Neuroanatomy — MCQs

On this page
A 52-year-man is brought to the physician because of a 2-week history of memory loss. Three weeks ago, he had a cardiac arrest that required cardiopulmonary resuscitation and intravenous epinephrine. On mental status examination, he cannot recall objects shown to him 20 minutes earlier but vividly recalls memories from before the incident. The remainder of the examination shows no abnormalities. Which of the following structures of the brain is most likely affected?
A 54-year-old man is brought to the emergency department 30 minutes after being hit by a car while crossing the street. He had a left-sided tonic-clonic seizure and one episode of vomiting while being transported to the hospital. On arrival, he is not oriented to person, place, or time. Physical examination shows flaccid paralysis of all extremities. A CT scan of the head is shown. This patient's symptoms are most likely the result of a hemorrhage in which of the following structures?
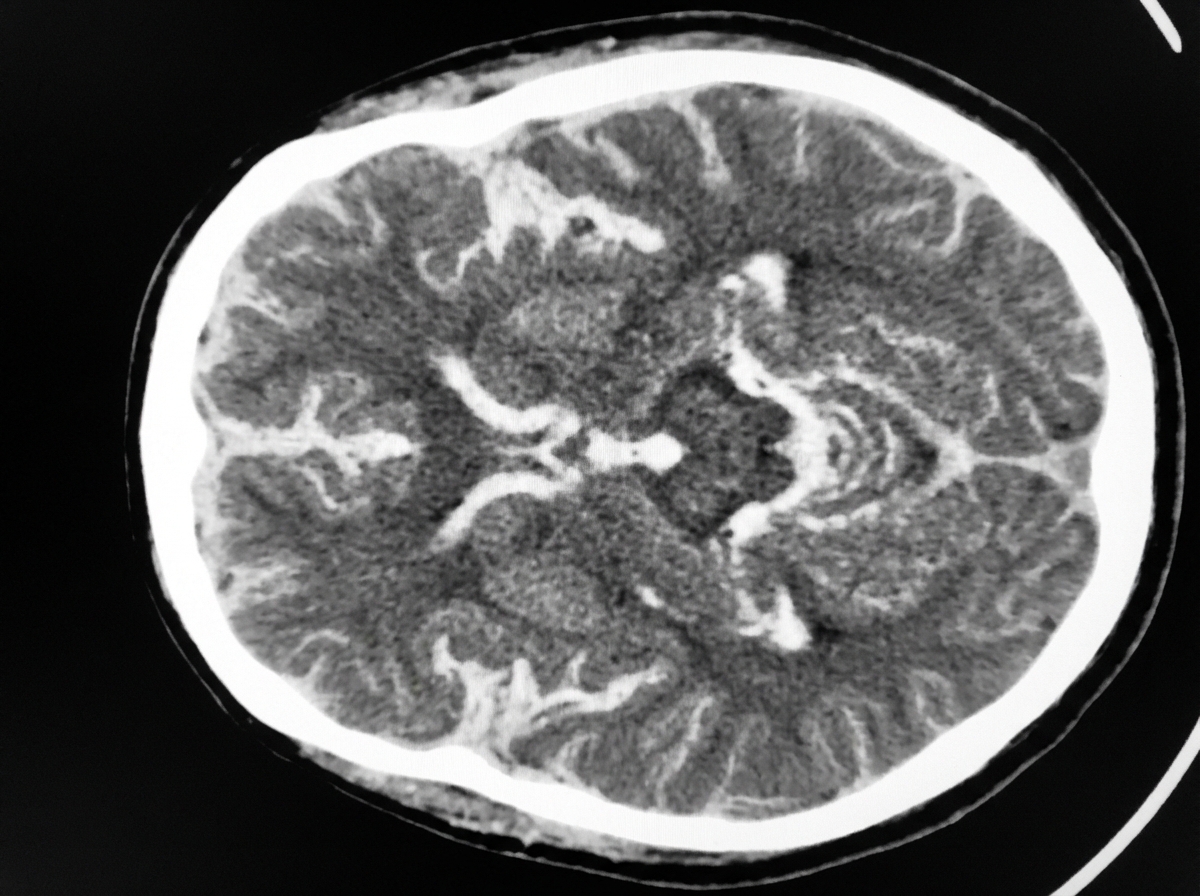
A 54-year-old man is referred to a tertiary care hospital with a history of 5 months of progressive difficulty in walking and left leg numbness. He first noticed mild gait unsteadiness and later developed gradual right leg weakness. His left leg developed progressive numbness and tingling. His blood pressure is 138/88 mm Hg, the heart rate is 72/min, and the temperature is 36.7°C (98.2°F). On physical examination, he is alert and oriented to person, place, and time. Cranial nerves are intact. Muscle strength is 5/5 in both upper extremities and left lower extremity, but 3/5 in the right leg with increased tone. The plantar reflex is extensor on the right. Pinprick sensation is decreased on the left side below the umbilicus. Vibration and joint position senses are decreased in the right foot and leg. All sensations are normal in the upper extremities. Finger-to-nose and heel-to-shin testing are normal. This patient’s lesion is most likely located in which of the following parts of the nervous system?
A 67-year-old female patient is brought to the emergency department after her daughter noticed she has been having meaningless speech. When assessing the patient, she calls the chair a table, and at times would make up new words. She does not appear to be aware of her deficit, and is carrying on an empty conversation. Her speech is fluent, but with paraphasic errors. Her repetition is impaired. On physical examination, a right upper quadrant field-cut is appreciated, with impairment in comprehension and repetition. Which of the following structures is most likely involved in this patient’s presentation?
A 67-year-old man is brought to the physician by his daughter because he frequently misplaces his personal belongings and becomes easily confused. His daughter mentions that his symptoms have progressively worsened for the past one year. On mental status examination, he is oriented to person, place, and time. He vividly recalls memories from his childhood but can only recall one of three objects presented to him after 5 minutes. His affect is normal. This patients' symptoms are most likely caused by damage to which of the following?
A 72-year-old man presents to his primary care physician due to worsening headache and double vision. His headache began several months ago, and he describes them as sharp and localized to the left side of the head. His double vision began one week prior to presentation. Medical history is significant for hypertension and type II diabetes mellitus, which is treated with lisinopril and metformin. He smokes a pack of cigarettes a day for the last 40 years. His temperature is 98.3°F (37°C), blood pressure is 148/84 mmHg, pulse is 60/min, and respirations are 14/min. On physical exam, a mild head turning towards the left is appreciated. Pupils are equal, round, and reactive to light, with a more pronounced esotropia on left-lateral gaze. The rest of the neurologic exam is otherwise normal. Magnetic resonance imaging (MRI) of the head and MR angiography shows a left-sided intracavernous carotid aneurysm. Which of the following nerves is most likely compressed by the aneurysm in this patient?
A 35-year-old man who suffered a motor vehicle accident 3 months ago presents to the office for a neurological evaluation. He has no significant past medical history and takes no current medications. He has a family history of coronary artery disease in his father and Alzheimer’s disease in his mother. On physical examination, his blood pressure is 110/60 mm Hg, the pulse is 85/min, the temperature is 37.0°C (98.6°F), and the respiratory rate is 20/min. Neurological examination is suggestive of a lesion in the anterior spinal artery that affects the anterior two-thirds of the spinal cord, which is later confirmed with angiography. Which of the following exam findings would have suggested this diagnosis?
A 73-year-old man presents to your office accompanied by his wife. He has been experiencing a tremor in his right hand for the last several months that seems to be worsening. He does not have any other complaints and says he’s “fine.” His wife thinks that he has also had more difficulty walking. His history is significant for hypertension and an ischemic stroke of the right middle cerebral artery 2 years ago. His medications include hydrochlorothiazide and daily aspirin. On physical exam you note that the patient speaks with a soft voice and has decreased facial expressions. He has a resting tremor that is worse on the right side. He has increased resistance to passive movement when you flex and extend his relaxed wrist. He has 5/5 strength bilaterally. Neuronal degeneration in which of the following locations is most likely responsible for the progression of this disease?
A 27-year-old man is brought to the emergency department because of a knife wound to his back. His pulse is 110/min, respirations are 14/min, and blood pressure is 125/78 mm Hg. Examination shows a 5-cm deep stab wound at the level of T9. He withdraws the right foot to pain but is unable to sense vibration or whether his right toe is flexed or extended. Sensation in the left leg is normal. Motor strength is 5/5 in all extremities. Rectal tone is normal. Which of the following spinal column structures was most likely affected?
A 60-year-old man is brought to the emergency department because of a 1-hour history of disorientation and slurred speech. He has a 10-year history of hypertension and hypercholesterolemia. His blood pressure is 210/110 mm Hg, and pulse is 90/min. Once the patient is stabilized, an MRI of the brain is performed, which shows an infarct of the left precentral gyrus involving the facial motor cortex. Given the MRI findings, which of the following neurological findings would most be expected?
Practice by Chapter
Cerebral cortex and lobes
Practice Questions
Basal ganglia
Practice Questions
Thalamus and hypothalamus
Practice Questions
Limbic system
Practice Questions
Cerebellum
Practice Questions
Spinal cord organization
Practice Questions
CSF production and circulation
Practice Questions
Meninges and blood-brain barrier
Practice Questions
Sensory pathways
Practice Questions
Motor pathways
Practice Questions
Functional neuroanatomy of vision
Practice Questions
Functional neuroanatomy of hearing and balance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
