Neuroanatomy — MCQs

On this page
A 32-year-old previously healthy female presents to her primary care physician with double vision. She first noted the double vision yesterday and saw no improvement this morning. She does not think it is worsening. She has not had any changes in her normal routine though she recalls one episode of right arm weakness 2 months ago. She did not seek treatment and the weakness subsided after several days. She does not have a history of head trauma. She denies headache, fever, chills, nausea, vomiting, paresthesias, extremity pain, or weakness. On exam she has right adduction palsy on leftward gaze. She has no focal weakness. Which of the following additional physical exam findings is associated with the lesion responsible for her ocular findings?
A 78-year-old right-handed male is brought in by ambulance after being found down in his home. After being aroused, the patient has difficulty answering questions and appears to be frustrated by his inability to communicate. He is able to speak his name and a few other words but his speech is not fluent. Subsequent neurologic exam finds that the patient is able to comprehend both one and two step instructions; however, he is unable to repeat phrases despite being able to understand them. He also has difficulty writing despite retaining fine motor control. CT reveals an acute stroke to his left hemisphere. Damage to which of the following sets of structures would be most likely to result in this pattern of deficits?
A 23-year-old man presents to the emergency room following a stab wound to the back. He was in a bar when he got into an argument with another man who proceeded to stab him slightly right of the midline of his back. He is otherwise healthy and does not take any medications. He has one previous admission to the hospital for a stab wound to the leg from another bar fight 2 years ago. His temperature is 99°F (37.2°C), blood pressure is 115/80 mmHg, pulse is 100/min, and pulse oximetry is 99% on room air. Cardiopulmonary and abdominal exams are unremarkable; however, he has an abnormal neurologic exam. If this wound entered his spinal cord but did not cross the midline, which of the following would most likely be seen in this patient?
A 63-year-old man is brought to the emergency department by his wife because she is concerned he is having another stroke. The patient says he woke up with right-sided facial weakness and drooping. Past medical history is significant for a recent case of shingles treated with acyclovir, and a stroke, diagnosed 10 years ago, from which he recovered with no residual functional deficits. On physical examination, there is weakness and drooping of the entire right side of the face. Sensation is intact. The remainder of the physical examination is unremarkable. Which of the following additional findings would also most likely be seen in this patient?
A 25-year-old previously healthy woman presents to her PCP reporting cessation of menses for the past 6 months. Previously, her period occurred regularly, every 30 days. She also complains of decreased peripheral vision, most noticeably when she is driving her car. She denies any recent sexual activity and a pregnancy test is negative. Upon further work-up, what physical exam finding is most likely to be identified?
A 4-year-old boy is brought to the physician because of a progressive headache and neck pain for 2 weeks. During this period, he has had multiple episodes of dizziness and tingling sensations in his arms and hands. A year ago, he underwent closed reduction of a dislocated shoulder that he suffered after a fall. He underwent surgical removal of a sac-like protuberance on his lower back, soon after being born. His temperature is 36.7°C (98°F), pulse is 80/min, and blood pressure is 100/80 mm Hg. His neck is supple. Neurological examination shows sensorineural hearing loss bilaterally and normal gross motor function. Fundoscopy reveals bilateral optic disk swelling. An MRI of the brain is shown. Which of the following is the most likely cause of this patient's symptoms?
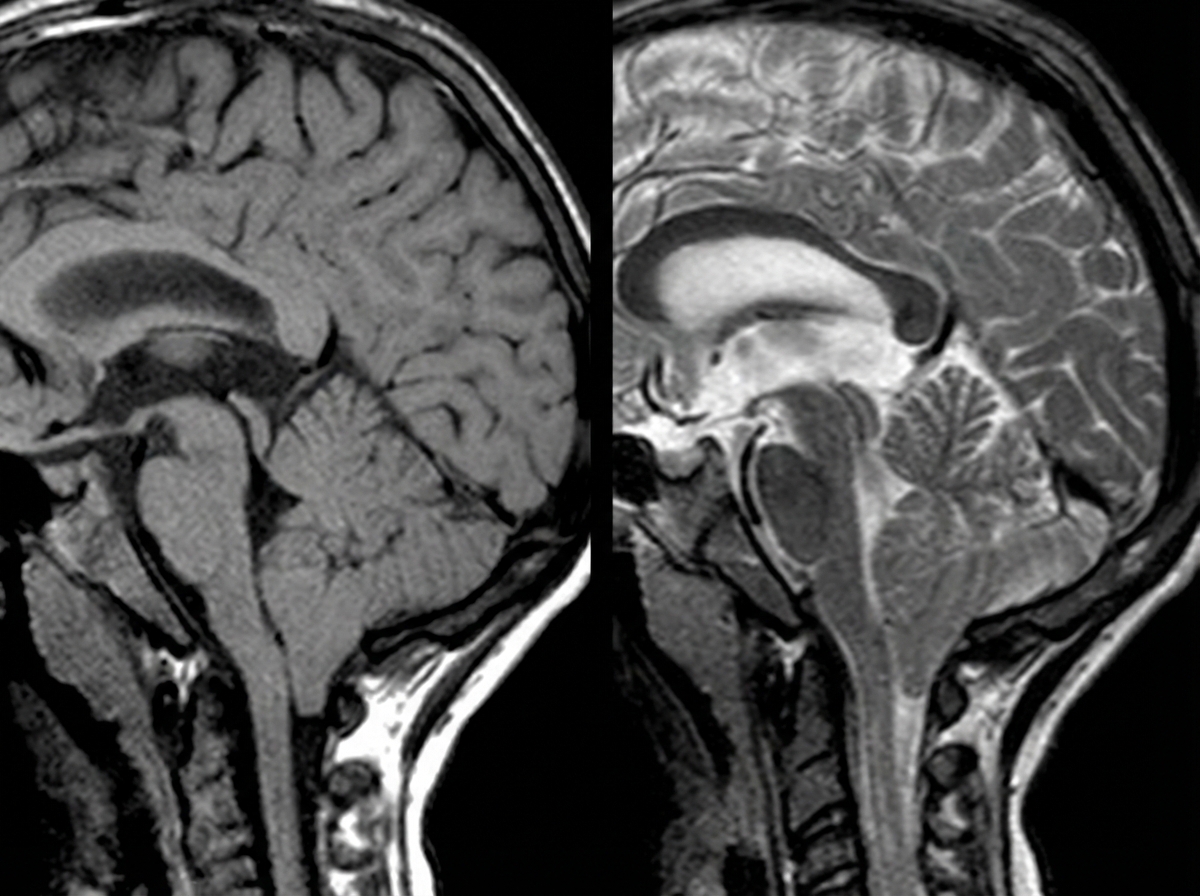
A 71-year-old woman presents to the emergency department with a headache for the past 30 minutes. She says that this is the worst headache of her life and that it came on suddenly after she hit her head. She says that she has also been experiencing visual problems with double vision when she looks to the left or the right. Visual examination reveals that her right eye cannot move right past the midline and her left eye cannot move left past the midline. Which of the following is most likely responsible for this patient's visual defects?
A 64-year-old man presents to his primary care clinic for a regular checkup. He reports feeling depressed since his wife left him 6 months prior and is unable to recall why she left him. He denies any sleep disturbance, change in his eating habits, guilt, or suicidal ideation. His past medical history is notable for hypertension, gout, and a myocardial infarction five years ago. He takes lisinopril, aspirin, metoprolol, and allopurinol. He has a 50 pack-year smoking history and was previously a heroin addict but has not used in over 20 years. He drinks at least 6 beers per day. His temperature is 98.6°F (37°C), blood pressure is 155/95 mmHg, pulse is 100/min, and respirations are 18/min. He appears somewhat disheveled, inattentive, and smells of alcohol. During his prior visits, he has been well-groomed and attentive. When asked what year it is and who the president is, he confidently replies “1999” and “Jimmy Carter.” He says his son’s name is “Peter” when it is actually “Jake.” This patient likely has a lesion in which of the following brain regions?
A 58-year-old man comes to the physician because of burning pain in his neck and arms for a year. He has also had paresthesias in his hands during this period. He has had increasing weakness in both hands during the past 3 months. He has type 2 diabetes mellitus, hypercholesterolemia, and hypertension. He was involved in a motor vehicle collision 3 years ago. Current medications include metformin, sitagliptin, enalapril, atorvastatin, and aspirin. He has had 7 sexual partners in his lifetime; he uses condoms inconsistently. He is oriented to time, place, and person. Vital signs are within normal limits. The pupils are equal and reactive to light. Examination of the upper extremities shows decreased muscle strength, absent reflexes, and decreased hand grip with fasciculations bilaterally. Sensation to temperature and pain is absent over the chest and bilateral upper arms. Vibration and joint position sensations are present in the upper limbs. Cranial nerve examination shows no focal findings. Examination of the lower extremities show no abnormalities. Which of the following is the most likely diagnosis?
A 26-year-old man comes to the physician for a follow-up examination. Two weeks ago, he was treated in the emergency department for head trauma after being hit by a bicycle while crossing the street. Neurological examination shows decreased taste on the right anterior tongue. This patient's condition is most likely caused by damage to a cranial nerve that is also responsible for which of the following?
Practice by Chapter
Cerebral cortex and lobes
Practice Questions
Basal ganglia
Practice Questions
Thalamus and hypothalamus
Practice Questions
Limbic system
Practice Questions
Cerebellum
Practice Questions
Spinal cord organization
Practice Questions
CSF production and circulation
Practice Questions
Meninges and blood-brain barrier
Practice Questions
Sensory pathways
Practice Questions
Motor pathways
Practice Questions
Functional neuroanatomy of vision
Practice Questions
Functional neuroanatomy of hearing and balance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
