Head & Neck — MCQs

On this page
Impaired gag reflex is seen due to a lesion in which cranial nerves?
Which tongue papillae do not have taste buds?
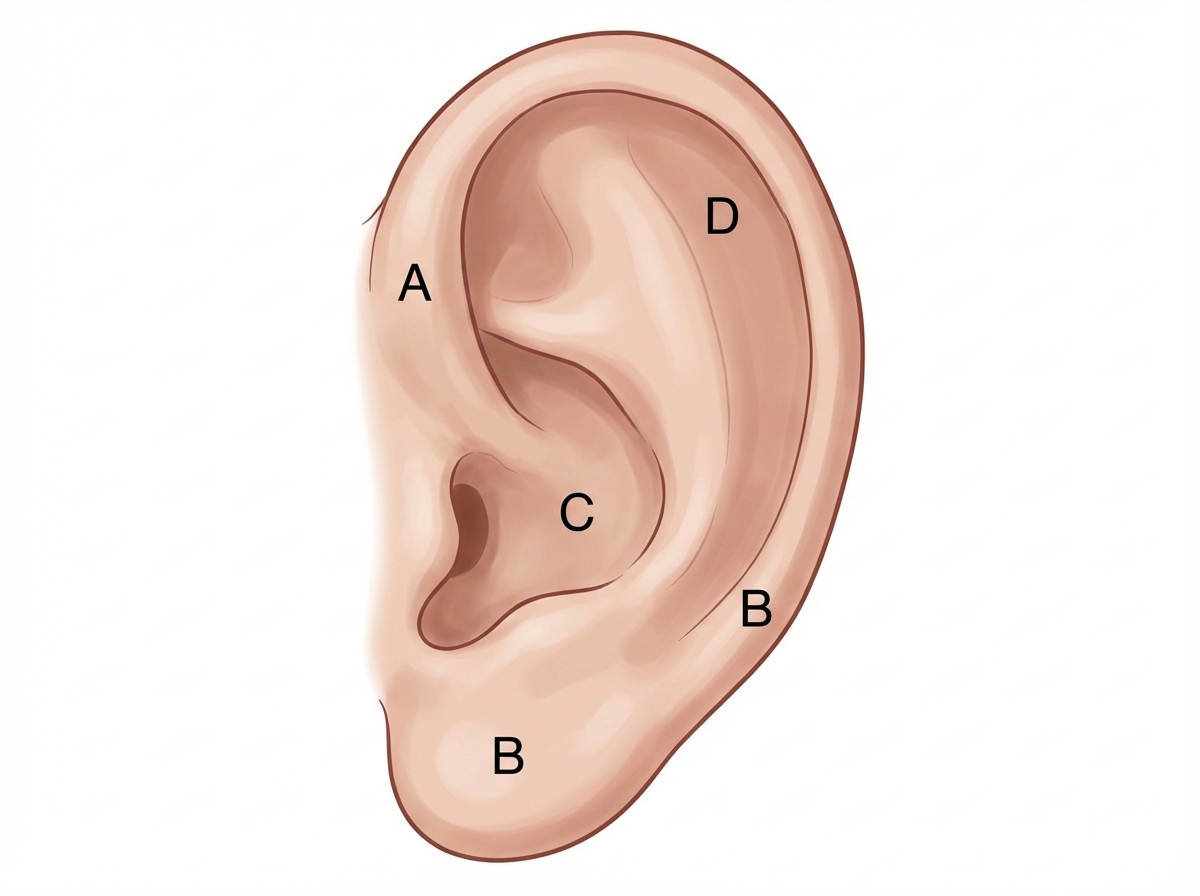
Match the following nerves to their respective areas of supply to the auricle
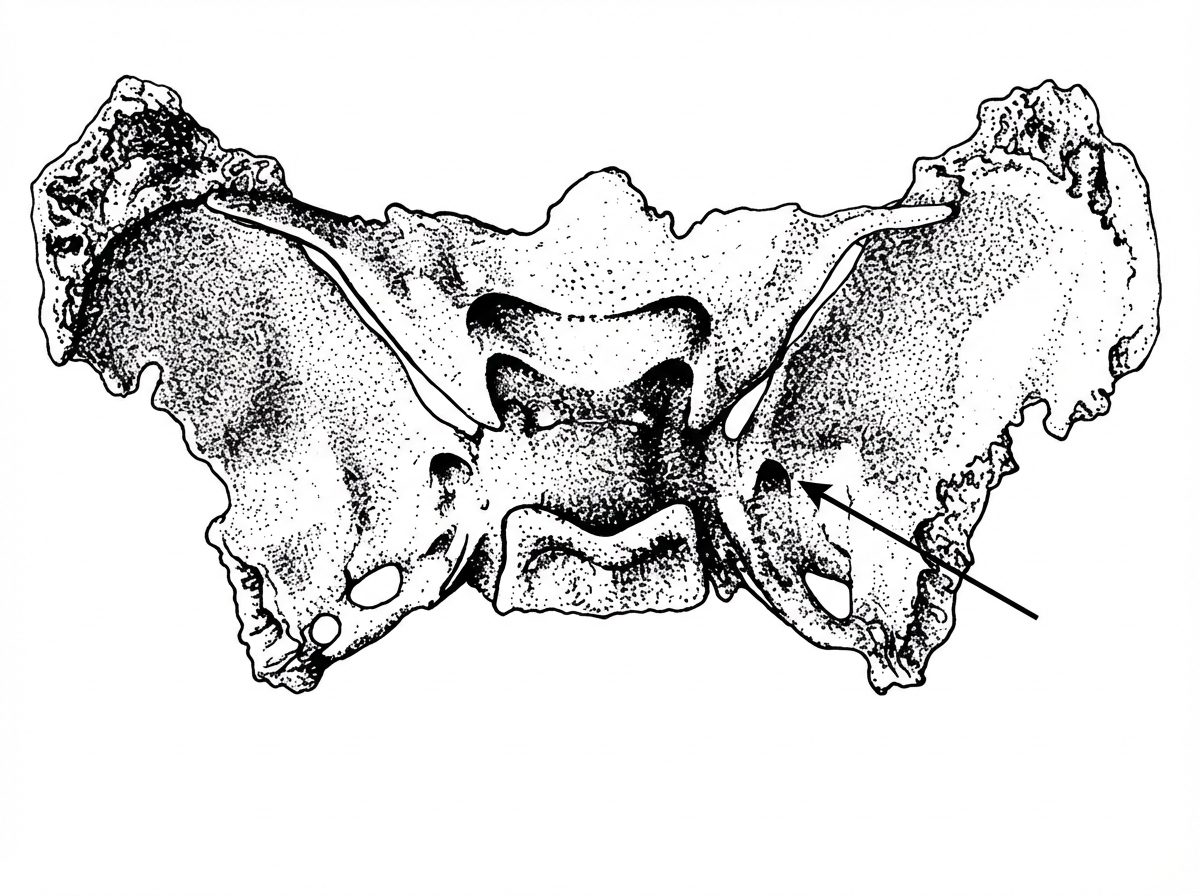
The nerve passing through the arrow-marked region in the provided image has been lesioned. Which of the following is the most likely clinical presentation?
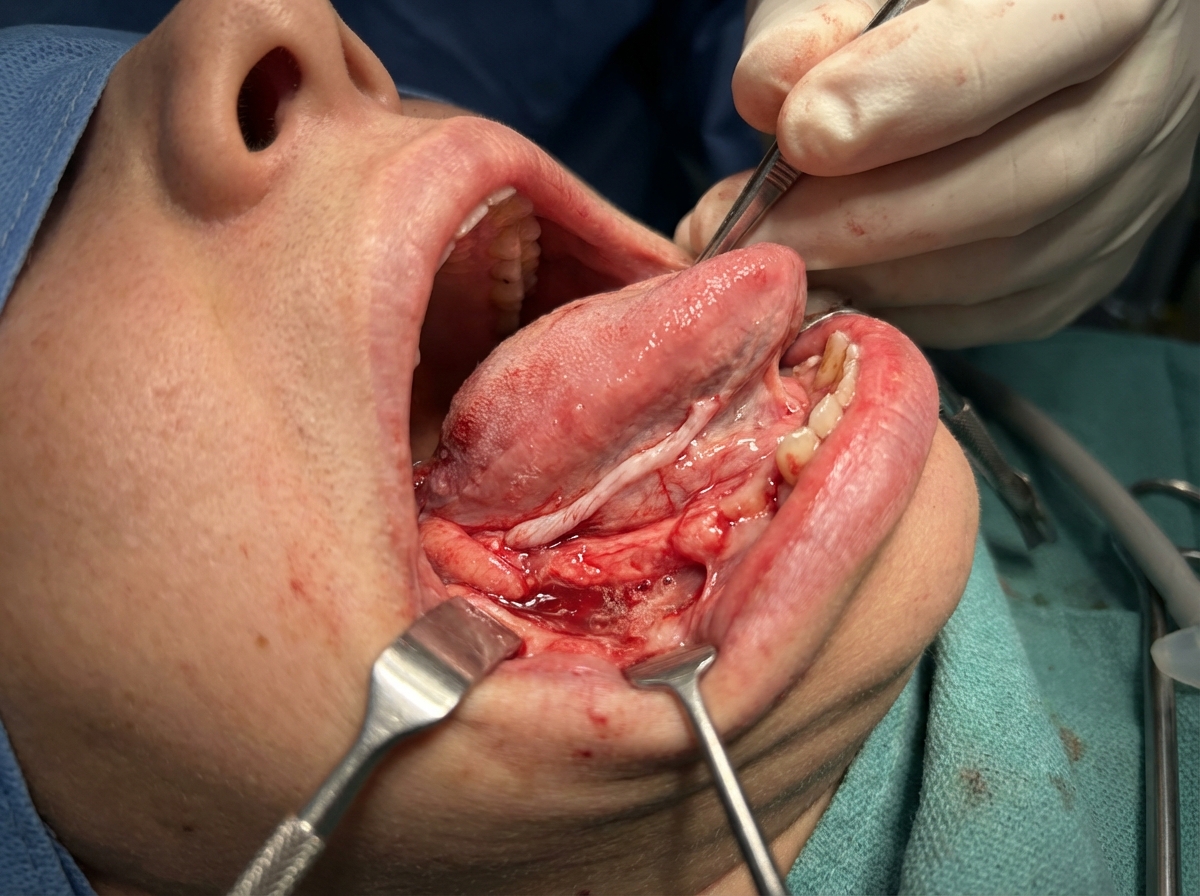
An absent gag reflex can result from injury to which of the following nerves?
Which of the following statements is true regarding the structure shown in the image?
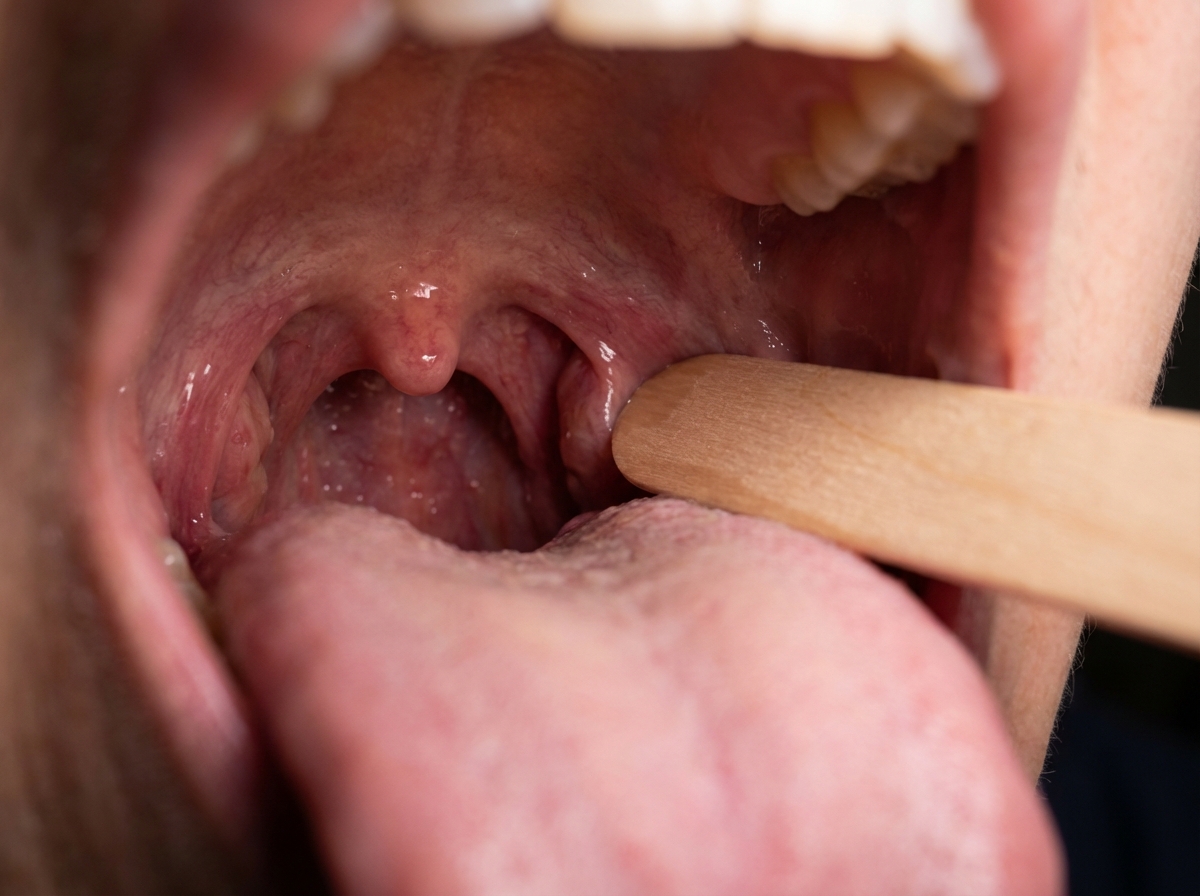
A patient was admitted with skull base trauma. The doctor was testing the marked structure in the pharyngeal region. Which of the following nerves was being tested?
Which nerve is responsible for gag reflex
A 32-year-old man presents to the emergency department with a severe headache. He says that the pain has been getting progressively worse over the last 24 hours and is located primarily in his left forehead and eye. The headaches have woken him up from sleep and it is not relieved by over-the-counter medications. He has been recovering from a sinus infection that started 1 week ago. His past medical history is significant for type 1 diabetes and he has a 10 pack-year history of smoking. Imaging shows thrombosis of a sinus above the sella turcica. Which of the following findings would most likely also be seen in this patient?
A 57-year-old man comes to the physician for a follow-up examination. During the last 6 months, he has had recurring pneumonia after undergoing a surgical operation. He reports that, when food has gone down his windpipe, he has not automatically coughed. Examination shows normal voluntary coughing, but an impaired cough reflex. The nerve responsible for this patient's symptoms is most likely damaged at which of the following anatomical sites?
Practice by Chapter
Skull and cranial cavity
Practice Questions
Face and scalp
Practice Questions
Orbital structures
Practice Questions
Ear anatomy and vestibular system
Practice Questions
Nasal cavity and paranasal sinuses
Practice Questions
Oral cavity and pharynx
Practice Questions
Larynx and vocal apparatus
Practice Questions
Triangles of the neck
Practice Questions
Deep structures of the neck
Practice Questions
Cranial nerves and their pathways
Practice Questions
Cervical sympathetic chain
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
