Congenital anomalies of GI tract — MCQs

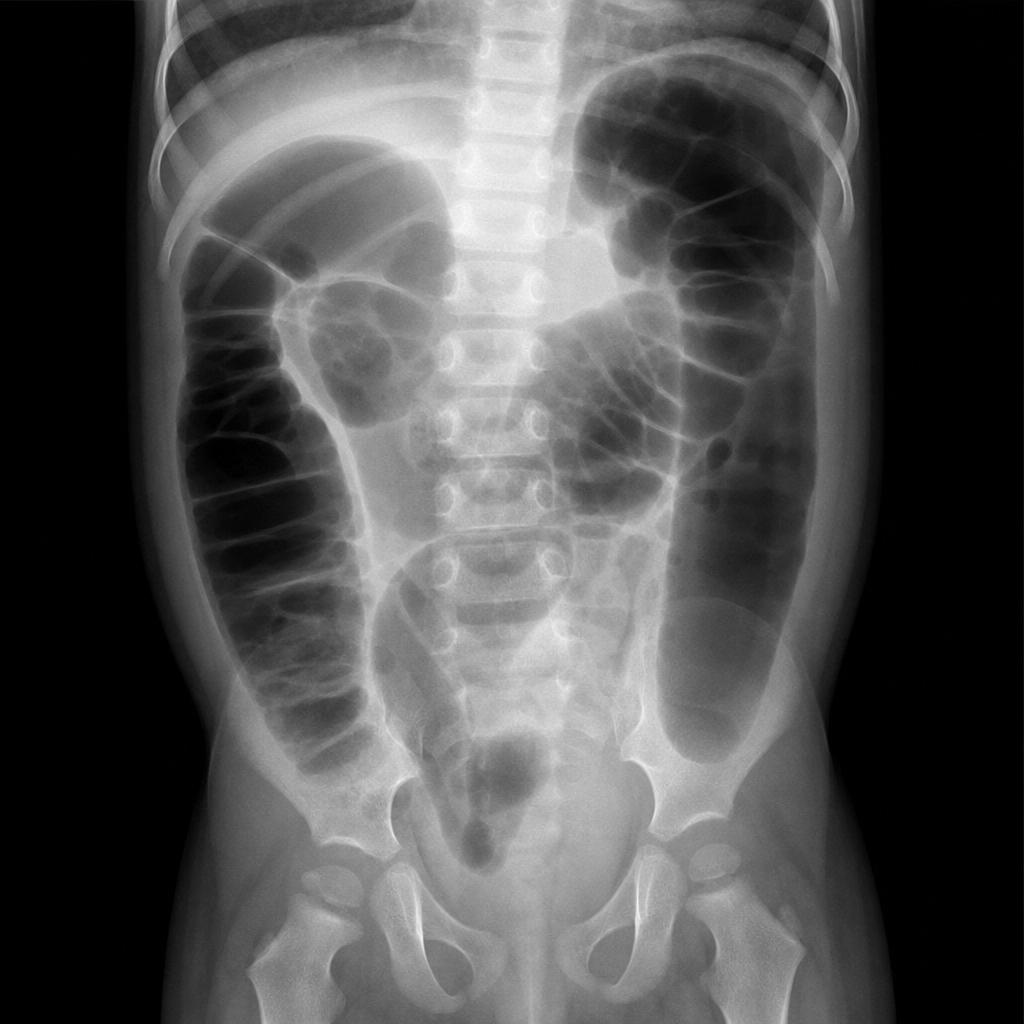
A 5-year-old boy with Down syndrome presents with his mother. The patient’s mother says that he isn’t playing or eating as much as he used to and seems lethargic. Expected developmental delays are present and stable. Physical examination reveals dry mucous membranes and abdominal distention with no tenderness to palpation. An abdominal radiograph is shown in the image below. Which of the following is the most likely diagnosis in this patient?
A 28-year-old primigravid woman is brought to the emergency department after complaining of severe abdominal pain for 3 hours. She has had no prenatal care. There is no leakage of amniotic fluid. Since arrival, she has had 5 contractions in 10 minutes, each lasting 70 to 90 seconds. Pelvic examination shows a closed cervix and a uterus consistent in size with a 38-week gestation. Ultrasound shows a single live intrauterine fetus in a breech presentation consistent with a gestational age of approximately 37 weeks. The amniotic fluid index is 26 and the fetal heart rate is 92/min. The placenta is not detached. She is scheduled for an emergency lower segment transverse cesarean section because of a nonreassuring fetal heart rate. The infant is delivered and APGAR score is noted to be 8 at 1 minute. The doctor soon notices cyanosis of the lips and oral mucosa, which does not resolve when the infant cries. The infant is foaming at the mouth and drooling. He also has an intractable cough. Which of the following is the most likely diagnosis?
A 4-week-old infant is brought to the emergency department by his parents with violent vomiting. It started about 3 days ago and has slowly gotten worse. He vomits after most feedings but seems to keep some formula down. His mother notes that he is eager to feed between episodes and seems to be putting on weight. Other than an uncomplicated course of chlamydia conjunctivitis, the infant has been healthy. He was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. The physical exam is significant for a palpable mass in the right upper quadrant. What is the first-line confirmatory diagnostic test and associated finding?
A 3-week-old boy has non-bilious projectile vomiting that occurred after feeding. After vomiting, the infant is still hungry. The infant appears dehydrated and malnourished. A firm, “olive-like” mass of about 1.5 cm in diameter is palpated in the right upper quadrant, by the lateral edge of the rectus abdominus muscle. On laboratory testing, the infant is found to have a hypochloremic, hypokalemic metabolic alkalosis. Which of the following is most likely the cause of this patient’s symptoms?
A 5-year-old girl is brought to a medical office for evaluation of persistent abdominal pain that has worsened over the past 24 hours. The mother states that the girl often has constipation which has worsened over the last 3 days. The mother denies that the girl has had bloody stools. The girl has not had a bowel movement or passed flatulence in 72 hours. She has vomited 3 times since last night and refuses to eat. She has no significant medical history, including no history of surgeries. On exam, there are no abdominal masses; however, the upper abdomen is distended and tympanic. What is the most likely underlying cause of the girl’s symptoms?
A new imaging modality is being tested to study vitelline duct morphology. A fetus at 20 weeks' gestation is found to have partial obliteration of this duct. Which of the following is the most likely sequela of this condition?
A 2-year-old boy is brought in to his pediatrician for a routine checkup. The parents mention that the child has been developing appropriately, although they have been noticing that the child appears to have chronic constipation. The parents report that their child does not routinely have daily bowel movements, and they have noticed that his abdomen has become more distended recently. In the past, they report that the patient was also delayed in passing meconium, but this was not further worked up. On exam, his temperature is 98.6°F (37.0°C), blood pressure is 110/68 mmHg, pulse is 74/min, and respirations are 14/min. The patient is noted to have a slightly distended abdomen that is nontender. Eventually, this patient undergoes a biopsy. Which of the following layers most likely reveals the causative pathologic finding of this disease?
An 8-month-old boy is brought to a medical office by his mother. The mother states that the boy has been very fussy and has not been feeding recently. The mother thinks the baby has been gaining weight despite not feeding well. The boy was delivered vaginally at 39 weeks gestation without complications. On physical examination, the boy is noted to be crying in his mother’s arms. There is no evidence of cyanosis, and the cardiac examination is within normal limits. The crying intensifies when the abdomen is palpated. The abdomen is distended with tympany in the left lower quadrant. You suspect a condition caused by the failure of specialized cells to migrate. What is the most likely diagnosis?
A 3-week-old firstborn baby girl is brought to the pediatric emergency room with projectile vomiting. She started vomiting while feeding 12 hours ago and has been unable to keep anything down since then. After vomiting, she appears well and hungry, attempting to feed again. The vomitus has been non-bloody and non-bilious. The last wet diaper was 10 hours ago. The child was born at 40 weeks gestation to a healthy mother. On examination, the child appears sleepy but has a healthy cry during the exam. The child has dry mucous membranes and delayed capillary refill. There is a palpable olive-shaped epigastric mass on palpation. Which of the following is the most likely cause of this patient's condition?
A 72-year-old male with a past medical history significant for aortic stenosis and hypertension presents to the emergency department complaining of weakness for the past 3 weeks. He states that, apart from feeling weaker, he also has noted lightheadedness, pallor, and blood-streaked stools. The patient's vital signs are stable, and he is in no acute distress. Laboratory workup reveals that the patient is anemic. Fecal occult blood test is positive for bleeding. EGD was performed and did not reveal upper GI bleeding. Suspecting a lower GI bleed, a colonoscopy is performed after prepping the patient, and it is unremarkable. What would be an appropriate next step for localizing a lower GI bleed in this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
