Neuroanatomy — MCQs

On this page
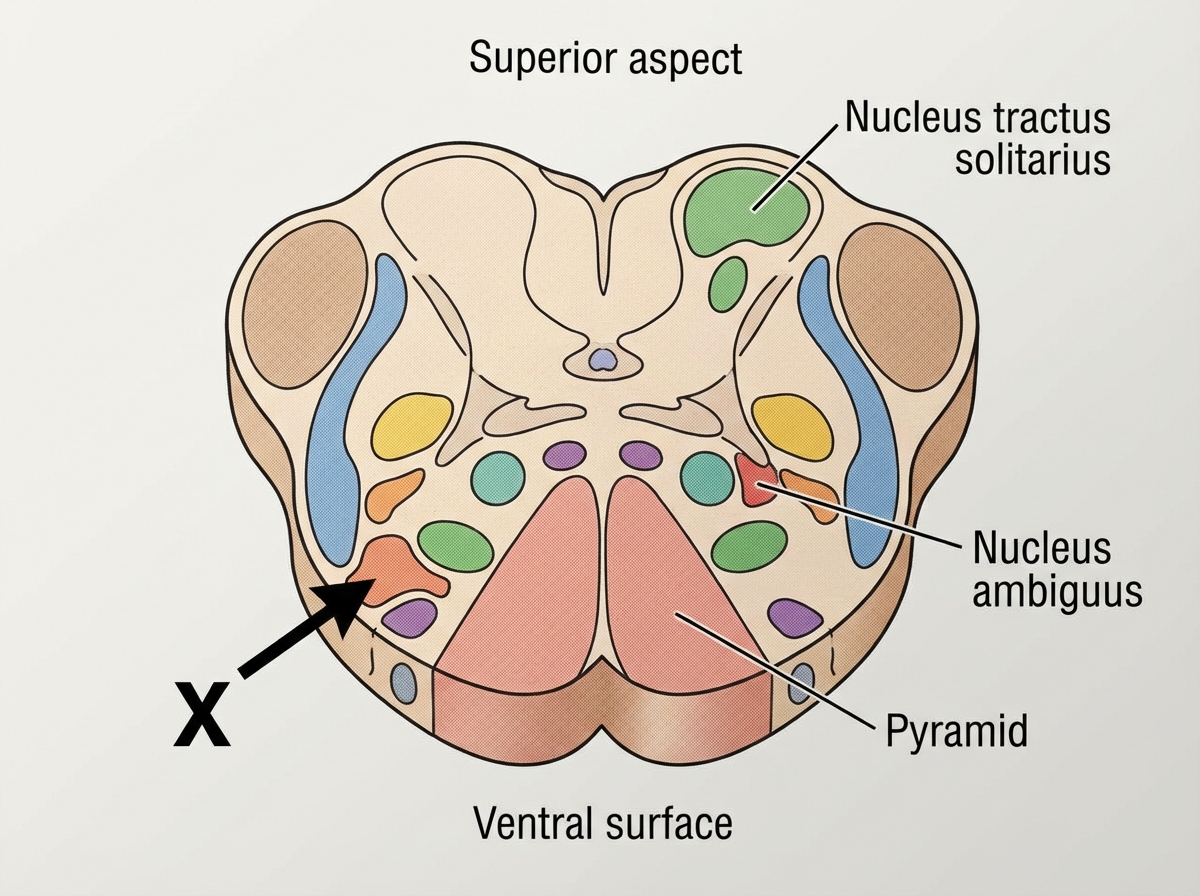
Name the center shown as $X$ in the cut section of medulla which is responsible for control of respiration.
Practice by Chapter
Cerebral cortex and lobes
Practice Questions
Basal ganglia
Practice Questions
Thalamus and hypothalamus
Practice Questions
Limbic system
Practice Questions
Cerebellum
Practice Questions
Spinal cord organization
Practice Questions
CSF production and circulation
Practice Questions
Meninges and blood-brain barrier
Practice Questions
Sensory pathways
Practice Questions
Motor pathways
Practice Questions
Functional neuroanatomy of vision
Practice Questions
Functional neuroanatomy of hearing and balance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
