Gross Anatomy — MCQs

On this page
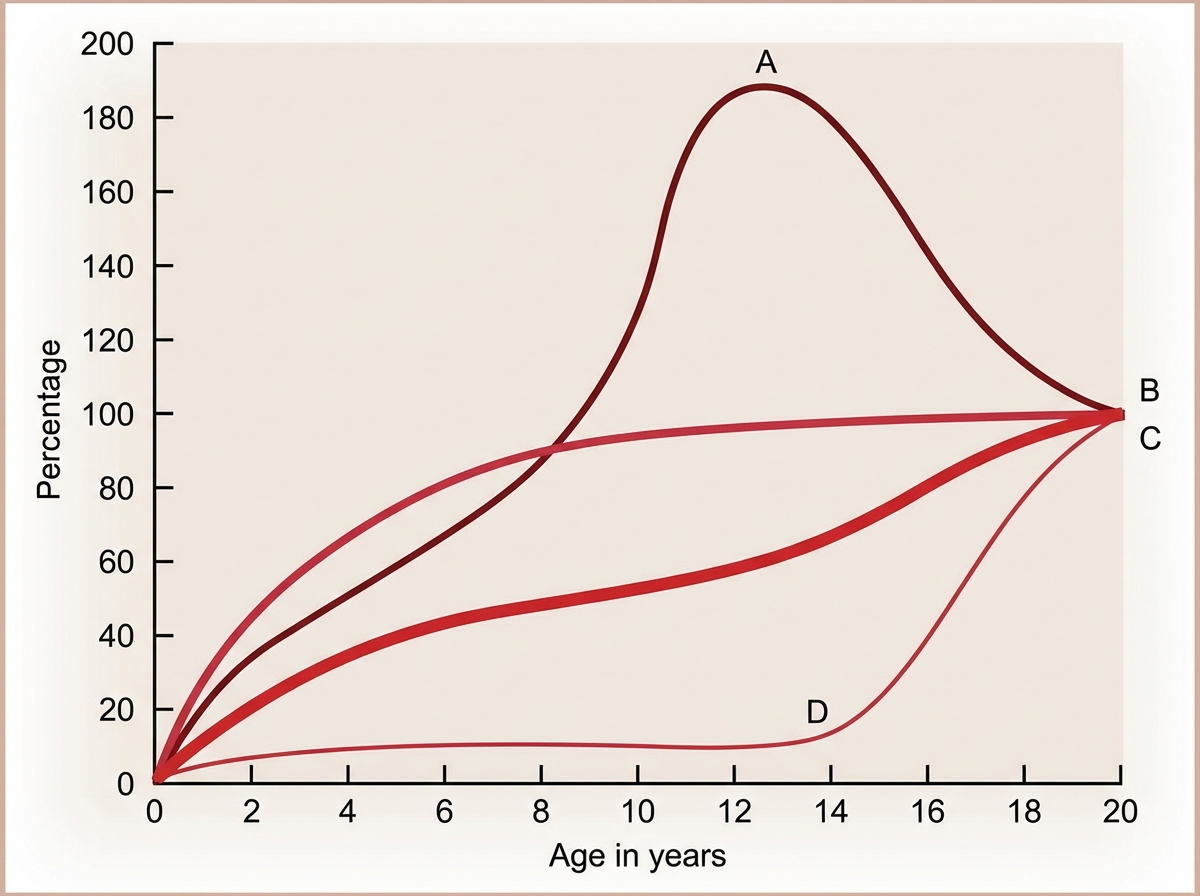
The Image shows the growth curve of different organs with age. Identify A in the graph.
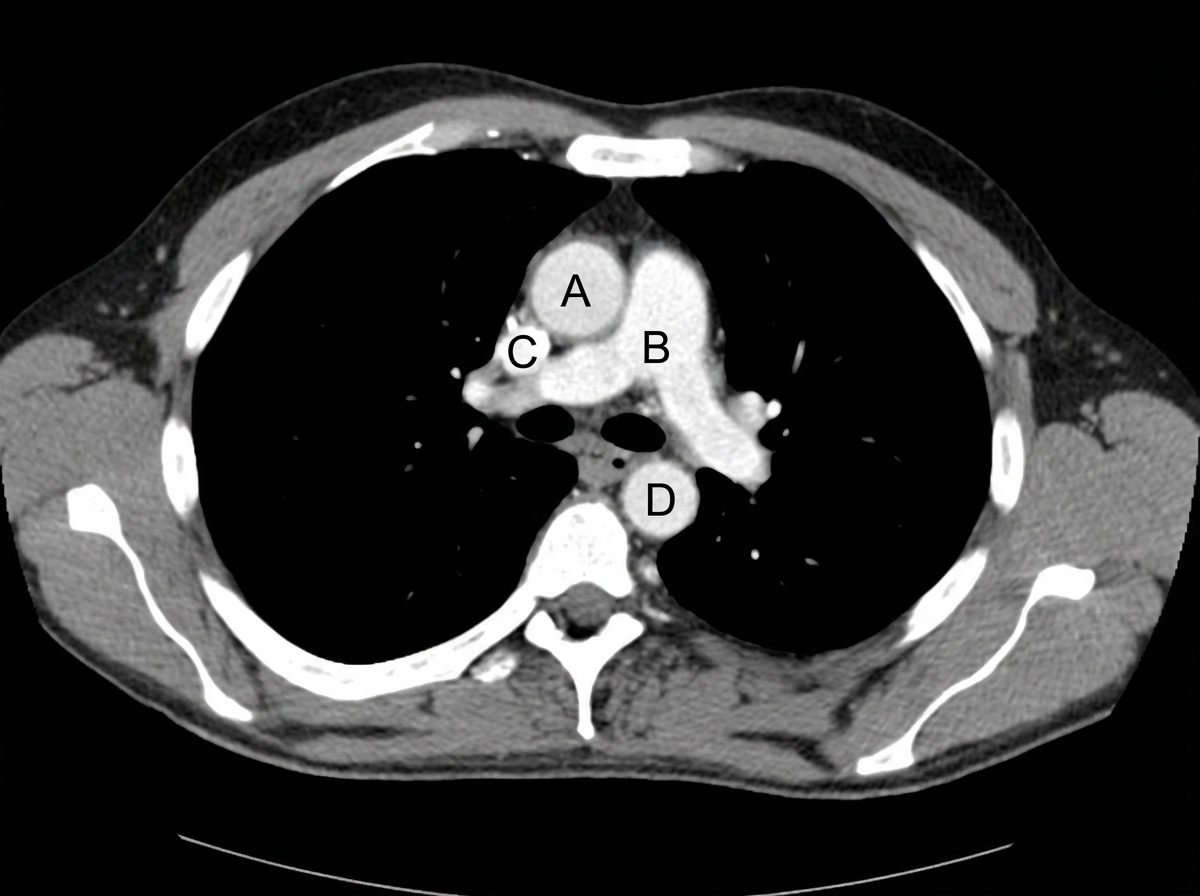
Identify the labeled structures correctly in the axial CT image of the thorax
Linear growth of bone is disturbed when a fracture occurs in which part?
The Image shows the growth curve of different organs with age. Identify A in the graph
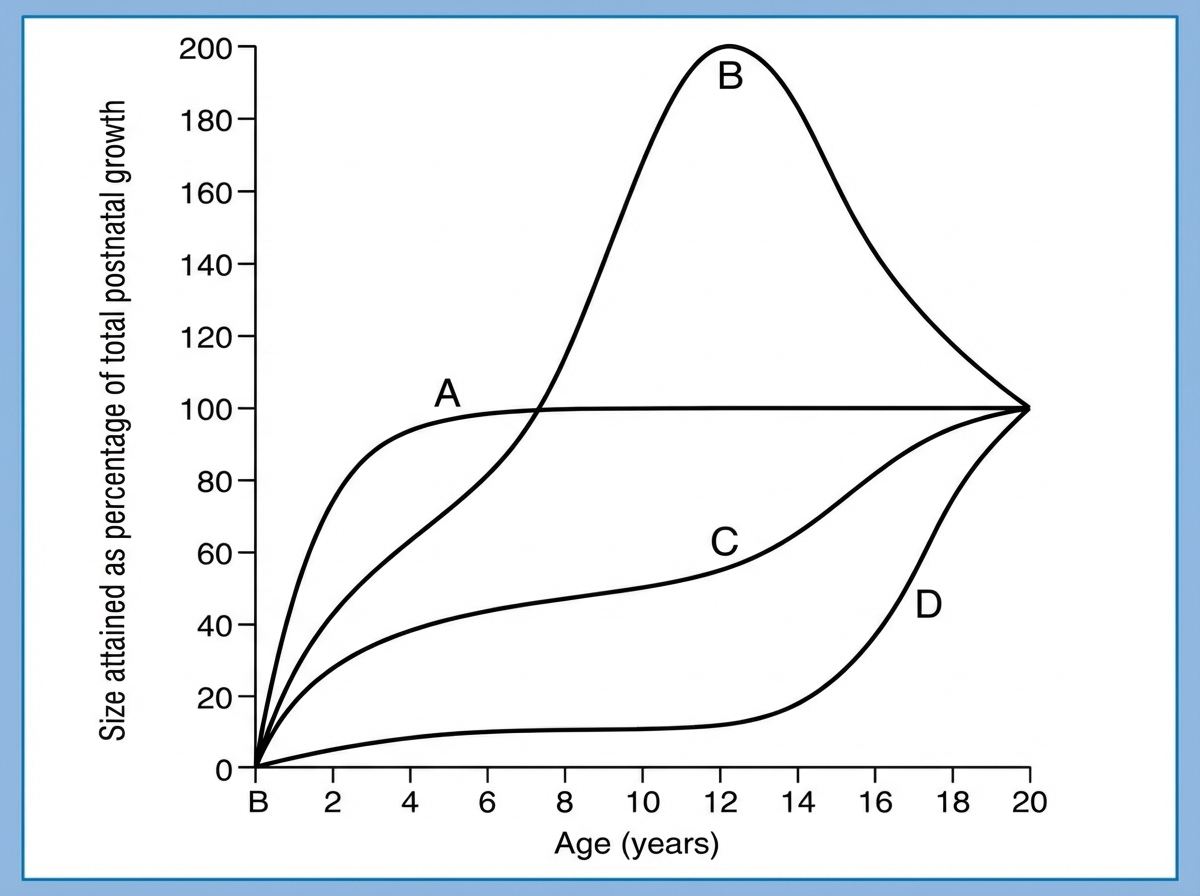
A 14-year-old boy is brought to the physician for the evaluation of back pain for the past six months. The pain is worse with exercise and when reclining. He attends high school and is on the swim team. He also states that he lifts weights on a regular basis. He has not had any trauma to the back or any previous problems with his joints. He has no history of serious illness. His father has a disc herniation. Palpation of the spinous processes at the lumbosacral area shows that two adjacent vertebrae are displaced and are at different levels. Muscle strength is normal. Sensation to pinprick and light touch is intact throughout. When the patient is asked to walk, a waddling gait is noted. Passive raising of either the right or left leg causes pain radiating down the ipsilateral leg. Which of the following is the most likely diagnosis?
A 53-year-old man with a history of alcoholic liver cirrhosis was admitted to the hospital with ascites and general wasting. He has a history of 3-5 ounces of alcohol consumption per day for 20 years and 20-pack-year smoking history. Past medical history is significant for alcoholic cirrhosis of the liver, diagnosed 5 years ago. On physical examination, the abdomen is firm and distended. There is mild tenderness to palpation in the right upper quadrant with no rebound or guarding. Shifting dullness and a positive fluid wave is present. Prominent radiating umbilical varices are noted. Laboratory values are significant for the following: Total bilirubin 4.0 mg/dL Aspartate aminotransferase (AST) 40 U/L Alanine aminotransferase (ALT) 18 U/L Gamma-glutamyltransferase 735 U/L Platelet count 11,000/mm3 WBC 4,300/mm3 Serology for viral hepatitis B and C are negative. A Doppler ultrasound of the abdomen shows significant enlargement of the epigastric superficial veins and hepatofugal flow within the portal vein. There is a large volume of ascites present. Paracentesis is performed in which 10 liters of straw-colored fluid is removed. Which of the following sites of the portocaval anastomosis is most likely to rupture and bleed first in this patient?
A 72-year-old male presents to a cardiac surgeon for evaluation of severe aortic stenosis. He has experienced worsening dyspnea with exertion over the past year. The patient also has a history of poorly controlled hypertension, diabetes mellitus, and hyperlipidemia. An echocardiogram revealed a thickened calcified aortic valve. The surgeon is worried that the patient will be a poor candidate for open heart surgery and decides to perform a less invasive transcatheter aortic valve replacement. In order to perform this procedure, the surgeon must first identify the femoral pulse just inferior to the inguinal ligament and insert a catheter into the vessel in order to gain access to the arterial system. Which of the following structures is immediately lateral to this structure?
A 65-year-old man presents to the emergency department with abdominal pain and a pulsatile abdominal mass. Further examination of the mass shows that it is an abdominal aortic aneurysm. A computed tomography scan with contrast reveals an incidental finding of a horseshoe kidney, and the surgeon is informed of this finding prior to operating on the aneurysm. Which of the following may complicate the surgical approach in this patient?
A 22-year-old Caucasian male is stabbed in his left flank, injuring his left kidney. As the surgeon undertakes operative repair, she reviews relevant renal anatomy. All of the following are correct regarding the left kidney EXCEPT?
A 21-year-old man was involved in a motor vehicle accident and died. At autopsy, the patient demonstrated abnormally increased mobility at the neck. A section of cervical spinal cord at C6 was removed and processed into slides. Which of the following gross anatomic features is most likely true of this spinal cord level?
Practice by Chapter
Anatomical terminology and positions
Practice Questions
Fascial planes and compartments
Practice Questions
Musculoskeletal system overview
Practice Questions
Cardiovascular system overview
Practice Questions
Respiratory system overview
Practice Questions
Digestive system overview
Practice Questions
Urinary system overview
Practice Questions
Reproductive system overview
Practice Questions
Integumentary system
Practice Questions
Anatomical variations and clinical significance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
