Embryology — MCQs

On this page
What is the pattern of inheritance in neural tube defects?
The covering of an omphalocele is derived from which of the following layers?
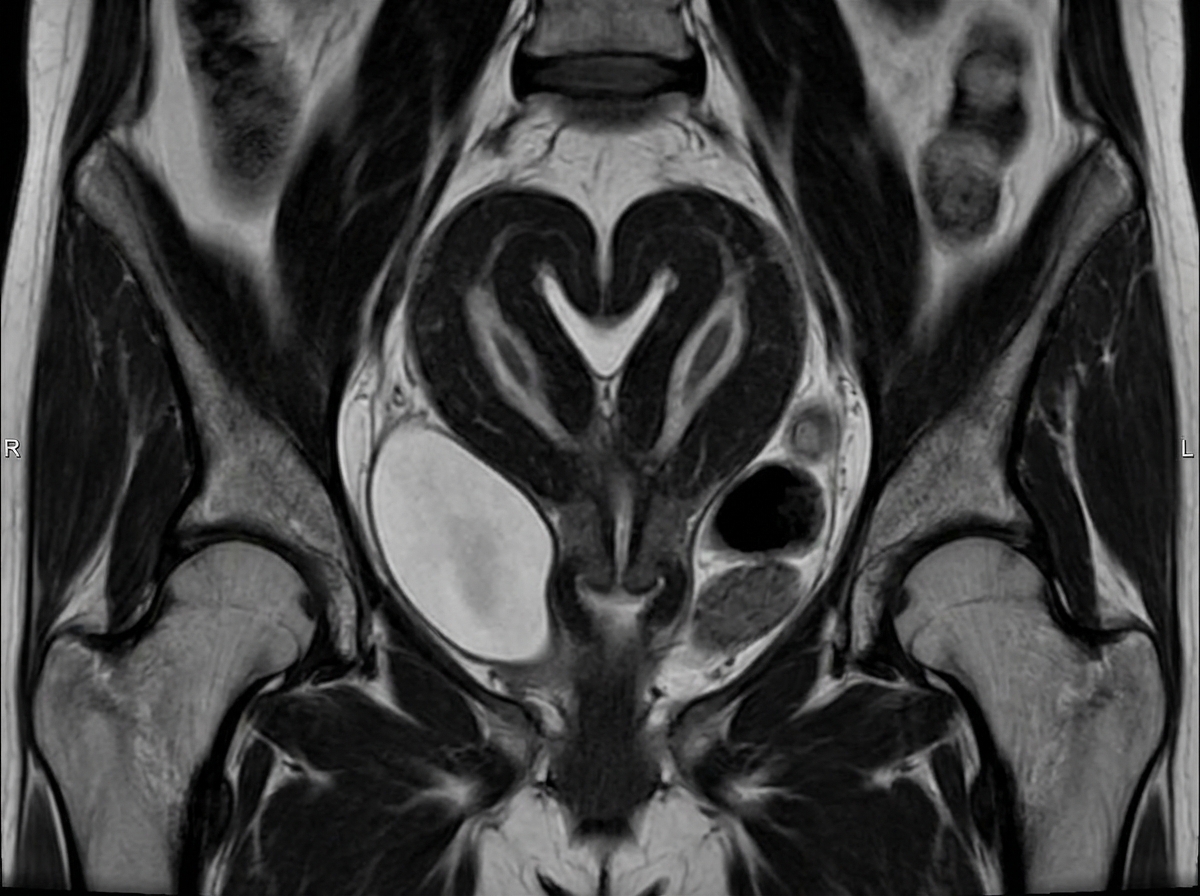
Identify the uterus shown in the image?
Scientists are studying human lung development by trying to identify which proteins and signaling factors trigger lung bud division and bronchiole branching. Their main focus is particularly around the 20th week of gestation, during which terminal bronchioles branch into respiratory bronchioles and further into alveolar ducts. Which of the following phases of embryonic lung development is the stage in which the scientists are interested in studying?
During the obstetric clerkship, the doctor is observing a 3rd-year resident assist a delivery. The patient only had 1 prenatal ultrasound that reported a male fetus. The delivery progresses without complications. The pediatrician-in-charge of the newborn notices a short, broad, upturned penis with an orifice in its dorsal aspect, and both testicles are present in the scrotum. Both the attending and PGY-3 resident immediately recognize the condition. Which of the following female anatomical structures is derived from the embryonic structure affected in this patient?
Practice by Chapter
Gametogenesis
Practice Questions
Fertilization and zygote formation
Practice Questions
Cleavage and blastocyst formation
Practice Questions
Implantation
Practice Questions
Bilaminar and trilaminar disc formation
Practice Questions
Neurulation and neural tube development
Practice Questions
Somite formation and derivatives
Practice Questions
Placenta and fetal membranes
Practice Questions
Limb development
Practice Questions
Urogenital system development
Practice Questions
Teratogens and critical periods
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
