart rate is 76/min, the respiratory rate is 16/min, and the temperature is 37.0°C (98.6°F). The patient is awake and oriented to time, place, and person. Extraocular movements are within normal limits. Muscle strength is normal in all 4 extremities. An urgent head CT is ordered and shown in the picture. What additional clinical features would be expected in this patient?
A 5-year-old boy who recently emigrated from Nigeria is brought to the emergency department because of a 2-day history of lower leg weakness, swallowing difficulty, and drooling of saliva. He has not yet received any childhood vaccinations. Two days after admission, the patient develops shortness of breath. Pulse oximetry shows an oxygen saturation of 64%. Despite resuscitative efforts, the patient dies of respiratory failure. At autopsy, examination of the spinal cord shows destruction of the anterior horn cells. Neurological examination of this patient would have most likely shown which of the following findings?
Practice by Chapter
Cerebral cortex and lobes
Practice Questions
Basal ganglia
Practice Questions
Thalamus and hypothalamus
Practice Questions
Limbic system
Practice Questions
Cerebellum
Practice Questions
Spinal cord organization
Practice Questions
CSF production and circulation
Practice Questions
Meninges and blood-brain barrier
Practice Questions
Sensory pathways
Practice Questions
Motor pathways
Practice Questions
Functional neuroanatomy of vision
Practice Questions
Functional neuroanatomy of hearing and balance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
