Upper limb fascial compartments — MCQs

A patient presents with difficulty extending their wrist following trauma to the posterior forearm. Which of the following muscles would be most affected by injury to the posterior interosseous nerve?
A 34-year-old woman comes to the physician because of a 3-month history of pain in her right thumb and wrist that radiates to her elbow. It is worse when she holds her infant son and improves with the use of an ice pack. Six months ago, she slipped on a wet floor and fell on her right outstretched hand. Her mother takes methotrexate for chronic joint pain. The patient takes ibuprofen as needed for her current symptoms. Examination of the right hand shows tenderness over the radial styloid with swelling but no redness. There is no crepitus. Grasping her right thumb and exerting longitudinal traction toward the ulnar side elicits pain. Range of motion of the finger joints is normal. There is no swelling, redness, or tenderness of any other joints. Which of the following is the most likely diagnosis?
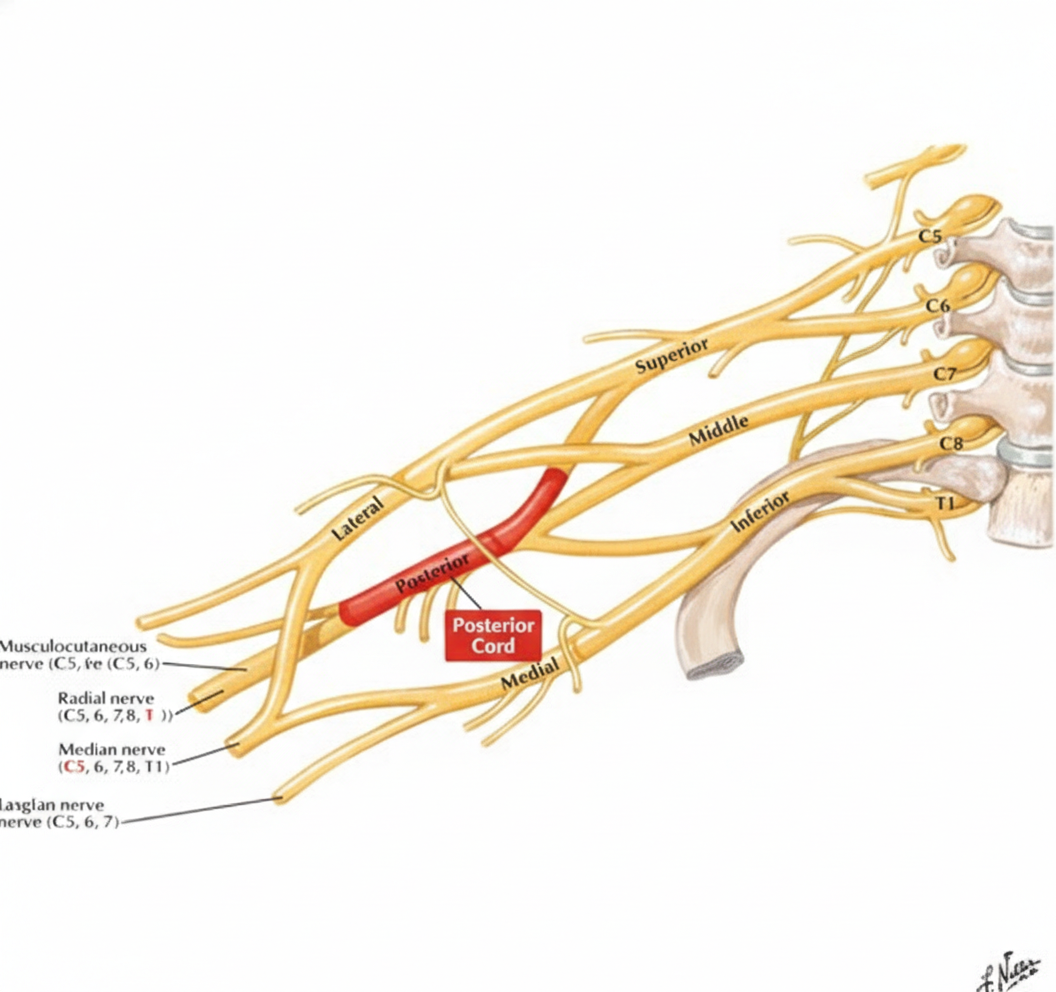
A 43-year-old woman comes to the physician because of tingling and weakness in her left arm for the past 2 days. An image of the brachial plexus is shown. Nerve conduction study shows decreased transmission of electrical impulses in the labeled structure. Physical examination is most likely to show impairment of which of the following movements?
A 45-year-old man comes to the physician for the evaluation of limited mobility of his right hand for 1 year. The patient states he has had difficulty actively extending his right 4th and 5th fingers, and despite stretching exercises, his symptoms have progressed. He has type 2 diabetes mellitus. He has been working as a mason for over 20 years. His father had similar symptoms and was treated surgically. The patient has smoked one pack of cigarettes daily for 25 years and drinks 2–3 beers every day after work. His only medication is metformin. Vital signs are within normal limits. Physical examination shows skin puckering near the proximal flexor crease. There are several painless palmar nodules adjacent to the distal palmar crease. Active and passive extension of the 4th and 5th digits of the right hand is limited. Which of the following is the most likely underlying mechanism of this patient's symptoms?
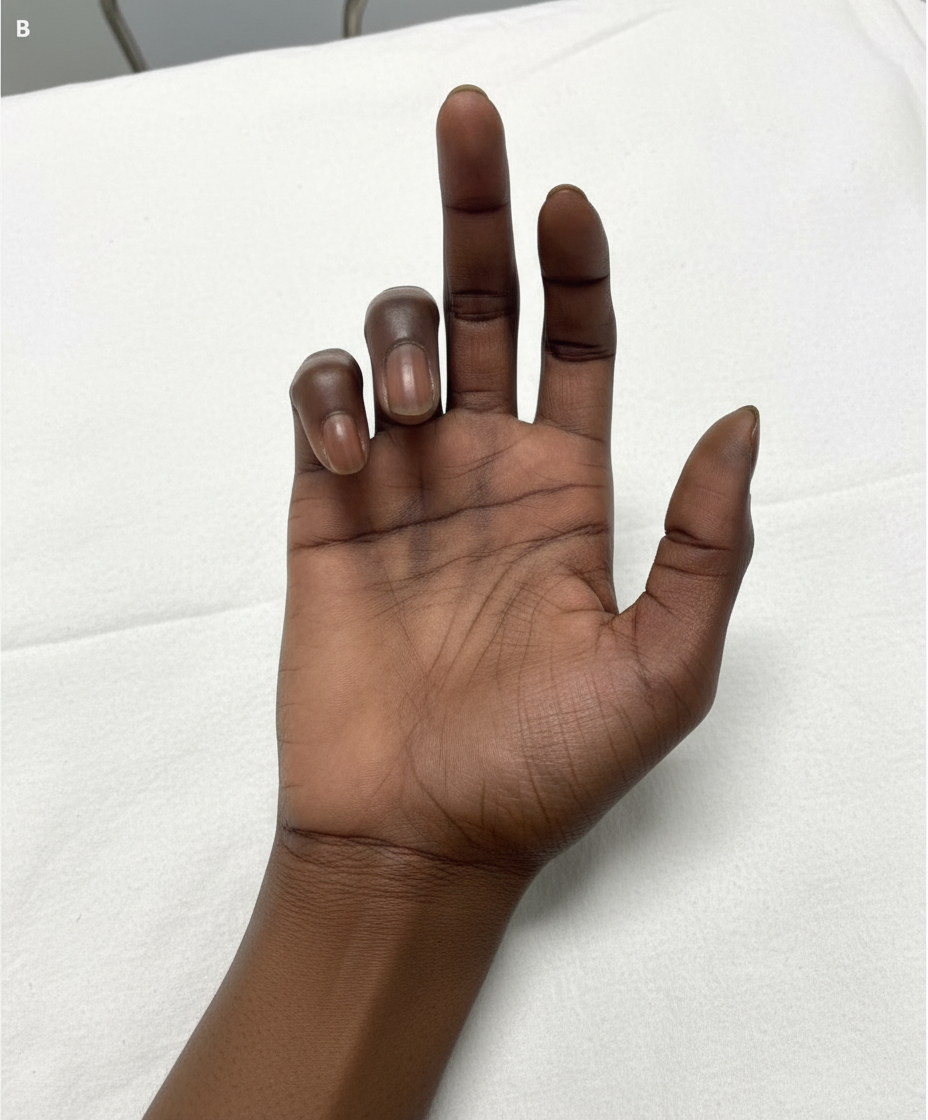
A 30-year-old man presents with weakness in his right hand. He says he has been an avid cyclist since the age of 20. He denies any recent trauma. Physical examination reveals decreased sensations over the 4th and 5th digits with difficulty extending the 4th and 5th digits. Strength is 4 out of 5 in the extensor muscles of the right hand and wrist. When the patient is asked to extend his fingers, the result is shown in the image. Which of the following nerves is most likely damaged in this patient?
A 23-year-old patient presents to the emergency department after a motor vehicle accident. The patient was an unrestrained driver involved in a head-on collision. The patient is heavily intoxicated on what he claims is only alcohol. An initial trauma assessment is performed, and is notable for significant bruising of the right forearm. The patient is in the trauma bay, and complains of severe pain in his right forearm. A physical exam is performed and is notable for pallor, decreased sensation, and cool temperature of the skin of the right forearm. Pain is elicited upon passive movement of the right forearm and digits. A thready radial pulse is palpable. A FAST exam is performed, and is negative for signs of internal bleeding. The patient's temperature is 99.5°F (37.5°C), pulse is 100/min, blood pressure is 110/70 mmHg, respirations are 12/min, and oxygen saturation is 98% on room air. Radiography of the right forearm is ordered. The patient is still heavily intoxicated. Which of the following is the best next step in management?
A 35-year-old man is referred to a physical therapist due to limitation of movement in the wrist and fingers of his left hand. He cannot hold objects or perform daily activities with his left hand. He broke his left arm at the humerus one month ago. The break was simple and treatment involved a cast for one month. Then he lost his health insurance and could not return for follow up. Only after removing the cast did he notice the movement issues in his left hand and wrist. His past medical history is otherwise insignificant, and vital signs are within normal limits. On examination, the patient’s left hand is pale and flexed in a claw-like position. It is firm and tender to palpation. Right radial pulse is 2+ and left radial pulse is 1+. The patient is unable to actively extend his fingers and wrist, and passive extension is difficult and painful. Which of the following is a proper treatment for the presented patient?
A 47-year-old woman presents to her primary care provider because of numbness and tingling on the palmar aspects of both hands. She denies any symptoms at the base of her thumbs. The symptoms are worse on the right (dominant hand) and are increased with activities such as driving or brushing her hair. She frequently wakes up with pain and has to shake her hand for pain relief. She has had rheumatoid arthritis for 9 years, for which she takes methotrexate. Her blood pressure is 124/76 mm Hg, the heart rate is 75/min, and the respiratory rate is 15/min. Lightly tapping over the middle of the anterior aspect of the right wrist leads to a tingling sensation in the palm. In this patient, electromyography (EMG) will most likely show which of the following results?
A 35-year-old man is brought to the trauma bay by ambulance after sustaining a gunshot wound to the right arm. The patient is in excruciating pain and states that he can't move or feel his hand. The patient states that he has no other medical conditions. On exam, the patient's temperature is 98.4°F (36.9°C), blood pressure is 140/86 mmHg, pulse is 112/min, and respirations are 14/min. The patient is alert and his Glasgow coma scale is 15. On exam, he has a single wound on his right forearm without continued bleeding. The patient has preserved motor and sensation in his right elbow; however, he is unable to extend his wrist or extend his fingers further. He is able to clench his hand, but this is limited by pain. On sensory exam, the patient has no sensation to the first dorsal web space but has preserved sensation on most of the volar surface. Which of the following structures is most likely injured?
A 35-year-old woman presents with progressive vision loss and severe headache. MRI shows cavernous sinus thrombosis with extension into the superior ophthalmic vein. Blood cultures grow Staphylococcus aureus. History reveals she had squeezed a facial pustule near her upper lip 5 days prior. Evaluate the anatomical explanation and risk stratification for this complication.
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
