Imaging/Clinical — MCQs

On this page
A 27-year-old man presents to the emergency department with back pain. The patient states that he has back pain that has been steadily worsening over the past month. He states that his pain is worse in the morning but feels better after he finishes at work for the day. He rates his current pain as a 7/10 and says that he feels short of breath. His temperature is 99.5°F (37.5°C), blood pressure is 130/85 mmHg, pulse is 80/min, respirations are 14/min, and oxygen saturation is 99% on room air. On physical exam, you note a young man who does not appear to be in any distress. Cardiac exam is within normal limits. Pulmonary exam is notable only for a minor decrease in air movement bilaterally at the lung bases. Musculoskeletal exam reveals a decrease in mobility of the back in all four directions. Which of the following is the best initial step in management of this patient?
A 71-year-old man with type 2 diabetes mellitus comes to the physician because of a 9-month history of pain and stiffness in the right knee. He reports that the stiffness lasts approximately 10 minutes after waking up and that the pain is worse in the evening. There is no history of trauma. He is 175 cm (5 ft 9 in) tall and weighs 102 kg (225 lb); BMI is 33 kg/m2. Examination of the right knee shows tenderness in the anteromedial joint line and crepitus during knee movement. Laboratory studies show an erythrocyte sedimentation rate of 15 mm/h and a serum uric acid concentration of 6.9 mg/dL. Which of the following is the most likely finding on imaging of the right knee?
A 45-year-old male alcoholic presents with fever, productive cough, and foul-smelling sputum for the past two weeks. Vital signs are T 38.3 C, HR 106, BP 118/64 and RR 16. Oxygen saturation on room air is 90%. Given a diagnosis of aspiration pneumonia, initial chest radiograph findings would most likely include:
A 65-year-old man is referred by his primary care provider to a neurologist for leg pain. He reports a 6-month history of progressive bilateral lower extremity pain that is worse in his left leg. The pain is 5/10 in severity at its worst and is described as a "burning" pain. He has noticed that the pain is acutely worse when he walks downhill. He has started riding his stationary bike more often as it relieves his pain. His past medical history is notable for hypertension, diabetes mellitus, and a prior myocardial infarction. He also sustained a distal radius fracture the previous year after falling on his outstretched hand. He takes aspirin, atorvastatin, metformin, glyburide, enalapril, and metoprolol. He has a 30-pack-year smoking history and drinks 2-3 glasses of wine with dinner every night. His temperature is 99°F (37.2°C), blood pressure is 145/85 mmHg, pulse is 91/min, and respirations are 18/min. On exam, he is well-appearing and in no acute distress. A straight leg raise is negative. A valsalva maneuver does not worsen his pain. Which of the following is the most appropriate test to confirm this patient's diagnosis?
A 41-year-old woman presents with back pain for the past 2 days. She says that the pain radiates down along the posterior right thigh and leg. She says the pain started suddenly after lifting a heavy box 2 days ago. Past medical history is irrelevant. Physical examination reveals a straight leg raise (SLR) test restricted to 30°, inability to walk on her toes, decreased sensation along the lateral border of her right foot, and diminished ankle jerk on the same side. Which of the following nerve roots is most likely compressed?
A 33-year-old man comes to the otolaryngologist for the evaluation of a 6-month history of difficulty breathing through his nose and clear nasal discharge. He has a history of seasonal atopic rhinosinusitis. Anterior rhinoscopy shows a nasal polyp obstructing the superior nasal meatus. A CT scan of the head is most likely to show opacification of which of the following structures?
A 28-year-old man is brought to the emergency department by ambulance after developing an altered mental state following blunt trauma to the head. The patient was competing at a local mixed martial arts competition when he was struck in the head and lost consciousness. A few minutes later, upon regaining consciousness, he had a progressive decline in mental status. Past medical history is noncontributory. Upon arrival at the hospital, the temperature is 37.0°C (98.6°F), the blood pressure is 145/89 mm Hg, the pulse is 66/min, the respiratory rate is 14/min, and the oxygen saturation is 99% on room air. He is alert now. A noncontrast CT scan is performed, and the result is provided in the image. Which of the following structures is most likely affected in this patient?
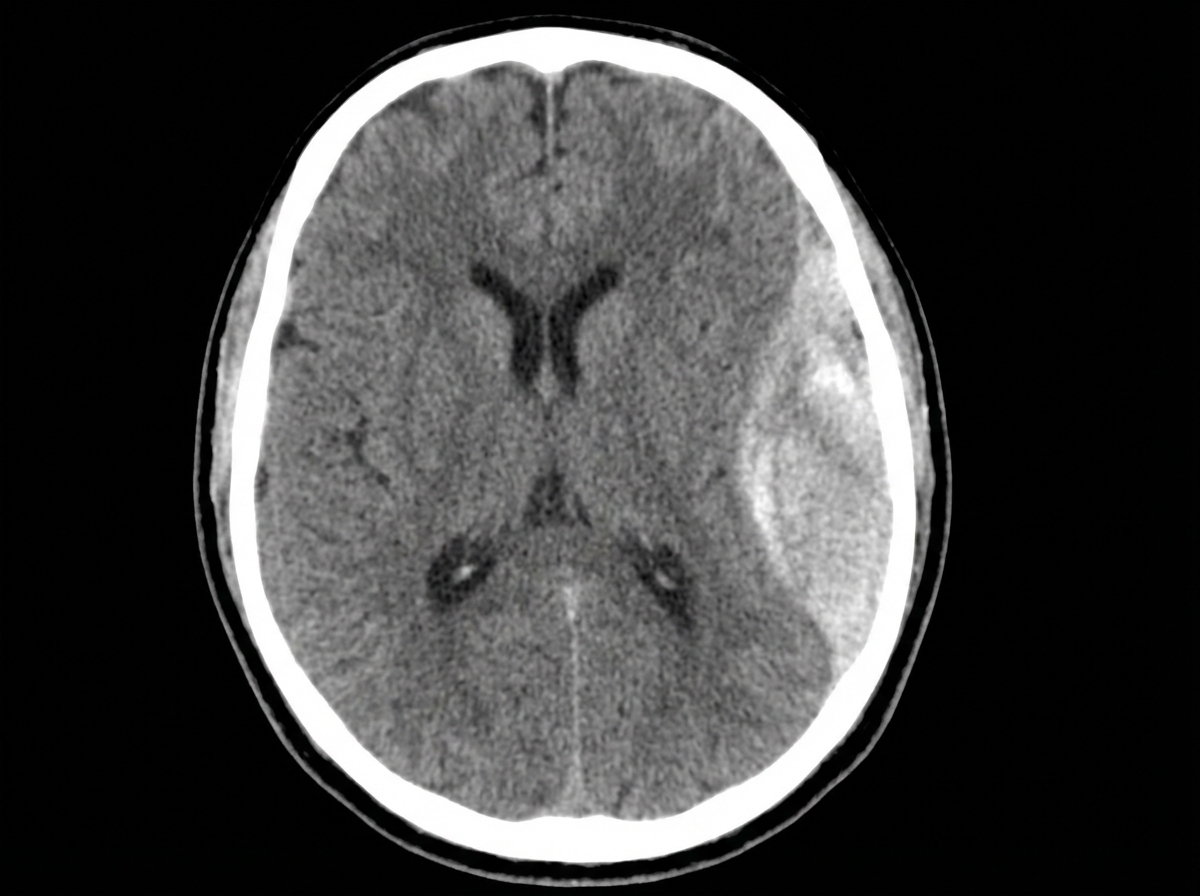
A 52-year-old man is brought to the emergency department by a friend because of a 5-day history of fever and cough productive of purulent sputum. One week ago, he was woken up by an episode of heavy coughing while lying on his back. He drinks large amounts of alcohol daily and has spent most of his time in bed since his wife passed away 2 months ago. His temperature is 38°C (100.4°F), pulse is 96/min, respirations are 24/min, and blood pressure is 110/84 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 87%. Physical examination shows poor dentition and swollen gums. A CT scan of the chest is most likely to show a pulmonary infiltrate in which of the following locations?
A 45-year-old man is brought to the emergency department 30 minutes after falling off a staircase and hitting his head on the handrail. He was unconscious for 10 minutes and vomited twice. On arrival, he is drowsy. Examination shows a fixed, dilated left pupil and right-sided flaccid paralysis. A CT scan of the head shows a skull fracture in the region of the pterion and a biconvex hyperdensity overlying the left frontotemporal lobe. This patient's condition is most likely caused by damage to a vessel that enters the skull through which of the following foramina?
A 5-year-old girl presents to the physician with increased muscle cramping in her lower extremities after walking extended distances. The young girl is in the 10th percentile for height. Her past medical history is notable only for a cystic hygroma detected shortly after birth. Which of the following findings is most likely in this patient?
Practice by Chapter
X-ray principles and interpretation
Practice Questions
CT scan principles and interpretation
Practice Questions
MRI principles and interpretation
Practice Questions
Ultrasound principles and interpretation
Practice Questions
Nuclear medicine imaging
Practice Questions
Angiography techniques
Practice Questions
Contrast studies
Practice Questions
Interventional radiology procedures
Practice Questions
Emergency imaging protocols
Practice Questions
Anatomical variants in imaging
Practice Questions
Common radiologic findings in pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
